
Research Article
Austin J Womens Health. 2015;2(1): 1009.
Hormonal and Her2 Receptor Immunohistochemistry of Breast Cancers in Ile-Ife, Nigeria
Omoniyi-Esan GO¹, Olaofe OO²*, Aremu OA³,Omonisi AE4, Olasode BJ5 and Adisa OA6
¹Department of Morbid Anatomy & Forensic Medicine, College of Health Sciences, Obafemi Awolowo University, Nigeria
²Department of Morbid Anatomy & Forensic Medicine, College of Health Sciences, Obafemi Awolowo University, Nigeria
³Departments of Morbid Anatomy & Forensic Medicine, Obafemi Awolowo University Teaching Hospital, Nigeria
4Departments of Morbid Anatomy & Forensic Medicine, Obafemi Awolowo University Teaching Hospital, Nigeria
5Department of Morbid Anatomy & Forensic Medicine, College of Health Sciences, Obafemi Awolowo University, Nigeria
6Department of Surgery, College of Health Sciences, Obafemi Awolowo University, Nigeria
*Corresponding author: Dr. Olaofe OO, Department of Morbid Anatomy & Forensic Medicine, College of Health Sciences, Obafemi Awolowo University, Nigeria
Received: April 03, 2015; Accepted: May 28, 2015; Published: May 29, 2015
Abstract
Aim: The aim of this study was to assess Estrogen Receptor (ER), Progesterone Receptor (PR) and ErB B2 receptor (Her2) status of Breast cancers in Obafemi Awolowo University Teaching Hospitals Complex (OAUTHC), Ile-Ife, Nigeria.
Materials and Method: A 5-year prospective study was done of all Breast cancers in Department of Morbid Anatomy and Forensic Medicine, OAUTHC, Ile-Ife, Nigeria, from January 2007 to December 2012.
Results: A total of 136 cases of Breast cancers were seen in the study period. Immunohistochemistry was done on all these cases. The mean age was 50.7±13.5 SD (yrs). The age range was 23-92 yrs. Phenotypic classification based on ER, PR and Her2 immunohistochemistry show 45 cases (33.1%) to be Basal-like (Triple negative), 30 cases (22.1%) are Her2 over expressing, 21 cases (15.4%) are Luminal B type, 20 cases (14.7%) are luminal A type.
Conclusion: A significant number of cases is Estrogen receptor positive; hence in a resource poor setting like ours, the use of anti-estrogens in treatment of breast cancer cases with unknown receptor status may be justified as these drugs are known to be relatively cheap. It is not possible to predict the breast cancer phenotypes by using the age at presentation.
Keywords: Breast Cancer; Hormonal Receptor; Immunohistochemistry
Abbreviations
ER: Estrogen Receptor; PR: Progesterone Receptor; Triple Neg: Triple Negative; OAUTHC: Obafemi Awolowo University Teaching Hospitals Complex; FNAC: Fine Needle Aspiration Cytology
Introduction
Breast cancer is a malignant neoplasm with a huge mental and financial burden in Nigeria [1]. It is known to cause up to 50% of all malignancies in females [2,3]. Breast cancer is known to have a relatively high mortality rate in African women [4,5]. This cancer apart from causing a significant mortality also markedly reduces the quality of life of the patient. Although there is relatively good awareness of breast cancer in some communities in Nigeria, substantial number of people still seems to be ignorant of the disease.
Some molecular studies have been done on breast cancers to identify the genetic or hereditary factors that contribute to the genesis of the disease. Many of these studies have identified a small but significant number of genetic mutations [6-8]. Identification of genetic mutations in families is important in preventive efforts. Despite identification of genetic factors in aetiology of the disease, only a few respondents in a study will agree for a prophylactic mastectomy if necessary [9].
Even though new molecules of clinical significance have been identified in Nigerian women [10], the Estrogen Receptor (ER), Progesterone Receptor (PR) and Her2 receptor statuses are still of utmost clinical significance. The standard treatment protocols in use today revolve around ER, PR, and Her2 receptor expression by the malignant cancer cells. This is used to determine treatment in patients who can afford the related drugs. There have been various efforts to introduce new drugs to treatment of these cases but most new drugs are expensive and hence not readily available.
In many cases of breast cancer in Nigeria, presentation to the hospital is relatively late; hence, the standard therapeutic modified radical mastectomy cannot be used. Chemotherapy is used for these patients [11-14]. It is therefore very important to study the receptor status of breast cancer to know its relationship with clinical data and its possible influence in our resource limited treatment protocol.
Aim
The aim of this study was to assess ER, PR and Her2 receptor status of Breast cancers in Obafemi Awolowo University Teaching Hospitals Complex (OAUTHC), Ile-Ife, Nigeria and to relate the findings with the age of the patient.
Materials and Methods
A 5-year prospective study was done of all Breast cancers in Department of Morbid Anatomy and Forensic Medicine, OAUTHC, Ile-Ife, Nigeria, from January 2007 to December 2012. The whole population of breast cancer cases seen in this period was included in the study. There was no sampling done. Inclusion criteria were all cases of breast cancer with tissue biopsy and conclusive histological diagnosis. Cases with incomplete data and inadequate tissue biopsy were excluded from the study. Relevant clinical data was extracted from histological request forms and case notes.
The cancer tissues were routinely fixed in buffered formalin. The tissues were further processed in an Automatic tissue Processor. Histologic diagnoses were made from haematoxylin and eosin stained sections obtained from the paraffin wax tissue blocks.
The sections from each representative block were subjected to immunohistochemistry. A standard immunohistochemistry protocol was used. 3-3’Diaminobenzidine tetrahydrochloride was used as chromogen and haematoxylin was used as counter stain. Immunohistochemical staining for estrogen receptor, progesterone receptor and Her2/neu were carried out retrospectively on sections from the processed tissue blocks. A standard positive control was used with each batch to ensure consistency between batches. A negative control was also used for standardization. The standard positive and negative controls were obtained from tissue blocks used for routine procedures in the laboratory.
Data analysis
The results obtained were analyzed using Statistical Package for Social Sciences version 15. The results were presented in charts. Chi square tests were used. The level of statistical significance was put at P = 0.05
Results
A total of 136 cases of Breast cancers were seen in the study period. Immunohistochemistry was done on all these cases. The data on age was available in 131 out of the 136 cases. Most of the cases were from biopsies (85 - 62.5%) while mastectomy accounted for the rest (51 - 37.5%). Females account for the overwhelming majority with 132 cases (97.1%) while males account for 4 cases (2.9%).
The mean age was 50.7±13.5 SD (yrs). The age range was 23-92 yrs. The age group 40-50 years account for the highest number of cases (46 cases- 35.1%) while the 50-60 yrs age-group account for the second highest with 28 cases (21.3%). The distribution of the cases in these age groups and others can be seen in (Figure 1).
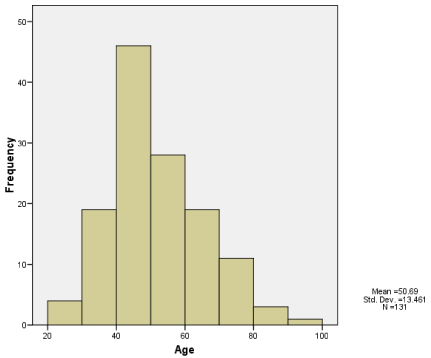
Figure 1: Age Distribution of Cases.
Above shows the age distribution of breast cancer cases with age group 40-
50 years recording the highest occurrence.
The histological diagnosis of most of the cases was in filtrating ductal carcinoma (Not otherwise specified). This accounts for 128 cases (94%). Mucinous carcinoma accounts for 4 cases (2.9%), metaplastic carcinoma accounts for 3 cases (2.2%) and microsecretory carcinoma accounts for 1 case (0.7%).
The cases positive for Estrogen Receptor (ER) were 47(34.6%) while 89(65.4%) were negative. The cases positive for Progesterone Receptor (PR) were 34(25%), while 102 (75%) were negative. Fiftytwo (38.2%) were positive for Her2 receptors, 64(47.1%) were negative and 20 (14.7%) were equivocal. The equivocal cases were not further analyzed using In-situ hybridization as facilities for this was not available.
Out of the 47 cases positive for ER, 30 were also positive for PR, while 17 were negative for PR. Thirty of the 34 cases positive for PR were found to be positive for ER, while 4 cases were found to be negative. Pearson Chi-square test show a strong association between ER and PR positivity, Χ² (1, N = 136) = 57.8, p < 0.001. There was however no association between Her2 and PR, Χ² (2, N = 136) = 1.4, p = 0.497 nor between Her2 and ER, Χ² (2, N = 136) = 3.554, p = 0.169.
Phenotypic classification based on ER, PR and Her2 immunohistochemistry show 45 cases (33.1%) to be Basal-like (Triple negative), 30 cases (22.1%) are Her2 over expressing, 21 cases (15.4%) are Luminal B type, 20 cases (14.7%) are luminal A type. Twenty cases (14.7%) with equivocal Her2 expression could not be sub-classified. Analysis of the male cases shows 3 to be of luminal a phenotype.
The mean age of the basal-like cases was 50.4±14.6SD (yrs) with the age range 23-85 years. The mean age of theHer2 over expressing cases was 52.4±13.8SD (yrs) with the age range 31-92 years. The mean age of the luminal B cases was 48.1±11.5SD (yrs) with the age range 30-73 years. The mean age of the luminal A cases was 52.8±10.8SD (yrs) with the age range 35-82 years. The ages of these cases and their distribution can be seen in (Figure 2).
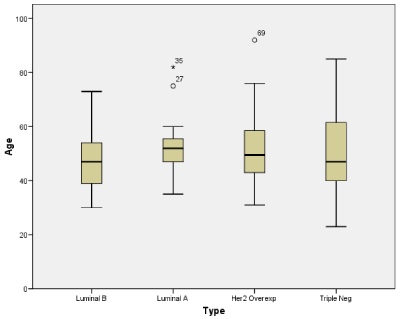
Figure 2: Box Plot Showing Age Distribution of the Various Sub-Types.
The box-plot above show a relatively even mean age of the various immunephenotypes
of breast cancer cases.
Discussion
Our study showed the mean age of breast cancer to be 50.7 years and the 40-50 year age group to have the highest number of cases. Females were found to be comparatively much more affected by breast cancer with only 2.9% found in males. We discovered that modified radical mastectomy was only done in 37.5% of cases with others being biopsies. A significant number of the breast cancers seen in our study were estrogen receptor positive (34.6%) with little or no differences in the ages of the different phenotypes. The triple negative cases were found to account for 33.1% of all cases. Expectedly, the expression of progesterone receptor was significantly associated with the expression of estrogen receptor.
The age distribution of breast cancer cases in our study suggests the need to make available, screening programs like mammography for women above 20 years with special emphasis on women above 40 years. This is important as there is no efficient, widely accessible screening program in our region. The screening protocol should involve all women above 20 years with frequency of screening increased in women above 40 years. Omoniyi-Esan et al had found the use of Fine Needle Aspiration Cytology (FNAC) to be an added genuine tool in a low resource locale as ours [15]. Although females are relatively overwhelmingly affected by breast cancer, finding cases in males makes it important to re-emphasize that they can also develop the disease. It is necessary to stress this because breast cancer in males in Nigeria had been associated with poor outcome [16].
We also noted that modified radical mastectomy was only done in 37.5% of cases with others being biopsies. A previous study in the study centre had found late presentation of cases to be preponderant [17]. The low proportion of mastectomy is most probably explained by the late presentation when only neoadjuvant chemotherapy could be done.
Women of African descent, particularly of West African Origin, are known to have a higher prevalence of ER negative tumours compared with white Europeans and East-African born blacks [18]. Although most reports had shown the preponderance of triple negative breast cancers in Nigeria, it is interesting to note that a significant amount is estrogen receptor positive (34.6%). Hence in a resource poor setting, the blind use of anti-oestogens (without knowing the receptor status) may be justified as these drugs are known to be relatively cheap.
Expectedly, expression of progesterone receptor significantly correlates with the expression of estrogen receptor. This is because progesterone receptor expression is physiologically related to expression of estrogen receptor.
The triple negative cases accounted for the highest proportion of all cases. This conforms to reports from other studies in Nigeria [4,17]. Treatment outcome in late stages of triple negative tumours are relatively poor as they are not sensitive to many chemotherapeutic agents. These triple negative cases are best diagnosed at an early stage and then excised. Our study further emphasizes the need for early diagnosis for appropriate application of curative surgical modalities.
The results also show little or no differences in the ages of the different phenotypes. This means that it is not possible to predict the phenotypes by the age at presentation.
We suggest more efforts be geared towards increasing the awareness of the disease. Awareness is the first battle against the scourge. Although many women are aware of the disease, total awareness should be the target [19].
Conclusion
A significant number of cases is Estrogen receptor positive; hence in a resource poor setting like ours, the use of anti-estrogens in treatment of breast cancer cases with unknown receptor status may be justified as these drugs are known to be relatively cheap. It is not possible to predict the breast cancer phenotypes by using the age at presentation.
References
- Nuhu FT, Adebayo KO, Adejumo O. Quality of life of people with cancers in Ibadan, Nigeria. J Ment Health. 2013; 22: 325-333.
- Awolola NA, Komolafe AO, Ojo OO, Taiwo OJ, Odesanmi WO, Ajumobi KO. The spectrum of malignant neoplasms in Ekiti State, south-west Nigeria. Nig Q J Hosp Med. 2011; 21: 276-283.
- Njeze GE. Breast lumps: a 21-year single-center clinical and histological analysis. Niger J Surg. 2014; 20: 38-41.
- Ijaduola TG, Smith EB. Pattern of breast cancer among white-American, African-American, and nonimmigrant west-African women. J Natl Med Assoc. 1998; 90: 547-551.
- Amend K, Hicks D, Ambrosone CB. Breast cancer in African-American women: differences in tumor biology from European-American women. Cancer Res. 2006; 66: 8327-8330.
- Gao Q, Adebamowo CA, Fackenthal J, Das S, Sveen L, Falusi AG, et al. Protein truncating BRCA1 and BRCA2 mutations in African women with pre-menopausal breast cancer. Hum Genet. 2000; 107: 192-194.
- Zhang B, Fackenthal JD, Niu Q, Huo D, Sveen WE, DeMarco T, et al. Evidence for an ancient BRCA1 mutation in breast cancer patients of Yoruban ancestry. Fam Cancer. 2009; 8: 15-22.
- Oluwagbemiga LA, Oluwole A, Kayode AA. Seventeen years after BRCA1: what is the BRCA mutation status of the breast cancer patients in Africa? - a systematic review. Springerplus. 2012; 1: 83.
- Oguntola AS, Olaitan PB, Omotoso O, Oseni GO. Knowledge, attitude and practice of prophylactic mastectomy among patients and relations attending a surgical outpatient clinic. Pan Afr Med J. 2012; 13: 20.
- Agboola AO, Musa AA, Ayoade BA, Banjo AA, Anunobi CC, Deji-Agboola AM, et al. Clinicopathological and molecular significance of Sumolyation marker (ubiquitin conjugating enzyme 9 (UBC 9) expression in breast cancer of black women. Pathol Res Pract. 2014; 210: 10-17.
- Arowolo OA, Njiaju UO, Ogundiran TO, Abidoye O, Lawal OO, Obajimi M, et al. Neo-adjuvant capecitabine chemotherapy in women with newly diagnosed locally advanced breast cancer in a resource poor setting (Nigeria): efficacy and safety in a phase II feasibility study. Breast J. 2013; 19: 470-477.
- Azubuike S, Okwuokei S. Knowledge, attitude and practices of women towards breast cancer in benin city, Nigeria. Ann Med Health Sci Res. 2013; 3: 155-160.
- Ogundiran TO, Ayandipo OO, Ademola AF, Adebamowo CA. Mastectomy for management of breast cancer in Ibadan, Nigeria. BMC Surg. 2013; 13: 59.
- Makanjuola SB, Popoola AO, Oludara MA. Radiation therapy: a major factor in the five-year survival analysis of women with breast cancer in Lagos, Nigeria. Radiother Oncol. 2014; 111: 321-326.
- Omoniyi-Esan G, Osasan S, Titiloye N, Olasode B. Cytopathological Review of Breast lesions in Ile-Ife Nigeria. The Internet Journal of Third World Medicine. 2008; 8.
- Ahmed A, Ukwenya Y, Abdullahi A, Muhammad I. Management and outcomes of male breast cancer in zaria, Nigeria. Int J Breast Cancer. 2012; 2012: 845143.
- Adisa AO, Arowolo OA, Akinkuolie AA, Titiloye NA, Alatise OI, Lawal OO, et al. Metastatic breast cancer in a Nigerian tertiary hospital. Afr Health Sci. 2011; 11: 279-284.
- Jemal A, Fedewa SA. Is the prevalence of ER-negative breast cancer in the US higher among Africa-born than US-born black women? Breast Cancer Res Treat. 2012; 135: 867-873.
- Bello M. Awareness is the first step in battle against breast cancer. Bull World Health Organ. 2012; 90: 164-165.