
Research Article
Austin J Womens Health. 2016; 3(1): 1019.
Surgical Replacement of the Uterosacral- and Pubourethral-Ligaments as Treatment for Urgency Urinary Incontinence
Ludwig S*, Stumm M, Mallmann P and Jager W*;
Department of Obstetrics and Gynecology, University of Cologne, Germany
*Corresponding author: Jager W and Ludwig S, Abteilung Gynakologie und Geburtshilfe, Department of Obstetrics and Gynecology, Universitat zu Köln, Kerpener Strasse 34, 50931 Köln, Germany
Received: December 16, 2015; Accepted: March 25,2016; Published: March 29, 2016
Abstract
Aim: The bilateral replacement of the uterosacral ligaments was developed for the treatment of female pelvic organ prolapse. The aim of the present study was to evaluate the effect of this treatment on Mixed Urinary Incontinence (MUI) and Urgency Urinary Incontinence (UUI) in patients with minor prolapse.
Materials and Methods: This was a retrospective study of 71 women suffering from MUI and UUI. Previous conservative treatments had failed. They were operated by Cervico-Sacropexy (CESA) or Vagino-Sacropexy (VASA).
All patients had apical vaginal prolapse (POP-Q stage I - II). Urinary incontinence was classified according to validated urinary incontinence questionnaires. The outcome was evaluated 4 months after surgery. Patients who were still urinary incontinent received an additional Transobturator Tape (TOT). The final outcome was assessed 4 months thereafter.
Results: 71 patients suffering from MUI and UUI with POP-Q stage I - II were surgically treated by CESA (n=26) and VASA (n=45). After CESA and VASA, the apical vaginal prolapse was repaired in all patients. 16 patients (62%) of the CESA group and 15 patients (33%) of the VASA group were cured of their urinary incontinence. The uncured patients agreed to an additional TOT and 53% of them were cured after this procedure. An overall cure rate for MUI and UUI of 77% was obtained by CESA and 71% by VASA.
Conclusion: Besides the repair of genital prolapse, the bilateral replacement of the uterosacral ligaments by CESA or VASA cured 33% to 62% of patients who suffered from MUI and UUI. After a TOT an overall cure rate ranging from 71% to 77% was observed
Keywords: Urgency urinary incontinence; Mixed urinary incontinence; Uterosacral ligaments; Cervico-Sacropexy; Vagino-Sacropexy
Abbreviations
BBUSQ-22: Birmingham Bowel and Urinary Symptoms Questionnaire; CESA: Cervico-Sacropexy; ICIQ-UI-SF: International Consultation on Incontinence Modular Questionnaire; MUI: Mixed Urinary Incontinence; OAB-SS: Overactive Bladder Symptom Score; POP: Pelvic Organ Prolapse; POP-Q: Pelvic Organ Prolapse Quantification System; PUL: Pubourethral Ligament; PVDF: Polyvinylidene Fluoride; SUI: Stress Urinary Incontinence; TOT: Transobturator Tape; UI: Urinary Incontinence; USL: Uterosacral Ligament; UUI: Urgency Urinary Incontinence; VASA: Vagino- Sacropexy
Introduction
In 2000, Barber et al. reported a new surgical procedure for the treatment of pelvic organ prolapse [1]. Basically, they sutured the apex of the vagina to the left and right Uterosacral Ligament (USL). Besides the “excellent anatomical correction of the prolapse“, they observed a “significant improvement of voiding function“ [1].
In 2003, Amundsen combined this bilateral uterosacral ligament fixation with a pubovaginal sling in patients who additionally suffered from Stress Urinary Incontinence (SUI) [2]. In all of their 33 patients, SUI was successfully treated after this combined procedure. However, the most remarkable observation in this study was that also 14 out of 17 (82%) patients suffering from Urgency Urinary Incontinence (UUI) were cured after these operations.
Barber and Amundsen focused their treatment on patients with advanced pelvic organ prolapse (POP-Q stages II– IV). However, the high cure rate of their combined treatment modality led us to hypothesize that a defect of the USL and Pubourethral Ligament (PUL) plays a critical role in the development of Mixed Urinary Incontinence (MUI) and UUI [3]. We therefore decided to offer women suffering from MUI and UUI even with less advanced pelvic organ prolapse (e.g. POP-Q stage I) a surgical replacement of the USL.
In contrast to Barber and Amundsen, we chose an abdominal approach because we decided to replace the defective USL. We sutured alloplastic (polyvinylidene fluoride, PVDF) USL tapes at the sacral bones and at the cervix (CESA) or vagina (VASA).
Besides the repair of prolapse, we analyzed the clinical outcome of 71 patients with UUI and MUI treated by CESA or VASA operation.
Materials and Methods
Patients
This study was initiated for patients suffering from Mixed Urinary Incontinence (MUI) and Urgency Urinary Incontinence (UUI) with otherwise asymptomatic pelvic organ prolapse. All patients had failed previous conservative treatments. They all had pelvic organ prolapse either of the uterus or vaginal vault, however, not reaching to the hymen (POP-Q stage I– II). All patients were operated by Cervico-Sacropexy (CESA) or Vagino-Sacropexy (VASA). If they still remained incontinent thereafter, they received a Transobturator Tape (TOT) in a second operation.
Exclusion criteria were Stress Urinary Incontinence (SUI) only, previous sacrospinous fixation, sacrocolpopexy, colposuspension and vaginal or abdominal pelvic mesh implantation.
All examinations and surgeries were performed at the Department of Obstetrics and Gynecology at University Hospital of Cologne, Germany.
All women underwent detailed internal genitalia urogynecological examination, preoperative cytology of the cervix and ultrasound screening. Details about previous operations (e.g. anterior colporrhaphy) were taken from the records.
Clinical examinations were performed before CESA or VASA and 4 months after the surgeries. The continence status was evaluated at that time by validated urinary incontinence questionnaires and personal interviews. A TOT was indicated when patients were not cured from their urinary incontinence after CESA or VASA. In these patients the follow-up was exactly the same as after CESA and VASA.
For the purpose of this report, patients who did not appear at follow-up examinations were excluded (“drop-outs“).
Evaluation of urinary incontinence
Urinary Incontinence (UI) was assessed and classified according to the recommendation of the ICS [4]. UI symptoms were based on micturition protocols and assessed by means of validated incontinence questionnaires (the Birmingham Bowel and Urinary Symptoms Questionnaire, BBUSQ-22, the International Consultation on Incontinence Modular Questionnaire, ICIQ-UI-SF and the Overactive bladder symptom score, OABSS) [5-7]. Whenever needed, a study nurse explained the questions to the patients.
For the purpose of this manuscript we deliberately decided to focus the analysis on the following three Questions:
Question 1: “How many times do you typically urinate from waking in the morning until sleeping at night?“
Question 2: “How often do you leak urine because you cannot defer the sudden desire to urinate?“
Question 3: “Does urine leak when you are active, exert yourself, cough or sneeze?“.
UUI was defined as =8 voids per day and / or involuntary urinary leakage =1 times a day. SUI was defined as urinary leakage during exercise, coughing or sneezing. MUI was defined as symptoms of both groups (UUI and SUI).
Evaluation of pelvic organ prolapse
Pelvic organ prolapse measurements were carried out according to the POP-Q system described by Bump et al. [8]. Patients were classified according to the apical descent, which is represented by POP-Q point C. The POP-Q measurements were done in lithotomyposition with Valsalva and cough maneuvers.
Operations
Cervico-sacropexy (CESA) and vagino-sacropexy (VASA): Cervico-sacropexy (CESA) or vagino-sacropexy (VASA) was performed; these are open abdominal surgical treatments described by Jager et al. [9]. In brief, specially designed Polyvinylidene Fluoride (PVDF) tapes (Dynamesh CESA, Dynamesh VASA, FEG Textiltechnik mbH, Aachen, Germany) were used to replace the Uterosacral Ligaments (USL) (Figure 1) [10,11].

Figure 1: Specially designed Polyvinylidene Fluoride (PVDF) tape (shown: Dynamesh CESA, FEG Textiltechnik mbH, Aachen, Germany).
They were placed in the peritoneal fold of the USL. In patients with a uterus, CESA was performed. After supra-cervical hysterectomy two PVDF tapes with the length of 8.8 cm were placed in the peritoneal fold of the USL bilaterally from the rectum [12]. These tapes were attached distally on the cervical stump and proximally to the presacral fascia in front of the S1 / S2 sacral vertebra by non-absorbable 2-0 sutures (Figure 2). In patients with total hysterectomy, VASA were performed using two PVDF tapes of 9.3 cm length placed at the vaginal stump on top of the vaginal cuff scar.
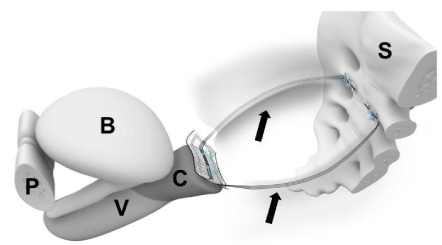
Figure 2: Position of a CESA tape. In patients with supracervical hysterectomy,
Cervico-Sacropexy (CESA) was performed by placing Polyvinylidene
Fluoride (PVDF) tapes in the peritoneal fold of the Uterosacral Ligaments
(USL) bilaterally from the rectum. These tapes were attached distally on
the cervical stump and proximal to the pre-sacral fascia in front of the S1
/ S2 sacral vertebra (In patients with total hysterectomy, Vagino-Sacropexy
(VASA) was performed using two PVDF tapes placed at the vaginal stump on
top of the vaginal cuff scar). S sacrum; C cervix; B bladder; V vagina; P pubic
bone; black arrows PVDF tape.
Transobturator tape: The transobturator tape was placed according to Delorme [13].
Definition of cure of MUI or UUI: The assessment of the clinical outcome was obtained 4 months after surgery. Furthermore, patients were contacted by a study nurse 12 months after surgery and thereafter. All patients were advised to contact our unit if urinary incontinence symptoms reappeared.
Cure of UUI was defined as =7 voids per day and no involuntary urinary leakage per day. Cure of SUI (only as part of MUI) was defined as no urinary leakage during exercise, coughing or sneezing. Cure of MUI was defined as cured UUI and cured SUI.
Data analysis
All measurements were documented on a Microsoft Excel database. Data were analyzed with SPSS (Version 21, Chicago, IL, USA) at a significance level of 5%. Chi-square-tests were used to detect differences between the groups at a level of statistical significance of p<0.05.
Details of Ethics Approval
Ethical approval for this study was obtained from the Local Ethics Commission of the Medical Faculty of the University of Cologne, Germany, in November 2012.
Results
71 patients suffering from MUI and UUI with pelvic organ prolapse were surgically treated by CESA and VASA (further referred as “CESA“ or “VASA“ group).
26 of these patients were operated by means of CESA and 45 patients by VASA. Most patients were older than 60 years, all patients had asymptomatic (no bulging feeling) pelvic organ prolapse (POP-Q stage I - II). No significant differences of the baseline clinical parameters between the CESA and VASA group were found (Table 1).
Parameter
CESA group
VASA group
p-value
(n=26)
(n=45)
mean (absolute range)
mean (absolute range)
Age, years
61 (28 - 81)
66 (44 - 83)
0.293
Body mass index
27 (17 - 39)
27 (17 - 45)
0.496
Parity
1 (0 - 4)
2 (0 - 6)
0.316
POP-Q stages
no.
no.
Stage 0
0
0
Stage I
22
44
Stage II
4
1
Stage III
0
0
Stage IV
0
0
Urinary incontinence questions
Options of response
no. (%)
no. (%)
p-value
Question 1
"How many times do you typically urinate
= 7 times a day
9 (35%)
19 (42%)
from waking in the morning until sleeping at
8 - 14 times a day
12 (46%)
14 (31%)
0.44
night?"
= 15 times a day
5 (19%)
12 (27%)
Question 2
'How often do you leak urine because you
0 time a day
3 (12%)
2 (4%)
cannot defer the sudden desire to urinate?"
1 - 4 times a day
11 (42%)
8 (18%)
0.02
5 times a day or more
12 (46%)
35 (78%)
Question 3
"Does urine leak when you are active, exert
0 time a day
7 (27%)
6 (13%)
0.154
Yourself, cough or sneeze?"
= 1 time a day
19 (73%)
39 (87%)
Table 1: Baseline clinical parameters and urinary incontinence questions of the 71 patients in the CESA and VASA group before surgery.
58 patients (82%) were suffering from MUI and 13 patients (18%) were suffering from UUI. In the VASA group more patients were suffering from MUI compared to the CESA group (Table 2). The most bothersome urinary incontinence symptom was urine leakage after sudden desire. Twenty-three patients (88%) of the CESA group and 43 patients (96%) of the VASA group lost urine =1 times a day. Twelve (46% in the CESA group) and 35 patients (78% in the VASA group) even lost urine =5 times a day. This problem was significantly more pronounced in the VASA group compared to the CESA group (Table 1). 19 patients (73%) in the CESA group and 39 patients (87%) in the VASA group complained of urine leakage with exercise, coughing or sneezing.
After CESA and VASA, all patients had a normal apical vaginal fixation (POP-Q stage 0). Regarding the urinary incontinence, cure (of MUI and UUI) was achieved in 16 out of 26 patients (62%) in the CESA group and in 15 out of 45 patients (33%) in the VASA group. 11 out of 19 patients (58%) with MUI were cured after CESA and 12 out of 39 patients (31%) with MUI were cured after VASA. After CESA, 5 out of 7 patients and after VASA 3 out of 6 patients were cured of their UUI.
Regarding the urinary incontinence symptoms, urinary leakage after sudden desire (=1 times a day) totally disappeared in more than 50% of patients in the CESA and VASA group. Additional symptoms of urine leakage with exercise, coughing or sneezing disappeared in 35% of patients after CESA and VASA.
After CESA and VASA 40 patients received a TOT, 10 patients of the CESA group and 30 patients of the VASA group. In total, after CESA and TOT, 20 out of 26 patients (77%) and in the VASA group 32 out of 45 patients (71%) were cured (Figure 3 and Table 2).

Figure 3: Cure rates for Urinary Incontinence (UI = mixed and urgency
urinary incontinence) before and after Cervico-Sacropexy (CESA) or Vagino-
Sacropexy (VASA) with or without Transobturator Tape (TOT) respectively.
Patients who were not cured after CESA or VASA received an additional
TOT. Clinical outcome was obtained 4 months after each type of surgery.
Percentages of absolute numbers are given in brackets.
First surgery
Urinary incontinence
n
Cured
Uncured
Additional surgery
n
Cured
Uncured
CESA
Urgency urinary incontinence (UUI)
7
5
2
+ TOT
2
1
1
Mixed urinary incontinence (MUI)
19
11
8
7
2
5
Stress urinary incontinence (SUI)
0
0
0
1
1
0
?
26
16
10
?
10
4
6
VASA
Urgency urinary incontinence (UUI)
6
3
3
+ TOT
7
1
6
Mixed urinary incontinence (MUI)
39
12
27
17
10
7
Stress urinary incontinence (SUI)
0
0
0
6
6
0
?
45
15
30
?
30
17
13
Table 2: Urinary incontinence before and after Cervico-Sacropexy (CESA) or Vagino-Sacropexy (VASA) and additional Transobturator Tape (TOT).
The follow-up period was between 6 and 24 months with a median of 16 months. During that period no mesh erosion or major complications of the operations were observed. All continent patients remained continent within the observation period.
Discussion
For several years it has been reported that after pelvic organ prolapse surgeries also urgency urinary incontinence symptoms disappeared in a considerable number of patients [14-18]. A comparable effect was noted in patients who received a TVT or TOT for SUI and also experienced a cure of their UUI [19].
These observations led us to the hypothesis that UI can be cured by a combined repair of the anterior and posterior level of the vagina in a thus far unknown percentage of patients [20,21].
We therefore decided to offer the apical fixation of the cervix or vaginal stump in combination with a TOT as treatment for urgency urinary incontinence patients who had failed all conservative treatments [9].
The USL were replaced by PVDF tapes [12]. These tapes were sutured at the pre-sacral fascia of the first or second vertebra of the sacrum and at the cervix or the vagina and placed below the peritoneal fold of the remaining USL. We chose PVDF because of diminished shrinkage and fibrosis formation compared to polypropylenes [11].
The repair of the apical level of the vagina by these CESA or VASA operations led to an overall cure rate of 44%. All these patients who were suffering from MUI or UUI were symptom-free immediately after surgery. No severe complications of surgery occurred and no side effects were noted.
Two interesting aspects of these apical fixations were detected. The cure rate obtained by the CESA operation (62%) was definitively higher than that after the VASA operations (33%) and in 35% of these patients the stress component disappeared without a repair of the anterior level.
The difference in outcome between CESA and VASA cannot be explained. The “VASA-patients“ were usually older than the “CESApatients“; however, not statistically significant. Otherwise, the documented pertinent clinical data and the severity of incontinence did not differ between the two groups.
Two more aspect came to our focus: on the one side, the cervix itself could exert an important physiological function. The USL are embryonically derived from the cervix and the posterior bladder wall physiologically adheres to the cervix. It remains unknown, whether or not it influences the outcome of VASA.
On the other side, several patients had an anterior colporrhaphy in combination with the previous vaginal hysterectomy. These previous operations were recorded; however, most patients could not remember details in that respect. Therefore, this aspect could not be further analyzed but should remain in the focus of future studies.
The second unexpected finding was the effect of the USL replacement on the SUI symptoms (as part of MUI). We expected that by the repair of the USL only the UUI symptoms disappeared. However, SUI symptoms disappeared in 35% of patients after CESA or VASA. So far, we have no explanation how the repair of the apical fixation of the vagina could cure SUI.
The repair of the anterior compartment (Level 1) by a TOT led to an additional cure rate of urinary incontinence in 40% of CESA patients and 57% of VASA patients. We have no explanation why the percentage was different between the CESA and VASA patients. This could be caused by the limited number of patients.
In accordance with the literature in 43% of the patients not only the stress component of the MUI was cured but also the urgency symptoms [19]. It is astonishing to note that this is nearly the direct opposite of the observations in USL replacement. In about one third of patients, the repair of the USL can cure SUI and in another third the repair of the PUL can cure UUI. The explanation of these observations will definitively give further insight in urinary continence mechanisms.
The ideas of Barber, Amundsen, Ulmsten and Petros have been adopted in the development of the CESA and VASA surgical treatment with and without TOT. The bilateral replacement of the USL cured UI in between 33% and 62% of patients. With an additional repair of the PUL more than two-thirds of these women were cured. Further studies should focus on the parameters, which delineate possible cure or failure and what must be done to cure the remaining third of patients.
Conclusion
Besides the repair of genital prolapse the bilateral replacement of the uterosacral ligaments by CESA or VASA cured between 33% and 62% of patients who suffered from mixed and urgency urinary incontinence. After an additional TOT an overall cure rate ranging from 71% to 77% was observed.
Acknowledgement
We would like to thank Mrs. Neumann who helped with data maintenance. We further thank Mrs. Hess and Mrs. Schmidt for their help in the outpatient clinic.
References
- Barber MD, Visco AG, Weidner AC, Amundsen CL, Bump RC. Bilateral uterosacral ligament vaginal vault suspension with site-specific endopelvic fascia defect repair for treatment of pelvic organ prolapse. American journal of obstetrics and gynecology. 2000; 183: 1402-1411.
- Amundsen CL, Flynn BJ, Webster GD. Anatomical correction of vaginal vault prolapse by uterosacral ligament fixation in women who also require a pubovaginal sling. J Urol. 2003; 169: 1770-1774.
- Petros PE, Ulmsten UI. An integral theory and its method for the diagnosis and management of female urinary incontinence. Scand J Urol Nephrol Suppl. 1993; 153: 1-93.
- Abrams P, Andersson KE, Birder L, Brubaker L, Cardozo L, Chapple C, et al. Fourth International Consultation on Incontinence Recommendations of the International Scientific Committee: Evaluation and treatment of urinary incontinence, pelvic organ prolapse, and fecal incontinence. Neurourology and urodynamics. 2010; 29: 213-240.
- Hiller L, Radley S, Mann CH, Radley SC, Begum G, Pretlove SJ, et al. Development and validation of a questionnaire for the assessment of bowel and lower urinary tract symptoms in women. BJOG: an international journal of obstetrics and gynaecology. 2002; 109: 413-423.
- Avery K, Donovan J, Peters TJ, Shaw C, Gotoh M, Abrams P. ICIQ: a brief and robust measure for evaluating the symptoms and impact of urinary incontinence. Neurourology and urodynamics. 2004; 23: 322-330.
- Homma Y, Koyama N. Minimal clinically important change in urinary incontinence detected by a quality of life assessment tool in overactive bladder syndrome with urge incontinence. Neurourology and urodynamics. 2006; 25: 228-235.
- Bump RC. The POP-Q system: two decades of progress and debate. Int Urogynecol J. 2014; 25: 441-443.
- Jäger W, Mirenska O, Brügge S. Surgical treatment of mixed and urge urinary incontinence in women. Gynecol Obstet Invest. 2012; 74: 157-164.
- Klink CD, Junge K, Binnebösel M, Alizai HP, Otto J, Neumann UP, et al. Comparison of long-term biocompability of PVDF and PP meshes. J Invest Surg. 2011; 24: 292-299.
- Klinge U, Klosterhalfen B, Ottinger AP, Junge K, Schumpelick V. PVDF as a new polymer for the construction of surgical meshes. Biomaterials. 2002; 23: 3487-3493.
- Siddique SA, Gutman RE, Schon Ybarra MA, Rojas F, Handa VL. Relationship of the uterosacral ligament to the sacral plexus and to the pudendal nerve. International urogynecology journal and pelvic floor dysfunction. 2006; 17: 642-645.
- Delorme E, Droupy S, de Tayrac R, Delmas V. Transobturator tape (Uratape): a new minimally-invasive procedure to treat female urinary incontinence. Eur Urol. 2004; 45: 203-207.
- Miranne JM, Lopes V, Carberry CL, Sung VW. The effect of pelvic organ prolapse severity on improvement in overactive bladder symptoms after pelvic reconstructive surgery. International urogynecology journal. 2013; 24: 1303-1308.
- Lensen EJ, Withagen MI, Kluivers KB, Milani AL, Vierhout ME. Urinary incontinence after surgery for pelvic organ prolapse. Neurourol Urodyn. 2013; 32: 455-459.
- Basu M, Wise B, Duckett J. Urgency resolution following prolapse surgery: is voiding important? Int Urogynecol J. 2013; 24: 1309-1313.
- Basu M, Duckett J. Effect of prolapse repair on voiding and the relationship to overactive bladder and detrusor overactivity. International urogynecology journal and pelvic floor dysfunction. 2009; 20: 499-504.
- Digesu GA, Salvatore S, Chaliha C, Athanasiou S, Milani R, Khullar V. Do overactive bladder symptoms improve after repair of anterior vaginal wall prolapse? International urogynecology journal and pelvic floor dysfunction. 2007; 18: 1439-1443.
- Tahseen S, Reid P. Effect of transobturator tape on overactive bladder symptoms and urge urinary incontinence in women with mixed urinary incontinence. Obstet Gynecol. 2009; 113: 617-623.
- Petros PE, Ulmsten UI. An integral theory of female urinary incontinence. Experimental and clinical considerations. Acta Obstet Gynecol Scand Suppl. 1990; 153: 7-31.
- DeLancey JO. Anatomy and biomechanics of genital prolapse. Clin Obstet Gynecol. 1993; 36: 897-909.