Abstract
Background: COPD is the most common chronic lung diseases and are major causes of lung related death and disability. Exercise training a core component of PR improves exercise capacity of patients with COPD although there are irreversible abnormalities in lung function. HF-NMES was successfully used as a localized training modality in severely disabled patients.
Objective: To evaluate the effectiveness of PR vs. HF-NMES emphasizing lower limb muscle training to improve the efficiency of 5 STS time and 6MWD in severe COPD patients.
Methods: The study population consisted of 45 patients diagnosed as severe COPD based on GOLD guidelines. 6 MWT distance and other parameters were measured at baseline and at 4th week, 8th week and 12th weeks of training programme. One way ANOVA was used to evaluate the association between 6MWD, 5STS time and CCQ score.
Results: Lower Limb Muscle Training Modalities (HF-NMES) improved exercise performance significantly, while it is known that the load on the cardiorespiratory system is rather low. Mean improvements in six minute walk distance exceeded in the HF-NMES group.
Conclusion: There is significant improvement in 5 STS time and 6 MWT distance following 12 weeks of lower limb muscle training in PR program and in HF-NMES for severe COPD patients.
Keywords: COPD; GOLD; HF-NMES; 6MWT; 6MWD; CCQ; ANOVA
Introduction
Pulmonary diseases are significant causes of morbidity and mortality in the present world. The COPD is the most common chronic lung diseases, and are major causes of lung-related death and disability [1].
In 2010, almost 24 million adults over the age of 40 in India had COPD. Data monitor expects this number to increase 34% to approximately 32 million by 2020. COPD is predominately a disease of men and only 40% of cases in India occur in women.
Pulmonary rehabilitation has emerged as a recommended benchmark of care for patients with chronic lung disease based on a growing body of scientific evidence [2].
Exercise intolerance is one of the main distressing manifestations of COPD. Patients with moderate and severe COPD commonly have difficulty performing normal daily tasks such as work, calisthenics, etc. The depression is associated with significant disturbances in physical function, [3] exercise capacity and health status also correlate with mortality [4]. Dyspnoea, leg exhaustion, and discomfort are the chief symptoms that reduce exercise [5]. Exercise training has been advocated as a valuable and restorative approach for these patient groups [6]. Recently High-Frequency Neuromuscular Electrical Stimulation (HF-NMES) has been successfully used as a localized training modality in severely disabled patients who are unable to follow formal pulmonary rehabilitation and/or tolerate higher training intensities [7-10].
In this study, HF-NMES was applied to patients with severe COPD and compared with pulmonary rehabilitation and conventional chest physiotherapy. The actual role of HF-NMES on lower limb muscle training in severe COPD patients and its undesirable consequences are still controversial.
In clinical practice, the 6-Minute Walk Test (6MWT) and 5 Sit To Stand Test (5STS) is commonly used to assess changes in functional exercise capacity in COPD patients following pulmonary rehabilitation with the primary outcome reported being the distance walked during the test i.e. Six Minute Walk Distance (6MWD) [11,12].
Methodology
Sample design
Non probability randomized sampling method was employed and informed consent was obtained from each subjects and this study has been approved by the ethical committee and Institutional review board of College of Physiotherapy SRIPMS Coimbatore.
Sample size
Totally 45 Patients are included in the study and randomly assigned to Group A and Group B and Group C.
Selection criteria
Inclusion criteria: [13,14]
- Patients with age group 40 to 60 years.
- Male patients of severe COPD diagnosed according to the GOLD guidelines.
- Patients with Manual muscle power grading of 3+ and above for quadriceps and hamstring muscles.
- No marked muscle wasting in the lower extremity.
- Baseline Modified Medical Research Council (MMRC) dyspnoea grade 3 or 4.
- Unstable cardiac disease.
- Patient with long-term use of supplemental oxygen.
- Patients with lower limb surgery within preceding 3 months.
- Exacerbation within preceding 4 weeks.
- Musculoskeletal disorders.
- Patients with cognitive deficit.
- Patients with metallic implant in lower limb.
- 6MWTdistance in meters.
- 5STS test time in seconds.
- Clinical COPD Questionnaire for measuring Quality of Life.
- 12 weeks.
- 3 day/ week.
- 40 minutes/ session.
- 12 weeks.
- 3 day/ week.
- 40 minutes/ session.
- Symmetrical, biphasic, square- pulsed current at 50Hz.
- Duty cycle: 2 s on and 10 s off in first week.
- 5 s on and 25 s off in second week.
- 10 s on and 30 s off for 3rd and 4th week and gradually progressed for 12 weeks.
- Pulse – 300 to 400 microseconds wide using highest tolerable amplitude.
- Leg press.
- Quadriceps extension.
- Squats.
- Straight leg raise.
- Step-ups or stair climbing.
- Sit-to-stand from progressively lower chairs.
- Postural drainage.
- Chest Percussion.
- Chest shaking.
- Huffing.
- Directed coughing.
- Relaxation techniques.
- Free exercise for lower limb.
- The 6-minute walk was linearly related to maximum METs (r = 0.687, P < 0.001), supporting the validity of the test. Patients walked significantly farther in each 6-minute walk (F = 19.83, P < 0.001), and strong test-retest reliability was demonstrated (intraclass correlation = 0.97). Distance walked decreased with older age (F = 19.49, P < 0.001), with men walking farther than women (F = 7.19, P < 0.01). The 6-minute walk was moderately correlated with scores from the DASI (r = 0.502, P < 0.001), and the Physical Function subscale of the SF-36 (r = 0.624, P < 0.001). The 6-minute walk is a valid and reliable method of assessing functional ability [27].
- Test-retest and interobserver intraclass correlation coefficients were 0.97 and 0.99, respectively, 5STS time correlated significantly with ISW, QMVC, SGRQ, ADO, ibode (r = 0.59,- 0.38,0.35,0.42 and 0.46) p< 0.001. 5STS time decreased with PR using different anchors, a conservative estimate for the MCD was 1.7s. It is a practical functional outcome measure suitable for use in most health care settings. 5STS is reliable, valid and responsive in patients with COPD [28].
- CCQ scores in patients (GOLD 0-III) were significantly higher than in healthy (ex) smokers. Furthermore, significant correlations were found between the CCQ total score (p= 0.48 to p=0.69) and SGRQ (p=0.67 to p=0.72). In patients with COPD, correlation between CCQ and FEV1% pred was p= -0.49. Test-retest reliability was determined (ICC = 0.94). CCQ is a self administered questionnaire specifically developed to measure clinical control in patients with COPD. Data support the validity, reliability and responsiveness of this short and easy administered questionnaire [29].
- Mannino DM. COPD: epidemiology, prevalence, morbidity, mortality, and disease heterogeneity. Chest. 2002; 121: 121–126.
- Spruit MA, Singh SJ, Garvey C, ZuWallack R, Nici L, Rochester C, et al. An official American Thoracic Society/ European Respiratory Society statement; key concepts and advances in pulmonary rehabilitation. Am J Respir Crit Care Med. 2013; 188:13-64.
- Lacasse Y, Rousseau L, Maltais F. Prevalence of depressive symptoms and depression in patients with severe oxygen-dependent chronic obstructive pulmonary disease. J Cardiopulm Rehabil. 2001; 20: 80–86.
- Oga T, Nishimura K, Tsukino M, Sato S, Hajiro T. Analysis of the factors related to mortality in chronic obstructive pulmonary disease: role of exercise capacity and health status. Am J Respir Crit Care Med. 2003; 167: 544–549.
- Maltais F, Decramer M, Casaburi R, Barreiro E, Burelle Y, Debigare R, et al. AN official American Thoracic Society and European Respiratory Society statement; Update on Limb Muscle Dysfunction in COPD: 2013 update. Am J Respir Crit Care Med. 2014; 189: 15-62.
- O’Shea SD, Taylor NF, Paratz JD. Progressive resistance exercise improves muscle strength and may improve elements of performance of daily activities for people with COPD: a systemic review. Chest. 2009; 136: 1269-1283.
- Sillen MJ, Janssen PP, Akkermans MA, Wouters EF, Spruit MA. The metabolic response during resistance training and NMES in patients with COPD, a pilot study. Respir Med. 2008; 102: 786-789.
- Fauge A, Alexandre F, Oliver N, Varray A, Heraud N. High vs. low-frequency neuromuscular electrical stimulation in COPD patients: What happens when current quantity is matched? ERJ. 2014; 44: 626.
- Caroline Helwick, Paratz, et al. Neuromuscular Electrical Stimulation Reduces Muscle Atrophy in Severe COPD. Respir Crit Care Med. 2010.
- American Thoracic Society. ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med. 2002; 166: 111-117.
- Spruit MA, Polkey MI, Celli B, Edwards LD, Watkins ML, Pinto-Plata V, et al. predicting outcomes from 6-minute walk distance in COPD. J Am Med Dir Assoc. 2012; 13: 291-297.
- Napolis LM, Corso SD, Alberto J, Malaguti C, Gimenes ACO, Nery LE. Neuromuscular electrical stimulation improves exercise tolerance in chronic obstructive pulmonary disease patients with better preserved fat-free mass. Clinics (Sao Paulo). 2011; 66: 401–406.
- Jones SE, Kon SS, Canavan JL, Patel MS, Clark AL, Nolan CM, et al. The five-repetition sit-to-stand test as a functional outcome measure in COPD. Thorax. 2013; 68: 15-16.
- Larson JL, Covey MK, Wirtz SE, Berry JK, Alex CG, Langbein WE, et al. Cycle Ergometer and Muscle Training in Chronic Obstructive Pulmonary Disease. Am J Respir Crit Care Med. 1999; 160: 500–507.
- Nici L, ZuWallack R, Wouters E, Zuwallack R, Ambrosino N, Bourbeau J, et al. On pulmonary rehabilitation: the American Thoracic Society/European Respiratory Society Statement on Pulmonary Rehabilitation. Eur Respir J. 2006; 28: 461–462.
- Neder JA, Sword D, Ward SA, Mackay E, Cochrane LM, Clark CJ. Home based neuromuscular electrical stimulation as a new rehabilitative strategy for severely disabled patients with Chronic Obstructive Pulmonary Disease (COPD) Thorax. 2002; 57: 333–337.
- Hicks CM. Research for physiotherapist-Project Design and Analysis; Churchill Livingstone. 1995; 2: 253.
- Spurit MA, Vanderhoven-August I, Janssen PP, Wouters EF. Integration of pulmonary rehabilitation in COPD. Lancet. 2008; 371: 12-13.
- American College of Chest Physicians and American Association for Cardiovascular and Pulmonary Rehabilitation. Pulmonary rehabilitation: joint ACCP and AACVPR evidence-based guidelines. Chest. 1997; 112: 1363–1396.
- Vivodtzev I, Debigare R, Gagnon P, Mainguy V, Saey D, Dube A, et al. Functional and muscular effects of neuromuscular electrical stimulation in patients withsevere COPD: a randomized clinical trial. Chest. 2012; 141: 716–725.
- Ozalevli S, Ozden A, Itil O, Akkoclu A. Comparison of the Sit-to-Stand test with 6 min walk test in patients with COPD. Respir Med. 2007; 101: 286-293.
- Bohannon RW. Test-retest reliability of the five-repetition sit-to-stand test: a systematic review of the literature involving adults. J Strength Cond Res. 2011; 25: 3205-3207.
- Rabe KF, Hurd S, Anzueto A, Barnes PJ, Buist SA, Calverley P, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med. 2007; 176: 352-355.
- Hermandes NA, Wouters EF, Meijer K, Annegarn J, Pitta F, Spruit MA. Resproducibility of 6-minute walking test in patients with COPD. Eur Respir J. 2011; 38: 261-267.
- Sue C. Jenkins. 6-Minute walk test in patients with COPD: clinical applications in pulmonary rehabilitation. Physiotherapy. 2007; 93: 175-182.
- Kadkar A, Maurrer, et al. The six minute walk test: A guide to assessment for COPD. 1997.
- Jones SE, Kon SS, Canavan JL, Patel MS, Clark AL, Nolan CM, et al. Five-repetition sit-to-stand test as a functional outcome measure in COPD. Thorax. 2013; 68: 1015-1020.
- Molen TVD, Willemse BWM, Schokker S, Hacken NHT, Postma DS, Juniper EF. Development, validity and responsiveness of the clinical COPD Questionnaire. Thorax. 2011.
- Sillen MJ, Speksnijder CM, Eterman RM, Janssen PP, Wagers SS, Wouters EF, et al. Effects OF NMES of muscles of ambulation in patients with COPD: a systemic review of the English- language literature. Chest. 2009; 136: 44-61.
Exclusion criteria: [14]
Assessment parameters:
The parameters are measured at baseline, 4th week, 8th week and at 12th week.
Study protocol
Group A: (Experimental group 1): Pulmonary rehabilitation programs are beneficial to patients with COPD and lower extremity strength training is considered a fundamental component of pulmonary rehabilitation.
Training protocol: 15 severe COPD patients were evaluated regarding pulmonary function, exercise capacity, quality of life. Patients were allocated to experimental group 1 (n=15) was submitted to a protocol of exercise sessions on a cycle ergometer with training intensity based on age predicted maximum heart rate (220-age) and dyspnoea score. Patients were instructed to pedal at a rate of 60 revolutions per minute (rpm) and they were encouraged to push themselves to the limits of their dyspnoea, without exceeding a heart rate equal to 80% of the predicted maximal heart rate. Patients should use pulseoxymeters to measure heart rate and they kept a book of training that included the time, work rate, and highest heart rate for each training session. An interval training protocol was used with patients performing four work sets, 5 min in duration, separated by rest intervals (2–4 min) of unloaded cycling [15] (Figure 1).

Figure 1: Experimental Group 1 Training Protocol.
Method: Bicycle ergometer training
Conventional chest physiotherapy: Conventional chest physiotherapy is referred to as a combination of postural drainage, airway clearance techniques such as percussion, vibration, shaking in severe COPD patients to improve breathing and exercise tolerance.
Group B: (Experimental group 2): NMES improves clinical and physiological function in COPD patients, appropriate rehabilitative plan to use prior to severe muscle atrophy and weakness develops in patients with COPD. NMES is a new rehabilitative strategy for severely disabled patients with COPD (Figure 2).
Figure 2: Experimental Group 1: Training Protocol.
Method
Bilateral NMES to quadriceps:
Training protocol: The subsequent treatment procedure was chosen to lessen the effects of fatigue on muscle contractility.
This training protocol was applied to each leg of the sequences 3 times per week for 12 weeks. 15 minutes at time in the first week, 30 minutes at a time in second week and 60 minutes at a time thereafter. Early training with HF-NMES before muscle wasting begins might be useful for enhancing exercise tolerance in COPD patients who are not yet severely disabled [16,17].
Strength training with weights: (Figure 3)

Figure 3: Strength training with weights
Strength training without weights:
Group C: (Control group): 15 patients with severe COPD were receiving Conventional Chest Physiotherapy (CCPT). This includes any combination of the following:
Data analysis
One way ANOVA (SPSS 18) was used to test the various parameters and their values are given below (Tables 1-3). (Graphs 1-3).
Source of variation
Sum of Squares
Degrees of freedom
Mean Squares
F Ratio
“P” value
Between Groups
3841.111
2
1920.556
16.187
.000
Within Groups
4983.333
42
118.651
Total
8824.444
44
Table 1: ANOVA table for six minute walk test distance.
Source of variation
Sum of Squares
Degree of freedom
Mean Square
F Ratio
“p” value
Between Groups
2822.578
2
1411.289
28.570
.000
Within Groups
2074.667
42
49.397
Total
4897.244
44
Table 2: ANOVA table for 5 sit to stand test time.
Sum of Squares
Df
Mean Square
F
Sig.
Between Groups
1528.133
2
764.067
22.183
.000
Within Groups
1446.667
42
34.444
Total
2974.800
44
Table 3: ANOVA table for CCQ.
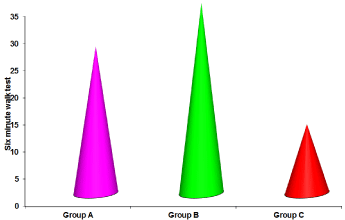
Figure 4: Six minute walk test data for three groups.
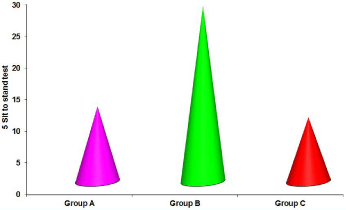
Figure 5: 5 Sit to stand test data for three groups.
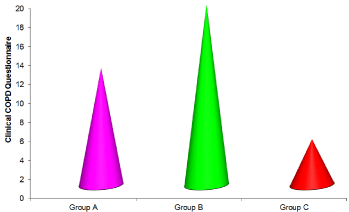
Figure 6: Clinical COPD Questionnaire Data for three groups.
Discussion
Skeletal muscle dysfunction plays a vital role in the symptoms and impairments in strength, endurance, and maximal exercise capacity experienced by COPD patients. Gosselink R, et al. (2013) showed that Peripheral muscle weakness adds to exercise restraint in COPD and the resultant inactivity leads to progressive deconditioning.
Carolyn L. Rochester, et al. (2010) conducted a study on exercise training in COPD and they found that exercise limitation usually begins with difficulty in Ambulating, thus exercise training have focused on training the muscles of the lower limbs, alone or in combination with training the arms or respiratory muscles [18].
This study was done with an objective to determine the efficacy of pulmonary rehabilitation programme vs. high frequency neuromuscular electrical stimulation emphasizing lower limb muscle training to improve the efficiency of 5 sit to stand test time and six minute walk distance in severe COPD patients. The statistical analysis was performed using ANOVA between group A, group B and group C showed the following outcome.
In six minute walk test, the mean scores for the functional improvement were 27, 35, 12.67 respectively for group A, group B and group C. The “F” ratio for one way ANOVA test calculated between the groups was 16.187 which were significant at the level of 0.000 at 42 degrees of freedom.
In 5STS, the mean scores for the functional improvements were -11.80, -27.67 and -10.07 respectively for groups A, B and C. The “F” ratio for one way ANOVA test calculated between the groups was 28.570 which were significant at the level of 0.000 at 42 degrees of freedom.
In CCQ, the mean scores for the functional improvements were -12.33,-19.07 and -4.80 respectively for group A, group B and group C. the “F” ratio for one way ANOVA test calculated between the groups was 22.183 which were significant at the level of 0.000 at 42 degrees of freedom.
From the value of “F” ratio there is significant variance between group A, B and C. hence we reject the null hypothesis and accept the alternate hypothesis.
Several randomized controlled trails in patients with COPD have demonstrated that PR improves dyspnoea, exercise tolerance and health related quality of life [19,20]. Research in this field has been important in our department for several years. Hence this study was done to compare the PR vs. HF-NMES and strength training and the results proves that HF-NMES is much effective than PR in severe COPD patients. HF-NMES is a good alternative for pulmonary rehabilitation [13].
A study done by Caroline Helwick, Paratz, et al. (2010) investigated the effects of Neuromuscular Electrical Stimulation and its effects on reducing muscle atrophy in severe COPD and they concluded that exercise performance, exercise induced symptoms of dyspnoea and fatigue improved significantly compared with baseline in patients who underwent HF-NMES and lower limb strength training. Moreover HF-NMES recruits motor units in a nonselective temporally synchronous pattern [21]. In COPD, atrophy of fast-twitch muscle fibers has been reported continuously. It can be hypothesized that at least some of these fibers can be trained by HFNMES [13-15] whereas these fibers might otherwise be recruited only by high-force voluntary efforts.
This study shows that lower-limb muscle training modalities improves exercise performance significantly, while it is known that the load on the cardio respiratory system is rather low [18]. Indeed, the mean improvements in six minute walk distance exceeded in the HF-NMES group [22-24]. This might be due to the fact that patients were still limited owing to their dyspnoea at the end of the exercise tests, while 5STS time would decrease significantly following HFNMES and lower limb strength training and that this reduction in time would correlate significantly with improvement in an established six minute walk test [25,26].
Conclusion
The outcome of data collection reveals that HF-NMES and lower limb strength training plays a vital role in the reduction of peripheral muscle weakness in patients with severe COPD. The recordable change shows in Six minute walk test, five Sit to Stand Test (5STS) and Clinical COPD Questionnaire (CCQ). It has been concluded that “There is significant improvement in 5STS time and 6MWT distance following 12weeks of lower limb muscle training in pulmonary rehabilitation program and HF-NMES for severe COPD patients.”
Reliability and validity
Six minute walk test
Five sit-to-stand test
Clinical COPD questionnaire
Ethical Committee Approval
This research is approved by the Institutional review board of Sri Ramakrishna Institute of Paramedical Sciences Coimbatore.
References
