
Case Report
Austin J Anesthesia and Analgesia. 2017; 5(2): 1060.
Trigeminal Trophic Syndrome: A Case Report
Fleischer BC¹, Pergolizzi JV¹*, Papagallo M², Taylor R¹ and Jo Ann LeQuang BA¹
¹NEMA Research, USA
²Albert Einstein Medical College, USA
*Corresponding author: Pergolizzi JV, NEMA Research, USA
Received: October 09, 2017; Accepted: October 24, 2017; Published: October 31, 2017
Introduction
Trigeminal Trophic Syndrome (TTS) is a rare neurological condition that occurs as a result of a lesion affecting the peripheral or central nervous system trigeminal pathway, such as might occur following an injury to the trigeminal ganglion [1]. Cases have also been reported following neurolysis of the Gasserian ganglion for the treatment of trigeminal neuralgia [1,2]. The overall pathogenesis of TTS is not well understood. In about a third of published cases, the patient had a history of stroke; other known associations include craniotomy, head trauma, and herpes zoster manifestation [2]. The mean age at presentation of TTS is 57 years (range 1 to 93 years) [1].
The first published reports of TTS appeared in 1933 by Wallenberg and Loveman. In one case, a “carcinomatous-like ulcer” appeared on the patient’s forehead following removal of the Gasserian ganglion. In the other case, the patient suffered from persistent facial ulcers with tissue damage to the ala nasi following ipsilateral neurolysis of the Gasserian ganglion for treatment of trigeminal neuralgia [3,4].
The classic presentation for clinical diagnosis of TTS is a triad of three symptoms: anesthesia, paresthesias, and skin ulcers within the trigeminal distribution. TTS is a diagnosis of exclusion with a differential based on clinical conditions, including malignancy, Wegener granulomatosis, infections, brown recluse spider bite, pyoderma gangrenosum, and factitious dermatitis. Differential diagnosis may require biopsy [5,6]. There is no specific diagnostic algorithm. Clinicians should look for prior history or cerebrovascular accident as these are common causations.
Facial ulcerations concentrate around the ala nasi [1,2], but TTS patients tend to feel facial paresthesias rather than facial pain. However, facial pain may be reported [7]. Patients may scratch, pick, or rub the areas of the face where they feel anesthesia or sensations described as burning, itching, or tingling. Compulsively picking the affected area leads to tissue injury and ulcers. Ulcers can be very persistent and progress soon after they appear, often as a result of the patient’s continuing self-injury [1,4,8]. Over time, the ulcers can damage the trigeminal nerve either by direct injury or by impeding the blood supply [9] in a course that varies from two weeks to 30 years, with a mean time of presentation around one or two years [1,2].
The following report presents a peculiar case of TTS in a patient who had been suffering from skin ulcers for eight years.
Case Presentation
A 48-year-old Caucasian female presented with an eight-year history of a persistent non-healing ulceration of the left cheek and chin. Her past medical history included intermittent cystic acne, which initially complicated the diagnosis. She also had a history of trigeminal neuralgia that was managed with bite splints, an orthodontic treatment that relieves pain and tension in the patient’s face. Two months after starting her orthodontic treatment, a large nodular lesion appeared on the patient’s left cheek. An initial culture of the lesion did not reveal any underlying cause. She also tested negative for Methicillin-Resistant Staphylococcus Aureus (MRSA).
The first attempt at treating the ulcer with an injection of triamcinolone acetonide was unsuccessful. Then the patient underwent a series of hyaluronic acid dermal filler injections which healed the ulcer over the course of six months, but left a large hard nodule under the patient’s skin along with noticeable hypopigmentation of the area.
The lesion was painless and pruritic. The patient experienced a relentless biting and stinging sensation, which caused her to pick and scratch. A tissue biopsy was unrevealing. Parasitic etiologies were excluded. The patient began to experience depression as the lesion interfered with her personal life and undermined her well-being. She was prescribed an antidepressant which she took for 10 months without improvement. She started to feel better upon discontinuation of the antidepressant. Over two years, two partially successful surgical attempts were made to remove the lesion. The lesion healed after surgery, but a prominent subcutaneous mass could still be felt at the lesion’s superior border.
Over the next year, the lesion fully ulcerated once more. At this point, the patient stated that the scratching and picking had gotten out of control. This lesion was different from any acne lesion the patient had ever experienced in the past. Repeated tissue analysis of the lesion excluded silicone or any other chemical substance or foreign body as possible cause. Skin sensitivity testing for allergy was performed on the patient with the result that positive skin sensitivity to some dental materials was determined. These dental materials were removed, but no improvement of the lesion was observed (Figures 1-4).
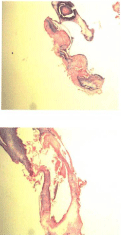
Figure 1: Both images were obtained from a biopsy taken in December 2013.
Note the perforation in the endothelium creating a tunnel.
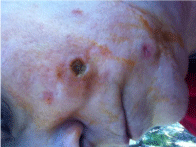
Figure 2: The ulcer on the patient’s right cheek.
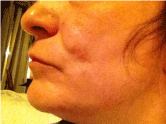
Figure 3: The ulcer had healed but a prominent subcutaneous protrusion
remained.
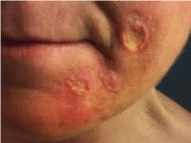
Figure 4: Facial disfiguration worsened over time.
The patient’s condition continued to worsen after February 2015. Evaluations led to multiple possible diagnoses including acne, silicone poisoning, picking, folliculitis, warts, and scabies. Many different treatment modalities were attempted. Treatment with ivermectin provided no improvement. The patient underwent six laser treatments for warts that did not improve the lesion. Laboratory tests for HIV and Celiac disease were both negative. Test results for food allergies were normal. Contact allergies to methyl isothiazolinone and formaldehyde were both positive, making the diagnosis of cystic acne a possibility. All products containing these chemicals were removed from the patient’s environment. The patient was also put on a diet that prevented swings in her insulin level. This action plan resulted in a significant weight loss and acne improved, however the ulceration on the patient’s cheek persisted.
By December 2015, additional biopsies were conducted to rule out cancer and fungal infections, but they reactivated the condition. The patient began a treatment of soaking the ulcer in a 30% solution of vinegar and water daily and she began wearing cotton gloves while sleeping. The solution and lifestyle modification of wearing gloves while sleeping resulted in gradual healing over time. However, the stinging sensation persisted and the patient felt a restrictive pressure in her left sinus.
In March 2016, the patient was evaluated by a dermatopathologist, and a final diagnosis of TTS was determined. The diagnosis was based on exclusion. The unilateral distribution of the lesions and the incessant pruritus were linked to neurocutaneous disease and, therefore, a neurological cause. The patient did not fulfill the classic triad of symptoms, in that she did not experience parethesias and anesthesia, which complicated and delayed the final diagnosis. The neurological causality of the lesion was the determinant used to reach the diagnosis of TTS. See Figure 5 for a timeline of events. The patient consulted with a neurologist and magnetic resonance imagining (MRI) was carried out which was inconclusive. The rarity of the disorder made the interpretation of MRI scans challenging.
The timeline of the patient’s diagnosis which was delayed because she did not have the classic triad of TTS symptoms.
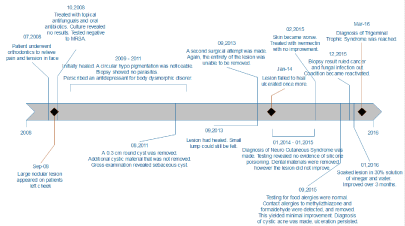
Figure 5: The timeline of the patient’s diagnosis which was delayed because she did not have the classic triad of TTS symptoms.
Discussion
TTS might be described as a two-step disorder in which a neurocutaneous itch or irritation provokes self-injury. Dysesthesia- a cutaneous symptom that might include pruritus, burning, tingling, anesthesia, paresthesia, hot or cold sensations, and even pain- can be caused by nerve damage when it occurs in a well-defined location [9]. This patient lacked the classic triad of symptoms in that she did not suffer anesthesia or parethesias in the trigeminal area but the dysesthesias, in particular pruritus, allowed diagnosis of underlying neuropathic damage.
TTN was difficult to diagnose because it is a rare disorder. There have only been 123 reported cases since the disease was first recognized in the literature in 1933 [1,10]. As demonstrated in the case above, misdiagnosis is common. Facial ulcers might be diagnosed as neoplasm or infections from bacteria, syphilis, deep mycosis, and parasites [2]. The difficulty of diagnosing TTS could be due to its rarity, making it a potentially underreported condition.
No standard protocol exists in regards to the treatment of TTS. A multidisciplinary approach is necessary because effective treatment of TTS involves many areas of medical expertise, including medical treatment, pain management, psychological counseling for depression and dysphoria, neurological evaluation, and surgery. Successful treatments for TTS include the application of topical antibiotics, pharmacological treatment, the use of mittens as a barrier, and surgical repair [2].
Over the course of her condition, the patient tried a variety of home remedies including a paste of baking soda and water, a paste of baking soda and castor oil, Dead Sea mud with potassium iodide, and a three-month course of treating the affected area with a 30% solution of vinegar and water. During this time, the patient started wearing cotton gloves to bed to prevent picking or scratching the area in her sleep. These efforts resulted in a gradual cosmetic improvement of the area but did not reduce facial sensations of stinging or itching.
Pain may or may not occur with TTS but this patient did not experience this as a painful condition. However, the patient’s sensations in the affected area led to compulsive picking at the skin which impeded treatment. This further advances picking and rubbing of the area, and ultimately impedes treatment. This can sometimes be managed by barriers or other treatments [1,11].
The physical appearance of TTS caused the patient considerable distress and even led to her being treated for depression. Psychological counseling may be appropriate for some patients as well as education so that the patient better understands how the condition can be exacerbated by picking and scratching [11].
Conclusion
Although TTS is rare, it may be under-diagnosed. Misdiagnosis of this condition can delay appropriate treatment. TTS is caused by neurological damage to the trigeminal ganglion, a sensory ganglion of cranial nerve V. Paresthesia from TTS often results in frequent disruption to ulcers, which results in further damage and prolonged healing. Although there is a classic triad of symptoms associated with TTS, TTS diagnosis is one of exclusion.
References
- Rashid R and Khachemoune A. Trigeminal trophic syndrome. Journal of the European Academy of Dermatology and Venereology. 2007; 21: 725-731.
- Sadeghi P, Papay FA, and Vidimos AT. Trigeminal Trophic Syndrome- Report of Four Cases and Review of the Literature. Dermatologic Surgery. 2004; 30: 807-812.
- McKenzie KG. Observations on results of the operative treatment of trigeminal neuralgia. Can Med Assoc. 1933; 29: 492-496.
- Weintraub E, Soltani K, Hekmatpanah J, Lorincz AL. Trigeminal trophic syndrome. A case and review. J Am Acad Dermatol. 1982; 6: 52-57.
- Sawada T, Asai J, Nomiyama T, Masuda K, Takenaka H, Katoh N. Trigeminal tropic syndrome: Report of a case and review of the published work. J Dermatol. 2014; 41: 525-528.
- Litschel R, Winkler H, Dazert S, Sudhoff H. Herpes zoster-associated trigeminal trophic syndrome: A case report and review. Eur Arch Oto Rhino layrngol. 2003; 260: 86-90.
- Garza I. The trigeminal trophic syndrome: An unusal cause of dysaesthesias, anaesthesia, and skin/soft tissue lesions. Cephalgia. 2008; 28: 980-985.
- Abyholm FE, Eskeland G. Defect of the ala nasi following trigeminal denervation. Case report. Scand J Plast Reconstr Surg. 1977; 11: 87-90.
- Shumway NK, Cole E, Fernandez KH. Neurocutaneous disease: Neurocutaneous dyesthesias. J Am Acad Dermatol. 2016; 74: 215-228.
- William NU and Christina Bilyeu W. Carbamazepine as a Treatment for Trigeminal Trophic Syndrome: A Case Report and Literature Review. Psychosomatics. 2015; 56: 580-582.
- Mishra SN, Nayak CS, Deshpande DJ, Pereira RR. Trigeminal trophic syndrome: A rare entity. Indian J Dermatol Venereol Leprol. 2011; 77: 729.