
Rapid Communication
Austin J Anat. 2018; 5(2): 1081.
A Program of Medical Students as Teaching Assistants in an Anatomy Course: Effectiveness and Improvement
Kevin D He, William T Li BS and Zhang G*
Department of Pathology, Sidney Kimmel Medical College, Thomas Jefferson University, USA
*Corresponding author: Zhang G, Department of Pathology, Sidney Kimmel Medical College, Thomas Jefferson University, 1020 Locust Street, Room 263G Jefferson Alumni Hall, Philadelphia, PA 19107, USA
Received: April 16, 2018; Accepted: April 24, 2018; Published: May 01, 2018
Abstract
Introduction: Enlisting medical students as Teaching Assistants (TAs) in an anatomy course is regarded as beneficial to both students and TAs. A TA program has been implemented at SKMC and was shown to enhance the development of core competencies of medical students. This study examines the effectiveness of TAs and identifies specific ways in which to improve their teaching.
Methods: A survey was sent to 146 Physician Assistant (PA) students taking anatomy at Thomas Jefferson University. Questions included positivelyand negatively-framed items related to anatomy dissection. Responses were graded on a 5-point Likert scale. A total of 62 responses were recorded.
Results: PA students indicated that TAs contributed positively to their learning (97% of respondents), and 64% believed that this experience motivated them to pursue a similar role in the future. On the other hand, 11% of PA respondents noted that TAs occasionally provided incorrect information, and 2% of respondents noted that TAs were often unavailable when needed.
Discussion: Use of medical students as TAs in the dissection laboratory is an effective method for supplementing PA education. Unmasking potential issues with medical student TAs requires the use of targeted questions, rather than limiting evaluations to general items. Our data suggest that TAs should prepare for teaching, admit gaps in knowledge, and focus on maintaining a professional attitude in the anatomy dissection laboratory.
Keywords: Teaching assistant; Anatomy; Medical education; Physician assistant; Interprofessional education
Introduction
Modern medical education emphasizes non-technical competency. Programs in early medical education that enhance interprofessional communication and teamwork introduce students to their future team members in the current landscape of healthcare. While skills-based interprofessional programs have been encouraged, few have implemented similar measures for interprofessional teaching [1-3]. Recommendations exist for development of such interprofessional programs in the pre-clinical setting and acquisition of shared competencies to facilitate patient care [4]. Research has indicated a positive impact of early teaching experiences on the development of core teaching competencies, [5] but data on medical student teaching in an interprofessional setting are limited. Only one other institution has reported using medical students to teach physician assistant students in a first year anatomy course [3,6]. These studies, however, do not address areas in which teaching assistants can improve across a variety of modalities, such as coordination of shared dissection time, baseline knowledge of anatomy with admission of the lack there of, and attentiveness to the specific needs of the student teams. Although reviews have described positive benefits to student teachers in areas of academic learning and professionalism [7,8] the student learners’ perspective is often left unaddressed. In determining areas wanting for improvement, it follows that student feedback and student perception of teaching assistants may be the most constructive input.
The medical student Teaching Assistant (TA) program was established in 2014 at Sidney Kimmel Medical College and has been shown to contribute to core competency development in medical students [9]. Here, we aim to continue analysis of this program with further insight on the impact teaching assistants have on Physician Assistant (PA) students. Attempts to unmask previously undiscovered and unaddressed areas for improvement with specific questionnaire items may allow for a more targeted approach to improving the experiences of both parties.
Methods
Description of the TA program
The Department of Pathology, Anatomy & Cell Biology at Thomas Jefferson University established a medical student as teaching assistant program in 2014. Eight to ten rising second year medical students are recruited each summer and are given the opportunity to support department faculty in the dissection lab during an eight-week human gross anatomy course for first year physician assistant students at the beginning of their didactic period. Prior to the beginning of the dissection course, the course director administrates a half-day training session for the recruited medical student TAs. The training session emphasizes the importance of preparation for teaching, professional interactions with PA students, and teamwork among the TAs. The PA anatomy course consists of 42 hours of lecture accompanied by 92 hours of cadaver dissection. PA students are separated into dissection groups ranging from 5-6 students per cadaver and are instructed to reference Grant’s Dissector modules. Faculty instructors are present in the lab to assist with dissection and answer questions. TAs is instructed to perform a similar role. Responsibilities of the TAs include provision of guidance during dissection, identification of structures, and clarification of questions. TAs additionally compiles study materials for students prior to their exams. TAs organizes three timed practice practical examinations simulating testing conditions prior to each of three block examinations.
Survey administered to PA students
A total of 146 PA students from the Jefferson College of Health Professions and Arcadia University attended cadaver dissection during human gross anatomy in 2017. A survey “Post-Course Survey 2017” was provided to all students upon completion of the course. Survey questions included positively- and negatively-framed items specific to anatomy dissection. Questions gauged student appraisal of TA effectiveness and professionalism in different aspects of dissection lab, and specific items targeted potential issues that the students may have had with their TAs with respect to accuracy, professionalism, availability, and dissection. A total of 62 out of 146 students completed the survey. An additional short survey form was administered to and completed by all 98 Arcadia University students. Items evaluated student perception of TA performance. Students were given the option to provide constructive feedback about the TAs.
Responses were collected anonymously, graded on a five-point Likert Scale (“Strongly Disagree,” “Disagree,” “Neutral,” “Agree,” “Strongly Agree”), and converted to a numerical scale (1 = Strongly Disagree, 2 = Disagree, 3 = Neutral, 4 = Agree, 5 = Strongly Agree). “N/A” was an accepted response. For item 20 out of 32, students were instructed to select “Disagree” to control for inattentive participant responses. Means and standard deviations were calculated using Microsoft Office Excel 2017. Graphical representations are shown.
Results
Teaching assistants positively impacted the educational experience of PA students.
PA students reported that TAs made a positive contribution to their learning experience, with 97% agreeing or strongly agreeing with this statement. The average numerical score was 4.7 (Figure 1). In addition, 98% of students stated that TAs maintained an appropriate level of professionalism during dissection, and 97% agreed or strongly agreed that students in future years would benefit from continued use of TAs (average numerical score = 4.8). Students also reported that TAs were helpful in lab (average numerical score = 4.7). Students commented throughout the course that they were appreciative of the resources provided by TAs, including study guides and practice laboratory practical examinations.
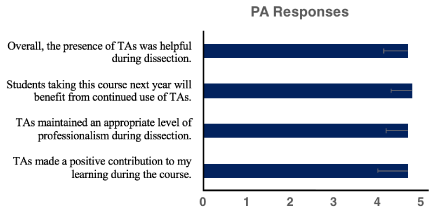
Figure 1: Positively-framed survey items. Student responses regarding
assessment of TA teaching effectiveness.
Teaching assistants must be aware of gaps in their academic knowledge
We posed four negatively-framed statements to students to assess their agreement or disagreement with these items (Figure 2). Of interest, 11% of respondents agreed that TAs provided incorrect or inaccurate information during dissection and did not follow-up with corrected information or an admission of error (average numerical score = 1.9), and 2% of students strongly agreed that TAs were rarely available when needed (average numerical score = 1.8). 2% of students agreed that TAs either dissected too much or limited their dissection experience (average numerical score = 1.4). No students strongly agreed or agreed with the statement that TAs interfered with dissection or interrupted the flow of their dissection group; however, 6% remained neutral on this subject (average numerical score = 1.3).
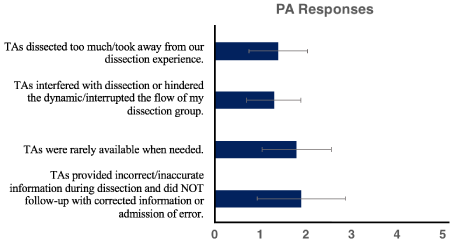
Figure 2: Negatively-framed survey items. Student responses regarding
areas in need of TA focus and improvement.
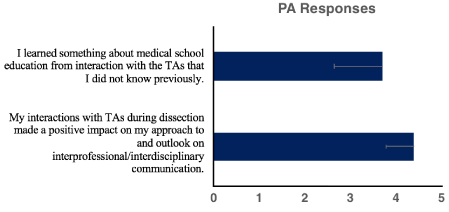
Figure 3: Interprofessional survey items. Student responses regarding the
impact of this teaching program on interprofessional communication.
The teaching assistant program supports interprofessional communication
Two survey items assessed student agreement with the positive impact of the program on interprofessional communication and evidence of social or extracurricular conversation (Figure 3). The data show that 93% of respondents agreed or strongly agreed that their interactions with TAs made a positive impact on their outlook on interprofessional and interdisciplinary communication (average numerical score = 4.4). In the context of casual conversation between the groups, 68% of the PA students either strongly agreed or agreed that they had learned something about medical education that they did not know previously (average numerical score = 3.7).
Discussion
Our data indicate that medical student TAs are effective resources in the dissection lab. PA students highly value the contributions of the TAs. Throughout the course, PA students conveyed their appreciation for the TAs’ time and involvement in their dissection experience.
Despite the mostly positive regard in which PA students held the TAs and their performance, survey items targeted areas that could potentially want for improvement. The aim of this study was to identify actionable areas and provide structured recommendations to the TAs in future iterations of this program.
We hypothesized that negatively-framed survey items may more effectively elicit issues students may have with TA performance. Positively-framed statements such as those assessing TA effectiveness above may not be a comprehensive measure of the effectiveness of this program. When answering a general question assessing the overall performance of TAs, students may not recall specific occasions on which TAs did not perform up to expectations or hindered their learning.
Noteworthy areas in which PA students found issue with TA behavior included i) providing misinformation, ii) lack of attentiveness to students’ needs for availability, and iii) involvement with dissection. Understandably, lack of knowledge is an unavoidable phenomenon in health education. Admission of knowledge gaps in certain areas is a virtue in medical education and should be freely acknowledged. Research and follow up, with either admission of error or response to the question, is highly recommended. Though the opportunities for misinformation may not be many, it is important to keep in mind that students under the stresses of a demanding curriculum look for accurate and reliable sources of information. Given that medical students at Sidney Kimmel Medical College had 7 months of non-anatomical coursework between the completion of their human gross anatomy course and the beginning of their responsibilities as TAs, it is understandable that only a brief review of the material may not be adequate for teaching. It is essential, however, that TAs understand when to admit an error.
It is also important for TAs to assess the needs of learners before interrupting a group dynamic to assist with dissection. Moreover, TAs should not spend disproportionate amounts of time with one group or in one area of the lab. Given that only one student agreed that TAs were over-involved with dissection and another that lack of availability was an issue, these two areas may not be as egregious as that of providing inaccurate information. The comments did elicit, however, a similar number of responses when comparing those related to availability and those related to provision of inaccurate information without follow up. It remains necessary for TAs to not limit their assistance to one or two tables and to be proactive in offering assistance to all students in the lab.
Our targeted approach to crafting a survey questionnaire with positively- and negatively-framed statements revealed instances where TAs did not appropriately handle students’ questions and attend to needs. These specific points cannot be elicited via sole utilization of positively-framed items. For example, despite the fact that 97% of respondents stated that TAs made a positive contribution to their learning, 11% indicated that TA students provided incorrect or inaccurate information. Although this may not have influenced their overall perception of the TAs in the anatomy course, it is important to utilize a targeted approach on questionnaires to unmask potential issues, rather than limiting evaluations to general items. This more clearly delineates areas wanting for improvement. Statements such as, “Did the teaching assistants at any point not meet expectations?” or “Can you recall instances where you took issue with or were disappointed by teaching assistants?” may be alternative approaches to identifying similar issues.
Because medical student TAs are the first students from a different program that the PA students have the opportunity to interact with, positive collaboration in this setting can significantly impact interprofessional communication. Communication is the key to proper working relationships, and so the lack of disagreement with the statement relating to interprofessional communication indicates that a supportive framework has been developed in the realm of interprofessional practice. The structure of the dissection lab encourages discussion between students and free movement from table to table. This also generates small, but meaningful conversation between students during natural pauses in their work. The presence and intermingling of the TAs during this time fosters discussion about the two groups’ respective experiences in their allied health fields. Familiarity encourages a positive outlook on the skills and experiences of both groups.
In summary, the program described in this study supports the growth of AAMC core competencies for medical education by developing medical students as teachers, [9] and it also enhances the competencies of physician assistants by allowing them to consider the idea of being involved in another’s education. Additional benefits that are potentially gained from use of student teaching assistants include lessening negative psychological impacts of human cadaver dissection, reducing apprehension towards dissection, improving dissection skill and confidence, and facilitating the professional growth of the student teachers [10-13]. Although human anatomy courses provided to physician assistant and medical students are undergoing experimentation [14-16] institutions that employ a similar curricular structure to the one described here should consider developing a similar program to benefit early physician assistant and medical education.
Our study was limited by the 62 responses received from the primary survey. We believe that it would be helpful to allow for commentary and constructive feedback after each individual survey item to pinpoint specific behaviors that can be improved upon in future years. Evaluation of TAs after completion of the course and their opinions on whether or not they agreed with any of the negatively-framed items would also form a more comprehensive understanding of the implications of using medical students as TAs.
Conclusion
In our approach to the push for core competency in modern medical education, we implemented a medical student-as-teaching assistant program for first year physician assistant students during human anatomy dissection. Though it has been previously assessed for its ability to develop medical students as teachers in fulfillment of the core competencies for medical education, the program provides a unique opportunity to evaluate the effectiveness and impact of medical student contributions to PA education from the perspective of physician assistant students. Continued improvement in the areas of error admission and collaborative dissection will benefit both parties. These areas should be taken into consideration when structuring a program of this nature, and TAs should be given additional guidance prior to its start. Utilizing medical students as teaching assistants can have a positive impact on physician assistant education.
Ethical Approval
According to the Institutional Review Board at Thomas Jefferson University, collection of statistical data on examinations/evaluations by Course Directors is EXEMPT from IRB review pursuant to Title 45 Code of Federal Regulations Part 46.101 (b) governing exempted protocol declarations.
Acknowledgement
The authors are indebted to Dr. Bruce Fenderson in the Department of Pathology, Anatomy & Cell Biology at Thomas Jefferson University for his expert editorial assistance.
References
- Sytsma TT, Haller EP, Youdas JW. Long-term effect of a short interprofessional education interaction between medical and physical therapy students. Anat Sci Educ. 2015; 8: 317-323.
- Shields RK, Pizzimenti MA, Dudley-Javoroski S. Fostering interprofessional teamwork in an academic medical center: Near-peer education for students during gross medical anatomy. Anat Sci Educ. 2015; 8: 331-337.
- Mcbride JM, Drake RL. Student-directed fresh tissue anatomy course for physician assistants. Anat Sci Educ. 2011; 4: 264-268.
- Thistlethwaite JE. Interprofessional education and the basic sciences: Rationale and outcomes. Anat Sci Educ. 2015; 8: 299-304.
- Andrew Jay E, Starkman SJ, Pawlina W. Developing medical students as teachers: An anatomy-based student-as-teacher program with emphasis on core teaching competencies. Anat Sci Educ. 2013; 6: 385-392.
- Mcbride JM, Drake RL. Student perceptions of an interprofessional educational experience: The importance of goal articulation. Anat Sci Educ. 2015; 8: 381-385.
- Yu T-C, Wilson NC, Singh PP. Medical students-as-teachers: a systematic review of peer-assisted teaching during medical school. Adv Med Educ Pract. 2011; 2: 157-172.
- Burgess A, McGregor D, Mellis C. Medical students as peer tutors: a systematic review. BMC Med Educ. 2014; 14: 115.
- Brown MT, Fenderson BA, Zhang G. Promoting the Development of Core Competencies during Early Medical Education: Implementation of a Teaching Assistant Program in Anatomy Course. Austin J Anat. 2017; 4: 1073.
- Houwink AP, Kurup AN, Kollars JP. Help of Third-Year Medical Students Decreases First-Year Medical Students’ Negative Psychological Reactions on the First Day of Gross Anatomy Dissection. Clin Anat. 2004; 17: 328-333.
- Mitchell BS, McCrorie P, Sedgwick P. Student attitudes towards anatomy teaching and learning in a multiprofessional context. Med Educ. 2004; 38:737-748.
- Cantwell S, Bonadurer GF, Pawlina W. Near-peer driven dissection selective: A primer to the medical school anatomy course. Clin Anat. 2015; 28: 985-993.
- Lachman N, Christensen KN, Pawlina W. Anatomy teaching assistants: Facilitating teaching skills for medical students through apprenticeship and mentoring. Med Teach. 2013; 35.
- Rizzolo LJ, Rando WC, O’Brien MK. Effectiveness of a shortened, clinically engaged anatomy course for physician assistant students. Anat Sci Educ. 2011; 4: 64-70.
- Isbell JA, Makeeva V, Caruthers K. The impact of Team-Based Learning (TBL) on physician assistant students’ academic performance in gross anatomy. J Physician Assist Educ. 2016; 27: 126-130.
- Philip CT, Unruh KP, Lachman N. An explorative learning approach to teaching clinical anatomy using student generated content. Anat Sci Educ. 2008; 1: 106-110.