
Research Article
Austin J Public Health Epidemiol. 2015; 2(3): 1026.
Hospital Characteristics and their Impact on Value-Based Purchasing
Haley DR*, Zhao M, Spaulding A and Hamadi H
Department of Public Health and Health Administration Programs, University of North Florida, USA
*Corresponding author: Haley DR, Department of Public Health and Health Administration Programs, University of North Florida, 1 UNF Drive, Jacksonville, Florida, USA
Received: September 25, 2015; Accepted: November 11, 2015; Published: November 20, 2015
Abstract
As part of the inpatient Hospital Value-Based Purchasing (HVBP) program, CMS implemented a new Total Performance Score (TPS) methodology to assess and financially reward hospitals for providing affordable, quality health care. In FY 2015, the Efficiency domain was added to the measure of the cost of care by individual hospitals. We used the Diffusion of Innovation (DOI) Theory as a conceptual model for our study. We also used data from the 2015 American Hospital Association (AHA) database and the 2015 Hospital Compare database. Multivariate regression analysis was used to examine the relationship between TPS, hospital characteristics and the new TPS methodology using SPSS, version 19. We found that for-profit, non-teaching, smaller and rural hospitals had significantly higher overall TPS, Process of Care, Patient Experience and Efficiency scores. The results suggest that hospital characteristics may have an important impact on value-based purchasing pay-for-performance results and their associated funding.
Keywords: Value based purchasing; Hospital characteristics; Medicare; Affordable care act; Health care reform; Quality
Introduction
The Patient Protection and Affordable Care Act of 2010 (ACA) created an inpatient Hospital Value-Based Purchasing (HVBP) program as an effort to achieve better health, better quality of care, and lower costs of providing care [1]. The HVBP concept imposes a financial-penalty for hospitals that do not meet specific process, outcome, and patient experience performance standards for Medicare beneficiaries. As part of this program, CMS implemented a new Total Performance Score (TPS) methodology to assess and financially reward hospitals for providing affordable, quality health care. In FY 2015, the following weighted domains were utilized to determine the TPS value: 1) Clinical Process of Care, 2) Patient Experience of Care, 3) Outcome, and 4) Efficiency Domains [2].
The Clinical Process of Care domain includes 12 clinical process measures that account for 20% of the TPS. The Patient Experience of Care domain is derived from the Hospital Consumer Assessment of Health care Providers and Systems (HCAHPS) survey and accounts for 30% of the TPS. Finally, the Outcome domain accounts for 30% of the TPS. This domain includes one Agency for Health care Quality and Research (AHQR) Patient Safety Measure (PSI-90 – Patient safety for selected indicators (composite)), one health care associated infections measure (CLABSI-central line-associated bloodstream infection) and three mortality outcomes: Acute Myocardial Infarction (AMI), Heart Failure (HF), and Pneumonia (PN) [3]. Mortality is defined as death within 30 days of operation or before hospital discharge [4].
The Efficiency domain was added in FY 2015 and measures the cost of care by each individual hospital. This domain is an important addition to the TPS methodology because it provides consumer transparency in health care. For the first time, it allows consumers to compare hospitals and identify ones that provide higher quality care at lower costs [5]. Furthermore, the Efficiency domain accounts for a sizeable 20% of a hospital’s TPS. In an effort to improve patient care and maximize reimbursement from CMS, it is important for policy makers and hospital administrators to understand factors that influence the new Efficiency domain which in turn influences the new TPS scoring for FY 2015. While there is a history of studies that examine hospital characteristics and the quality of care, there is a lack of research on the relationship between hospital characteristics and TPS and no research on hospital characteristics and its relationship to the new FY 2015 TPS methodology.
Some studies have found that certain characteristics such as hospital ownership, bed-size and location influence hospital quality [6-8]. For example, one study of 2,491 U.S. acute care hospitals eligible for the VBP program found that hospital ownership and geographic region had an influence on an earlier version of CMS’ HVBP methodology [9]. However, the relationship between hospital characteristics and transparency continues to be lacking [10-12]. Therefore, this research is important because it will provide new insight into CMS’s new FY 2015 HVBP methodology and their relationship to hospital characteristics.
Conceptual model
As the health care environment changes toward pay-forperformance and greater transparency, CMS seeks to accelerate the diffusion of change for all hospitals across the United States, through the VBP arrangement. However, some hospitals appear to be early adopters of change while other hospitals continue to struggle in this rapidly changing health care environment. The Diffusion of Innovation (DOI) Theory was developed by E.M. Rogers in 1962 and is one of the oldest social science theories. It has been further refined from a study of propositions that were synthesized from more than 1,500 publications pertaining to the communication of innovations [13,14]. This Theory indicates that over time, an idea will gain momentum and diffuse through a specific population or social system. Ultimately, this diffusion should result in the adoption of a new idea, behavior, or product. Adoption means that something is done differently as a result of the new knowledge gained from the diffusion because there is a perception that the idea, behavior, or product is new or innovative [14].
It is believed that there are factors that can positively or negatively influence the speed of diffusion within an organization. For example, it is believed that hospitals that lack the capital to implement new and effective process improvement technology, training and education will have a slower diffusion of innovation than hospitals that have access to capital [15].
H1: For-profit hospitals will have higher TPS, Process of Care, Patient Experience and Efficiency scores compared to not-for-profit hospitals because for-profit hospitals have the capital to more readily invest in innovative and more effective process measures.
Organizational size may also influence the diffusion and innovation process. A meta-analysis of 21 empirical studies found that organizational size, as defined by workforce size, has a profound impact on IT innovation adoption [16]. This study found that IT innovation adoption was actually slower in smaller organizations because of their lack of capital to invest in information technology. However, it is hypothesized that smaller hospitals can more quickly diffuse and implement more innovative and effective process standards across their organization compared to the lag of diffusion within larger system-owned hospitals [17]. It is also believed that smaller and rural hospitals may have a closer relationship with the population with its medical service area which may cause higher consumer satisfaction.
H2: Smaller and rural hospitals will have a higher TPS, Process of Care, Patient Experience and Efficiency scores compared to systemowned hospitals where diffusion may experience an organizational lag.
Organizational purpose may also influence the speed of innovation diffusion. Hospitals which are focused at least in part, to teaching are more likely to adopt cutting edge technologies, and adopt process related to improved quality of care provided. As such, we expect that teaching status plays a strong role in whether or not the hospitals has adopted the innovation [18,19].
H3: Teaching hospitals will have a culture that will facilitate innovation and diffusion resulting in higher TPS, Process of Care, Patient Experience and Efficiency scores.
Materials and Methods
Data sources
The 2015 American Hospital Association (AHA) database and the 2015 Hospital Compare on Hospital Value-Based Purchasing (HVBP) –Total Performance Score (TPS) database through CMS were merged together to conduct this analysis. The AHA database includes information on hospital characteristics and services from over 6,000 hospitals in the United States. The Hospital Compare on HVBP–TPS contains the weighted and unweighted scores of Clinical Process of Care, Patient Experience of Care, Outcome, Efficiency, and the TPS of participating hospitals.
Variables and measures
The dependent variables for this study are the weighted four domain scores and TPS that come from the Hospital Compare database HVBP–TPS. The four domains consist of: the Process of Care Domain, the Patient Experience of Care Domain, the Outcome Domain, and the Efficiency Domain. The Total Performance Score is a weighted combination of the four domains where the Process of Care Domain is 20% of the total, Patient Experience of Care is 30%, the Outcome Domain is 30%, and the Efficiency Domain is 20% [2]. The independent variables for this study include the following hospital characteristics: hospital ownership (government owned non-federal, private not-for-profit, for-profit), hospital size (small, medium, large), system status (system vs. non-system), location (rural vs. urban), teaching status (major teaching, minor teaching, and non-teaching).
Hospital ownership status, defined as government (non-federal), not-for-profit, and for-profit, may reflect different objectives, resource allocation, and ultimate quality of care. Hospital size, defined as the number of staffed hospital beds, was separated into three categories: small, medium, and large. Hospitals with fewer than 100 beds are defined as small hospitals, hospitals with 500 beds and more beds are defined as large hospitals, and the hospitals in between are medium size. Hospital system means that a hospital belongs to a multihospital system. In addition, Hospital located in rural areas, as opposed to urban ones, may not have enough resources to provide high quality of care. Finally, teaching hospitals usually treat patients with more complex medical problems and may incur different quality compared to non-teaching facilities. Major teaching hospitals refer to hospitals that belong to members of the Council of Teaching Hospitals (COTH); minor teaching hospitals are hospitals that have approved residency programs.
Analysis
Both descriptive statistics and bivariate analysis are conducted for the study. All analyses were performed in SPSS, version 19.
Findings
Table 1 shows the descriptive statistics for all of the study variables used in this study. For the 3,074 hospitals within the dataset, the mean TPS was 41.72. The mean weighted scores for Process of Care, Patient Experience of Care, Outcome, and Efficiency were 11.71, 13.73, 13.75, and 4.64 respectively. In this sample, approximately 14% of the hospitals were government owned, 63% were not-for-profit, and 23% were for-profit. Among these hospitals, about 30% were small hospitals, 56% medium size hospitals, and 15% were large size hospitals. Sixty-seven percent of hospitals in the sample belonged to a hospital system. Approximately 27% of the hospitals are located in rural areas. Regarding teaching status, about 8% were major teaching hospitals that belong to the COTH, 26% were minor teaching hospitals that had approved residency programs, and the remaining 66% were non-teaching hospitals (Table 1).
Quality Scores
Frequency or Mean
Pop
Percent
Total Performance Score
41.72
3074
Process of Care Domain (weighted)
11.71
2950
Experience of Care Domain (weighted)
13.73
3042
Outcome of Care Domain (weighted)
13.75
2745
Efficiency of Care Domain (weighted)
4.64
3063
Hospital Characteristics Variables
Ownership
Government (Non-Federal)
428
3009
14%
Not-For-Profit
1884
3009
63%
For-Profit
697
3009
23%
Size
Small
894
3009
30%
Medium
1676
3009
56%
Large
439
3009
15%
System
Yes
2021
3009
67%
No
988
3009
33%
Location
Rural
818
3009
27%
Urban
2191
3009
73%
Teaching Status
Major Teaching Hospital
243
3009
8%
Minor Teaching Hospital
783
3009
26%
Non-teaching Hospital
1983
3009
66%
Table 1: Descriptive characteristics.
Figure 1 displays the relationship between hospital ownership and performance scores. For-profit hospitals had higher TPS, Process of Care scores, and Patient Experience scores. However, compared to other hospitals, for-profit hospitals had a lower Efficiency score. No significant difference was found regarding Outcome scores (Figure 1).
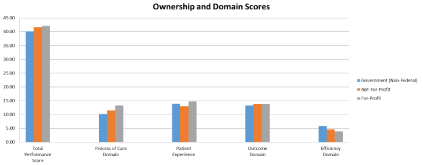
Figure 1: The Effect of Ownership on Hospital Performance.
Figure 2 displays the effects of hospital bed size on performance. Small hospitals had higher TPS, Process of Care, Patient Experience, Outcome, and Efficiency scores compared to medium and large hospitals. However, the difference for Process of Care and Outcome scores was found to be marginal (Figure 2).
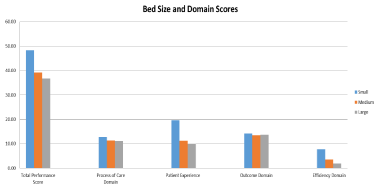
Figure 2: The Effect of Bed Size on Hospital Performance.
Figure 3 shows the correlation between hospital system status and hospital performance. Compared with non-system owned hospitals, system- owned hospitals had lower TPS, Experience of Care, and Efficiency scores. However, system-owned hospitals had higher Process of Care scores. No significant difference was identified in terms of Outcome Domain scores (Figure 3).
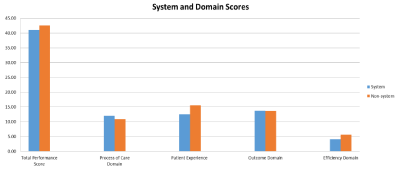
Figure 3: The Effect of System on Hospital Performance.
Figure 4 indicates the effect of location on hospital performance. Compared with urban hospitals, rural hospitals had higher scores for TPS, Patient Experience, and Efficiency Domains. However, rural hospitals had lower scores in Process of Care. There was no significant difference regarding Outcome Domain scores (Figure 4).
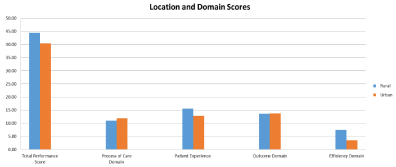
Figure 4: The Effect of Location on Hospital Performance.
Figure 5 presents the effect of teaching status on hospital performance. Compared to major teaching hospitals and minor teaching hospitals, non-teaching hospitals had significantly higher scores in all four Domains and the TPS (Figure 5).
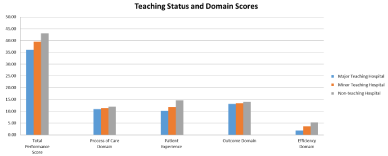
Figure 5: The Effect of Teaching Status on Hospital Performance.
Discussion
This analysis provides insight into the new FY 2015 CMS TPS methodology. Specifically, our research supports our hypothesis that for-profit hospitals have significantly higher TPS, Process of Care, Patient Experience and Efficiency scores compared to notfor- profit hospitals. Not-for-profit hospitals may rely more heavily on investment income to boost profit margins and may have difficulty investing during volatile times [20]. Therefore, the recent and prolonged volatility of the financial market may have decreased the availability of capital for not-for-profit hospitals to invest in the acceleration of training and technology innovations to quickly improve TPS and its domains.
Consistent with other studies [21], our study found that hospital size does matter in terms of diffusion and Efficiency. Specifically, our study supported our hypothesis that smaller and rural hospitals had significantly higher TPS, Process of Care, Patient Experience and Efficiency scores compared to system-owned hospitals. Smaller and rural hospitals may have a better relationship with their community since the medical service area population is typically smaller. In addition, the smaller and rural hospital’s workforce typically comprises residents of the smaller medical service area resulting in a more personal view of the hospital. Therefore, patients may perceive a more positive Patient Experience compared to larger hospitals. In addition, smaller and rural hospitals may be able to more easily and rapidly diffuse new process-of-care innovations across the hospital due to its smaller size.
Finally, our hypothesis that teaching hospitals would have significantly higher TPS, Process of Care, Patient Experience and Efficiency scores was not supported by this research. This was surprising because it is believed that teaching hospitals would value innovation more and therefore would more quickly diffuse innovations across the hospital. While the results are surprising, there may important factors that negatively influence the diffusion process within teaching hospitals compared to non-teaching hospitals. For example, teaching hospitals are typically larger than community hospitals and hospital size was found to influence the diffusion of innovation. In addition, teaching hospitals often care for disadvantaged and higher risk populations. These populations may negatively impact some or all of the domains of TPS.
Limitations and future research
This research uses data from multiple databases to provide new insight into CMS’s new FY 2015 HVBP methodology and their relationship to hospital characteristics. However, since this research uses a cross-sectional analysis methodology we cannot determine trend or the effect other initiatives may be having on hospitals pursuit of VBP scores. A longitudinal study should be used for future studies to better measure the diffusion of the VBP Domains over time. In addition, while descriptive and bivariate analyses were conducted in this study, multivariate analysis should be used for future studies to control for potential confounders. Finally, future studies should consider including other variables such as market competition to provide additional and a more robust analysis.
Policy implications
Despite these limitations, this study provides important insight into the relationship between specific hospital characteristics and the domains of CMS’ new FY 2015 TPS methodology. The results demonstrate that for-profit, non-teaching, smaller and rural hospitals had significantly higher overall TPS and TPS domain scores. The results suggest that hospital characteristics may have an important impact on value-based-purchasing, pay-for-performance results and their associated funding.
This research is important because it helps hospital administrators understand hospital characteristics and their impact on valuebased purchasing. Administrators can more effectively target organizational policies to improve care and bolster TPS, Process of Care, Patient Experience, Outcome and Efficiency Domains in addition to maximizing reimbursement under the emerging pay-forperformance methodologies.
Furthermore, the findings presented in this study offer important implications for policymakers. Given that the United States health care system will continue to focus on improved quality as a result of market forces and the ACA, those trying to improve hospital quality and patient safety should consider a combination of characteristic hospital elements. Accordingly, CMS may want to revisit the Clinical Process of Care Measures, Patient Experience of Care Dimensions, Outcome, and Efficiency Domains that comprise hospital TPS in order to include hospital characteristics and thereby gain a more robust indication of hospital quality.
References
- Vanlare JM, Conway PH. Value-based purchasing-national programs to move from volume to value. New England Journal of Medicine. 2012; 367: 292-295.
- CMS. Hospital Value-Based Purchasing. 2015.
- CMS. Hospital Value-Based Purchasing. In: CMS editor. 2015.
- Dimick JB, Staiger DO, Birkmeyer JD. Ranking hospitals on surgical mortality: the importance of reliability adjustment. Health services research. 2010; 45: 1614-1629.
- Zhao M, Haley DR, Spaulding A, Balogh HA. Value-Based Purchasing, Efficiency, and Hospital Performance. The health care manager. 2015; 34: 4-13.
- Keeler EB, Rubenstein LV, Kahn KL, Draper D, Harrison ER, McGinty MJ, et al. Hospital characteristics and quality of care. Jama. 1992; 268: 1709-1714.
- Dimick JB, Welch HG, Birkmeyer JD. Surgical mortality as an indicator of hospital quality: the problem with small sample size. Jama. 2004; 292: 847-851.
- Ayanian JZ, Weissman JS. Teaching hospitals and quality of care: a review of the literature. Milbank Quarterly. 2002; 80: 569-593.
- Borah BJ, Rock MG, Wood DL, Roellinger DL, Johnson MG, Naessens JM. Association between value-based purchasing score and hospital characteristics. BMC health services research. 2012; 12: 464.
- Hibbard JH, Stockard J, Tusler M. Does publicizing hospital performance stimulate quality improvement efforts? Health Affairs. 2003; 22: 84-94.
- Sinaiko AD, Rosenthal MB. Increased price transparency in health care–challenges and potential effects. New England Journal of Medicine. 2011; 364: 891-894.
- Fung CH, Lim Y-W, Mattke S, Damberg C, Shekelle PG. Systematic review: the evidence that publishing patient care performance data improves quality of care. Annals of internal medicine. 2008; 148: 111-123.
- Rogers EM, Havens AE. Predicting Innovativeness. Sociological Inquiry. 1962; 32: 34-42.
- Rogers EM, Shoemaker FF. Communication of Innovations; A Cross-Cultural Approach. 1971.
- Brown CE, Wickline MA, Ecoff L, Glaser D. Nursing practice, knowledge, attitudes and perceived barriers to evidence-based practice at an academic medical center. Journal of advanced nursing. 2009; 65: 371-381.
- Lee G, Xia W. Organizational size and IT innovation adoption: A meta-analysis. Information & Management. 2006; 43: 975-985.
- Damanpour F, Evan WM. Organizational innovation and performance: the problem of" organizational lag". Administrative science quarterly. 1984: 392-409.
- Furukawa MF, Raghu T, Spaulding TJ, Vinze A. Adoption of health information technology for medication safety in US hospitals, 2006. Health Affairs. 2008; 27: 865-875.
- Kupersmith J. Quality of care in teaching hospitals: a literature review. Academic Medicine. 2005; 80: 458-66.
- Song PH, Smith DG, Wheeler JR. It was the best of times; it was the worst of times: A tale of two years in not-for-profit hospital financial investments. Health Care Management Review. 2008; 33: 234-242.
- Coyne JS, Richards MT, Short R, Shultz K, Singh SG. Hospital cost and efficiency: do hospital size and ownership type really matter? Journal of Healthcare Management. 2009; 54: 163.