Review Article
Austin J Surg. 2014;1(2): 1010.
Initial Burn Management
Medhat Emil Habib*
Department of Plastic, Reconstructive and Burns, Mafraq Hospital, UAE
*Corresponding author: Medhat Emil Habib, Department of Plastic, Reconstructive and Burns, Mafraq Hospital, Abu Dhabi, UAE
Received: February 11, 2014; Accepted: March 31, 2014; Published: April 04, 2014
Abstract
Proper evaluation and management of burn patients greatly reduce the morbidity and mortality of such cases. The initial management of a severely burnt patient is similar to that of any trauma patient. The primary and secondary surveys allow the patients to be assessed and managed in a systematic way according to the priorities to be looked after. This article describes the initial management of the burnt patients according to these surveys.
Keywords: Burn
Introduction
The skin is the largest organ in the body, comprising 15% of body weight and covering approximately 1.7 m2 in the average adult. A burn injury implies damage or destruction of skin and⁄or its contents by thermal, chemical, electrical or radiation energies or combinations of them [1]. Attention to basic principles of initial burn trauma resuscitation should minimize the morbidity and mortality of these injuries.
Brief history should include the time of burn; the type of clothes worn at that time, location and circumstances of the injury e.g. closed space, where the patient was found and history of sustaining associated injury while trying to escape. Past medical and social history, current medication usage, drug allergies, and tetanus status should be rapidly determined [2].
Immediate Resuscitation and Primary Survey
Airway
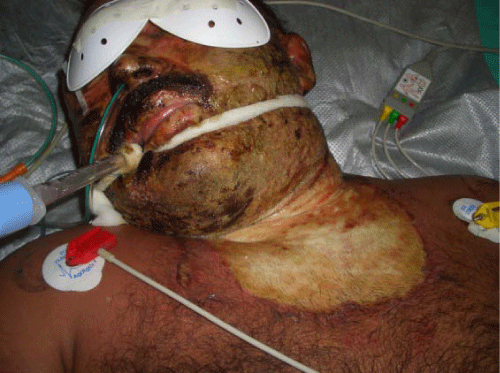
The doctor should be alert to the possibility of airway involvement (Figure 1). Clinical indications of inhalation injury include:
Figure 1 :Indications of inhalation injury.
1. History of closed–space exposure
2. History of change of voice
3. Deep face or neck burns
4. Singed nasal hairs, eyebrows or moustache
5. Carbonaceous debris in the mouth and pharynx or sputum.
6. Carboxyhaemoglobin level greater than 10%
7. Stridor– Immediate intubation
Intubation should be performed prior to transport of the patient to a burn center to protect the airway. Circumferential burns of the neck may lead to swelling of the tissues around the airway. Therefore, early intubation is indicated in this situation.
Breathing
Smoke may damage the lungs in three ways:
- Intoxication ⁄hypoxaemia
- Respiratory tract injury due to irritants
- Thermal damage
Intoxication can result from release of gases in the fire scene. Carbon monoxide has a higher affinity for haemoglobin than oxygen, and will lead to tissue anoxia. Symptoms range from a throbbing headache with nausea and vomiting to coma, convulsions and cardiac arrest [3]. Cherry–red skin colour is rare. Pulse oxymeters are inaccurate in the presence of carboxyhaemoglobin and cannot be relied upon. Specific investigations include COHb levels, arterial blood gases, and fibrotic bronchoscope. 100% oxygen is the initial treatment and may necessitate intubation and ventilation. Chest physiotherapy and tracheo–bronchial toileting are usually required. Hyperbaric oxygen may be useful.
Other gases such as hydrogen sulphide, hydrogen cyanide and hydrogen chloride may be inhaled, particularly if paints or furniture have been involved in the fire. Cyanide poisoning is suspected if the patient is apnaeic and has a metabolic acidosis indicating tissue hypoxia. Hydroxocobalamin injection (Vitamin B12a ) can be givento patients with cyanide poisoning to form cyanocobalamin which is removed from the body in the urine. Soot is an irritant that will cause chemical injury if left in the airway. It can be treated with nebulizers.
Circulating Blood Volume
Burn shock can develop rapidly if fluid resuscitation is delayed. Adult patients with more than 15% total body surface area (TBSA) burn and children with more than 10% burn require IV access [1]. There is a considerable debate about the type of fluid to be used for resuscitation of burn patients [4,5]. The Parkland formula is the most commonly used formula worldwide [6]. Ringer Lactate is administered as
4ml X body weight X % of burn
1⁄2 of this amount is given in the 1st 8 hours and the second1⁄2 of this amount during the following 16 hours [7].
Muir and Barclay formula used colloids throughout the 36 hours post burns by the formula:
1⁄2ml X % of burns X weight (Kg)
This amount is given during each of the periods of 4, 4, 4, 6, 6 and 12 hours post burn.
Studies showed that due to the capillary permeability in cases of burns, colloid replacement seems to be of no benefit in the immediate post–burn period (Initial 12–24 hours). Since sodium seems to be the ion that is lost to the circulation as a result of disruption of the Na–Kpump of the cells, sodium ions and not colloid appear to be the key to resuscitation [8].
A combination of both the Parkland and the Muir and Barclay formulas constructed a new formula published by the author in a recent study in 2013[9]. Crystalloids were used in the first 12 hours of the shock period, in the form of normal saline, followed by colloids, in the form of 5% purified plasma proteins fraction during the following 24 hours.
The formula used in the first 12 hours is
4ml X body weight X % of burn
1⁄2 of this amount is given in the 1st 8 hours and 1⁄8th of this amount during the following 4 hours. After the first 12 hours are over, plasma starts according to the formula:
1⁄2 X Body weight X % of burn
This amount is administered during each of the following 6,6 and 12 hours.
Please note that:
- The calculation of the amount of fluids required starts from the time of occurrence of the burns and not from the time of admission to the hospital.
- Maintenance fluids are added to the calculated fluids.
- All resuscitation formulas are meant to serve as guides only [1]. They should not be followed as rules and fluids adjustment should be done according to the vital signs as pulse and blood pressure, urine output, dehydration symptoms and signs and the haematocrit value.
- Fluids administered should try to keep the urine output about 0.5–1 ml⁄Kg⁄hour in adults and 1–1.5 ml⁄Kg⁄hour in children. High flow is recommended in electric burns.
Secondary Survey and Related Adjuncts
Physical Examination
1. Assess for associated injuries
2. Estimate the extent and depth of burn
Body Surface Area
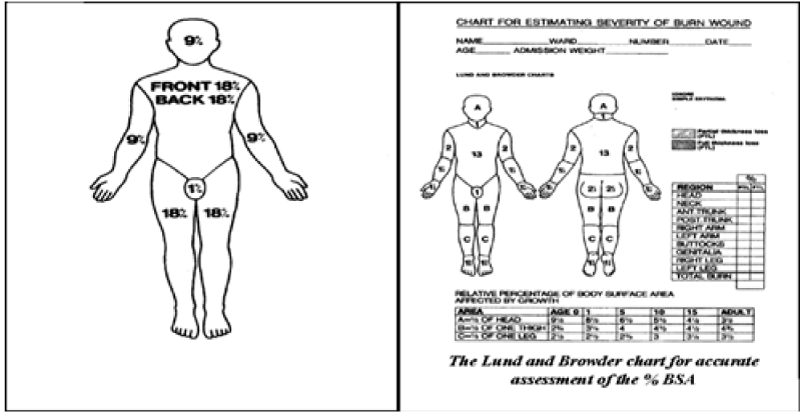
There are many ways to assess the total body surface area burnt (Figure 2).
Figure 2 :Assessment of Body Surface Area.
1. Rule of 9’s
Is a quick, but not accurate, way of estimating, the surface area that is affected by a burn.
- Face & Scalp 9%
- Anterior trunk 18%
- Posterior trunk 18%
- Upper limb each 9%
- Lower limb each 18%
- Perineum 1%
- Sally Abston, Patricia Blakeney, Manubhai Desai, Patricia Edgar, John Heggers, David N Herndon, et al. Acute Burn management, Total Burn Care, Resident Orientation Manual February. 2000.
- Victor Zielinki, Burn management- New Treatments, Burn management Journal. 2007.
- Warwick A Ames. Anaestetic Management of the Major Burn, Update in anaesthesia. 1999; 53-56.
- Holm C. Resuscitation in shock associated with burns. Tradition or evidence-based medicine? Resuscitation. 2000; 44: 157-164.
- Webb R. “Crystalloid or Colloid for Resuscitation. Are We Any the Wiser?” Critical Care. 1999; 3: 25-28.
- Tricklebank S. “Modern Trends in Fluid Therapy for Burns,” Burns. 2009; 35: 757-767.
- Baxter CR, Shires T. “Physiological Response to Crystalloid Resuscitation of Severe Burns,” Annals of the New York Academy of Sciences. 1968; 150: 874-894.
- Martin C. Robson, Brian F. Burns. Treatment of the Burns Victim. Cuschiere A, Giles GR, Moosa AR. 3rd edn. Essential Surgical Practice, Butterworth-Heinemann Ltd 1995, 554-700.
- Medhat Emil Habib, Said Al-Busaidi, Gihan Adly Latif, Ali Saleem Mehdi, Thomas C. The Combination of Parkland Formula, Using Normal Saline, with Muir & Barclay Formula for Fluid Resuscitation in the Initial Burn Shock Period. Modern Plastic Surgery. 2013; 3: 142-149.
In children the head is about 18% of the total body surface area with less area of the lower limbs.
2. A good way of estimating burns is by considering that the patient’s hand is 1% of his surface area [2].
3. The Lund and Browder Chart
Is a more accurate way of assessment? It facilitates proper estimation of the burnt area in different ages.
Depth of Burn
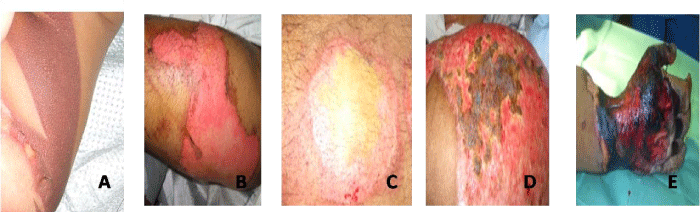
The depth of burn is important in evaluating the severity of the burn, planning for wound care and predicting functional and cosmetic results (Figure 3).
Figure 3 :Evaluating the severity of the burns: A) First-degree burns B) Second-degree burns: Superficial partial-thickness burn injury C) Second-degree burns: Deep partial-thickness burn injury D) Third degree or full-thickness burns E) Fourth-degree burns.
1. First–degree burns involve the epidermis layer of the skin. It is characterized by pain, erythema, and lack of blisters. These burns heal without scar formation. First–degree burns are not considered in calculation of the total body surface area (TBSA) burned and do not require intravenous fluid replacement therapy.
2. Second–degree burns or Dermal Burns are subdivided into superficial and deep partial–thickness burns.
Superficial partial–thickness burn injury involves the papillary dermis, containing pain–sensitive nerve endings. Burn Blisters or bullae are present, and the burns usually appear pink and moist. These burn injuries heal with little or no scarring.
Deep partial–thickness burn injury damages both the papillary and reticular dermis. These injuries may not be painful and often appear white or mottled pink. Deep partial–thickness burns can produce significant scarring.
3. Third degree or full–thickness burns involve all layers of the epidermis and dermis and may destroy subcutaneous structures. They appear white or charred. These burns are insensate because of destruction of nerve endings. Third–degree burns are best treated with skin grafting to limit scarring.
4. Fourth–degree burns involve structures beneath the subcutaneous fat, including muscle and bone [2].
Flow Sheet
The intake and output should be calculated and all the medications given to the patient should be mentioned.
Baseline Determinations for the Major Burn Patient
1. Laboratory Investigations: Routine blood investigations have to be done. Arterial blood gas analysis and carboxyhaemoglobin are required in cases of inhalation burns. Cardiac enzymes level and myoglobin in urine are required in cases of electrical injuries.
2. Other investigations: X–ray chest is required in inhalation burns. X–rays may also be required in appraisal of associated injuries. ECG is required in cases of electrical burns.
Circumferential Extremity Burns: Maintain Peripheral Circulation
1. Remove jewelry, watch, etc.
2. Assess the status of the distal circulation, checking for cyanosis, impaired capillary filling, or progressive neurological signs as paraesthesia and deep tissue pain. All extremities, especially with deep circumferential burns, should be examined for pulses. If pulses are absent, and fluid resuscitation is adequate, the involved limb should undergo urgent escharotomy for release of the constrictive, unyielding eschar. Escharotomies are generally performed at the bedside under IV sedation using electrocautery. Midaxial incisions are completed through the bleeding tissue, extending the full length of the eschar to assure adequate release. Limbs should be elevated above heart level.
3. Occasionally, escharotomy alone will fail to relieve intracompartmental pressures and a formal fasciotomy is indicated. This may be required in patients with associated skeletal trauma, crush injury, or burns involving tissues beneath the investing fascia [1].
Gastric Tube Insertion
A nasogastric (NG) tube should be placed in all intubated patients and in most of the patients with major burns [2]. Enteral nutrition should be started as early as possible to provide nutrition to, and avoid breakdown of, the enterocytes lining the GIT mucosa. In case of abdominal distension, aspiration can be done through the tube.
Narcotics, Analgesics and Sedatives
Narcotics, analgesics and sedatives should be administered mostly by the intravenous route either in small frequent doses or preferably as a continuous intravenous infusion. Patient controlled analgesia (PCA) is an effective aid in this regard.
Wound Care
Silver containing dressing materials are the most commonly used types of dressings nowadays. Early involvement of the physiotherapist in the burn management is important [2].
Antibiotics
Prophylactic antibiotics are not indicated in small burns. Major Burns require the administration of antibiotics based on the culture sensitivity tests.
Tetanus
Determination of the patient’s tetanus immunization is important.
Psychiatric Assistance
Burn patients often suffer from psychiatric disorders which may be the cause of burns e.g. suicidal attempt or may be a result of the burn including pain, anxiety, posttraumatic stress disorders, fear of disfiguring and fear of death. Early psychiatric support is of fundamental importance to these patients.
Conclusion
Initial burn resuscitation requires obtaining a brief history about the circumstances of the burn with immediate attention to the airway, breathing and fluid resuscitation of the patient as primary survey steps. Secondary survey measures include physical examination of the patient for other injuries and assessment of the percentage and the depth of the burns. Intake and output should be measured and base line investigations should be obtained. Proper analgesia, wound care, psychiatry and physiotherapy management are fundamental aspects in the treatment of these patients.
References