Abstract
We are presenting the case of familial hypercholesterolemia, an important cause of premature and advanced coronary disease that is often misdiagnosed. In this case, we demonstrate not only the difficulty to attach the goals of lipid level, but also the importance of familial screening.
Keywords: Familial hypercholesterolemia; Coronary disease; Lipids
Case Presentation
A fifty year old man was transferred to the State Heart Institute of Rio de Janeiro (IECAC) for a coronarography after a non-ST-segment elevation myocardial infarction. He had history of hypertension and dyslipidemia since the age of 26, family history of sudden death (father at age 24) and a family history of dyslipidemia (brother and son).
During admission, an arcus corneae (Figure 1) was seen, suggesting familial hypercholesterolemia. The coronarography showed trivascular disease with 90% obstruction in medium LAD, proximal 80% in Cx and 99% proximal in right coronary artery. Because of the coronary anatomy a coronary bypass surgery was indicated.
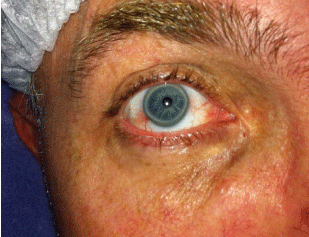
Figure 1: Arcus corneae.
During the pre-operatory exams a lipidogram was performed with a TC of 326mg/dl, HDL-28mg/dl, LDL-256mg/dl, and TG- 210mg/dl. The diagnosis of Familial Hypercholesterolemia (FH) was made using the Dutch criteria.
His son was screened and his lipid panel revealed: TC-312mg/dl, LDL-248mg/dl, HDL-38mg/dl and TG- 130mg/dl.
Currently, he is an outpatient the at the Rio de Janeiro State Coronary Disease Outpatient Unit, 3 years after surgery using atorvastatin 40mg, ezetemibe 10mg, atenolol 25mg bid, ASA 200mg od, and amlodipine 5mg od. He is asymptomatic, and hisTC-203, TG-132, HDL-32 and LDL-144.
Discussion
Familial hypercholesterolemia is a hereditary disease characterized by high plasma cholesterol levels, especially LDL-C, and is related to premature coronary disease. It can be linked to mutations that involve LDL receptors (LDL-R) ApoB or PCSK9 [1].
Some studies showed that the prevalence of FH in patients with acute coronary syndrome can be up to 8%, and in young people may reach 47.1% [2,3].
The Dutch Lipid Clinic Network Score diagnostic criteria involve family history, clinical history, physical exam, LDL levels and the DNA analysis. Our patient scored more than 8 points, confirming the diagnosis [1].
The most important medication for FH is statin therapy, but the patient didn’t tolerate the 80mg of atorvastatin because of myalgia, so we added ezetimibe. Even with double therapy he isn’t within the target LDL [1].
PCSK9 inhibitors are a promising medication that proved to lower LDL levels in patients with FH, in monotherapy or in association with statins and ezetimibe. They are used subcutaneously twice a month and have been associated with a reduction of up to 62% in LDL levels in heterozygous FH patients [4-6].
References
- Santos RD, Gagliardi AC, Xavier HT, Casella Filho A, Araújo DB, Cesena FY, et al. First Brazilian Guidelines for Familial Hypercholesterolemia. Arq Bras Cardiol. 2012; 99: 1-28.
- Nanchen D, Gencer B, Auer R, Raber L, Stefanini GG, Klingenberg R, et al. Prevalence and management of familial hypercholesterolaemia in patients with acute coronary syndromes. Eur Heart J. 2015; 36: 2438-2445.
- De Backer G, Besseling J, Chapman J, Hovingh GK, Kastelein JJ, Kotseva K, et al. Prevalence and management of familial hypercholesterolaemia in coronary patients: An analysis of EUROASPIRE IV, a study of the European Society of Cardiology. Atherosclerosis. 2015; 241: 169-175.
- Raal FJ, Stein EA, Dufour R, Turner T, Civeira F, Burgess L, et al. PCSK9 inhibition with evolocumab (AMG 145) in heterozygous familial hypercholesterolaemia (RUTHER-FORD-2): a randomised, double-blind, placebo-controlled trial. Lancet. 2015; 385: 331-340.
- Robinson JG, Nedergaard BS, Rogers WJ, Fialkow J, Neutel JM, Ramstad D, et al. Effect of evolocumab or ezetimibe added to moderate- or high-intensity statin therapy on LDL-C lowering in patients with hypercholesterolemia: the LAPLACE-2 ran-domized clinical trial. JAMA. 2014; 311: 1870-1882.
- Robinson JG, Farnier M, Krempf M, Bergeron J, Luc G, Averna M, et al. Efficacy and safety of alirocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015; 372: 1489-1499.
