
Research Article
Austin J Radiat Oncol & Cancer. 2015;1(1): 1005.
Volumetric and Dosimetric Influences of Internal Target Delineation Based on 4D CT Measured Tumor Motion in the Treatment of Lung Cancer with Stereotactic Body Radiotherapy
Zhou YQ, Xie CY, Yi JL, Han C, Zheng XM and Jin XC*
Department of Radiotherapy and Chemotherapy, First Affiliated Hospital of Wenzhou Medical University, China
*Corresponding author: Jin XC, Department of Radiotherapy and Chemotherapy, First Affiliated Hospital of Wenzhou Medical University, Wenzhou 325000, China
Received: October 20, 2014; Accepted: February 25, 2015; Published: February 27, 2015
Abstract
Purpose: To investigate the volumetric and dosimetric impact of Internal Target Volume (ITV) delineations with tumor motions measured from 4D CT in the Stereotactic Body Radiotherapy (SBRT) treatment of lung cancers.
Materials and Methods: Three ITV definition methods for six lung cancer patients were investigated. The first one is combining all the Gross Tumor Volumes ( GTVs) in the 10 respiratory phases of 4D CT data sets (ITV all); the second is adding the measured tumor motions in Anterior-Posterior (AP), Left-Right (LR) and Cranial-Caudal (CC) directions from 4D CT to the GTV in free-breathing CT (ITV motion); the third is adding 5 mm in the AP, LR direction and 10 mm in the CC direction to the GTV in free-breathing CT (ITV general). The target volumes and dosimetric differences resulted from different ITVs were analyzed.
Results: The average ratios of ITV motion and ITV general to ITV all were 2.36 and 3.51, respectively. The volume of ITV motion and ITV general was close to each other, except for case two and case five with the largest and smallest dimension. The PTV coverage was very close for these three ITV definitions. The Lung Mean Dose (LMD) was decreased as the TIV decrease. The average LMD of ITV all was 77.4 cGy and 106.1 cGy less than those of ITV motion and ITV general, respectively.
Conclusion: Due to the relative small dimensions of tumor for SBRT treatment, no significant dosimetric differences were observed between these two ITV generation methods. Considering the workload and time required to generate ITV all, ITV motion may be a good option.
Keywords: Lung cancer; Internal target volume; Stereotactic radiotherapy; Four dimensional computer tomography; Volumetric-modulated arc therapy
Introduction
Lung cancer is the leading cause of cancer deaths in both men and women in the world and in China [1,2]. Currently, Stereotactic Body Radiotherapy (SBRT), a technique that allows delivery of very high doses of radiation and usually in several large fractions (hypofractionated), is considered as a treatment option for patients with medically inoperable early-stage Non-Small-Cell Lung Carcinoma (NSCLC) as well as those with oligometastatic lung cancers [3-5]. Due to its relatively high fraction dose, a precise definition of the target with a relatively tight Planning Target Volume (PTV), conformal RT planning with the management of target motion and high daily quality set-up verification prior to each treatment were required for SBRT.
Respiratory induced tumor motion of lung cancer is a crucial consideration in determination an internal margin around Gross Tumor Volume (GTV) to form an Internal Target Volume (ITV), which can avoid both inadequate tumor coverage and unnecessary surrounding normal tissue irradiation for individual patient. However, many of the original experiences with lung SBRT used standard, population-based margins for consideration of internal target movements and did not specifically delineate tumor contours that encompassed the tumor trajectory over the entire breathing cycle [6]. Such population-based estimates may overestimate or underestimate the margin needed for a given patient because breathing characteristics are quite variable among patients [7].
Four dimensional Computed Tomography (4D CT) has been widely used in lung cancer to estimate and determine ITV for lung cancer [8,9]. Ideally, manually contouring GTV in all 10 breath phases of a 4D CT sets is required to form ITV. However, this is very time-consuming and labor-intensive. What’s more, we may fail to reconstruct 4DCT images for cases with an irregular breathing pattern. To reduce the workload of contouring multiple GTVs, contouring only in a few breath phases image sets [10], average CT [11], Maximum Intensity Projection (MIP) technique and slow CT has been suggested to form the ITV, but with variable conclusions [7,12]. On the other hand, the 4D CT sets has been considered as a reliable and effective tool for assessing tumor and organ motion [13,14]. It is of interests to investigate whether we could simple use the measured tumor motion obtained from 4D CT to define the patient specific ITV in free-breath 3D-CT. The main purpose of this study is to investigate the volumetric and dosimetric differences of different ITV delineations in the SBRT treatment of lung cancers.
Materials and Methods
Patients and simulation
Six lung cancer patients were enrolled in this study. Four patients had primary disease of lung cancer (Stage 1, non-small cell lung cancer-NSCLC) and two patients had metastatic disease with an average age at the time of treatment of 56 years (range 45–71). This study was approved by the Institutional Review Board and performed at the first Affiliated Hospital of Wenzhou Medical University.
Patients were immobilized using BodyFix system to improve positioning reproducibility and to reduce the target motion with arms placed on their forehead. A16-slice Brilliance Big Bore CT scanner (Philips Healthcare, Cleveland, and OH.) equipped with Bellows system was used to acquire high quality free-breath 3D CT and 4D CT images for each patient. Bellows is a deformable rubber belt that when placed across the patient’s chest/waist measures the changes in lung volume and generates a breathing signal corresponding to the lung volume. Contrast of 100 mL with a concentration of 300 mg I/mL was injected synchronously during image acquisition in order to enhance the visibility of tumors on CT. A time delay was programmed within image acquisition protocol so that the start of contrast injection was initiated simultaneously with the start of the scanner’s timer countdown.
After CT images were scanned and reconstructed, CT images were sent to Extended Brilliance Workspace and retrospectively sort the reconstructed into 10 respiratory phases, each of which reflected 10% of the respiratory cycle. The motion ranges at the tumor centroid in the Left-Right (LR), Anterior-Posterior (AP), and Cranial-Caudal (CC) directions were measured in the transverse, sagittal, and coronal planes with a grid spacing of 1 mm for all 10 phase bins registered by pulmonary gating option.
Target delineation and treatment planning
All CT datasets were transferred into a commercial treatment planning system (Monaco 5.0, Elekta). The system uses an enhanced pencil beam algorithm to calculate the open field dose. Then, the fluence optimization begins in which the weights of all individual pencil beams are varied simultaneously. The GTV was contoured in each of the 10 4D CT data sets and the 3D CT sets by a senior radiotherapy oncologist using standardized lung window level setting. Three approaches were applied to determine the ITV for these lung cancer patients. The first one is to combine all the ten GTVs in the 10 respiratory phases of the 4D CT data sets (ITVall); the second is to add the measured tumor motions in AP, LR and CC directions from 4D CT to the GTV in the free-breath 3D CT data (ITVmotion); finally, a third conventional ITV was created by adding 5 mm in the AP, LR direction and 10 mm in the CC direction to the GTV generated from free-breathing helical CT scans (ITVgeneral). A uniform margin of 3 mm was added to the ITVs to form the Planning Target Volume (PTV).
Partial arc Volumetric Modulated Arc Therapy (VMAT) plans with a gantry rotation angle of 180 degree were generated by Monaco 5.0 for these PTVs at a prescription dose of 55 Gy in 5 fractions with a Biological Equivalent Dose (BED) of 118 Gy. Dosimetric constraints from RTOG 236 were applied during planning: 95% of the PTV was to receive the prescribed dose; 99% of the PTV was to receive 90% of the prescribed dose, as well as the constrains of the ratio of the prescription isodose volume to PTV, Maximum dose 2 cm from PTV (D2cm) in any direction, ratio of 50% prescription isodose volume to the PTV (R50%) [15]. Physical constraints used for VMAT optimization including a leaf motion of 0.46 cm/deg, a minimum segment area of 8 cm2, a minimum segment MU requirement of 20, a maximum of 100 iterations per plan, a 10 iteration segment weight reoptimization to enhance target coverage and a final arc space degree of 4.
Volumetric and dosimetric evaluation
Target volumes obtained using different ITV definitions were measured and compared. The dosimetric differences resulted from volumetric differences based on DVH were analyzed. The maximum dose (Dmax), mean dose (Dmean), minimum dose (Dmin) of PTV. Additional parameters for PTV, such as the conformality index, defined as the ratio of the PTV to the total volume that receives 100% of the prescribed dose, the maximum dose to normal tissue 2.0 cm in all directions from the PTV, (D2cm), the ratio of the volume of the 50% of prescription dose to the volume of the PTV, were also evaluated. For OAR evaluation, the Dmean of lung, the percent volume of lung receiving 5, 10, 15, 20, 30 Gy (V5, V10, V15, V20, V30), the Dmax of spinal cord and the dose irradiated to 1cc of spinal cord (D1) were evaluated.
Statistics
Results were described as mean ± Standard Deviation (SD). Comparisons among different ITV methods were analyzed with one way ANOVA method. When an overall significant difference was observed, the post hoc Turkey’s test was used to determine which pair-wise comparisons differed. All statistical analysis was conducted with SPSS 17.0 software. Differences were considered statistically significant for p < 0.05.
Results
Figure 1 shows the volumetric differences for different ITV definition. The dimension of the GTV and detailed volumetric differences of ITVmotion and ITVgeneral related to ITVall, generated from all 10 phases CT sets, and were presented in table 1. The average ratio of ITVmotion and ITVgeneral to ITVall were 2.36 and 3.51, respectively. Extreme large volume differences were observed for case two and case five, which has the largest and smallest tumor dimensions. The volume of ITVmotion and ITVgeneral was close to each other, except for case two and case five. The time needed to contour ITVmotion was about 10-15 min, while the time needed to contour ITVall was about 30 min.
Patient
Dimension (cm)
ITVmotion/ITVall
ITVgeneral/ITVall
ITVmotion/ITVgeneral
1
2.93
2.54
3.08
0.83
2
3.05
3.46
2.30
1.51
3
2.24
2.40
2.40
1.00
4
2.19
1.89
3.78
0.50
5
1.22
1.94
7.20
0.27
6
2.84
1.92
2.32
0.83
average
2.41
2.36
3.51
0.82
Table 1: Detailed tumor dimension and volumetric differences.
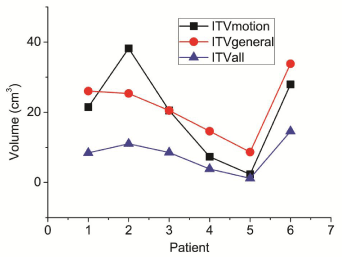
Figure 1: Volumetric differences for three different internal target volume
definitions.
Dosimetric variations for different ITV definitions were presented in table 2. The PTV coverage was very close for these three ITV definitions. The LMD was decreased as the TIV decrease. The average LMD of ITVall was 77.4 cGy and 106.1 cGy less than those of ITVmotion and ITVgeneral, respectively; the V5, V10, and V20 of ITVall were about 1-2% less than those of ITVmotion and ITVgeneral, although without significant differences were observed.
ITVmotion
ITVgeneral
ITVall
P
PTV
Dmax (cGy)
5986.5±42.9
5973.8±33.4
5947.5±40.9
0.25
Dmin (cGy)
5177.6±208.1
5099.1±175.8
5282.9±124.0
0.21
Dmean(cGy)
5671.1±14.5
5666.2±4.9
5668.9±15.4
0.80
HI
1.04±0.005
1.05±0.004
1.05±0.008
0.37
CI
0.73±0.11
0.79±0.04
0.67±0.09
0.08
R100%
1.12±0.02
1.13±0.01
1.12±0.02
0.44
D2cm (cGy)
3421.3±201.3
3424±212.1
3425.2±203.2
0.65
R50%
5.4±0.05
5.3±0.03
5.4±0.03
0.54
Lung
Dmean (cGy)
504.8±146.0
533.5±141.2
427.4±119.1
0.40
V5
18.6±5.4
19.9±5.3
16.7±4.8
0.57
V10
12.7±3.5
13.3±3.2
11.2±2.9
0.52
V20
8.2±3.1
8.7±3.0
6.1±2.1
0.27
V30
5.4±2.2
5.6±2.3
3.9±1.7
0.36
Spinal cord
Dmax (cGy)
1118.2±247.1
1026.6±265.8
1053.2±236.7
0.81
D1 (cGy)
1044.2±226.6
967.7±266.5
976.2±206.2
0.83
Table 2: Dosimetric differences on PTV and OARs for different ITV definitions.
Discussion
Respiratory induced tumor motion and its effects on the target definition and treatment delivering were major concerns in the treatment of lung cancer patients. The volumetric and dosimetric differences for different ITV definitions based on 4D CT in the SBRT treatment of lung cancer were investigated in this study.
Respiratory motion for lung cancer is often unpredictable and is not necessarily covered by generous isocentric expansion of GTV contoured on general CT images [16]. As presented by the ratio between ITVmotion to ITVgeneral in table 1, the individual motion characteristics were rather random. When a patient has a large respiratory motion, the ITVgeneral will be too small to achieve enough coverage, such as in case two. On the contrary, if a patient has a small respiratory motion, ITVgeneral will be too big to irradiate much more normal lung tissues, such as in case five. This finding is consisted with the results of previous studies that population based ITV may not account for the tumor motion [16,17].
Four dimensional CT provides a tool for individualized target volume incorporating tumor motion. However, how to best utilize the information of a 4D CT to construct the ITV is currently debated [18,19]. The TIV based on motion measurement was about two times larger than ITV based on 4D CT in this article. However, the delineation error and artifacts in 4DCT may reduce the accuracy of ITVall. Louie et al. demonstrated significant intra-observer and interobserver variability in delineation of GTV in the 4DCT [20]. Persson et al. showed the considerable deviations in delineated GTV were introduced by artifacts [21]. In addition, Cai et al. reported the gating window ITV (ITVGW) derived from 4DCT may be underestimated due to respiratory variations and suggested expanding another margin to account for the potential error in generating the PTVGW [22]. These limitations in 4DCT inevitably impact on accessing the volumetric differences between ITVmotion and ITVall. Furthermore, the vast amount of data generated via 10 phases of 4DCT may substantially increase the time needed for image review and target/ critical structure delineation.
The dosimetric differences among different ITV definitions were relatively small in this study. There was no significant difference on target coverage and conformal index observed. The LMD and the percent volume of lung receiving certain dose of ITVall were smaller than those of ITVmotion and ITVgeneral due to the smaller volume. The doses to the normal tissues were very close among ITVall, ITVmotion and ITVgeneral. This was different from previous study in which significant decrease in LMD, V5, V10, V20, V25 and V30 were observed with the decrease of ITV volume [23]. This difference could be caused by different tumor dimension, and different normal lung delineations and window/level settings were applied. In this study, the target volume was not excluded in the normal lung tissue. This difference could also due to the relative small number of patients investigated in this study.
One limitation of this study is a relatively simple algorithm was used to calculate the delivered dose distributions. Many studies have discussed that dose calculation algorithm has a great impact on lung cancer treatment, especially for SBRT with small fields [24,25]. During optimization, the same pencil beam algorithm was consistently used with the same dose constraints for target and organs for each plan to reduce the calculation bias. A more accurate algorithm, such as the superposition/convolution or Monte Carlo based algorithms should be used for lung SBRT planning in clinical practice in order to obtain accurate patient dose.
Conclusion
ITV based on the respiratory motion detected with 4D was a little large than ITV generated based on the 10 respiratory phases 4DCT sets. However, due to the relative small dimensions of tumor for SBRT treatment, no significant dosimetric differences were observed between these two ITV generation methods. Considering the workload and time required to generate ITVall, ITVmotion may be a good option.
Acknowledgment
The study was supported by a grant from the Wenzhou Science and Technology Bureau (H20100068).
References
- Pisani P, Parkin DM, Ferlay J. Estimates of the worldwide mortality from eighteen major cancers in 1985. Implications for prevention and projections of future burden. Int J Cancer. 1993; 55: 891-903.
- Li L, Yao K, Zhang S, Ru F, Zhou X. Statistical Analysis of Data from 12 Cancer Registries in China. Bull Chin Cancer. 2002; 11: 497-507.
- Ettinger DS, Akerley W, Borghaei H, Chang AC, Cheney RT, Chirieac LR, D'Amico TA. Non-small cell lung cancer, version 2.2013. J Natl Compr Canc Netw. 2013; 11: 645-653.
- Takeda A, Kunieda E, Ohashi T, Aoki Y, Koike N, Takeda T. Stereotactic body radiotherapy (SBRT) for oligometastatic lung tumors from colorectal cancer and other primary cancers in comparison with primary lung cancer. Radiother Oncol. 2011; 101: 255-259.
- Norihisa Y, Nagata Y, Takayama K, Matsuo Y, Sakamoto T, Sakamoto M, et al. Stereotactic body radiotherapy for oligometastatic lung tumors. Int J Radiat Oncol Biol Phys 2008; 72: 398–403.
- Underberg RW, Lagerwaard FJ, Cuijpers JP, Slotman BJ, van Sornsen de Koste JR, Senan S. Four-dimensional CT scans for treatment planning in stereotactic radiotherapy for stage I lung cancer. Int J Radiat Oncol Biol Phys. 2004; 60:1283-1290.
- Ezhil M, Vedam S, Balter P, Choi B, Mirkovic D, Starkschall G, et al. Determination of patient-specific internal gross tumor volumes for lung cancer using four-dimensional computed tomography. Radiat Oncol 2009; 4: 4.
- Liu HH, Balter P, Tutt T, Choi B, Zhang J, Wang C, et al. Assessing respiration-induced tumor motion and internal target volume using four-dimensional computed tomography for radiotherapy of lung cancer. Int J Radiat Oncol Biol Phys 2007; 68:531-540.
- Jin JY, Ajlouni M, Chen Q, Yin FF, Movsas B. A technique of using gated- CT images to determine internal target volume (ITV) for fractionated stereotactic lung radiotherapy. Radiother Oncol 2006; 78: 177-184.
- Rosu M, Balter JM, Chetty IJ, Kessler ML, McShan DL, Balter P, et al. How extensive of a 4D dataset is needed to estimate cumulative dose distribution plan evaluation metrics in conformal lung therapy? Med Phys. 2007; 34: 233-45.
- Admiraal MA, Schuring D, Hurkmans CW. Dose calculations accounting for breathing motion in stereotactic lung radiotherapy based on 4D-CT and the internal target volume. Radiother Oncol. 2008; 86: 55-60.
- Keall PJ, Mageras GS, Balter JM, Emery RS, Forster KM, Jiang SB, Kapatoes JM. The management of respiratory motion in radiation oncology report of AAPM Task Group 76. Med Phys. 2006; 33: 3874-3900.
- Guckenberger M, Wilbert J, Meyer J, Baier K, Richter A, Flentje M. Is a single respiratory correlated 4D-CT study sufficient for evaluation of breathing motion? Int J Radiat Oncol Biol Phys. 2007; 67: 1352-1359.
- Dinkel J, Welzel T, Bolte H, Hoffmann B, Thierfelder C, Mende U, et al. Four-dimensional multislice helical CT of the lung: qualitative comparison of retrospectively gated and static images in an ex-vivo system. Radiother Oncol 2007; 85: 215–222.
- Michalski J, Fowler J, Johnstone D, Gore E, Timmerman RD, Choy H, et al. A Phase II Trial of Stereotactic Body Radiation Therapy (SBRT) in the Treatment of Patients with Medically Inoperable Stage I/II Non-Small Cell Lung Cancer. Radiation therapy oncology group, RTOG 0236.
- Rietzel E, Liu AK, Chen GT, Choi NC. Maximum-intensity volumes for fast contouring of lung tumors including respiratory motion in 4DCT planning. Int J Radiat Oncol Biol Phys. 2008; 71: 1245-1252.
- van Sonsen de Koste JR, Lagerwaard FJ, Nijssen-Visser MR, Graveland WJ, Senan S. Tumor location cannot predict the mobility of lung tumors: a 3D analysis of data generated from multiple CT scans. Int J Radiat Oncol Biol Phys 2003; 56: 348–354.
- Van Dam IE, van Sörnsen de Koste JR, Hanna GG, Muirhead R, Slotman BJ, Senan S. Improving target delineation on 4-dimensional CT scans in stage I NSCLC using a deformable registration tool. Radiother Oncol 2010; 96: 67-72
- Zhao B, Yang Y, Li T, Li X, Heron DE, Huq MS. Image-guided respiratory-gated lung stereotactic body radiotherapy: which target definition is optimal? Med Phys. 2009; 36: 2248-2257.
- Louie AV, Rodrigues G, Olsthoorn J, Palma D, Yu E, Yaremko B, et al. Inter-observer and intra-observer reliability for lung cancer target volume delineation in the 4D-CT era. Radiother Oncol. 2010; 95: 166-171.
- Persson GF, Nygaard DE, Brink C, Jahn JW, Munck af Rosenschöld P, Specht L, et al. Deviations in delineated GTV caused by artefacts in 4DCT. Radiother Oncol. 2010; 96: 61-66.
- Cai J, McLawhorn R, Read PW, Larner JM, Yin FF, Benedict SH, et al. Effects of breathing variation on gating window internal target volume in respiratory gated radiation therapy. Med Phys. 2010; 37: 3927-3934.
- Yeo SG, Kim ES. Efficient approach for determining four-dimensional computed tomography-based internal target volume in stereotactic radiotherapy of lung cancer. Radiat Oncol J. 2013; 31: 247-251.
- Ding GX, Duggan DM, Lu B, Hallahan DE, Cmelak A, Malcolm A, et al. Impact of inhomogeneity corrections on dose coverage in the treatment of lung cancer using stereotactic body radiation therapy. Med Phys. 2007; 34: 2985-2994.
- Traberg Hansen A, Petersen JB, Høyer M, Christensen JJ. Comparison of two dose calculation methods applied to extracranial stereotactic radiotherapy treatment planning. Radiother Oncol. 2005; 77: 96-98.