
Research Article
Austin J Radiat Oncol & Cancer. 2016; 2(1): 1019.
Inter-Fraction Variations of D2cc Brachytherapy Dose Received By Bladder and Rectum in Patients with Inoperable Cervical Cancer
Marosevic G¹*, Butler EB² and Mileusnic D¹
¹Center for Radiotherapy, International Medical Centers, City of Banja Luka, Bosnia and Herzegovina
²Department of Radiation Oncology, The Methodist Hospital, Houston, Texas, USA
*Corresponding author: Goran Marosevic, Center for Radiotherapy, International Medical Centers, City of Banja Luka, Bosnia and Herzegovina
Received: May 17, 2016; Accepted: June 20, 2016; Published: June 22, 2016
Abstract
Purpose: To examine the inter-fraction variations of the D2cc of the brachytherapy dose applied to bladder and rectum in patients with inoperable cervical cancer on the CT basis. Methods and Materials. This prospective study included 30 patients with cervical cancer FIGO IIb-IVa stage who were treated with concomitant chemo-radiotherapy. Intracavitary brachytherapy was performed with applicators type Fletcher tandem and ovoids, once a week at the HDR regime (high dose rate). Computer tomography was made after every application. The analysis was made whether there is a statistically significant difference in the inter-fraction variations of the D2cc of the brachytherapy dose to bladder and rectum. Statistical significance of differences among the examined groups was tested with ANOVA test as well as the Tukey post-hoc analysis. The difference among the groups analyzed was considered significant if P<0.05.
Results: Statistical significance has been found neither in the change of the dose for all fractions in relation to the first one nor by the post-hoc analysis by Tukey method for the differences in the dose for all fractions mutually for bladder (p=0.45) and for rectum (p=0.73). One standard deviation of the brachytherapy dose for bladder is 1.09Gy and for rectum it is 1.045Gy (15.6% and 15% of the prescribed dose).
Conclusion: There is no significant inter-fraction change of the brachytherapy dose D2cc of the bladder and rectum during the inoperable cervical cancer brachytherapy. However, two standard deviations need to be included while calculating the total EQD2cc of the bladder and rectum.
Keywords: Inter-fraction variations; Brachytherapy; Inoperable cervical cancer
Introduction
Intracavitary brachytherapy has been an obligatory type of the treatment of the locally advanced cervical cancer for decades. The main principles of brachytherapy are based on traditional schools (Paris, Manchester, Stockholm, Fletcher, etc.), that are still dominant in planning brachytherapy for cervical cancer [1]. Verification of the applicator position and organs at risk (bladder and rectum, as well as the sigmoid for 3D brachytherapy) is done with the aim to optimize brachytherapy dose in order to achieve complete dose distribution around the target volume, while sparing organs at risk as much as possible. Prescription of dose is done according to the standard Manchester system of the dose into the point A [2]. Nowadays, CT (computer tomography) and MR (magnetic resonance) based brachytherapy are becoming a standard treatment of locally advanced gynecological tumors [3-6]. Intracavitary brachytherapy of cervical cancer consists of multiple applications, usually four to five. As recommended by the GEC-ESTRO working group, it is important for the 3D image guided brachytherapy of cervical cancer to verify what is the dose received by 0,1 cm3, 1 cm3 and 2 cm3 (D0,1cc, D1cc and D2cc, respectively) of bladder and rectum volume [7]. Doses received by organs at risk for all brachytherapy applications are summed up together with the external dose, and the total cumulative dose is determined by using the linear-quadratic model [8]. In planning brachytherapy, CT does not give us the possibility to precisely delineate tumor and plan the distribution of the therapy dose to the tumor (as is the case with MR planning). However, it is possible to obtain precise data on contribution of the brachytherapy dose to the organs at risk [9,10]. Georg P. et al. correlated the level of complications with the dose received by the abovementioned referential volumes of the organs at risk [11]. Recently, Hollowey et al. published the results including the application related variation of the dose received by the sigmoid, under the conditions that the same volume of sigma always receives the brachytherapy dose [12].
The aim of this research is to examine the inter-fraction variations of the D2cc of the brachytherapy dose applied to bladder and rectum in patients with inoperable cervical cancer on the CT basis. If the statistical significance does not exist, is it necessary to do computer tomography for every application?
Patients and Methods
Patients
This prospective study included patients with cervical cancer, FIGO IIb-IVa stage, who were treated with concomitant chemoradiotherapy at the University Clinical Centre Tuzla, at the Department for radiotherapy of the Clinic for oncology, hematology and radiotherapy. The study was conducted on a consecutive sample of 30 patients treated in the period April 2010 – May 2012. Inclusion criteria were non-operated patients, brachytherapy was performed with an intra-uterine applicator and two vaginal ovoids.
Methods
Patients were treated with external conformal radiotherapy with the dose of 45Gy in 25 fractions to the tumor, parametria and regional lymph nodes along with the concomitant chemotherapy with Cisplatin with the dose of 40 mg/m2. External radiotherapy was performed on the linear accelerator Elekta Sinergy® and with the energy of 15 MV. Intracavitary brachytherapy was started after 10 to 13 fractions of external radiotherapy. Intracavitary brachytherapy was performed with applicators type Fletcher tandem and ovoids, once a week at the HDR regime (high dose rate) with radioactive Iridium (192Ir) on Flexitron®. Rectum and bladder filling protocols required that a patient takes 20mg bisacodyl laxative suppositories (Dulcolax®) 12 hours prior to every brachytherapy application and urinates immediately before every brachytherapy application. During every application, bladder and rectum were tamponed by same radiation oncologist with gauze soaked in the lopromid (Ultravist®) contrast liquid which was in 4 to 1 ratio with the physiological solution. The therapy dose (TD) of 7Gy was prescribed to the A point according to the Manchester system.
After each brachytherapy application (five in total), computer tomography of pelvis was made. Bladder and rectum were delineated during each CT scan. Bladder and rectum delineation was made on every CT slice: rectum at 1cm from anus to the recto-sigmoid transition through the entire thickness of the organ wall, and bladder following the outer contour of the entire organ volume. Planning of brachytherapy dose distribution for each application was made on the basis of computer tomography with the planning software system Flexiplan Isodose Control®
The quantity of the D2cc of the brachytherapy dose to bladder and rectum for each application was defined. The analysis was made whether there is a statistically significant difference in the interfraction variations of the D2cc of the brachytherapy dose to bladder and rectum between the planning for all applications in relation to the first application. A post-hoc analysis of the variations of the D2cc of the brachytherapy dose was made between applications.
Statistical analysis
In statistical processing of the results, standard methods of descriptive statistics were used (arithmetic mean with the standard deviation and the numerical range from minimum to maximum value). Statistical significance of differences among the examined groups was tested with ANOVA test as well as the Tukey post-hoc analysis. Statistical hypotheses were tested at the significance level of α = 0.05, i.e. the difference P<0.05 was considered statistically significant. SPSS 17.0 (SPSS Inc, Chicago, IL) statistics software was used for the data analysis.
Results
The study included thirty patients. A total of 150 brachytherapy applications were performed. Table 1 shows the patient demographics. The average age of patients at the time of the treatment was 52, and most of them were at FIGO IIb stage of planocellular cervical cancer.
Characteristics
AS ± SD*
Age
Cancer stage FIGO
52 ± 11
IIb
24 (80%)
IIIb
5 (16,7%)
IVa
1 (3,3%)
*AS – Mean; SD – Standard deviation
Table 1: Patient Demographics.
The results of the minimum brachytherapy dose expressed in Gy, received by the most exposed 2cm3 (D2cc) of bladder for each application are presented as arithmetic means with standard deviation in Table 2. The lowest value of D2cc of bladder was measured in the second application on average (4.3±1.4), while the highest value was measured in the fifth application (4.6±1.3). The total (TRT + BHT) biologically equivalent dose in 2Gy by application (EQD2) for bladder was on average 76.7 ± 5.6 Gy.
Applications
AS ± SD*
Application I
4,4 ±1,4
Application II
4,3 ±1,4
Application III
4,7 ±1,2
Application IV
4,4 ±1,2
Application V
4,6 ±1,3
*AS – Mean; SD – Standard deviation
Table 2: D2cc of bladder for each application, given in Gy.
The results of the minimum brachytherapy dose expressed in Gy, received by the most exposed 2cm3 (D2cc) of rectum for each application are presented as arithmetic means with standard deviation in Table 3. The lowest value of D2cc of rectum was measured in the fifth application on average (4.7 ±0.7), while the highest value was measured in the second and fourth application (5.0 ±1.0). The total (TRT + BHT) biologically equivalent dose in 2Gy by application (EQD2) for rectum was on average 81.9 ± 3.4 Gy.
Applications
AS ± SD*
Application I
4,9 ±1,0
Application II
5,0 ±0,8
Application III
4,9 ±0,9
Application IV
5,0 ±1,0
Application V
4,7 ±0,7
*AS – Mean; SD – Standard deviation
Table 3: D2cc of rectum for each fraction given in Gy.
Inter-fraction variations, the change in the D2cc of the brachytherapy dose received by 2cm3 of bladder during each application in relation to the first application, are shown in Table 4 and Figure 1. All values are given in Gray (Gy). The mean value of change of D2cc of bladder ranged from 0.23Gy in the fourth application to 0.56Gy in the third application, with the total standard deviation of 1.09Gy (15.6% of the prescribed dose). The analysis of variance did not show statistical significance in the dose change for all fractions in relation to the first one. The same can be said for the Tukey post-hoc analysis of the differences in the dose for all applications in correlation (p=0.45). The range of change in the D2cc of the brachytherapy dose of bladder ranged from the decrease of the dose by 2.2Gy (31.4%) to the increase by 2.7Gy (38.5 %). The range of the change in the brachytherapy biologically equivalent dose in 2 Gy per application (EQD2) at D2cc of bladder among the patients ranged from 2.6Gy to 14.6Gy.
**Dose change at D2cc
AS*
SD¶
Minimum
Maximum
II-I application
0.55
1.08
-1.90
2.70
III-I application
0.56
0.66
-1.00
1.50
IV-I application
0.23
0.84
-2.20
1.50
V-I application
0.37
0.06
-2.10
2.70
*AS – Mean; ¶SD – Standard deviation; **ANOVA; p= 0.45
Table 4: Change in the D2cc of brachytherapy dose given in Gy for bladder for each application in relation to the first one.
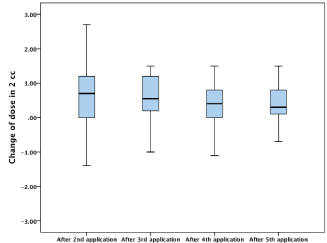
Figure 1: Change in the D2cc of brachytherapy dose given in Gy for bladder
for each application in relation to the first one.
Inter-fraction variations, the change in the D2cc of the brachytherapy dose received by 2cm3 of rectum during each application in relation to the first application are shown in Table 5 and Figure 2. All values are also given in Gy. The mean value of change of D2cc of rectum ranged from -0.17Gy in the fifth application to 0.10Gy in the second application, with the total standard deviation of 1.045Gy (15% of the presrcibed dose). The analysis of variance did not show statistical significance in the dose change for all fractions in relation to the first one. The same can be said for the Tukey post-hoc analysis of the differences in the dose for all applications in correlation (p=0.73). The range of the change in the D2cc of the brachytherapy dose of rectum ranged from the decrease of the dose by 2.2Gy (31.4%) to the increase by 2.0Gy (28.6 %). The range of change in the brachytherapy biologically equivalent dose in 2Gy per application (EQD2) at D2cc of rectum among the patients ranged from 3.1Gy to 13.7Gy.
**Dose change at D2cc
AS*
SD¶
Minimum
Maximum
II-I application
0.1
1.01
-1.8
1.6
III-I application
0.01
0.97
-1.7
2
IV-I application
0.07
1.08
-2.2
2
V-I application
-0.17
1.03
-2
1.9
*AS – Mean; ¶SD – Standard deviation; **ANOVA; p= 0.73
Table 5: Change in the D2cc of brachytherapy dose given in Gy for rectum for each application in relation to the first one.
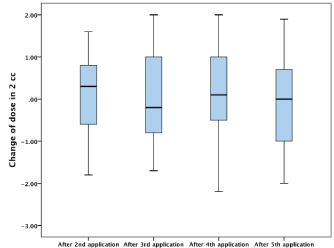
Figure 2: Change in the D2cc of brachytherapy dose given in Gy for rectum for
each application in relation to the first one.
Discussion
It is recommended to monitor and report the dose received by small volumes of organs at risk in the gynaecological brachytherapy [13,14]. This study examined the dose received by 2cm3 (D2cc) of bladder and rectum and it was shown how the brachytherapy dose received by 2 cm3 of bladder changed from one application to another on average from 4.3 ±1.4 Gy to 4.7 ±1.2 Gy (Table 2), while for the rectum the dose ranged from 4.7 ±0.7 Gy do 5.0 ±1.0 Gy (Table 3). An average total (TRT + BHT) biologically equivalent dose in 2Gy per application (EQD2) is calculated by linear-square model based algorithm, and it includes the dose, its speed, and the number of applications during the entire radiotherapy [8]. This model is implemented into the routine practice by the model α/β = 3 Gy for the organs at risk and T1/2 = 1.5h for all tissues [15,16].
In a multi-centric research published in the study by Jurgenliemk- Schulz et al. [1], variations were examined in the planning of MRI based brachytherapy treatment of cervical cancer, and a comparative analysis of DVH parameters of 3D plans recommended by GECESTRO was made. One of the goals was to keep D2cc of bladder and rectum below EQD2 90Gy and 75Gy respectively. The results of this multi-centric research showed that in the MRI brachytherapy nonoptimized planning without interstitial needles an average dose of EQD2cc for bladder was 92 ± 8 Gy, while for rectum the dose was 64 ± 3Gy. Comparing this with the results in this study (76.7 ± 5.6Gy for bladder and 81.9 ± 3.4Gy for rectum) it can be said that in this study the contribution of the dose on bladder was even lower, but rectum received somewhat higher dose on average. Lower EQD2cc in this study, when compared to the abovementioned study, can be explained by the fact that this study included the front vaginal packing, which made bladder more distant from the radio-active source. Also, in this study the contrast liquid was not applied on the bladder, so it had a small volume during each application and was more distant from the radio-active source than when filled with the contrast. Higher EQD2cc in this study, when compared to the abovementioned one, can be explained by the fact that, in this study, one application more was prescribed, which, according to the LQ model, is 14 Gy. Therefore, while comparing the results, it is evident that there was no difference in the EQD2cc dose of rectum. Although this was not an MRI based study, it has been proved that CT scanning is equally valid in the evaluation of DVH parameters of the organs at risk [10].
Based on this concept, Georg et al. [11] correlated the dose received by 2 cm3 of rectum during the definite radiotherapy (including the MR based brachytherapy) for the patients with inoperable cervical cancer. The results of the DVH parameters in correlation with the clinical symptoms measured by the LENT/SOMA scale showed the complications of LENT/SOMA 0 for D2cc = 63 ± 8Gy and LENT/ SOMA 1-4 for D2cc = 72 ± 6Gy. Taking into consideration D2cc of rectum in this study, we can expect a higher number of our patients with complications of higher grade.
By using the 3D imaging, this study examined not only the contribution of the dose on bladder and rectum, but also the interfraction variations, that is the change in the D2cc brachytherapy dose of bladder and rectum as the organs at risk during the brachytherapy treatment. Statistical significance was not found in the change of the dose for all applications in relation to the first one, as well as the differences in the change of the dose for all the applications in correlation. However, it is important to notice a large range of minimum and maximum changes of the dose at D2cc of bladder - min. 2.2Gy (31.4% of the dose per brachytherapy application) and max. 2.7Gy (38.5% of the dose per brachytherapy application), and for the rectum - min. 2.2Gy (31.4% of the dose per brachytherapy application) to the increase by 2.0Gy (28.6% of the dose per brachytherapy application). Regarding such extreme variations which can occur from one application to another, it is necessary to do computer tomography for each application, and use it as the basis for planning and optimizing the dose to the organs at risk. It is very important to notice the total standard deviation of inter-fraction variations of the brachytherapy dose, which was 1.09Gy (15.6%) for bladder and 1.05Gy (15%) for rectum. These results correspond to those of the multi-centric study in which one standard deviation was ranged from 12% to 24.7% for bladder and from 15.1% to 24.8% for rectum. The effect of these variations on the total biologically equivalent dose is around 20% [17]. Basically, provided that we want to predict the total dose received by D2cc of the organs at risk in 95% of the cases, we need to calculate the inter-fraction variations of the brachytherapy dose and include two standard deviations in both directions.
Holloway et al. [12] monitored the proximity distance of the sigmoid from applicators, their variance, the predictor of the change in the brachytherapy dose, as well as the level of complications on the sigma in the brachytherapy of cervical cancer, using computer tomography as the planning basis. Around 20% of HDR applications required the manipulation of the proximity “dwell” positions in order to decrease the dose on the sigma. Also, the proximity distance of the most exposed point of the sigma from the tandem had a significant correlation to the sigmoid dose (p<0.0001). The brachytherapy dose during the HDR treatment (27.5Gy in 5 applications to the A point) in their study for D2cc of the bladder ranged from 11.6Gy to 52.3Gy and 7.2Gy to 40.8Gy for rectum. All this shows that the extreme variations of the brachytherapy dose to the organs at risk were present in their study as well, which corresponds to the results of this study.
However, all the things mentioned are valid provided that the same 2cm3 volume of the organs at risk for each application received the minimum brachytherapy dose. This is the presumption on which all the previous reports in the studies were based. Basically, the worst case scenario is reported. The question is: “What if there are interfraction displacements of 2cm3 volume of the organ that receives the minimum brachytherapy dose?” Is the worst case scenario feasible?
To conclude, during the brachytherapy of inoperable cervical cancer there is no significant inter-fraction change in D2cc of the brachytherapy dose to bladder and rectum. One standard deviation of inter-fraction variations of the D2cc of the brachytherapy dose for bladder was 15.6% and 15% for rectum of the prescribed brachytherapy dose. The values of two standard deviations need to be included in the calculation of the total biologically equivalent dose received by 2 most exposed cm3 of the bladder and rectum volume. Computer-based planning of brachytherapy for inoperable cervical cancer is necessary for every application during the brachytherapy treatment.
References
- Jürgenliemk-Schulz IM, Lang S, Tanderup K, et al. Gyn GEC ESTRO network. Variation of treatment planning parameters (D90 HR-CTV, D 2cc for OAR) for cervical cancer tandem ring brachytherapy in a multicentre setting: comparison of standard planning and 3D image guided optimisation based on a joint protocol for dose-volume constraints. Radiother Oncol. 2010; 94: 339-345.
- Perez CA, Kavanagh BD. Principles and practice of radiation oncology 2008. Philadelphia: Lippincott Williams & Wilkins. 2008; 1532-1609.
- Gerbaulet A, Pötter R, Haie-Meder C. Cervix cancer. In: Gerbaulet A, Pötter R, Mazeron JJ, Meertens H, Van Limbergen E (Eds.) GEC ESTRO handbook of brachytherapy 2002. Brussels: ESTRO; 301-63.
- Weitmann HD, Pötter R, Waldhäusl C, et al. Pilot study in the treatment of endometrial carcinoma with 3D image-based high-dose-rate brachytherapy using modified Heyman packing: clinical experience and dose-volume histogram analysis. Int J Radiat Oncol Biol Phys. 2005; 62: 468-478.
- Lindegaard JC, Tanderup K, Nielsen SK, et al. MRI-guided 3D optimization significantly improves DVH parameters of pulsed-dose-rate brachytherapy in locally advanced cervical cancer. Radiat Oncol Biol Phys. 2008; 71: 756-764.
- De Brabandere M, Mousa AG, Nulens A, Swinnen A, Van Limbergen E. Potential of dose optimisation in MRI-based PDR brachytherapy of cervix carcinoma. Radiother Oncol. 2008; 88: 217-226.
- Pötter R, Haie-Meder C, Van Limbergen E, et al. GEC ESTRO Working Group. Recommendations from gynaecological (GYN) GEC ESTRO working group (II): concepts and terms in 3D image-based treatment planning in cervix cancer brachytherapy-3D dose volume parameters and aspects of 3D image-based anatomy, radiation physics, radiobiology. RadiotherOncol. 2006; 78: 67-77.
- Lang S, Kirisits C, Dimopoulos J, Georg D, Pötter R. Treatment planning for MRI assisted brachytherapy of gynecologic malignancies based on total dose constraints. Int J Radiat Oncol Biol Phys. 2007; 69: 619-627.
- Datta NR. From ‘points’ to ‘profiles’ in intracavitary brachytherapy of cervical cancer. Curr Opin Obstet Gynecol. 2005; 17: 35-41.
- Viswanathan AN, Dimopoulos J, Kirisits C, et al. Computed tomography versus magnetic resonance imaging-based contouring in cervical cancer brachytherapy: results of a prospective trial and preliminary guidelines for standardized contours. Int J RadiatOncolBioloPhys. 2007; 69: 963-964.
- Georg P, Kirisits C, Goldner G, et al. Correlation of dose-volume parameters, endoscopic and clinical rectal side effects in cervix cancer patients treated with definitive radiotherapy including MRI-based brachytherapy. RadiotherOncol. 2009; 91: 173-180.
- Holloway CL, Racine ML, Cormack RA, O’Farrell DA, Viswanathan AN. Sigmoid dose using 3D imaging in cervical-cancer brachytherapy. Radiother Oncol. 2009; 93: 307-310.
- Pötter R, Haie-Meder C, van Limberg E, et al. Recommendations from gynaecological (GYN) GEC ESTRO working group (II): concepts and terms in 3D image based treatment planning in cervix cancer brachytherapy-3D dose volume parameters and aspects of 3D image-based anatomy, radiation physics, radiobiology. RadiotherOcol. 2006; 78: 67-77.
- Sakata K, Nagakura H, Oouchi A, Someya M, Nakata K, Shido M, et al. High-dose-rate intracavitary brachytherapy: results of analyses of late rectal complications. Int J Radiat Oncol Biol Phys. 2002; 54: 1369-1376.
- Nag S, Cardenes H, Chang S, et al. Image-Guided Brachytherapy Working Group. Proposed guidelines for image-based intracavitary brachytherapy for cervical carcinoma: report from Image-Guided Brachytherapy Working Group. Int J Radiat Oncol Biol Phys. 2004; 60: 1160-1172.
- Kirisits C, Pötter R, Lang S, Dimopoulos J, Wachter-Gerstner N, Georg D. Dose and volume parameters for MRI-based treatment planning in intracavitary brachytherapy for cervical cancer. Int J Radiat Oncol Biol Phys. 2005; 62: 901-911.
- Tanderup K. Inter- and intra- fraction uncertainties and imaging strategies (MRI/CT) in brachytherapy. In: ESTRO Course book. ESTRO Teaching Course Image-Guided Radiotherapy & Chemotherapy in Gyneacological Cancer. 2012.