
Case Report
Austin J Womens Health. 2015; 2(2): 1014.
Apical Myocardial Thickening in a Patient with Stroke and Takotsubo Stress Cardiomyopathy
Vazquez DLF¹, Cheong BY² and Hernandez-Vila EA²*
¹Department of Internal Medicine, Hospital Angeles Puebla, USA
²Department of Cardiology, Texas Heart Institute, USA
*Corresponding author: Hernandez-Vila EA, Department of Cardiology, Texas Heart Institute, USA
Received: July 16, 2015; Accepted: November 02, 2015; Published: November 04, 2015
Abstract
Takotsubo Cardiomyopathy (TC) is characterized by akinesis and ballooning of the left ventricle and since its initial report in 1991, has gained recognition as an important cause of acute heart failure. The relationship of TC and stroke is well known, however, it is often challenging to determine causality between these two entities. We present a case of a 41-year-old woman who presented to the Emergency Department with altered mental status and weakness. The patient was diagnosed with stroke and TC that presented with the unusual finding of apical thickening on cardiac imaging.
Keywords: Takotsubo; Stress cardiomyopathy; Stroke; Apical disease; Apical hypertrophy
Case Presentation
A 41-year-old African-American woman who was found unconscious at home by her husband, presented to the Emergency Department with altered mental status and weakness. Her medical history included diabetes mellitus type II, hypertension, hyperlipidemia and Sjogren’s syndrome. Her temperature was 36.5°C; heart rate, 76 beats/min; blood pressure, 126/70 mmHg; respiratory rate, 18 breaths/min; and oxygen saturation, 97% on room air. Physical examination revealed aphasia; eyes deviated to the left side and right sided weakness. Initial score on the National Institutes of Health Stroke Scale was 23, indicating a severe stroke.
The patient’s admission Electrocardiogram (ECG) showed diffuse T wave inversion in the inferior and anterolateral leads with a prolonged QT interval (Figure: 1). A previous ECG taken 3 years ago was normal (Figure: 2). Initial laboratory studies indicated normal CK and CK-MB levels and a negative troponin I. A gradual elevation of troponin I was observed and became maximally elevated 5 hours after admission at 0.1ng/ml (Reference: <0.04 ng/ml). Brain Natriuretic Peptide (BNP) was found to be elevated at 391pg/ml.
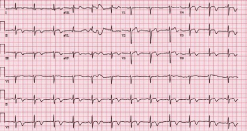
Figure 1: ECG at admission demonstrated diffuse T wave inversion that
extended beyond the territory of any single coronary artery. QT prolongation
was also observed (QTc = 468 ms).
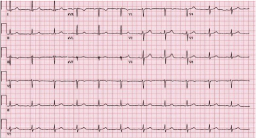
Figure 2: Normal ECG of the patient 3 years prior to presentation.
The patient underwent cerebral angiogram, with successful mechanical embolectomy of the left distal internal carotid artery and M1 and superior and inferior M2 segments of the left middle cerebral artery.
On the 2nd hospital day, a Transthoracic Echocardiogram (TTE) revealed decreased Left Ventricular Ejection Fraction (LVEF) of 45- 49% and apical akinesis (Figure: 3). These changes were compared to a prior TTE performed in 2010 which was unremarkable. A Transesophageal Echocardiogram (TEE) was performed two days later and confirmed the akinesis of all apical segments with a decreased overall left ventricular systolic function, but a source of thrombus was not found. Upon further questioning, the patient reported that she felt severe chest pain prior to becoming unconscious, strongly suggesting the possibility of cardioembolism as the culprit.
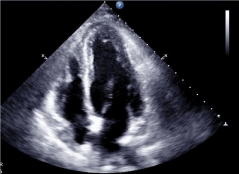
Figure 3: Transthoracic echocardiogram exhibiting apical akinesis and
ballooning.
A repeat TTE was performed on the 8th hospital day which showed resolution of the apical akinesis with normalization of LVEF. Interestingly, this study revealed the new finding of a small Left Ventricle (LV) suggestive of mild apical hypertrophy. A contrast agent for LV opacification was used to better delineate the chamber (Figure: 4). Nine days after presentation, ECG changes persisted with evolutionary changes consistent with stress cardiomyopathy (Figure: 5). Cardiac Magnetic Resonance (CMR) with and without contrast was performed prior to discharge, to assess apical wall motion abnormalities and determine myocardial viability and damage. This study found a normal LV size with a normal LVEF of 62%. Apical ballooning was not seen, but the study confirmed the finding of mild thickening of the apex in the prior TTE. It was also able to determine the absence of prior myocardial damage and abnormal myocardial enhancement (Figure: 6).

Figure 4: Transesophageal echocardiogram with contrast demonstrating
apical thickening.
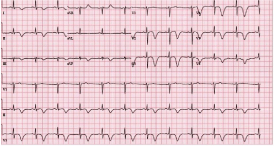
Figure 5: Giant inverted T waves and QT prolongation (QTc = 518 ms)
were observed nine days after presentation, consistent with the evolutionary
changes found in the recovery phase of Takotsubo cardiomyopathy.

Figure 6: Cardiac magnetic resonance displaying mild thickening with
obliteration of the apex in systole and diastole.
Discussion
The relationship between stroke and TC is well known [1,2] and determining the relation of cause and effect is often challenging [3]. Furthermore, the diagnosis is complicated because TC often mimics acute myocardial infarction and the presence of coronary artery disease does not necessarily exclude TC [4]. The criteria for diagnosing TC include transient hypokinesis, akinesis or dyskinesis in the left ventricular mid-segments with or without apical involvement (apical pattern being the most commonly found abnormality), absence of obstructive coronary disease, new ECG abnormalities (ST segment elevation and/or T-wave inversion) or modest elevation in cardiac troponin and the absence of pheochromocytoma and myocarditis [5]. In our patient the clinical presentation along with the cardiac biomarker profile and cerebral angiogram suggested a non-ischemic cause for her symptoms.
Epidemiological studies have found that of all patients presenting to the hospital with a suspected acute coronary syndrome 2% will be ultimately diagnosed with TC. In women the incidence can be as high as 10% [6]. This condition is more common in older post-menopausal women and has been mainly described in the Asian and Caucasian populations [7]. Nevertheless, because awareness of this condition has increased in recent years, the number of cases in other populations is expanding [6]. TC is thought to be precipitated by excess sympathetic activity, often secondary to a stressful event. Coronary vasopasm, disorder of the microcirculation and lack of estrogen have also been proposed as alternative causes [5].
Our patient presented with the sequence of chest pain prior to stroke implying the possibility of cardioembolism. Myocardial infarction was reasonably excluded due to the absence of a significant elevation in CK, CK-MB and a mildly elevated troponin, that quickly began down trending the next day after admission, indicating minimal myonecrosis. BNP levels were elevated at the time of admission, indicating a certain degree of ventricular dysfunction. This marker has been found to be elevated in almost all TC patients and in higher concentrations when compared with STEMI and NSTEMI patients [8].
The patient had no previous history. Of coronary artery disease and her ECG was characteristic of TC, demonstrating the classic diffuse T wave inversion [9]. Our patient also had no previous history of CAD with a prior calcium score of 0 which was measured as an outpatient before this event. A thrombus was not found on cardiac imaging, however; since thromboembolism has been found to be a common complication in TC [10], and no other potential source of thrombi were detected on cardiac imaging, we believe thromboembolism from TC is the most likely explanation in this case.
The CMR confirmed the apical thickening seen in the prior TTE which is an unusual finding in the setting of a suspected stress cardiomyopathy [11]. Even though the apical thickness was measured at only 6 mm on CMR, not meeting the criteria for true apical hypertrophy; the apical thinning towards the apex that is characteristic of normal individuals was absent in our patient [12].
In conclusion, we present a case of TC and stroke with the unusual finding of apical thickening in which CMR played a key role in confirming the resolution of the apical akinesis and the improvement in LVEF. This highlights the increasing importance of CMR to distinguish TC from ischemia, infarction and other myocardial diseases [13-15].
References
- Gregorio DC, Grimaldi P, Lentini C. Left ventricular thrombus formation and cardioembolic complications in patients with Takotsubo-like syndrome: a systematic review. Int J Cardiol. 2008; 131: 18-24.
- Young ML, Stoehr J, Aguilar MI, Fortuin FD. Takotsubo cardiomyopathy and stroke. Int J Cardiol. 2014; 176: 574-576.
- Y-Hassan S, Winter R, Henareh L. The causality quandary in a patient with stroke, Takotsubo syndrome and severe coronary artery disease. J Cardiovasc Med (Hagerstown). 2015; 2: 118-121.
- Prasad A, Lerman A, Rihal CS. Apical ballooning syndrome (Tako-Tsubo or stress cardiomyopathy): a mimic of acute myocardial infarction. Am Heart J. 2008; 155: 408-417.
- Yoshikawa T. Takotsubo cardiomyopathy, a new concept of cardiomyopathy: clinical features and pathophysiology. Int J Cardiol. 2015; 182: 297-303.
- Sharkey SW, Maron BJ. Epidemiology and clinical profile of Takotsubo cardiomyopathy. Circ J. 2014; 78: 2119-2128.
- Donohue D, Movahed MR. Clinical characteristics, demographics and prognosis of transient left ventricular apical ballooning syndrome. Heart Fail Rev. 2005; 10: 311-316.
- Ahmed KA, Madhavan M, Prasad A. Brain natriuretic peptide in apical ballooning syndrome (Takotsubo/stress cardiomyopathy): comparison with acute myocardial infarction. Coronary artery disease. 2012; 23: 259-264.
- Thakar S, Chandra P, Hollander G, Lichstein E. Electrocardiographic changes in Takotsubo cardiomyopathy. Pacing Clin Electrophysiol. 2011; 34: 1278-1282.
- Mitsuma W, Kodama M, Ito M, Kimura S, Tanaka K, Hoyano M, et al. Thromboembolism in Takotsubo cardiomyopathy. Int J Cardiol. 2010; 139: 98-100.
- Roy RR, Hakim FA, Hurst RT, Simper D, Appleton CP. Two cases of apical ballooning syndrome masking apical hypertrophic cardiomyopathy. Texas Heart Institute journal / from the Texas Heart Institute of St Luke's Episcopal Hospital. Texas Children's Hospital. 2014; 41: 179-183.
- Cisneros S, Duarte R, Fernandez-Perez GC, Castellon D, Calatayud J, Lecumberri I, et al. Left ventricular apical diseases. Insights Imaging. 2011; 2: 471-482.
- Eitel I, Von Knobelsdorff-Brenkenhoff F, Bernhardt P, Carbone I, Muellerleile K, Aldrovandi A, et al. Clinical characteristics and cardiovascular magnetic resonance findings in stress (takotsubo) cardiomyopathy. Jama. 2011; 306: 277-286.
- Nowak R, Jaguszewski M, Fijalkowski M, Fijalkowska M, Gruchala M. CMR to distinguish Takotsubo cardiomyopathy from myocardial infarction in acute course of ischemic stroke in a male patient. International journal of cardiology. 2015; 184: 397-398.
- Kedar J, Pandey T, Kaushik C, Viswamitra S, Molavi B. Magnetic resonance imaging findings in apical ballooning syndrome or takotsubo cardiomyopathy. Indian heart journal. 2012; 64: 99-102.