Research Article
Austin J Public Health Epidemiol. 2014;1(1): 1003.
Weight Loss Practice by Weight Status Among Adolescents
Duan R1,2†, Vidot DC1†, Hlaing WM1*
1Department of Public Health Sciences, University of Miami Miller School of Medicine, USA
2Department of Epidemiology, Florida International University, USA
†Duan and Vidot contributed equally to the manuscript
*Corresponding author: Hlaing WM, Department of Public Health Sciences, University of Miami, Miller School of Medicine, Clinical Research Building, 1120 NW 14th Street, Suite 914, Miami, Florida 33136, USA
Received: May 20, 2014; Accepted: June 13, 2014; Published: June 17, 2014
Abstract
Aim: To determine the association of weight status and Unhealthy Weight Loss Practice (UWLP) among 12-to-18-year-old adolescents
Methods: A cross-sectional study of 12-to-18 year olds (N=6,212) from the 2011 Youth Risk Behavior Survey in Florida was conducted. UWLP was categorized based on self-report of at least one of three methods to lose weight: 1) ≥ 24 hours of fasting, 2) diet pill use and 3) laxative use/purging. The reference group included those with no reported UWLP. Logistic regression, adjusted for demographic, substance use, and exercise variables, assessed relationships between weight status (defined by age-sex-specific body mass index percentiles) and UWLP.
Results: Analysis was restricted to 5,323 adolescents who had complete weight status information. About 13.3% of adolescents reported at least one UWLP. A quarter of the sample (25.1%) was either overweight or obese. The prevalence of UWLP was highest in obese (23.1%) and overweight (17.6%) adolescents compared to 11.1% of healthy weight adolescents. Obese and overweight adolescents were significantly more likely than healthy weight adolescents to exhibit at least one UWLP (adjusted odds ratios [AOR]=2.85, 95% confidence interval [CI]=2.17-3.74; AOR=1.66, 95% CI=1.27-2.16, respectively). Adolescents who reported tobacco (AOR=1.78, 95% CI=1.31- 2.40), alcohol (AOR=1.58, 95% CI=1.27-1.96), marijuana (AOR=1.0, 95% CI=0.72-1.39) or cocaine use (AOR=3.69, 95% CI=2.37-5.75) had higher odds of UWLP compared to non-user counterparts.
Conclusions: Overweight and obese adolescents present with higher odds of engaging in UWLP compared to healthy weight peers. These findings have important implications as the prevalence of obesity in adolescence remains a concern in Florida and in the United States.
Keywords: Adolescents; Obesity; Overweight; Unhealthy weight loss; YRBS
Abbreviations
AOR: Adjusted Odds Ratios; BMI: Body Mass Index; CDC: Centers for Disease Control and Prevention; CI: Confidence Intervals; OR: Odds Ratios; UWLP: Unhealthy Weight Loss Practice; US: United States; YRBS: Youth Risk Behavior Survey
Introduction
Obesity remains one of the top public health concerns in the United States (U.S.) [1]. Alarmingly, the prevalence of obesity among U.S. adolescents aged 12-to-19 years has quadrupled from 5% to 21% in the past 30 years [2,3]. In Florida, the proportion of overweight or obese children between the ages 10-to-17-years was 33.1% in 2007, which was higher than the nation's (31.6%) prevalence [4].
Studies have shown that obese adolescents are not only more likely to have at least one cardiovascular disease risk factor, they are also significantly more likely to exhibit negative health outcomes such as bone and joint problems, sleep apnea, and psychological problems such as poor self-esteem [5-9]. In addition, there has been a recent increase in the proportion of adolescents with type 2 diabetes corresponding to the rise of overweight status and obesity [9]. The increased risk of negative health outcomes contribute toward the rising cost of medical care, which was about $1,429 higher per year in obese people compared to those of healthy weight [9,10]. The economic burden caused by childhood obesity alone is estimated to be about $14 billion annually in direct health expenses [11,12]. When comparing children covered by Medicaid to those under private insurance, Medicaid children were about six times more likely to be treated for a diagnosis of obesity [12].
It is known that adolescence is a vital stage in development in regard to establishing health behaviors that have the potential to persist into adulthood [13]. Adolescence is a period that is gaining more recognition for weight loss interventions and treatments, such as bariatric surgery [14,15], which contributes toward the evidence that obesity during adolescence is of concern. Furthermore, previous studies have shown that the risk for eating disorders and associated weight-related behaviors are at the highest during the period of adolescence [16-18]. Adolescents with eating disorders such as anorexia nervosa and bulimia nervosa have been shown to exhibitcommon risk factors attributed to obesity such as weight and shape concerns, loss of control of food consumption, and unhealthy weight regulation behaviors [19]. Eating disorders are also increasing as a cause of morbidity and mortality in young individuals [20].
The primary aim of this study was to determine the relationship between weight status (underweight, healthy weight, overweight, and obese) and unhealthy weight loss practice among 12-to-18-year-old high school students using the Youth Risk Behavior Survey (YRBS) of Florida. We hypothesized that the prevalence of unhealthy weight loss practice differs among underweight, healthy weight, overweight and obese adolescents. We also aimed to evaluate the relationship between perceived and actual weight status among adolescents.
Methods
Study population
Study population consisted of 12-to-18-year-old students (N=6,212) from the Youth Risk Behavior Survey (YRBS) collected from Florida high schools in 2011. The YRBS is a Center for DiseaseControl and Prevention (CDC) survey administered to public high school students in the spring or fall semesters of odd-numbered years [21] that uses a two-staged, cluster sample design to select a sample representative of 9th to 12th grade students in its jurisdiction [22]. Details of survey administration are described elsewhere [22].
Briefly, in-class questionnaires were completed by the student on a computer-scannable format. A few in-class strategies were employed to minimize the possibility of students seeing each other's responses as they completed the questionnaire. Questionnaire booklets were sealed and placed in an unmarked envelope at end of administration to further protect response privacy [22]. According to the data collection protocol [22], students who were absent on the day the questionnaire was initially administered still had the opportunity to complete the questionnaire at a later date. This allowed for increased response rates and collection of data representative of all high school students in Florida. In 2011, Florida school, student, and overall response rates were 92%, 78%, and 75%, respectively. The corresponding national school, student, and overall response rateswere 81%, 87%, and 71%, respectively [23]. Parents of the students provided passive permission by signing a form only if they did not want their child to participate in the survey [22].
Weight loss practice
The primary outcome of interest was the Unhealthy Weight Loss Practice (UWLP) defined as those who reported one or more of three methods to lose weight: (1) ≥ 24 hours of fasting, (2) diet pill use, and (3) laxative use or purging. The response from the following questions were used to define UWLP: (1) During the past 30 days, did you go without eating for 24 hours or more (also called fasting) to lose weight or to keep from gaining weight?; (2) During the past 30 days, did you take any diet pills, powders, or liquids without a doctor's advice to lose weight or to keep from gaining weight? (Do not include meal replacement products such as Slim Fast.); (3) During the past 30 days, did you vomit or take laxatives to lose weight or to keep from gaining weight?"[24] The reference group was defined as students who reported none of the three aforementioned methods to lose weight or to keep from gaining weight.
Weight status
Perceived weight status was categorized into three groups (underweight, healthy weight, and overweight) from five original response options based on the following question: "How do you describe your weight?" (very underweight, slightly underweight, about the right weight, slightly overweight, and very overweight) [24]. Very underweight and slightly underweight were grouped as "underweight"; about the right weight was grouped and named as "healthy weight"; and slightly overweight and very overweight were grouped as "overweight". Actual weight status was defined using the CDC standardized age-sex-specific Body Mass Index (BMI) percentiles based on self-reported height and weight. Underweight, healthy weight, overweight, and obese were defined as less than the 5th percentile, 5th percentile to less than the 85th percentile, 85th to less than the 95th percentile and equal to or greater than the 95th percentile of BMI, respectively [25].
Covariates
Gender, age, race/ethnicity, grade, substance use, and exercise performed were considered covariates a priori. The YRBS captured gender as male/female and age as 12 years old or younger, 13 years old, 14 years old, 15 years old, 16 years old, 17 years old, and 18 years old or older. Race/ethnicity was defined as White, Black or African American, Hispanic, American Indian/Alaska Native, Asian, and Native Hawaiian/Other Pacific Islander. Due to small sample size, American Indian/Alaska Native, Asian, and Native Hawaiian/Other Pacific Islander were combined to create an "other" race/ethnic group. The current grade level in school was classified as 9th, 10th, 11th, and 12th grade, as well as ungraded or other grade [24]. Substance use, including cigarette, alcohol, marijuana and cocaine use were defined using the following questions: "(1) During the past 30 days, on how many days did you smoke cigarettes?; (2) During the past 30 days, on how many days did you have at least one drink of alcohol?; (3) During the past 30 days, how many times did you use marijuana?; (4) During the past 30 days, how many times did you use any form of cocaine, including powder, crack, or freebase?". Cigarette, alcohol, marijuana, and cocaine use were treated as individual binary variables (1=use, 0=no-use) in current analysis. Exercise, treated as a continuousvariable, was defined as the number of days per week having 20 minutes of vigorous exercise or 30 minutes of moderate exercise [24].
Statistical analysis
Statistical Analytic Software (SAS) version 9.3 (SAS Institute, Inc., Cary, North Carolina) was used for all analyses. The sampling design, weight and non-response effects were taken into account in all analyses. Weighted survey frequencies and Rae-Scott Chi-Square tests were used to compare demographic, school performance, substance use and unhealthy weight loss method differences between weight status groups (underweight, healthy weight, overweight, and obese). ANOVA was used to compare the mean days of exercise between groups. Both univariate and multivariable logistic regression were used to evaluate the association between UWLP and selected demographics (age, gender, race/ethnicity, and grade), school performance, behavioral variables (cigarette, alcohol, marijuana and cocaine use, exercise), and weight status. Results are reported as unadjusted and adjusted odds ratios (AOR) with 95% Confidence Intervals (CI). All tests were performed at a significance level of 0.05.
Result
Sample characteristics
The sample (N=6,212) represented 787, 657 public high school students (grades 9-12) in Florida. Analysis was restricted to 5,323 (weighted N=678,193) students with complete weight status information (889 students had missing weight status). Overall, there were more males (50.4%) and whites (47.3%) than their respective counterparts in the entire sample. The majority of the sample (> 64%) was 16 years of age or older in each weight status group.
About 14.0%, 37.3%, 22.3% and 2.7% of the adolescents reported smoking cigarette, drinking alcohol, using marijuana or cocaine respectively. There were no significant differences of cigarette smoking, alcohol and cocaine use cross the four weight status groups. Obese adolescents had the highest (25.0%) and overweight adolescents had the lowest (17.8%) proportion of marijuana use. There were no significant differences in exercise frequency among the four weight status groups. Detailed demographic characteristics byweight status groups are described in Table 1.
Underweighta
(Nb=25,295)
Healthy Weight a
(Nb=482,368)
Overweighta
(Nb=92,366)
Obesea
(Nb=78,165)
χ2
p-value
(nc =202)
(nc =3,777)
(nc =736)
(nc�=608)
n c
%d
n c
%d
n c
%d
n c
%d
Age
6.9
0.077
12-15 years
55
26.5
1352
34.7
269
35.8
197
31.5
>=16 years
147
73.5
2425
65.3
467
64.2
411
68.5
Gender
78.2
< 0.001
Male
103
55.2
1676
47.4
354
51.2
386
66.7
Female
99
44.8
2101
52.6
382
48.8
222
33.3
Grade Level
18.7
0.028
12th
58
30.4
838
24.0
133
19.6
124
21.4
11th
53
26.7
892
23.9
176
24.7
147
25.0
10th
47
21.9
982
25.1
210
26.9
179
29.2
9th
44
21.0
1042
27.0
210
28.8
153
24.4
Race/Ethnicity
93.2
< 0.001
Others
26
8.7
302
5.4
53
4.9
50
5.6
Hispanics
55
26.6
1050
25.4
208
26.9
163
25.4
African-Americans
27
13.3
730
19.7
201
27.3
175
29.4
Whites
89
51.4
1632
49.5
260
40.9
209
39.6
School Performance
56.5
< 0.001
Grade C or worse
42
22.7
834
22.9
170
24.6
195
35.4
Mostly Bs
95
52.2
1603
45.1
348
50.3
235
42.7
Mostly As
45
25.2
1106
32.0
168
25.1
122
22.0
Substance use
Smoke Cigarette
25
15.1
492
13.5
110
15.7
85
14.5
3.1
0.370
Drink Alcohol
63
33.7
1388
38.0
250
34.9
220
36.9
3.1
0.373
Marijuana Use
39
22.5
812
22.7
128
17.8
150
25.0
10.4
0.016
Cocaine Use
6
3.1
94
2.5
23
3.1
22
3.5
2.2
0.530
Table 1: Demographic characteristics of study participants (nc=5,323) by actual weighted status.
Prevalence of weight status and weight loss practices
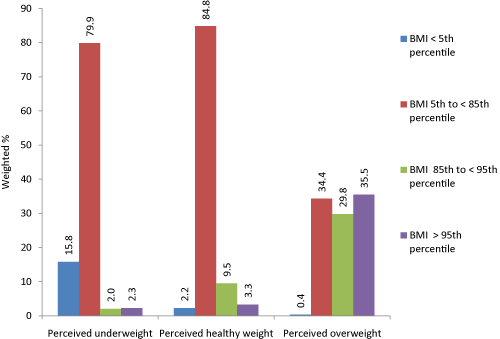
Most adolescents (71.1%) were within the healthy weight per BMI percentile; however, 13.6% were overweight and 11.5% were obese. About14.1%, 60.1% and 25.8% of adolescents perceived their weight status to be underweight, healthy weight or overweight, respectively. The agreement between perceived and actual weight was 16% (underweight), 85% (healthy weight), and 65% (at-risk for overweight and overweight combined). Approximately 9.8%, 2.4% and 1.1% of adolescents reported one, two and three unhealthy weight loss practices, respectively (Data not shown). Over 80% of adolescents who perceived themselves to be underweight or healthy weight were actually in the healthy weight BMI percentile range. About 0.4% of underweight and 34.4% of healthy weight adolescents perceived themselves to be overweight (Figure 1). The prevalence of at least one reported unhealthy weight loss practice was highest in overweight (17.6%) and obese (23.1%) adolescents compared to 11.1% of healthy weight adolescents (Table 2).
Figure 1 :Perceived and actual weight status among Florida adolescents, 2011.
Underweight
Healthy Weight
Overweight
Obese
χ2
p-value
N
%*
N
%*
N
%*
N
%*
Current weight control measures
663.6
< 0.001
Lose weight
24
11.6
1330
34.9
506
69.0
447
74.0
Gain weight
82
41.9
810
22.4
60
8.4
26
4.6
Stay the same weight
38
18.8
889
23.9
92
12.6
63
11.2
Not doing anything about weight
53
27.8
685
18.8
71
10.0
58
10.2
Fast > 24 hours to lose weight
13
5.8
307
8.0
88
11.6
93
15.3
37.2
< 0.001
Take diet pills to lose weight
7
3.3
141
3.8
52
7.1
60
10.0
52.8
< 0.001
Take laxatives or purge to lose weight
2
0.9
131
3.4
31
3.9
39
5.9
15.6
0.001
At least one unhealthy weight Loss practice
19
8.5
424
11.1
130
17.6
139
23.1
83.3
< 0.001
Mean
SE**
Mean
SE**
Mean
SE**
Mean
SE**
F-value
p-value
Days of Exercise
3.9
0.2
4.3
0.1
4.2
0.1
4.1
0.1
2.2
0.109
Table 2: Weight loss practice, substance use and exercise by actual weight status.
Correlates of unhealthy weight loss practices
Compared to the referent healthy weight group, overweight (OR=1.70, 95% CI=1.38-2.11) and obese (OR=2.41, 95% CI=1.93- 3.00) adolescents were more likely to exhibit at least one unhealthy weight loss practice. Adolescents between the ages 12 and 15 years were less likely (OR=0.79, 95% CI=0.66-0.95) to exhibit at least one unhealthy weight loss practice compared to older adolescents (16 years or older). In addition, females were more likely (OR=2.02, 95% CI=1.70-2.39) to exhibit at least one unhealthy weight loss practice compared to their male counterparts. Adolescents who reported tobacco (OR=2.85, 95% CI=2.30-3.54), alcohol (OR=2.26, 95% CI=1.91-2.68), marijuana (OR=2.05, 95% CI=1.69-2.47) or cocaine (OR=6.17, 95% CI=4.61-8.27) use were associated with significantly higher odds of unhealthy weight loss practice compared to their respective non-user counterparts. Students with grade C or worse were more likely (OR=1.89, 95%CI=1.50-2.37) than grade A students to report at least one unhealthy weight loss practice (Table 3).
Unadjusted ORa
95% CI
Adjusted ORa
95% CI
Lower
Upper
Lower
Upper
Age
12-15 years
0.79
0.66
0.95
0.89
0.64
1.25
>=16 years
1.00
1.00
Gender
Females
2.02
1.70
2.39
3.17
2.44
4.13
Male
1.00
1.00
Race/Ethnicity
Other
1.17
0.90
1.52
1.05
0.70
1.56
Hispanic/Latino
1.53
1.29
1.82
1.31
1.02
1.67
Black or African American
1.15
0.91
1.46
1.00
0.73
1.38
White
1.00
1.00
Grade
12th Grade
1.20
0.97
1.50
1.09
0.72
1.65
11th Grade
1.28
1.02
1.60
1.05
0.71
1.54
10th Grade
1.16
0.89
1.51
1.11
0.80
1.55
9th�� Grade
1.00
1.00
School Performance
Grade C or Worse
1.89
1.50
2.37
1.59
1.24
2.04
Grade B
1.22
0.97
1.54
1.08
0.85
1.38
Grade A
1.00
1.00
Weight Status
Obese
2.41
1.93
3.00
2.85
2.17
3.74
Overweight
1.70
1.38
2.11
1.66
1.27
2.16
Underweight
0.74
0.47
1.16
0.88
0.53
1.48
Healthy Weight
1.00
Smoke Cigarette
2.85
2.30
3.54
1.78
1.31
2.40
Drink Alcohol
2.26
1.91
2.68
1.58
1.27
1.96
Marijuana Use
2.05
1.69
2.47
1.00
0.72
1.39
Cocaine Use
6.17
4.61
8.27
3.69
2.37
5.75
Exercise
0.95
0.91
0.98
1.00
0.95
1.05
Table 3: Unadjusted and adjusted Odds Ratios (OR) of at least one unhealthy weight loss practice.
In the multivariable logistic model controlling for demographics, substance use, and exercise variables, obese (AOR=2.85, 95% CI=2.17- 3.74) and overweight (AOR=1.66, 95% CI=1.27-2.16) adolescents were more likely than healthy weight adolescents to exhibit at least one unhealthy weight loss practice. In the final model, gender, smoking, drinking, and cocaine use were significantly associated with unhealthy weight loss practice. Females were significantly more likely to exhibit any unhealthy weight loss practice (AOR=3.17, 95% CI=2.44 - 4.13) compared to males. Adolescents who reported smoking cigarette (AOR=1.78, 95% CI=1.31-2.40), drinking alcohol (AOR=1.58, 95% CI=1.27-1.96), or using cocaine in past 30 days (AOR=3.69, 95% CI=2.37-5.75) were significantly more likely to exhibit at least one unhealthy weight loss practice compared to their respective non-users (Table 3).
Discussion
A quarter of the adolescents in our sample were either overweight or obese, which is comparable to the national prevalence [4]. Similarly, prevalence of overweight and obese remained stable around 25% in Florida youths in the last decade (i.e., alternating survey years from 2001 through 2011) [26]. The proportions (%) of overweight among Florida youth in the corresponding (survey year) were 13.9 (2001), 13.6 (2003), 14.3 (2005), 15.1 (2007), 14.7 (2009), and 13.6 (2011). The proportions (%) of obese among Florida youth in the corresponding (survey year) were 10.1 (2001), 12.1 (2003), 10.8 (2005), 11.2 (2007), 10.2 (2009), and 11.5 (2011) [26]. Results from the current study suggest that overweight and obese adolescents were significantly more likely than their healthy weight counterparts to exhibit at least one unhealthy weight loss practice. The odds of engaging in unhealthy weight loss practices were higher among females, adolescents aged 16 years or older, those with grade C or worse, and among those who reported use of tobacco, alcohol, marijuana, or cocaine. These findings have important implications for public health considering the high prevalence of obesity, and related chronic conditions (e.g., cardiovascular disease and diabetes) in the U.S. beginning at a young age and increasing across late adolescence into adulthood.
Previous studies have documented risky behaviors, such as substance use, to be associated with disordered eating [27]; however, to the author's knowledge, our study is the first to evaluate such relationship among Florida adolescents using the YRBS, a standardized instrument and survey in the field. In addition, previous studies using the YRBS suggested that females on a national level were more likely than males to engage in unhealthy weight loss practices [28-30]. Our finding among Florida adolescents in 2011 was congruent with this national finding. In addition, gender difference with females more likely than males to engage in unhealthy weight loss practice was evident across all survey years (i.e., 2001 through 2011) in Florida [26]. This important gender-variation finding is relevant in implementing prevention and/or intervention efforts to reduce unhealthy weight loss practice among youth.
Our study adds to the literature by specifically examining unhealthy weight loss practices of adolescents in Florida, a statethat has reported an increase in prevalence of overweight and obese children since 2003.[4] Further, it investigates the role of specific co-occurring risk behaviors such as poor academic performance and the use of specific substances in unhealthy weight loss practice. Eiche et al. [27] examined the perception of weight and substance use on disordered eating and found that tobacco, cocaine, and alcohol use was predictive of disordered eating behavior. Our study examined the role of aforementioned substances with the addition of marijuana on the engagement of unhealthy weight loss practices. While the results were similar, the primary objective of our study was to examine actual weight and unhealthy weight loss practices rather than weight perception. Our findings contribute to the literature by adding to the evidence of weight status and the odds of engaging in unhealthy weight loss practice using actual weight status (i.e., CDC-defined age-sex specific BMI percentile). Previous studies among national youth evaluated the relationship between youth-perceived weight status and unhealthy weight loss practice. This is of significance since it suggests that both perceived and actual weight status contributed toward these unhealthy weight loss behavior and practice. Results from our study also showed that the prevalence of unhealthy weight loss practices were the highest among overweight and obese adolescents. The majority of overweight (69%) and obese (74%) adolescents reported "to lose weight" as the primary reason for the use of weight control measures. Of the unhealthy weight loss practices, fasting for > 24hours was the most prevalent method to lose weight in each weight status group (underweight, healthy weight, overweight, and obese). While a national trend analysis of YRBS data from 1999-2009 [31] indicated obese adolescents to be more likely than non-obese adolescents to engage in weight control methods, our study showed that Florida adolescents of various weight status groups were engaging in unhealthy weight loss methods.
While the prevalence of overweight and obese remained stable around 25% among Florida youth in the last decade (2001 through 2011), it should be noted that prevalence of unhealthy weight loss practice fluctuated during the same time. It should also be noted that the following findings were derived from a CDC data site [26] without formal statistical tests to compare between survey years. The proportions of fasting more than 24 hours had decreased steadily from 2001 (12.3%) to 2011 (9.6%) [26]. While the downward trend was noted for diet pill/powder/liquid use in general, its prevalence went up slightly from 2009 (5.1%) to 2011 (5.3%). Frequencies of vomiting or using laxatives fluctuated during the last decade with the highest frequency in 2007 (5.1%) and the lowest frequency in 2011 (4.1%) [26]. Future studies should examine the characteristic differences in the unhealthy weight loss methods used in conjunction with other health risk behaviors such as substance use and abuse in adolescents.
Some limitations of this study should be noted. First, temporal relationship between weight status and unhealthy weight loss practice cannot be determined due to the cross-sectional YRBS design. Second, perceived and actual weight status information were self-reported. The study's strengths are (1) the YRBS data were collected using a standardized and validated instrument; and (2) a probability sampling method was used to obtain a representative sample of Florida adolescents from high schools. The current study not only evaluated the unhealthy weight loss practice and behavior, but alsoassessed the co-existing health compromising behaviors such as cigarette, alcohol, and illegal drug use.
Conclusions
Overweight and obese adolescents are significantly more likely than their healthy weight counterparts to exhibit at least one unhealthy weight loss practice such as &ge 24 hours of fasting, diet pills use, and laxative use or purging. It has been suggested that adolescent overweight and obesity status is likely to continue into adulthood;[13,31-33] therefore, considering the current trends of obesity and associated negative health outcomes in adulthood, it is highly recommended that healthy weight management and weight loss practices be reinforced in adolescence.
References
- Minino AM. NCHS Data Brief: Death in the United States, 2011. 2013.
- Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of obesity among adults: United States, 2011-2012. NCHS Data Brief. 2013; 1-8.
- National Center for Health Statistics (NCHS). Health, United States, 2011: With Special Features on Socioeconomic Status and Health. 2012.
- Child Policy Research Center, National Initiative for Children's Healthcare Quality, Data Resource Center for Child and Adolescent Health. Florida State Fact Sheet. 2011.
- Freedman DS, Khan LK, Dietz WH, Srinivasan SR, Berenson GS. Relationship of childhood obesity to coronary heart disease risk factors in adulthood: the Bogalusa Heart Study. Pediatrics. 2001; 108: 712-718.
- Freedman DS, Dietz WH, Srinivasan SR, Berenson GS. Risk factors and adult body mass index among overweight children: the Bogalusa Heart Study. Pediatrics. 2009; 123: 750-757.
- Griffin ML, Weiss RD, Mirin SM, Lange U. A comparison of male and female cocaine abusers. Arch Gen Psychiatry. 1989; 46: 122-126.
- Sutherland ER. Obesity and asthma. Immunol Allergy Clin North Am. 2008; 28: 589-602.
- Centers for Disease Control and Prevention (CDC). Overweight and Obesity: Basics about Childhood Obesity. 2012.
- Centers for Disease Control and Prevention (CDC).Childhood obesity facts. 2013.
- Thomson Medstat Research. Childhood obesity: Costs, treatment patterns, disparities in care, and prevalent medical conditions. 2006.
- National Collaborative on Childhood Obesity Research. Childhood Obesity in the United States. 2009.
- Dietz WH. Health consequences of obesity in youth: childhood predictors of adult disease. Pediatrics. 1998; 101: 518-525.
- Hofmann B. Bariatric surgery for obese children and adolescents: a review of the moral challenges. BMC Med Ethics. 2013; 14: 18.
- Ibele AR, Mattar SG. Adolescent bariatric surgery. Surg Clin North Am. 2011; 91: 1339-1351.
- Martinsen M, Sundgot-Borgen J. Higher prevalence of eating disorders among adolescent elite athletes than controls. Med Sci Sports Exerc. 2013; 45: 1188-1197.
- Rohde P, Stice E, Marti CN. Development and predictive effects of eating disorder risk factors during adolescence: Implications for prevention efforts. Int J Eat Disord. 2014.
- Patton GC, Selzer R, Coffey C, Carlin JB, Wolfe R. Onset of adolescent eating disorders: population based cohort study over 3 years. BMJ. 1999; 318: 765-768.
- Haines J, Kleinman KP, Rifas-Shiman SL, Field AE, Austin SB. Examination of shared risk and protective factors for overweight and disordered eating among adolescents. Arch Pediatr Adolesc Med. 2010; 164: 336-343.
- Arcelus J, Mitchell AJ, Wales J, Nielsen S. Mortality rates in patients with anorexia nervosa and other eating disorders. A meta-analysis of 36 studies. Arch Gen Psychiatry. 2011; 68: 724-731.
- Centers for Disease Control and Prevention (CDC).A Guide to Conducting Your Own Youth Risk Behavior Survey. 2012.
- Brener ND, Kann L, Shanklin S, Kichen S, Eaton DK, Hawkins J, et al. Methodology of the Youth Risk Behavior Surveillance System. Morbidity and Mortality Weekly Report. 2013; 62: 1-23.
- Eaton DK, Kann D, Kinchen S, Shanklin S, Flint KH, Hawkins J, et al. Youth Risk Behavior Surveillance- United States 2011. Morbidity and Mortality Weekly Report. 2012; 61: 1-162.
- Centers for Disease Control and Prevention (CDC). 2011 State and Local Youth Risk Behavior Survey. 2011.
- Centers for Disease Control and Prevention (CDC). About BMI for Children and Teens. 2011.
- Centers for Disease Control and Prevention (CDC). Youth Online: High School YRBS. Florida 2005 Results.
- Eichen DM, Conner BT, Daly BP, Fauber RL. Weight perception, substance use, and disordered eating behaviors: comparing normal weight and overweight high-school students. J Youth Adolesc. 2012; 41: 1-13.
- Forman-Hoffman V. High prevalence of abnormal eating and weight control practices among U.S. high-school students. Eat Behav. 2004; 5: 325-336.
- Lampard AM, Maclehose RF, Eisenberg ME, Neumark-Sztainer D, Davison KK. Weight-Related Teasing in the School Environment: Associations with Psychosocial Health and Weight Control Practices among Adolescent Boys and Girls. 2014 [in Press].
- Gonsalves D, Hawk H, Goodenow C. Unhealthy Weight Control Behaviors and Related Risk Factors in Massachusetts Middle and High School Students. Matern Child Health J. 2013.
- Demissie Z, Lowry R, Eaton DK, Nihiser AJ. Trends in Weight Management Goals and Behaviors Among 9th-12th Grade Students: United States, 1999-2009. Matern Child Health J. 2014.
- Freedman DS, Khan LK, Dietz WH, Srinivasan SR, Berenson GS. Relationship of childhood obesity to coronary heart disease risk factors in adulthood: the Bogalusa Heart Study. Pediatrics. 2001; 108: 712-718.
- Freedman DS, Khan LK, Serdula MK, Dietz WH, Srinivasan SR, Berenson GS, et al. Inter-relationships among childhood BMI, childhood height, and adult obesity: the Bogalusa Heart Study. Int J Obes Relat Metab Disord. 2004; 28: 10-16.