
Review Article
Austin J Public Health Epidemiol. 2016; 3(3): 1038.
Impact of Migration on Non Communicable Disease Risk Factors: Comparison of Gulf Migrants and their Non Migrant Contemporaries in the District of Origin in Kerala, India
Begam NS* and Mini GK
Department of Public Health and Epidemiology, Sree Chitra Tirunal Institute for Medical Sciences and Technology (SCTIMST), Kerala
*Corresponding author: Shamim Begam N, Department of Public Health and Epidemiology, Sree Chitra Tirunal Institute for Medical Sciences and Technology (SCTIMST), Achutha Menon Centre for Health Science Studies (AMCHSS), Trivandrum, Kerala 695011, India
Received: March 29, 2016; Accepted: April 28, 2016; Published: May 02, 2016
Abstract
Introduction: We assessed the prevalence of Non-Communicable Disease (NCD) risk factors between gulf migrant workers and non-migrant workers of Malappuram district, Kerala.
Methods: Using a multistage cluster sampling technique, 191 migrant and 193 non-migrant men between 25-65 years of age were selected. Data on NCD risk factors were collected using World Health Organization (WHO) steps protocol. Multivariate analysis was used to find the relation between migration and NCD risk factors.
Results: Prevalence of current tobacco use was 21.4% among migrants and 16.6% among non migrants, current alcohol use was 8.9% among migrants and 12.4% among non migrants, physical inactivity was 26.7% among migrants and 23.8% among non migrants, poor diet habit was 86.9% among migrants and 76.2% among non migrants, history of chronic diseases was 37.5% among migrants and 21% among non migrants, working 7 days /week was 35% among migrants and 1% among non migrants, working >8hrs/day was 76.9% among migrants and 33.1% among non migrants, sleeping less than 6hrs / day was 41.3% among migrants and 14% among non migrants. Prevalence of hypertension was 59.7% among migrants and 29.8% among non migrants (p= <0.001) (adjusted or 2.5, 95% CI=1.38-4.46), abdominal obesity was 79.5% among migrants and 44.5% among non migrants (p= <0.001) (adjusted or 2.4, 95% CI=1.35-4.31). Among migrant hypertensive 43.5% were aware, 33.9% were on treatment and 12.2% achieved adequate control, the corresponding figures for non migrants were 56.9%, 53.4%, and 48.3% respectively.
Conclusion: Majority of the risk factors were significantly higher among gulf migrants than non-migrants, which calls for urgent intervention to reduce these risk factors in this population.
Keywords: Migrant workers; Non communicable diseases; Risk factors; Malappuram; Kerala; India
Introduction
The high incidence of Non Communicable Diseases (NCDs) and its risk factors is very much related to growing changes to unhealthy life styles, ageing and rapid urbanization [1,2]. Each of these risk factor increases the risk for NCDs through independent mechanisms [3]. In spite of being related to each other the occurrence of one risk factor makes way for another leading to greater risk for developing NCDs [4]. It has been evident that the major risk factors associated with NCDs are tobacco use, harmful alcohol intake, unhealthy diet (low fruits and vegetable consumption) and low physical activity. These are well modifiable through life style changes and primary prevention methods giving a greatest impact on reducing NCD mortality and morbidity [5,6]. Prevention, early detection and management of these risk factors would be an effective option in controlling these NCD and to reduce the disease burden [7]. The global risk report states that threat of chronic NCDs is rated above the current global financial crisis and the probable cost has been estimated from $250 billion to $1 trillion [8]. Studies suggest that despite repeat calls for action, the NCD burden is increasing and remaining unattended in developing countries [9]. World health Organization has declared NCDs as a growing threat globally especially in developing countries [10]. NCDs are responsible for maximum number of deaths in working age group globally affecting more of younger age group in poor countries than in the rich countries [11]. Migration is an important, current global issue that affects health in complex ways and has been proved as an important factor in developing NCDs and its risk factors [12]. Globally there is an acceleration of international migration at 2.9 % of annual growth rate and differentiation of migration with different types of migration like labour migration, asylum seekers and refugees. These factors increase the complexity of the situation calling for an immediate attention of the concerned authorities [12]. Research findings in countries of origin of key migrant categories in the affluent countries confirms the high and growing prevalence of NCDs such as Cardiovascular Diseases (CVD), diabetes and it’s risk factors [13]. Chronic anxiety, homesickness and isolation are leading to stress related health issues among migrants. Migrants are not addressed well in health studies, and their health issues remain mostly unreported [12,13].
For the last four decades, workers from the Indian subcontinent are migrating to Arabian Gulf as a result of poverty, perceived wage differences and constant demand for cheap labour [14]. Kerala state reported the highest flow of labour migration from the country until recently. Gulf countries accounts for 96% of the total international migrants from Kerala [14]. About 95% of gulf migrants from Kerala are males. Very little attention has been given to the adaptation and survival of migrants in the host country and associated health impacts [14,15]. Studies conducted in United States (US) and Europe among the migrant Indians show high prevalence of NCDs and their risk factors compared to the native population [16-19].
A comparative study done between migrant and non migrant Gujarat is reports that the NCD risk factors such as high Body Mass Index (BMI), blood pressure, lipids, non-esterified fatty acids, and high calorie diet were high among migrants [16]. A study done on migrant Asian Indians living in the United Kingdom (UK) found higher levels of obesity, blood pressure, total cholesterol, blood glucose, and insulin resistance higher than their siblings in Punjab [17]. Indian immigrants were found to have high incidence of overweight, with minimal exercise and activity profiles while in the host country as per studies in the US [18]. High prevalence of adverse body fat patterning, dyslipidaemia and insulin resistance beginning at a young age have been consistently reported in Asian Indians irrespective of their geographic locations [19]. Along with the ethnic predisposition, lifestyle changes after migration resulted in an early onset and high prevalence rates of diabetes and metabolic syndrome among Asian Indians in United States [20].
Considering the high vulnerability to the non communicable disease risk factors due to the forced adaptation to the lifestyles, living and working environments of the host country, it is significant to explore a comparative study on the NCD risk factors and its determinants among migrants and non migrants. The present study compares the prevalence of NCD risk factors among gulf migrant workers and non migrant workers of Malappuram district in Kerala, India.
Methodology
The study was done in Malappuram district which is one of the districts with high gulf migrant population in Kerala State [14]. Since majority of migrants were men, for the present study women were not included [14]. This was a community based cross sectional study among adult men aged 25-64 years. Using a multi stage cluster sampling method- Among the 15 block panchayats of Malappuram district, Tanur was randomly selected. Out of the total nine gramapanchayats of Tanur Block, four were randomly selected [21]. In the third stage, five wards (the ward is the smallest geographical unit of the decentralized government in Kerala) were randomly selected from the selected panchayats as the study area. Two clusters of 10 individuals each were identified for both gulf migrant workers and non-migrant workers from each of these selected wards. The first household was selected randomly and remaining was continuously surveyed. For all the clusters the same process was repeated (Figure 1). The study was conducted during July to September 2013 which was the vacation time in gulf countries because of the Ramadan festival. Most of the gulf migrant workers had come on vacation which helped us to obtain the gulf migrants easier.
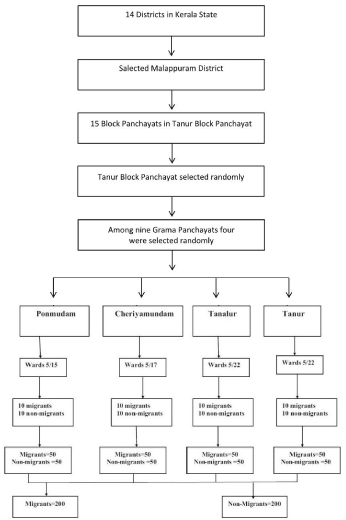
Figure 1: Schematic Representation of sample selection.
Gulf migrant workers included individuals, who were permanent residents of Malappuram district, non-resident Keralites worked in gulf countries (gulf countries in this study included United Arab Emirates (UAE), Kingdom of Saudi Arabia (KSA), Qatar, Oman, Kuwait and Bahrain) for a minimum of five years and those who had returned from gulf within one month prior to the survey (Figure 2). Non migrant workers were individuals who were permanent residents of Malappuram district (residing in the district for a minimum of last five years) and those who had never worked outside Kerala.
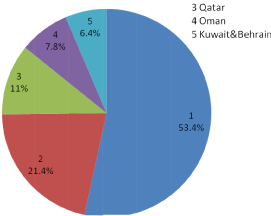
Figure 2: Working country based distribution of gulf migrant workers.
Since there is no literature available on the prevalence of NCD risk factors among gulf migrants in these areas, we conducted a pilot study on hypertension among gulf migrant workers and nonmigrant workers in the selected district and found to be 30% and 53% respectively. Considering the alpha error at 5% with 80% power, design effect of 2 and considering the non-response rate of 20%, the sample size was calculated as 384. Thus we approached 400 samples (200 migrants and 200 non migrants) for the study. The response rate was 95.5 % among migrants and 96.5 % among non migrants. Finally we analyzed a total of 384 samples (191 migrants and 193 non migrants).
Using WHO steps questionnaire for Non-Communicable Disease (NCD) risk factor surveillance we collected step 1 and step 2 variables [22]. The English questionnaire was translated into Malayalam (local language) and back translated to English by independent translators. Anthropometric measurements (step 2) like height, weight, waist circumference and Blood Pressure (BP) were measured. Blood Pressure was measured using a calibrated automatic BP apparatus (OMRON -4, Omron Corporation, Kyoto, Japan). Height, weight and waist-circumference were measured using Stadiometer, SECA weighing machine and SECA constant tension tape respectively. All the measurements were taken according to the WHO STEPS protocol [22]. Details on self reported diabetes and family history of NCD were also collected. All the participants for the study were interviewed at their homes by trained field workers under the supervision of the first author (SB).
Statistical Analysis
The data was analyzed using SPSS software version 17.0 (SPSS Inc, Chicago, IL). Descriptive analysis was done to study the sample characteristics and to compare the prevalence of risk factors in both gulf migrants and non-migrants. Statistical significance was fixed at P value <0.05. The NCD risk factors was compared between migrant and non-migrants using Student’s t-test, Chi-square test, univariate and multivariate logistic regression modeling were performed for finding out the predictors of hypertension and abdominal obesity prevalence.
Definitions used
Physical activity calculated using the Metabolic Equivalents (MET) min/week and classified in to High (>3000 MET Minutes/ week), moderate (600 to 2999 MET Minutes/week) and low (<600 MET Minutes/week). Abdominal obesity was defined as waist circumference >90 cms in men, overweight was defined as BMI >25 Kg/m2 and obesity as >30 Kg/m2 [22]. Current tobacco users were those who used any form of tobacco in the last 30 days, alcohol users were those who consumed at least one standard drink of alcohol in last 12 months, diet with less than five servings (400 gms) of fruits and vegetables per day were considered as low fruit and vegetable intake [23]. Hypertension was defined as systolic blood pressure =140 mm of Hg or diastolic blood pressure =90 mm of Hg and or on medication for hypertension according to JNC VII criteria [24].
Ethical clearance
Ethical clearance for the study was obtained from the institute ethics committee of the Sree Chitra Tirunal Institute for Medical Sciences and Technology, Trivandrum. All participants gave written informed consent.
Results
The basic characteristics of migrants and non migrants are presented in (Table 1). Distribution of migrants in the working countries is depicted in (Figure 2). History of non communicable diseases like cardio vascular diseases, chronic respiratory diseases, cancers and diabetes were significantly higher among migrants compared to non-migrants. There was no significant difference between parental history of NCD among migrants (56.6%) and non migrants (50.3%). Prolonged working hours, availing no holidays and lack of adequate sleep was significant among migrants; details are presented in (Table 2). Prevalence of step 1 and step 2 variables are presented in (Table 3). Prevalence of hypertension, overweight and abdominal obesity with duration of gulf migration, is depicted in (Figure 3).
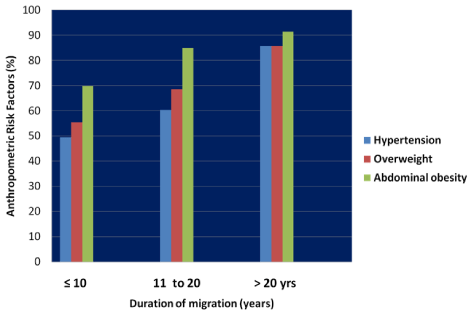
Figure 3: Changes in Anthroprometric Risk Factors with duration of Migration.
Variable
Migrant
N=191
n (%)
Non-migrant
N=193
n (%)
Total
N=384
n (%)
P value
Age groups (years)
< 35
35-44
45-54
55-64
43 (25.5)
70 (36.6)
61 (31.9)
17 (8.9)
70 (36.3)
65 (33.7)
29 (15.0)
29 (15.0)
113 (29.4)
135 (35.2)
90 (23.4)
46 (12.0)
< 0.05
Religion
Muslims
Others
150 (78.4)
41 (21.6)
125 (64.7)
68 (35.3)
275 (71.6)
109 (28.4)
< 0.05
Marital status
Currently Married
Others
177 (92.7)
14 (7.3)
167 (86.5)
26(13.5)
344 (89.6)
40 (10.4)
0.490
Education
high school level
higher secondary level
university educated
106 (55.5)
46 (24.1)
39 (20.4)
112 (58.1)
35 (18.1)
46 (23.8)
218 (56.7)
81 (21.1)
85 (22.2)
0.329
Occupation
Unskilled
Semiskilled
Professionals
Others
89 (46.5)
61(32.0)
19 (10.0)
22 (11.5)
82 (42.5)
63 (32.6)
21 (10.9)
27 (14.0)
171 (44.6)
124 (32.3)
40 (10.4)
49 (12.7)
0.821
Table 1: Basic characteristics of the study sample.
Variable
Migrant N=191 n (%)
Non-migrant N=193 n (%)
Total N=384 n (%)
P value
No of working days on a
typical week Working All 7 days
67 (35.0)
2 (1.0)
69 (18.0)
< 0.001
No of working hours on
a typical day Working> 8 hrs
147 (77.0)
64 (33.0)
211 (55.0)
< 0.001
No of sleeping hours� on
a typical day Sleeping<6 hrs
79 (41.4)
27 (14.0)
106 (27.6)
< 0.001
Table 2: Working and sleeping duration.
Variables
Migrants
N=191
Non-migrants
N=193
Total
N=383
P value
Current tobacco use1
41(21.4)
32(16.6)
73(19.0)
0.222
Passive smoking2
88 (46.1)
38 (19.7)
126 (32.8)
<0.001
Current alcohol use3
17(8.9)
24(12.4)
41(10.7)
0.262
Low fruits and vegetable intake4
166(86.9)
147(76.2)
313(81.5)
<0.05
Physical activity
Low5
Moderate6
High7
51(26.7)
64(33.5)
76(39.8)
46(23.8)
75(38.9)
72(37.3)
93(25.3)
139(36.2)
148(38.5)
0.542
Abdominal obesity8
152(79.6)
86(44.6)
238(62.0)
<0.001
Overweight9
126(65.9)
89(46.1)
215(55.9)
<0.001
Hypertension10
115(60.2)
58(30.0)
173(45.0)
<0.001
Diabetes11
73(38.2)
37(19.2)
110(28.6)
<0.001
1Use of any form of tobacco within last one month, 2Exposed to second hand smoke within last one month 3Consumed alcohol in the last months, 4Less than five servings of fruits and vegetables per day, 5<600MET minutes/week, 6600-2999 MET minutes per week, 7>=3000 MET minutes per week, 8Waist circumference >=90 cms, 9BMI >=25 kg/m2, 10Systolic BP >=140 or Diastolic BP>=90 or on medication for hypertension, 11Self reported.
Table 3: Prevalence of NCD risk factors among migrants and non-migrants.
Uni-variate and multi-variate logistic regressions were attempted taking hypertension and abdominal obesity as outcome variables. Migrants were found 3 times more likely to be hypertensive and 2.5 times more likely to have abdominal obesity compared to non migrants after adjusting for other common variables; this is presented in (Table 4).
Variables
Hypertension Adjusted Odds ratio (95% CI)
Abdominal Obesity� Adjusted Odds ratio� (95% CI)
Migration
No
Reference
Reference
Yes
2.84 (1.83-4.94)*
2.51(1.35-4.31)*
Age (in years)
= 40
Reference
Reference
>40
2.47(1.50-4.07)*
2.47(1.50-4.07)*
Working hours on a typical day
= 8hrs
NA
Reference
> 8hrs
2.03(1.21-3.40)*
Hypertension
No
NA
Reference
Yes
1.73(1.02-2.98)*
Diabetes1
No
Reference
Reference
Yes
1.97(1.12-3.40)*
1.76 (0.95-3.32)*
*P<0.05 , NA= Not applicable , 1Self-reported , Other variables considered in the model are monthly income, current use of any tobacco , passive smoking, fruits and vegetable consumption , physical activity, sleeping hours on a typical day, over weight and current alcohol use.
Table 4: Multi-variate logistic regression analysis results of hypertension and abdominal obesity prevalence.
Discussion
This is the first study to compare the prevalence of non communicable disease risk factors among gulf migrant workers and their non-migrant contemporaries in Malappuram district (Kerala state, India). Fruits and vegetable consumption were found to be considerably low among both migrants (13.1%) and non-migrants (23.8%) in our study. This is higher than the prevalence of unhealthy diet reported by other studies conducted in Kerala [25,26]. The possible reason was that majority of the sample men were Muslims and the study was conducted in the month of ‘Ramadan’ (Auspicious month of fasting) during which the diet pattern of the Muslim community change to more of meat consumption and less of vegetables.
Prolonged working hours (35.0%), lack of holidays from work (77.0%) and inadequate sleeping hours (41.4%) among migrants was found in our study. More than a third of the migrants were working seven days a week while such a condition is rare among nonmigrants. Difficult working conditions and human right violations among migrant workers in gulf countries were reported previously [30]. Higher number of working hours and inadequate sleep among migrants as compared to non-migrants could be increasing the stress among this group making them at higher risk of developing NCDs and risk factors [27].
The prevalence of hypertension (59.7% vs. 29.8%), abdominal obesity (79.5% vs. 44.5%), overweight (66% vs. 46%) and self reported diabetes (38.2% vs. 19.2%) was significantly higher among migrants compared to non-migrants in our study. This difference in prevalence is comparable to a study on British Guajarati’s and their contemporaries in the village of origin which reports that prevalence of 23.7% of hypertension among non- migrant Gujarat’s and 46.9% among migrant Guajarati’s [16]. People from the Indian subcontinent living in west London and their siblings in India found that Indian men in west London had significantly higher systolic and diastolic blood pressure, body mass index and other Coronary risk factors compared to their siblings in Punjab [17]. A study done on Indian migrants to London and natives in India reports 23% prevalence of hypertension in migrants compared to 1.4% in natives of Punjab, this study also reports that migrant Indians were an average 10 kg heavier than the native counterparts and the measure of obesity was strongly related to blood pressure elevation [18]. South Asian ethnicity is found as a major risk factor for Coronary Heart Disease [28]. Migrants acquire NCD risk factor profile similar to that of host country exposing their underlying genetic risk for CHD [16,17]. Higher prevalence of overweight, central obesity and hypertension was reported in an earlier study among young South Asian male migrant population in the United Arab Emirates [31]. Gulf migrants undergo lots of stress in the process of acculturation and tend to adapt the unhealthy diet pattern of the working countries making them highly vulnerable to the incidence of overweight and obesity [29,30]. This might be the reason for higher prevalence of overweight, central obesity and hypertension among migrants in the present study.
Migrants were at greater risk of developing diabetes compared to non-migrants [32]. The high prevalence of self reported diabetes in our migrants might also be due to the stress factor. There is a two way associations between stress and diabetes [33].
Since the odds of hypertension (adjusted or 2.84, 95% CI=1.83- 4.94) and abdominal obesity (adjusted or 2.51, 95% CI=1.35-4.31) was significantly higher among migrants even after adjusting for several known variables stress could have been the major factor that led to a higher prevalence among migrants. We did not measure stress in our population due to logistic and technical reasons. We noticed a consistent increase in the prevalence of hypertension, overweight and abdominal obesity with duration of migration indicating strong association between gulf migration and these risk factors.
Conclusion
The study reports that the burdens of NCD risk factors such as hypertension, low fruits and vegetable intake, general obesity (BMI), abdominal obesity and self reported diabetes was are significantly higher among the gulf migrant workers compared to non-migrant cotemporaries. Most of the gulf migrants are unskilled and semi skilled workers with lower education, who need to be imparted awareness prevention and treatment of NCDs and risk factors. In adequate rest and prolonged working hours among migrant workers are indicating work related stress which needs to be explored in detail. Strategies should be developed to reduce the prevalence of NCD risk factors among gulf migrants.
This study gives baseline data and scope for future studies to understand the factors associated with the high incidence of NCD risk Factors among gulf migrant workers, also provides strong justification for the health profession to step up health advocacy with respect to policies to reduce rates of NCD risk factors among gulf migrant workers
Limitations of the Study
Religious beliefs and social norms against alcohol and tobacco use in the study population could have resulted in under reporting of the same. The results of our study generalize best to the gulf migrant community, although they may also be relevant to the other migrant communities.
References
- World Health Organization; Non communicable diseases - Fact sheet 2011.
- Lim SS, Vos T, Flaxman AD, Danaei G, Shibuya K, Adair-Rohani H, et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012; 380: 2224-2260.
- World Health Organization; Assessment of burden of non communicable diseases.
- Mehan MB, Srivastava N, Pandya H. Profile of non communicable disease risk factors in an industrial setting. J Postgrad Med. 2006; 52: 167-171.
- India steps Non-communicable Disease Risk Factors Survey 2003-2005.
- Beaglehole R, Ebrahim S, Reddy S, Voute J, Leeder S. Chronic Disease Action Group. Prevention of chronic diseases: a call to action. Lancet. 2007; 370: 2152-2157.
- Murray CJ, Vos T, Lozano R, et al. A systematic analysis for the Global Burden of Disease Study. Lancet 2012; 380: 2197-2223.
- Geneau R, Stuckler D, Stachenko S, McKee M, Ebrahim S, Basu S, Chockalingham A. Raising the priority of preventing chronic diseases: a political process. Lancet. 2010; 376: 1689-1698.
- Ebrahim S, Pearce N, Smeeth L, Casas JP, Jaffar S, Piot P. Tackling non-communicable diseases in low- and middle-income countries: is the evidence from high-income countries all we need? PLoS Med. 2013; 10: 1001377.
- Reid CM, Thrift AG. Hypertension 2020: confronting tomorrow's problem today. Clin Exp Pharmacol Physiol. 2005; 32: 374-376.
- Unwin N, Alberti KG. Chronic non-communicable diseases. Ann Trop Med Parasitol. 2006; 100: 455-464.
- Jayaweera H, Ida P. Migration and non-communicable diseases. 2013.
- Michael B, Kumar N. Health and migration: Institute for Health and Society. University of Oslo. 2011; 8: 2440-2509.
- Irudaya Rajan S. India migration report 2013: Social costs of migration. Delhi: Routledge. 2013.
- Zachariah KC, Rajan SI. Kerala’s gulf connection 1998-2011, economic and social cost of migration. Delhi: Orient Black Swan. 2012.
- Patel JV, Vyas A, Cruickshank JK, Prabhakaran D, Hughes E, Reddy KS, et al. Impact of migration on coronary heart disease risk factors: comparison of Gujaratis in Britain and their contemporaries in villages of origin in India. Atherosclerosis. 2006; 185: 297-306.
- Bhatnagar D, Anand IS, Durrington PN, Patel DJ, Wander GS, Mackness MI, et al. Coronary risk factors in people from the Indian subcontinent living in west London and their siblings in India. Lancet. 1995; 345: 405-409.
- Keil JE, Britt RP, Weinrich MC, Hollis Y, Keil BW. Hypertension in Punjabi females: comparison between migrants to London and natives in India. Hum Biol. 1980; 52: 423-433.
- Times of India report on NRI’s and Diabetes; Patterns of obesity and diabetes among NRIs and Indian citizens.
- Chowdhury TA, Hitman GA. Type 2 diabetes in people of South Asian origin: potential strategies for prevention. British Journal of Diabetes & Vascular Disease. 2007; 7: 270-279.
- Tanur Block Panchayat.
- Chronic disease and health promotion. World Health Organization. Step wise approach to surveillance (Steps).
- World Health Organization: Diet, nutrition and the prevention of chronic diseases: report of a joint WHO/FAO expert consultation.
- Chobanian A, Bakris GL, Black HR, et al. The seventh Report of the Joint National Committee on Prevention, Evaluation, and Treatment of High Blood Pressure: The JNC Report. JAMA. 2003; 289: 2560-2572.
- Thankappan KR, Shah B, Mathur P, Sarma PS, Srinivas G, Mini GK, et al. Risk factor profile for chronic non-communicable diseases: results of a community-based study in Kerala, India. Indian J Med Res. 2010; 131: 53-63.
- Diamond J. Diabetes in India. Nature 2011; 469: 476-479.
- Landsbergis P. Long work hours, hypertension, and cardiovascular disease. Cad Saude Publica. 2004; 20: 1746-1748.
- Cappuccio FP, Cook DG, Atkinson RW, Strazzullo P. Prevalence, detection, and management of cardiovascular risk factors in different ethnic groups in south London. Heart. 1997; 78: 555-563.
- Baynouna LM, Revel AD, Nagelkerke JD, Jaber TM. Associations of cardiovascular risk factors in Al Ain- United Arab Emirates. Cardiovascular Diabetology. 2009; 8: 21-25.
- ECHR report on Migrant workers in the United Arab Emirates (UAE): A snapshot of the UAE.
- Shah SM, Loney T, Sheek-Hussein M, El Sadig M, Al Dhaheri S, El Barazi I, et al. Hypertension prevalence, awareness, treatment, and control, in male South Asian immigrants in the United Arab Emirates: a cross-sectional study. BMC Cardio vasc Disord. 2015; 15: 30.
- Carballo M, Siem F. Migration and Diab
- American Diabetes Association. 2013.