Abstract
Introduction: Heart Failure (HF) is commonly the final stage of all cardiopathies, and its prognosis is closely related to the number of hospitalizations.
Objective: To evaluate the evolution of the hospitalization indexes, duration, and mortality rates from 2008-2014 among HF patients over 60 years of age in the Brazilian Public Health System (SUS), compared with patients under 60.
Methods: Data were obtained from the DATASUS database, assessing hospitalizations for HF from the period of 2008 to 2014.
Results: A total of 78,117,726 hospitalizations occurred, with 22.2% among patients over 60 years of age. HF was the cause of hospitalization in 7.5% of older and 0.9% of younger patients. The absolute number of hospitalizations for HF declined from 81,359 in 2008 to 64,003 in 2014 among patients <60 years and from 187,628 in 2008 to 160,287 in 2014 among the older population. The value of hospitalization for HF increased independent of age range, as did the mean hospital stay and the mortality rate increased in both groups, but remained higher in the >60 group.
Conclusion: HF is a severe public health problem that, despite new medications that reduce hospitalizations and mortality of HF patients, the associated mortality rate continues to climb. Although the mean value of hospitalization is lower among the older population, the total cost in 5 years was more than double, especially due to the higher number of hospitalizations among these patients.
Keywords: Heart failure; Older population; Hospitalizations; Mortality rate
Introduction
Heart failure is commonly the final stage of all cardiopathies. With increased life expectancy, improvements in clinical treatment of cardiovascular disease and greater survival rates of patients submitted to chemotherapy and subsequent chemotherapy-induced cardiomyopathy, its incidence tends to increase [1-3].
With the medical advances in identification of the pathophysiology, research of new drugs to block specific systems, and the use of pacemakers and resynchronization devices for the treatment and prevention of ventricular dysfunction progression, survival and quality of life of these patients has increased progressively [1,3-9].
Heart failure is a syndrome whose prognosis is closely related to functional capacity, to the degree of systolic dysfunction, and to the number of hospitalizations. It is known that patients who are hospitalized for heart failure present a re-hospitalization rate above 50% within 6 months [1,10-14].
In Brazil, the older population (>60 years of age) has been increasing at an accelerated pace. It is predicted that the population over 60 years of age, corresponding to 10% of the total population in 2010, will reach 28.3 million (13.7%) in 2020, and 52 million (23.8%) in 2040, or nearly one quarter of the country’s total inhabitants.
The objective of this study was to evaluate the evolution of the hospitalization rates from 2008 to 2014 within the Brazilian Public Health System (Sistema Único de Saúde - SUS) among older patients (>60 years of age) with HF, length of hospitalization, and mortality rate, compared with patients <60 years of age.
Methods
Data were obtained from DATASUS, the open epidemiologic database of the Brazilian Public Health System [15]. We assessed hospitalizations due to HF (ICD-10 I50) from the period of 2008- 2014. The variables gender, number of hospitalizations, geographic region, age range, average hospitalization duration, mortality rate, and mean hospitalization cost (AIH - the mean value reimbursed by the SUS for general and disease-specific hospitalizations).
Results
From the period of 2008-2014, a total of 78,117,726 hospitalizations were recorded, of which 17,350,352 (22.2%) were for patients above 60 years of age. Of all hospitalizations for this age group, HF was the cause for hospitalization in 7.5% of cases, as compared to 0.9% among the <60 age group.
The absolute number of hospitalizations for HF declined from 81,359 in 2008 to 64,003 in 2014 (-21.3%) among patients under 60 years of age; while among patients >60, the number of hospitalizations declined from 187,628 in 2008 to 160,287 in 2014 (-14.6%).
The hospitalization cost increased among patients hospitalized for HF independently of age range, increasing from R$993.51 in 2008 to R$1,625.37 in 2014 (an increase of 63, 6%) for the <60 age group, as compared to R$889.23 in 2008 to R$1,319.11 in 2014 (48.3%) among patients >60 years of age. Calculating the hospitalization costs for HF over 7 years, the cost for patients >60 years was R$1,556,429,901.01, compared with R$770,172,424.71 for patients <60 years of age (Figure 1).
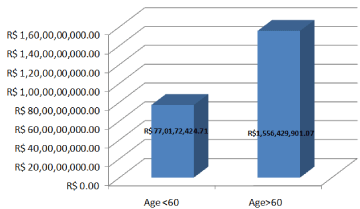
Figure 1: AIH (mean value reimbursed by the SUS for general and diseasespecific
hospitalizations) values for heart failure hospitalizations for patients
<60 and >60 years of age between 2008-2014.
There was also an increase in mean hospital stay from 6.2 days to 6.8 days (9.7%) in patients <60 and an increase of 7 to 7.6 days (8.6) among patients >60. Despite medical advances during the period, the mortality rate also increased, from 6.3% to 6.7% (increase of 6.3%) among patients <60 and from 9.0% to 11.0% (increase of 22.2%) in patients >60 years of age.
Discussion
HF is undoubtedly a serious public health problem. With the high prevalence of arterial hypertension and diabetes in the Brazilian population associated with an increased life expectancy, there is an increase in the size of the at-risk population. Since the late 1990’s there are epidemiological records demonstrating that cardiovascular disease represent a significant number of hospitalizations and that congestive heart failure is among the leading causes [1,16,17]. Although this study presents the limitations of the characteristics of the database itself, including inability to isolate baseline characteristics and sub-analysis by gender, we feel it does highlight important epidemiological aspects of HF in Brazil.
The importance of the older population in the context of HF is noted in several epidemiological studies, identifying that more than 50% of patients diagnosed with HF are over 60 years of age, and present a higher number of co-morbidities as compared with younger patients. Associated to this greater severity, the HF mechanism itself is different, as older adults are more likely to present diastolic HF, identified as the principal etiology of hypertensive cardiopathy, in contrast to younger patients which present systolic dysfunction secondary to ischemic cardiopathy [1,18,19].
However, even with new drugs that aim to reduce hospitalization and mortality rates among patients with HF, the mortality rate due to this condition is increasing [17].
Not only has mortality been increasing but also HF patient costs. It is known that after a hospitalization, up to 50% of patients are rehospitalized within 90 days, resulting in greater costs in addition to negatively impacting quality of life [1,10,11].
This study demonstrates that despite a reduction in absolute number of hospitalizations, HF patients present a longer period of hospitalization and present an increase in in-hospital mortality. Chaudhry et al. reported a 30-day mortality rate of 9.8%, and that each 5-year age increase presents a 1.19 fold increase in risk of death [20].
Regarding the data from this study, it is important to note that these data are representative of the Brazilian population and that variation in hospitalization rates, length of stay, and HF-related deaths vary from country to country [21]. Regarding Brazilian data, there are some studies reporting a high mortality rate, with rates varying from 8.7% to 27.8% [14,18,22-24]. The BREATHE study also presented high in-hospital mortality rates among patients hospitalized for HF, at 12.6%, in addition to reporting that 30% of patients are hospitalized for poor adherence to drug treatment regimens [22].
A concerning fact is the cost of the HF patient. HF is a syndrome e with a high incidence of re-hospitalization, which also impacts patient prognosis, mortality, and quality of life, in addition to increasing costs within the health system. We observed that the accumulated 6-year cost for treating HF among patients >60 years of age was nearly Double the costs of treating the patients in the younger age bracket, despite the >60 patient group presenting a mean AIH value lower than that of the younger patients.
Conclusion
We conclude that based on the above data, even with the reduction in the absolute number of hospitalizations, HF related mortality is increasing. The older population presents a greater risk of in-hospital death and presents a greater aggregated cost as compared with younger patients with the same diagnosis, within the SUS, but this is likely repeated in non-governmental and insurance hospitals.
References
- Bocchi EA, Marcondes-Braga FG, Bacal F, Ferraz AS, Albuquerque D, Rodrigues D, et al. Sociedade Brasileira de Cardiologia. Atualizaço da Diretriz Brasileira de Insuficiência Cardíaca Crônica - 2012. ArqBrasCardiol. 2012; 98: 1-33.
- Gotsman I, Zwas D, Zemora Z, Jabara R, Admon D, Lotan C, et al. Clinical outcome of patients with chronic heart failure followed in a specialized heart failure center. Isr Med Assoc J. 2011; 13: 468-473.
- Pfeffer MA, Braunwald E, Moye LA, Basta L, Brown EJ Jr, Cuddy TE, et al. Effect of captopril on mortality and morbidity in patients with left ventricular dysfunction after myocardial infarction. Results of the survival and ventricular enlargement trial. The SAVE Investigators. N Engl J Med. 1992; 327: 669-677.
- Effects of enalapril on mortality in severe congestive heart failure. Results of the Cooperative North Scandinavian Enalapril Survival Study (CONSENSUS). The CONSENSUS Trial Study Group. N Engl J Med. 1987; 316: 1429-1435.
- Packer M, Bristow MR, Cohn JN, Colucci WS, Fowler MB, Gilbert EM, et al. The effect of carvedilol on morbidity and mortality in patients with chronic heart failure. U.S. Carvedilol Heart Failure Study Group. N Engl J Med. 1996; 334: 1349-1355.
- Granger CB, McMurray JJ, Yusuf S, Held P, Michelson EL, Olofsson B, et al. Effects of candesartan in patients with chronic heart failure and reduced left-ventricular systolic function intolerant to angiotensin-converting-enzyme inhibitors: the CHARM-Alternative trial. Lancet. 2003; 362: 772-776.
- Cleland JG, Daubert JC, Erdmann E, Freemantle N, Gras D, Kappenberger L, et al. The effect of cardiac resynchronization on morbidity and mortality in heart failure. Cardiac Resynchronization-Heart Failure (CARE-HF) Study Investigators. N Engl J Med. 2005; 352: 1539-1549.
- Pitt B, Zannad F, Remme WJ, Cody R, Castaigne A, Perez A, et al. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study Investigators. N Engl J Med. 1999; 341: 709-717.
- Willenheimer R, van Veldhuisen DJ, Silke B, Erdmann E, Follath F, Krum H, et al. Effect on survival and hospitalization of initiating treatment for chronic heart failure with bisoprolol followed by enalapril, as compared with the opposite sequence: results of the randomized Cardiac Insufficiency Bisoprolol Study (CIBIS)III. Circulation. 2005; 112: 2426-2435.
- Chun S, Tu JV, Wijeysundera HC, Austin PC, Wang X, Levy D, et al. Lifetime analysis of hospitalizations and survival of patients newly admitted with heart failure. Circ Heart Fail. 2012; 5: 414-421.
- Joynt KE, Jha AK. Who has higher readmission rates for heart failure, and why? Implications for efforts to improve care using financial incentives. Circ Cardiovasc Qual Outcomes. 2011; 4: 53-59.
- Barretto AC, Del Carlo CH, Cardoso JN, Morgado PC, Munhoz RT, Eid MO, et al. Hospital readmissions and death from Heart Failure--rates still alarming. Arq Bras Cardiol. 2008; 91: 335-341.
- Albanesi Filho FM. Insuficiência cardíaca no Brasil. ArqBrasCardiol. 1998; 71: 561-562.
- Carlo CH, Cardoso JN, Ochia ME, Oliveira MT Jr, Ramires JA, Pereira-Barretto AC. Variaço Temporal no Prognóstico e Tratamento da Insuficiência Cardíaca Avançada - Antes e Após 2000. Arq Bras Cardiol. 2014; 102: 495-504.
- Ministério da Saúde. [Internet]. DATASUS. Informaçes de saúde (TABNET). [acesso em 2015 set. 9].
- Amaral AC, Coeli CM, Costa Mdo C, Cardoso Vda S, Toledo AL, Fernandes CR. Perfil de morbidade e de mortalidade de pacientes idosos hospitalizados. Cad Saude Publica. 2004; 20: 1617-1626.
- Kaufman R, Azevedo VMP, Xavier RMA, Geller M, Chaves RBM, Castier MB. Insuficiência Cardíaca: Análise de 12 Anos da Evoluço em Internaçes Hospitalares e Mortalidade. Internacional Journalof Cardiovascular Sciences. 2015; 28: 276-281.
- Nogueira PR, Rassi S, Corrêa Kde S. Perfil epidemiológico, clínico e terapêutico da insuficiência cardíaca em hospital terciário. Arq Bras Cardiol. 2010; 95: 392-398.
- Almeida GAS, Teixeira JBA, Barichello E, Barbosa MH. Perfil de saúde de pacientes acometidos por insuficiência cardíaca. Esc Anna Nery. 2013; 17: 328-335.
- Chaudhry SI, Wang Y, Gill TM, Krumholz HM. Geriatric conditions and subsequent mortality in older patients with heart failure. J Am Coll Cardiol. 2010; 55: 309-316.
- Christ M, Störk S, Dörr M, Heppner HJ, Müller C, Wachter R, et al. Heart failure epidemiology 2000-2013: insights from the German Federal Health Monitoring System. Eur J Heart Fail. 2016; 18: 1009-1018.
- Albuquerque DC, Souza Neto JD, Bacal F, Rohde LEP, Pereira SB, Berwanger O, et al. I Registro Brasileiro de Insuficiência Cardíaca - aspectos clínicos, qualidade assistencial e desfechos hospitalares. Investigadores Estudo BREATHE. Arq Bras Cardiol. 2015; 104: 433-442.
- VillaCorta H, Mesquita ET, Cardoso R, Bonates T, Maia ER, Silva AC, et al. Preditores de sobrevida obtidos na unidade de emergência em pacientes atendidos por insuficiência cardíaca descompensada. Rev Port Cardiol. 2003; 22: 495-507.
- Silva PGMBe, Ribeiro DJ, Fernandes VA, Rinaldi DVS, Ramos DL, Okada MY, et al. Impacto inicial de uma clínica de insuficiência cardíaca em hospital cardiológico privado. Rev Bras Cardiol. 2014; 27: 90-96.
