
Review Article
Austin J Anesthesia and Analgesia. 2021; 9(1): 1096.
What do we know about SARS-Cov-2 and Anesthesia Management?
Erdost HA*, Ozbilgin S and Kuvaki B
Department of Anesthesiology and Reanimation, School of Medicine, Dokuz Eylul University, Izmir, Turkey
*Corresponding author: Hale Aksu Erdost, Department of Anesthesiology and Reanimation, School of Medicine, Dokuz Eylul University, Izmir, Turkey
Received: January 06, 2021; Accepted: February 02, 2021; Published: February 09, 2021
Abstract
In general, COVID-19 is an acute disease, and the most common symptoms at onset are fever, dry cough, and fatigue, partly with nausea, diarrhea, or other gastrointestinal symptoms [1,2]. Also it has association with neurological symptoms, cardiovascular involvement, and hypercoagulability [3-13]. Anesthesiologists are confronted with these patients not only in intensive care but also in the operating room. In this brief review we focused on what do we know about COVID-19, and how to manage anesthesia and operating room when surgery is needed under the light of our experience and expertise in the field.
Keywords: COVID-19, Perioperative Management, SARS-Cov-2; Novel Coronavirus
Introduction
In Wuhan, Hubei Province, China first patients with pneumonia of unknown origin were identified in December 2019. On January 7, 2020, the Chinese Center for Disease Control and Prevention and Wuhan City health authorities reported a novel coronavirus from the respiratory tract. The novel coronavirus 2019 officially named severe acute respiratory syndrome coronovirus 2 (SARS-CoV-2) has spread quickly in China and from China to Korea, Japan, Italy, Iran and Singapore. SARS-CoV-2 is an enveloped, single and positive stranded RNA virus. The virus particles have a diameter of about 60-140 nm [1].
In general, COVID-19 is an acute disease, and the most common symptoms at onset are fever, dry cough, and fatigue, partly with nausea, diarrhea, or other gastrointestinal symptoms [1,2]. Patients may develop severe symptoms with diffuse alveolar injury, progressive respiratory failure, and Acute Respiratory Distress Syndrome (ARDS). However, the incidence of less common features like nausea, vomiting, diarrhea and abdominal pain varies significantly among different populations, along with an early and mild onset frequently followed by typical respiratory symptoms [3]. In a review of case series 2-40% of patients had gastrointestinal symptoms (including nausea, vomiting, diarrhoea, abdominal pain) [4,5]. Also Holshue et al. [6] published a case of COVID-19 patient who represented a 2-day history of nausea and vomiting on admission and then developed a slowdown in bowel movement on second day at hospital. Previous studies have shown gastrointestinal system involvement, and this was verified by biopsy of different parts of the gastrointestinal tract. In China minimally invasive autopsies from lung, heart, thyroid, kidney, liver, pancreas, spleen, bone marrow, intestinal tract including stomach and intestine, and skin were performed on three patients died of SARS-CoV-2 pneumonia. While the SARS-CoV-2 is mainly distributed in the lungs, the infection also involves the heart, vessels, liver, kidney, and other organs [7]. Moreover it is known that 36.4% (78/214) of patients with COVID-19 develop neurological symptoms, including headache, disturbed consciousness, and paresthesia. Severely affected patients are more likely to develop neurological symptoms than patients who have mild or moderate disease [8].
Besides these symptoms it has been reported that SARS- CoV- 2 has association with cardiovascular events including myocardial injury [9], myocarditis [10], cardiac arrhythmias [3,11], heart failure [12], and reduced systolic function [13]. In a retrospective cohort study from China SARS-CoV-2 was found to be associated also with hypercoagulable state and risk of venous thromboembolic events like pulmonary embolus [11].
With all these, ocular manifestation can occur such as conjuctival hyperemia and chemosis. Wu et al, [14] reported SARS-CoV-2 could be detected even in tears.
Preoperative management
In addition to emergency surgery in COVID-19 patients, the health care providers should also plan cases, like oncologic surgery or surgeries, which can’t be postponed for a longer period. These cases may be COVID-19 patients or not. How to manage these patients is a considerable issue not only for healthcare staff but also for the patients and their families because there is a high risk of transmission from human to human [15-17]. Studies in China have revealed that tight and methodological infection control rules could provide low infection rates during the perioperative anesthesia period. These rules are essential especially for the health care staff, including anesthesiologists, nurses, and intensive care staff and also cleaning staff working in the operating room. Janbabai et al. [18] explained possible pathways of transmission, which may be from the patient to the healthcare personnel, from healthcare personnel to the patient, between health care personnel and between patients.
The American College of Surgeons has recently proposed a schema to help with triage decision-making for elective cases [19]. Many operations in the region are for cancer or highly symptomatic patients, and as such the current guidance is not to postpone. It is important to recognize that decisions are fluid, and each hospital must make them based on current availability of resources and good clinical judgment.
Preoperative evaluation of the patient: If an undiagnosed but suspicious patient has to undergo urgent surgery, the surgery should not be delayed until the diagnostic tests are concluded. They must follow the same protocols as a patient with proven COVID-19 infection. The rational use of available resources should be prioritized and both stigmatization of patients and unnecessary alarm situations should be avoided.
If there is time, the patient’s file, especially recorded medical history and existing laboratory results, as well as any other available radiologic examinations should be viewed in a safe area before contacting the patient. Reviewing the case with the primary surgeon and the doctor who is treating the patient for COVID may give the anesthesiologist the opportunity to decide about the anesthesiologic approach. The anesthesiologist has to decide if a physical examination and interview with the patient should be done in the ward or if it is suitable to do this in the OR. If the anesthesiologist decides to see the patient on the ward, then Personal Protective Equipment (PPE) should be worn before entering the patient’s room.
At hospitalization of a patient body temperature should be measured. If the body temperature is higher than 37.3°C, the patient should be taken immediately to the clinics for fever disorders and the hospital’s infection authorities should be informed. Chen et al. [20] previously described preoperative anesthetic approach to patients with urgent surgery in the early stages of the pandemic. They suggest, that emergency surgery needs to be handle with a triage model. The primary triage should be done before admission to the hospital. A secondary triage before entering the operating room should be performed by anesthesiologists, including reviewing the medical history, a brief physical examination, and reviewing the chest computed tomography and/or chest x-ray. Also patient’s body temperature should be retaken before entering the OR.
There may be a higher risk of perioperative complications for COVID-19 positive patients and there may be a risk of being infected at the perioperative period for non-COVID-19 patients. Therefore, the informed consent should have added information about COVID pandemia for COVID-19 positive and non-COVID-19 patients. In a retrospective cohort study Lei et al. [21] showed none of the patients had signs or symptoms of COVID-19 before surgery. Remarkably, symptoms of COVID-19 appeared immediately after the completion of surgery, and SARS-CoV-2 infection was confirmed by the laboratory immediately after [21]. Common complications were ARDS (32,4%), secondary infection (29,4%), shock (29,4), arrhthmia (23,5%), acute cardiac injury (14,7 %), and acute kidney injury (5,9%). The same study also showed a 44% increase in intensive care needs and 20% increase in mortality after surgery. These should be definitely kept in mind before making a decision to operate.
Examination: Be aware the patient may not know who you are because of the PPE. For this reason, it is recommended to introduce you before examination. Taking history should be clear and short. Auscultation may not be performed most of the time due to the isolation precautions. After examination and leaving the patient’s room, PPE doffing must be done in a place reserved for this.
In most of the patients common laboratory abnormalities were increase total lymphocytes, prolonged thrombin time, and high lactate dehydrogenase levels. It has been shown in previous studies that patients with abnormal laboratory results require more intensive care. For this reason, complete blood count, biochemistry, coagulation tests and at least chest x-ray tests should be performed in the patient to be operated. As we know about COVID-19 so far, it has multiple clinical presentations which may be associated with cellular immune deficiency, coagulation activation, myocardial injury, hepatic injury, and kidney injury. Therefore tests should include; White blood cell (Neutrophil, Lymphocyte, Monocyte) count, Platelet count, Prothrombin time, Activated partial thromboplastin time, D-dimer, Creatine kinase, Creatine kinase-MB, Lactate dehydrogenase, Alanine aminotransferase, Aspartate aminotransferase, Total bilirubin, Blood urea nitrogen, Creatinine, Hypersensitive troponin I, Procalcitonin [3].
Personal Protective Equipment (PPE)
PPE is essential in all interventions requiring close contact to the patient such as aerosol-generating procedures including endotracheal intubation, manual mask ventilation before intubation, non-invasive ventilation, cardiopulmonary resuscitation, tracheostomy and bronchoscopy, application of high flow nasal cannula “HFNC” or surgical intervention, regional anesthesia, cannulation and catheterization.
Known or suspected COVID-19 patient must be regarded as high risk, so the perioperative management should be considered standard grade 3 PPE, including N95/FPP2, goggles, face shield, gown, protective coverall, protective overshoes All personnel and surgeons must be trained to prevent contamination during wearing and removal of these garments. These precautions are necessary not only to protect themselves, but also to protect each other [22]. Donning and doffing PPE is shown in Table 1 and Figure 1. After the preparation is completed, follow the shortest clean path to the patient.
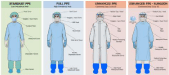
Figure 1: Donning and doffing PPE.
*Enhanced PPE; It is recommended for anesthesia team and surgical team for patients known to be COVID-19 positive/suspected COVID-19 to be operated. The
surgical team will wear sterile gowns and gloves in the operating room.
PPE Donning
One person for observe the donning
Remove Your Head cover And Surgical Mask
Put Your Shoe Covers
Hand Hygiene
N-95 /FFP 2 Mask
New Head cover
Surgical Mask On N-95/FFP2 to Protect The Mask
Hand Hygen
Medical Protecting Coverall
Googles
Faceshield
Leg Covers Waterproof Boots
Hand Hygiene
Waterproof Gown
Double Gloves
PPE Doffing
First Glove
Leg Covers Waterproof Boots
Second Glove
Hand Hygiene
Waterproof Gown
Hand Hygiene
Faceshield
Hand Hygiene
Medical Protecting Coverall
Googles
Hand Hygiene
Surgical Mask
Hand Hygiene
While Entering the Second Zone Head Cover and Shoe Covers
In Second Zone
Hand Hygiene
Put New Head Cover and Surgical Mask On N-95 (for protection the N-95)
Table 1: Donning and Doffing order PPE (In our clinic we prepared the donning and doffing with the consult of infection committee of our hospital) According to the contents of the glove and disinfectant, sterilization over gloves is foreseen disinfectant can disrupt the glove’s por structure and not recommended.
How should the operating room be arranged?
Operating rooms are potential high-exposure regions linked to airway manipulation and aerosolization of respiratory particles, so all health workers including surgeons; anesthesiologists, nurses, and cleaners are at high risk [23]. Anesthesiologists are additionally responsible for management of intensive care units. Thus, the exposure, and subsequent nosocomial and community transmission potential, is an extraordinary risk.
Consider using a checklist to ensure appropriate precaution is taken for operations with suspected or known COVID-19 infection. Simulation has been helpful in establishing new routines in the operating theatre [23].
Operating rooms and preoperative areas allocated for COVID-19 patients should be ventilated with negative pressure systems and the negative pressure level should be checked [24]. Negative room pressure is an isolation technique used in hospitals and medical centers to prevent cross-contamination from room to room [25]. Negative pressure is generated and maintained by a ventilation system that removes more air from the room than air is allowed into the room. Air is allowed into the room through a gap under the door (typically about 1.27 cm high). Except for this gap, the room should be as airtight as possible, allowing no air in through cracks and gaps, such as those around windows, light fixtures and electrical outlets. Leakage from these sources can compromise or eliminate room negative pressure [25]. Managing a patient infected with 2019-nCoV in operating rooms with positive pressure airflow creates a risk of viral spread. High-risk procedures producing aerosols like intubation should not be performed in positive pressure environments. Hospital should consult with biomedical engineers to see whether any operating room can be transformed to a negative pressure environment by changes in airflow or not. Hospitals without negative pressure systems should turn off positive pressure systems and air conditioning [20,23,26].
The WFSA open directives related to the use of isolation areas state the following: an infection control team should be determined to develop guidelines, monitor commitment of staff, and revise protocols.
Additionally, criteria related to how the workflow will begin in isolation areas are mandatory [27]. These criteria are, in order:
• Personnel should be assigned to check definitively that the isolation room pressure meets infection control criteria;
• Ensure all anesthesiologists, nurses, assistants and surgeons participating in the operation are informed in time;
• State the necessary personal protective equipment (PPE) for the area;
• State all equipment including disposable ones for COVID-19 positive cases;
• Place markings on doors to inform personnel and reduce traffic entering and leaving the isolation room to a minimum; and
• Each organization should define protocols for decontamination of the room after a suspected or positive case to reduce unnecessary contact by personnel or other patients to a minimum
Unnecessary articles including personal items like mobile phones and pens should not be brought to the operating room [23,28,29]. Within the Operating Room (OR) area, there should be signs stating where personal protective equipment should be worn and where removed and people should know these locations. The operating room door should be kept closed during the operation and entry-exit should be kept to a minimum [27]. Only people involved in direct care should be permitted to enter the operating room, unnecessary movement should be prevented. Technical personnel should periodically check the suitability of laminar flow and functions of high-effect filters. If possible, many facilities should accept they will have limited numbers of operating rooms and create a special COVID-19 working area [23].
Protocols should be developed for COVID-19 + patients including determination of special teams to manage these cases every day [23].
Surfaces in operating rooms should be cleaned well between cases. For all material including pulse oximetry probes, thermometers, blood pressure cuffs and other reusables, 70% alcohol solution or 0.5% chlorine solution rapidly kills the virus causing COVID-19 of SARS-CoV-19 on surfaces [30,31]. Patients with known or suspected COVID-19 infection should wear surgical masks when being transported through hospital spaces or in rooms without negative pressure isolation [32-34].
How should the anesthesia working station be arranged?
The anesthesia machine in the operating rooms allocated to COVID-19 patients should belong only to that room. Large, transparent nylon covers should cover anesthesia machines, the nylon cover should be discarded after every operation, and necessary disinfection should be performed appropriately [20]. Every patient should have a separate respiratory cycle. Filters should be inserted between the facemask or inserted airway device (intubation tube or laryngeal mask) and hoses of the respiratory cycles and in inspiratory and expiratory connections of the respiratory cycles (Figure 2) [20]. However, ASA states that as this may increase dead space for pediatric patients, therefore filters should be placed on the expiratory end of the corrugated breathing circuit before expired gas enters the anesthesia machine. Gas sampling should be protected with a HEPA filter and gases emerging from the gas analyzer should be discarded and prevented from entering room air [35]. Unnecessary equipment should be removed from the room. All necessary anesthesia and emergency medications and other material should be prepared outside the room and brought in. Trays with appropriate size should be prepared to place dirty materials on [26].

Figure 2: Installing the filters in the anesthesia device.
The use of a balloon valve system is not recommended. However, if there is a need to use it, a filter should be placed between the patient and extension piece and also between the balloon and extension piece (Figure 3). Care should be taken that a reservoir be attached to balloon valve systems.
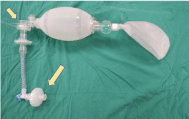
Figure 3: Installing the filters in the Bag valv.
Anesthesia management
The ASA does not indicate any point about whether general or regional anesthesia management should be used for emergency or elective surgeries of patients suspected or diagnosed with COVID-19, but underlines points that should be paid attention to when the method is decided [35].
General anesthesia
If general anesthesia will be used, it is recommended that a HEPA filter be inserted between the Y part of the respiratory cycle and the patient’s mask, endotracheal tube or laryngeal mask. Alternatively, for pediatric patients or where the additional dead space or weight of the filter will be a problem, the HEPA filter should be inserted at the expiratory end of the respiratory cycle before gas enters the anesthesia machine [35]. The Chinese Association of Anesthesiologists [20] recommends intubation with general anesthesia for patients with suspected or diagnosed COVID-19 with the aim of reducing the contamination risk from coughs. Other anesthesia methods may be chosen according to the individual circumstances of patients.
Anesthesia induction should begin after ensuring everyone in the room is wearing PPE. If general anesthesia will be administered, Rapid Serial Induction (RSI) is recommended, to prevent manual ventilation of the patient’s lungs and potential aerosolization. If manual ventilation is required, small tidal volumes may be used.
1Prepare your intubation equipment beside the patient and plan to discard to limit the movement distance of contaminated equipment. Strongly consider prophylactic antiemetics to reduce the risk of vomiting and possible viral spread risk [36]. Preoxygenate with 100% O2 before induction. During preoxygenation, the patient’s nose and mouth should be covered with 2 layers of damp gauze pads or face and surroundings should be covered with a large nylon cover with the aim of avoiding secretions from the patient. It should be ensured that the damp gauze does not block the patient’s airway. To be sure there is no leak during mask ventilation, care should be taken that there is a square ETCO2 waveform. Apneic oxygenation techniques should be avoided due to the risk of aerosolization [37]. Sufficient muscle relaxation should be ensured to prevent coughing during intubation. Mask ventilation should be minimized and cricoid pressure should not be applied.
While ESA [38] and SIARTTI [39] recommends cricoid compression if there is ongoing reflux, we have the opposite view. If the anesthesiologist always applies the cricoid maneuver in daily practice and has experience and practice in relation to this topic, then yes, this maneuver may be applied for intubation of COVID-19 patients. But, if the cricoid maneuver is not performed during practical anesthesia administration and there is no experience, then there is no need for this maneuver for intubation of COVID-19 patients.
Preoxygenation and anesthesia induction
Preoxygenation should be applied according to respiratory and hemodynamic status with a face mask without leak to protect the clinician.
TV with 3 min FiO2 = 1 (100%) or
ZVK 8 respirations FiO2 = 1 (100%) or
CPAP/PSV 10 cm H2O + PEEP 5 cmH2O
RSI with hypnotic agent chosen according to hemodynamics and full-dose neuromuscular blocker (rocuronium bromide)
Intravenous injection of penehyclidine hydrochloride or atropine before anesthesia, which can reduce airway secretions [40]. General anesthesia-inducing drugs: midazolam, propofol, fentanil/sufentanil/ remifentanil. Opioids should be given as intravenous bolus to avoid the occurrence of cough.
Ketamine: ketamine is not recommended as it increases secretions. However, ketamine is the anesthetic agent with best bronchodilator properties. If there is a need for bronchodilator efficacy and hemodynamic stability, it can be considered on a patient basis.
Decisions related to airway management should be taken using the basic principles explained above.
Some important basic principles from the guidelines of Difficult Airway Society, the Association of Anaesthetists, the Intensive Care Society, the Faculty of Intensive Care Medicine and the Royal College of Anaesthetists about airway management for anaesthesia are [41]:
• Airway management should be safe, accurate, and swift.
• There is likely to be a lower threshold for use of an SGA over facemask ventilation and also a lower threshold for tracheal intubation.
• If using an SGA, spontaneous ventilation may be preferred to controlled ventilation, to avoid airway leak.
• Drug choices may differ from when intubating a patient with critical illness and, in particular if the patient is not systemically unwell, ketamine may not be chosen as the induction agent.
• Note that tracheal intubation is associated with more coughing during extubation than when an SGA is used.
Avoiding this may include
• Use of an SGA instead of tracheal intubation
• Changing a tracheal tube to an SGA before emergence
• Use of i.v. or intracuff lidocaine; i.v. dexmedetomidine; opioids (e.g. fentanyl, remifentanil) before extubation.
Airway Management
The airway management algorithm in the operating room for patients positive or suspected of having COVID-19 is given in the infographic (Table 2). The anesthesiologist strictly implements three levels of protection (40). Many current guidelines about airway management for patients with suspected or confirmed COVID-19 state that PPE for airborne precautions is effective and must be worn at all times during intubation and all other aerosol generating procedures [39,41-44]. However, as communication skills may be made more difficult with PPE, we recommend that every department creates their own airway management algorithm, and provides practical training to the working team employees. Additionally, it is recommended to perform intubation kit preparations [45].
Airway management for COVID-19 patients
Intubation
Experienced 2 person for intubation team, most experienced practitioner for intubation
Preoxygenation (Check to respiratuar/hemodynamic status)
45° head up position
Use a intubation protective box if possible (minimize the explosure)
Pre-oxygenate with face mask using two hands
Least 3 min-most 5 min, FiO2 100%
Observe a square ETCO2 waveform, to make sure there is no leak
or 1 min at FVC 8 breaths FiO2 100%
or CPAP/PSV 10 cmH2O + PEEP 5 cmH2O, FiO2 100%
Aviod Bag-Mask ventilation if possible
RSI for all patients (make sure usage of NMB enough for induction dosage)
If the practitioner knows how to apply cricoid pressure, can apply
Use videolaryngoscope
If second attemp intubation failed, consider second generation supraglottic airway devices
Maximum try 3 attempts
Between attempts two person facemask oxygenation
Inflate cuff before initial ventilation
Confirm with capnography/Ultrasound
If cannot intubate cannot ventilate, early cricothyroidotomy
Extubation
Prophylactic anti-emetics
Adequate analgesia (If can be done add regional analgesia)
Antitussive drugs (remifentanil, lidocaine and dexmedetomidine) reduce the risk of coughing and minimise agitation on extubation
Use protective box if possible (minimize the explosure)/
Use closed aspiration system
Ensure no residual block
No positive airway pressure during extubation (ventilator off / reduce min fresh gas flow)
Consider attempting to extubate at end-expiration
Two handed mask if necessary
Confident of the patients awakeness
Place a surgical mask on the patient
Under surgical mask supplemental oxygen can be delivered via nasal oxygen cannula
Table 2: The airway management algorithm in the operating room for patients positive or suspected of having COVID-19.
To avoid the face of the person performing intubation being close to the patient’s face, ideally a video laryngoscope with a separate screen to the blade should be used [32]. Intubation should be performed without leaning over the patients face with the tube clamped in the distal section. If intubation is considered to be difficult, a guide wire should be inserted. The endotracheal tube should reach the ideal depth in a single attempt (frequently 22 cm from mouth edge). The cuff should be inflated (without allowing leaks) and then the tube clamp should be removed. Endotracheal tube insertion should be confirmed with end tidal carbon dioxide [27,44]. If difficult airway is predicted, flexible bronchoscopy intubation may be performed using a video bronchoscope with screen distant from the patient.
The ASA makes the following recommendations for intubation: double gloves, with the outer glove removed after intubation should be used to reduce environmental contamination to a minimum. In places where intubation is performed, the most experienced team in that location should perform intubation. As a result in operating rooms, there should be the most experienced anesthesiologist present. Unless specifically stated, awake fibreoptic intubation should be avoided. Droplets containing viral pathogens may become aerosols during this procedure [35].
Suctioning the endotracheal tube or administering nebulized medications is a different problem. If suctioning is anticipated, a closed suction system (like those used in intensive care) should be placed between the endotracheal tube and filter as soon as the endotracheal tube is inserted. In line nebulizers will need to be placed on the patient side of the filter to deliver medication effectively. If closed suction is not already in place or an inline nebulizer adapter is needed, the ventilator should be paused and the endotracheal tube clamped whenever it is disconnected from the HMEF.
During the SARS epidemic, surgical procedures were completed in isolation ICU rooms to remove the risk of in-facility transport and the need to make environmental changes to operating rooms. It is recommended that intravenous anesthesia use be chosen rather than volatile gas anesthetic machines in intensive care [27]. Wax et al. [26] mentioned the need for TIVA administration considering that COVID-19 positive patients, especially, do not improve or are not extubated quickly after the procedure. Many reviews have mentioned that COVID-19 has similar basic features to SARS and MERS epidemics. For anesthesia management of this special patient group with transmission by aerosol, we recommend the use of TIVA if appropriate after patient-based assessment for general anesthesia administration.
In the preoperative period for patients infected with 2019-nCoV, pneumothorax should strongly be considered in any patients with general anesthesia administered for sudden respiratory disorder. Considering the potential delay in obtaining a chest roentgen for a patient in isolation, mobile ultrasound may be used to rapidly assist pneumothorax diagnosis [41].
Extubation
Various techniques have been developed for extubation. “D’Silva et. al [46] developed a technique to minimize exposure of staff in proximity during extubation. The ‘mask over tube’ technique described as follows uses a second airway filter. The second airway filter is critical to ensure that disconnecting the circuit on extubation does not allow the anesthetist to be exposed directly to droplets or aerosols produced by extubation or associated coughing.
The extubation procedure has the same risks as intubation. Extubation should be completed with PPE. Closed system aspiration should be performed. If possible, it is recommended that extubation be performed in the operating room. Deflate ETT cuff and extubate whilst maintaining facemask seal. Discard ETT and connect circuit to the second airway filter facemask to the anesthetic circuit. Maintain a two-handed mask seal until any immediate post-extubation coughing has subsided and regular breathing via the circuit is confirmed [46].
Residual block should always be remembered and to avoid this, neuromuscular antagonists should be used if necessary. If extubation is not possible, they should transfer to the ICU while preserving PPE.
Regional Anesthesia
The ESRA recommendations are that airway interventions performed during General Anesthesia (GA) cause aerosol production and this leaves the health team at risk of exposure to COVID-19 transmission during both intubation and extubation. In all possible conditions, they recommend to prefer regional anesthesia. The possibility of acute respiratory tract infection transmission to a health worker during tracheal intubation is known to be 6.6 times that of those who do not perform tracheal intubation [24,47,48]. ESRA also state that regional anesthesia will be beneficial for patients due to reducing postoperative complication risk and to avoid GA and this will become more important in the context of the current respiratory tract infection [49,50]. Good planning should be made in order to perform surgeries fully with regional anesthesia. In the intraoperative period, the most unwanted situation is the need to transfer to GA unexpectedly. Due to surgery duration or complexity, if the possibility of transfer to GA is high, it will be more appropriate to begin with GA. This situation requires good communication between the anesthesia and surgery teams [24]. Patients are definitely required to wear surgical masks [42]. High-flow oxygen through the nasal cannula should be avoided because it may cause spread of droplets and aerosol production [43]. If the patient requires oxygen support, a nasal cannula can be used and a surgical mask may be placed above the oxygen mask to limit the spread of droplets. To reduce the aerosolization risk, oxygen support should be held at minimal flow to ensure saturation at the desired level. As it may cause crossinfections, use of common areas like block rooms or waiting sections should be avoided. The most experienced person should perform regional anesthesia administration. Personal protective equipment should be worn before entering the room [24].
Regional anesthesia is also recommended for patients undergoing operations for obstetric reasons. The infected mother should wear a surgical mask. If oxygen support is required, nasal cannula should be used.
Transport
Patient transport is a common part of anesthesia practice and will almost certainly be required when COVID-19 patients require an urgent procedure in the operating room. Institutions should have local guidelines for the preferred transport routes and use of PPE for the patient and health care workers during transport. Intubated patients will require continuous ventilation during transport. Transport ventilators and self-inflating resuscitation bags should be used with a high-quality viral filter mounted at the airway. Ventilators typically exhaust exhaled gas to the immediate environment so added protection would include placing a high-quality viral filter at the end of the expiratory limb [51].
For patients where the dead space imposed by the filter is a concern, a Mapleson D type transport circuit eliminates concern about the impact of additional dead space if the filter is placed on the device side of the fresh gas flow inlet and fresh gas flow is set to exceed minute ventilation [51].
When initiating the transport process, leave the viral filter in place on the endotracheal tube and connect the filter to the transport ventilation device. Use in-line suction and nebulization devices. Clamp the endotracheal tube whenever it is disconnected from the filter to maintain a closed system.
Once a “high-quality” viral filter is in place on the endotracheal tube, the breathing circuit can be disconnected from the filter while moving a patient or to reconnect to a different ventilation device. The filter will reliably stop viruses exhaled by the patient from contaminating the room [51]. Chinese Association of Anesthesiologists recommendation [20]; if a suspected or confirmed COVID-19 patient is stable after surgery and does not meet the criteria for admission to the ICU, they should be transferred directly back to the negative-pressure ward or isolation ward after extubation in the operating room. During transfer, the circulating nurse and anesthesiologist should wear proper personal protective equipment outside the operating room. The patient should be covered with one disposable operating sheet and then transferred to the negativepressure or isolation ward through a dedicated lobby and elevator. The patient must wear a surgical mask during transfer. The surfaces of passageways and the elevator should be cleaned and covered. If the patient is kept intubated, a single-patient-use respiratory bag must be used during transfer. In literature most of the authors are not recommending the use of a ventilator during transfer, instead they strongly advice to transfer these patients with a single use bag valv mask. But unfortunately most countries do not have the same financial means to use disposable bag valv mask. So if you have to transfer the patient who is intubated and requires mechanical ventilation is to be transported by using a ventilator, then at least HEPA filters should be used.
During transfer, the team should wear PPE even outside the operating room. During transfer, an extubated patient should wear a surgical mask. After standard cleaning processes for the places the patient has passed and the transfer bed, these should be disinfected with products appropriate to the hospital disinfection rules.
After surgery, anesthesia devices and trays should be cleaned and disinfected. At this point, cleaning should be performed according to cleaning recommendations prepared by the Ministry of Health. All single-use material should be carefully thrown in the waste. Nylon covers on devices used in the operating room like anesthesia mask, perfusors and defibrillators should be carefully collected and thrown in the waste.
ESA recommendations [38]; Follow bio-containment regulations. In addition to all the suggestions mentioned above, we recommend that patients be transported to the intensive care units or services with stretchers designed with a specially prepared box. Thus, by using this box, any possible aerosol propagation from the in-hospital lifters along the corridors will be prevented.
References
- Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet (London, England). 2020; 395: 497-506.
- Chan JF, Yuan S, Kok KH, To KK, Chu H, Yang J, et al. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-toperson transmission: a study of a family cluster. Lancet (London, England). 2020; 395: 514-523.
- Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020.
- Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, et al. China Medical Treatment Expert Group for Covid-19.China Medical Treatment Expert Group for Covid-19. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020.
- Zhang JJ, Dong X, Cao YY, Yuan YD, Yang YB, Yan YQ, et al. Clinical characteristics of 140 patients infected with SARS-CoV-2 in Wuhan. Allergy. 2020.
- Holshue ML, DeBolt C, Lindquist S, Lofy KH, Wiesman J, Bruce H, et al. For the Washington State 2019-nCoV Case Investigation team. First case of 2019 novel coronavirus in the United States. N Engl J Med. 2020; 382: 929-936.
- Yao XH, Li TY, He ZC, Ping YF, Liu HW, Yu SC, et al. A pathological report of three COVID-19 cases by minimally invasive autopsies. 2020; 49: 411-417.
- Wu Y, Xu X, Chen Z, Duan J, Hashimoto K, Yang L, et al. Nervous system involvement after infection with COVID-19 and other coronaviruses. Brain Behav Immun. 2020; 87: 18-22.
- Yang X, Yu Y, Xu J, Shu H, Xia J, Liu H, et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a singlecentered, retrospective, observational study. Lancet Respir Med 2020.
- Bonow RO, Fonarow GC, O’Gara PT, Yancy CW. Association of coronavirus disease 2019 (covid-19) with myocardial injury and mortality. JAMA Cardiol. 2020.
- Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020; 395: 1054-1062.
- Driggin E, Madhavan MV, Bikdeli B, Chuich T, Laracy J, Bondi-Zoccai G, et al. Cardiovascular considerations for patients, health care workers, and health systems during the coronavirus disease 2019 (covid-19) pandemic. J Am Coll Cardiol. 2020.
- Inciardi RM, Lupi L, Zaccone G, Italia L, Raffo M, Tomasoni D, et al. Cardiac involvement in a patient with coronavirus disease 2019 (covid-19). JAMA Cardiol. 2020.
- Wu P, Duan F, Luo C, Liu Q, Qu X, Liang L, et al. Characteristics of ocular findings of patients with coronavirus disease 2019 (covid-19) in Hubei Province, China. JAMA Ophthalmol. 2020.
- Li Q, Guan X, Wu P, Wang X, Zhou L, Tong Y, et al. Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus- Infected Pneumonia. N Engl J Med. 2020; 382: 1199-1207.
- Zhao S, Ling K, Yan H, Zhong L, Peng X, Yao S, et al. Anesthetic Management of Patients with COVID 19 Infections during Emergency Procedures. J Cardiothorac Vasc Anesth. 2020; 34: 1125-1131.
- Huang X, Wei F, Hu L, Wen L, Chen K. Epidemiology and Clinical Characteristics of COVID-19. Arch Iran Med March. 2020; 23: 268-271.
- Janbabai G, Razavi S, Dabbagh A. How to manage perioperative patient flow during COVID-19 pandemic: a narrative review. Journal of Cellular & Molecular Anesthesia, 2020; 5: 47-56.
- https://www.facs.org/about-acs/COVID-19/information-for-surgeons/triage.
- Chen X, Liu Y, Gong Y, Guo X, Zuo M, Li J, et al. Chinese Society of Anesthesiology, Chinese Association of Anesthesiologists. Perioperative Management of Patients Infected with the Novel Coronavirus: Recommendation from the Joint Task Force of the Chinese Society of Anesthesiology and the Chinese Association of Anesthesiologists. Anesthesiology. 2020.
- Lei S, Jiang F, Sua W, Chend C, Chene J, Meif W, et al. Clinical characteristics and outcomes of patients undergoing surgeries during the incubation period of COVID-19 infection, E Clinical Medicine. 2020.
- Institute of Medicine (US) Committee on R&D Needs for Improving Civilian Medical Response to Chemical and Biological Terrorism Incidents. Chemical and Biological Terrorism: Research and Development to Improve Civilian Medical Response. Washington (DC): National Academies Press (US). 1999.
- Ademuyiwa AO, Bekele A, Berhea AB, Borgstein E, Capo-Chichi N, Derbew M, et al. COVID-19 Preparedness within the Surgical, Obstetric and Anesthetic Ecosystem in Sub Saharan Africa. Ann Surg. 2020.
- Practice Recommendations on Neuraxial Anesthesia and Peripheral Nerve Blocks during the COVID-19 Pandemic. 2020.
- Hoffman PN, Weinbren MJ, Stuart SA. A practical lesson in negative-pressure isolation ventilation. J Hosp Infect. 2004; 57: 345-346.
- Wax Randy S, Christian Michael D. Practical recommendations for critical care and anesthesiology teams caring for novel coronavirus (2019-nCoV) patients. 2020.
- Tang G, Ming Chan AK. Perioperative management of suspected/ confirmed cases of COVID-19. General Anaesthesia Tutorial 421. 2020.
- CDC PPE Donning and Doffing Sequence. 2020.
- Personal protective equipment: Our process if COVID-19 is suspected | The Loop. 2020.
- COVID-19 Clinical Response | Partners In Health. 2020.
- WHO. Water, sanitation, hygiene and waste management for the COVID-19 virus. 2020.
- Chen C-C, Willeke K. Aerosol penetration through surgical masks. Am J Infect Control. 1992; 20: 177-184.
- Rowley E, Dingwall R. The use of single-use devices in anaesthesia: balancing the risks to patient safety*. Anaesthesia. 2007; 62: 569-574.
- Milton DK, Fabian MP, Cowling BJ, Grantham ML, McDevitt JJ. Influenza Virus Aerosols in Human Exhaled Breath: Particle Size, Culturability, and Effect of Surgical Masks. PLoS Pathog. 2020; 9.
- Information for Health Care Professionals. 2020.
- Kamming D, Gardam M, Chung F. Editorial I. Anaesthesia and SARS. Br J Anaesth. 2003; 90: 715-718.
- SAS COVID-19 Resources. 2020.
- AIRWAY MANAGEMENT. 2020.
- http://www.siaarti.it/SiteAssets/News/COVID19%20%20documenti%20 S I A A R T I / S I A A R T I%2 0%2 0 C o v i d 1 9%2 0%2 0 A I RWA Y%2 0 MANAGEMENT%20(English%20version).pdf
- Huang J, Zeng J, Xie M, Huang X, Wei X, Pan L. How to perform tracheal intubation for COVID-19 patients safely and effectively: Experience AND tips from Sichuan, China. Journal of Clinical Anesthesia. 2020; 64: 109800.
- Cook TM, El-Boghdadly K, McGuire B, McNarry AF, Patel A, Higgs A. Consensus guidelines for managing the airway in patients with COVID-19: Guidelines from the Difficult Airway Society, the Association of Anaesthetists the Intensive Care Society, the Faculty of Intensive Care Medicine and the Royal College of Anaesthetists. Anaesthesia. 2020; 75: 785-799.
- World Health Organization. Coronavirus disease (COVID-19) advice for the public: when and how to use masks. 2020.
- Simonds AK, Hanak A, Chatwin M, Morrell M, Hall A, Parker KH, et al. Evaluation of droplet dispersion during non-invasive ventilation, oxygen therapy, nebuliser treatment and chest physiotherapy in clinical practice: implications for management of pandemic influenza and other airborne infections. Health Technol Assess. 2010; 14: 131-172.
- Gottlieb M, Holladay D, Burns KM, Nakitende D, Bailitz J. Ultrasound for airway management: An evidence-based review for the emergency clinician. Am J Emerg Med. 2020. 38: 1007-1013.
- Lopez RA, Anthony A, Zuo L, Enomoto TM, Aziz MF. Your COVID-19 Intubation Kit. Anesth Analg. 2020.
- D’Silva DF, McCulloch TJ, Lim JS, Smith SS, Carayannis D. Extubation of patients with COVID-19. Br J Anaesth. 2020.
- World Healty Organization. Infection prevent and control of epidemic-and pandemic-prone acute respiratory diseases in health care. Geneva: WHO. 2014.
- Tran K, Cimon K, Severn M, Pessoa-Silva CL, Conly J. Aerosol generating procedures and risk of transmission of acute respiratory infections to healthcare workers: A systematic review. PloS One. 2012; 7: e35797.
- Warren J, Sundaram K, Anis H, Kamath AF, Mont M, Higuera CA, et al. Spinal anesthesia is associated with decreased complications after total knee and hip arthroplasty. J Am Acad Orthop Surg. 2020; 28: e213-e221.
- von Ungern-Sternberg BS, Boda K, Chambers NA, Rebmann C, Johnson C, Sly PD, et al. Risk assessment for respiratory complications in paediatric anaesthesia: A prospective cohort study. Lancet. 2010; 376: 773-783.
- Faq on Anesthesia Machine Use, Protection, and Decontamination during. The Covid-19 Pandemic. 2020.