Abstract
Coronary heart disease, referred to as CHD, is myocardial dysfunction and organic disease caused by coronary atherosclerosis stenosis and insufficiency of the blood supply, which has seriously affected human health as the deadliest diseases in the world [1]. Results showed that CHD is associated with hyperlipidemia, hypertension, smoking, diabetes, heredity and many other factors [2]. Currently, a variety of methods have been applied to treat the disease all over the world. In this paper, we make a mini review to the current situation of interventional treatment of CHD in China, and point out the existing inadequacies. Hoping to improve the curative effect in the treatment of CHD, we also put forward the corresponding solutions, and predict the future development trend.
Keywords: Coronary heart disease; Interventional therapy; Hypertension
Introduction
Coronary atherosclerotic heart disease is a heart disease characterized by myocardial ischemia, hypoxia or necrosis, which were caused by stenosis or obstruction of the coronary arteries brought on by atherosclerotic lesions of the coronary arteries, often referred to as CHD. It is the most common cardiovascular disease, with the highest mortality rate in the world. In recent years, the incidence of disease continues to rise, and it is a great threat to human health. WHO divided coronary heart disease into five types, including asymptomatic heart disease, angina pectoris, myocardial infarction, ischemic heart failure and sudden death. Although drug therapy, supportive therapy, surgical treatment and interventional therapy are all used clinically in the treatment of coronary heart disease, interventional therapy is the most widely used and with the best curative effect [3]. The interventional therapy of coronary artery disease is to send the catheter through the radial artery or other artery to the ascending aorta by the way of the carotid artery under the influence of the modern radiology image, and then explore the left or right coronary artery insertion, and then inject a certain amount of contrast agent to develop the coronary artery, with the aim to define the location, extent, and extent of the anatomy deformity and obstruction of the coronary artery, and finally examine and treat the cardiovascular disease [4]. Although interventional therapy has made great progress in the treatment of coronary heart disease, there are still some shortcomings, such as restenosis and a series of complications. If we can clearly understand the mechanism leading to restenosis and reduce the chance of complications by certain measures, interventional therapy will definitely make new achievements in the treatment of coronary heart disease.
Present Situation of Interventional Therapy for Coronary Heart Disease
Historical progress of interventional therapy for coronary heart disease
In 1929, Werner Forssmann, a German surgeon, proposed for the first time that a catheter could be inserted into the heart, which could be used to inject drugs into the heart or measure the blood pressure of the heart. However, it is not accepted because the catheter inserted into the heart may cause sudden death. Werner Forssmann personally tested and demonstrated the safety of the treatment with X rays, but has not been taken seriously yet. It was not until 1941 that two American doctors, Dickinson and Andre F. Cournand, recognized the feasibility of the treatment. Then cardiac catheterization was first applied to the measure of pulmonary arterial pressure and cardiac output, and diagnosis of congenital and rheumatic heart disease, this opened the prelude to cardiovascular interventional therapy. Werner Forssmann also won the Nobel prize for medicine in 1956.
The stage of percutaneous transluminal coronary angioplasty
Percutaneous transluminal coronary angioplasty, also referred to as PTCA (Figure 1), is a therapeutic method used to treat a coronary artery by dilating a narrow or obstructed coronary artery by sending a balloon catheter through percutaneous puncture. In 1964, Dotter, an American doctor, successfully treated a patient with severe embolism of the femoral artery using a home-made balloon catheter. In 1974, the German Andreas Grentzig successfully completed the world’s first case of PTCA. By 1985, Grint Metzger completed 2623 cases of PTCA alone, with the success rate as high as 90%. Since then, PTCA has been widely used in the world. With the improvement of equipment and the improvement of technology, the success rate of PTCA was also rising, and gradually became the most important method for the treatment of coronary artery obstructive disease. However, PTCA still faces a series of problems, such as acute vascular occlusion, low cardiac output syndrome, severe arrhythmia and the rate of restenosis in the middle and late stage is up to 50%. These are mainly because balloon dilate and tear atherosclerotic plaques [5]. The advent of BMS in 1987 overcame the shortcomings of PTCA.
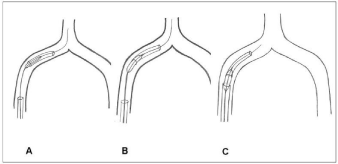
Figure 1: A PTCA balloon is passed over the wire into the broken catheter
fragment. The balloon is inflated to hold the broken catheter fragment [6].
The stage of bare-metal stents
Bare-metal coronary artery stents, also referred to as BMS, are used in percutaneous coronary intervention for a variety of indications, including stable and unstable angina, acute Myocardial Infarction (MI), and multiple-vessel disease. Urich Sigwart, a Swiss scholar working in France for the first time in 1987, applied metalbare stents to the human body, a bold landmark in the development of coronary artery therapy. BMS can maintain patency of the blood vessel by implanting stents, so it can be used to prevent Acute Myocardial Infarction (AMI). The restenosis rate after BMI is about 20~30%, only about 50% of PTCA. But because of the existence of metal foreign bodies in the blood vessel, the reaction of neointimal hyperplasia is more serious than PTCA.
The stage of drug eluting stents
A drug-eluting stent, also referred to as DES, is a peripheral or coronary stent (a scaffold) placed into narrowed, diseased peripheral or coronary arteries that slowly releases a drug to block cell proliferation, which came out in 2002 [7]. The broad spectrum of drug-eluting stents is divided into two broad categories. One is antithrombotic drug-coated stent, which coated phosphoryl choline, heparin, carbide, silicon carbon alloy and other substances on the stent surface to reduce thrombosis, thereby effectively preventing restenosis. The other is antiproliferative drug-coated stent, which fixed some anti-value-added drugs, such as paclitaxel, to the stent through a carrier. The drug is continuously released and interacts with the vascular lining to prevent hyperplasia and stenosis of the intima. Compared with BMS, DES significantly reduced the incidence rate of revascularization induced by restenosis, but there was no significant difference in the rate of death or myocardial infarction. DES has been widely used because of its greatly reduced stenosis rate, and is regarded as the second milestone in interventional treatment of coronary artery disease [8].
The stage of total absorption biodegradable vascular scaffold
Through the continuous research and development of scientific research personnel,biodegradable vascular scaffold, also referred to as BVS, came into being. In 2006, the company launched its first biodegradable stent. The polymeric materials, like PLLA and PDLLA, are continuously reduced in vivo by hydrolysis and enzymatic hydrolysis, eventually turned to water and carbon dioxide, which can be completely degraded in two or three years. Compared to DES, BVS can reduce the probability of stent thrombosis and stent rupture, and is conducive to the restoration of normal function of blood vessels. What is more, it does not affect the inspection of CT and MRI [9].
Current Situation of Interventional Therapy for Coronary Heart Disease
In the past thirty years, with the continuous development and improvement of coronary interventional treatment instruments and the emergence and application of new interventional technologies, the interventional therapy for coronary heart disease has made new progress in the international arena. But up to now, in terms of quality and quantity, coronary artery interventional therapy still cannot meet the needs of patients with coronary heart disease in our country. Interventional therapy has not yet formed a scale in most hospitals, and many families could not afford proper treatment because of the cost. What is more, due to technical reasons, the level of treatment of interventional techniques shows regional differences in China (Figure 2). There is a big gap between China and the developed countries, whether it is in the aspect of technical level or medical equipment. The development of direct stenting and unprotected left main coronary artery stenting in recent years, indicating that coronary artery interventional therapy has entered a highly mature stage of development.
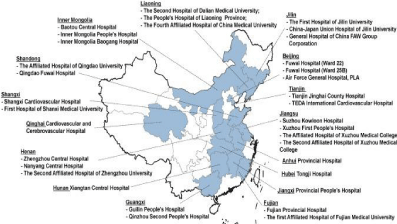
Figure 2: Geographic distribution of participating hospitals in the China patient-centered evaluative assessment of cardiac events (PEACE), prospective study of
percutaneous coronary intervention (PCI). The 34 participating centers are located in 20 of the 31 provinces in China [10].
The scope of application of coronary intervention
Early PTCA was limited to the treatment of stable angina pectoris, single coronary artery lesions and other simple lesions. However, after thirty years of development, PTCA can be used for the treatment of unstable angina, AMI, multivessel disease and other complex diseases.
The approach selection of coronary artery interventional therapy
Percutaneous transluminal coronary intervention: Clinical practice shows that percutaneous transluminal coronary intervention therapy can lead to a series of complications such as bleeding, subcutaneous hematoma, and arrhythmia, seriously affect the health of patients. Therefore, we should do good postoperative care, and take effective measures to reduce the probability of occurrence of complications in a certain extent [11].
Transradial transluminal coronary intervention: In recent years, transradial transluminal coronary intervention is widely applied for clinic. Compared with the femoral artery puncture, there is no need to lie in bed and with the advantages of faster recovery, it can significantly improve the curative effect. And it is more suitable for patients with femoral artery or external iliac artery stenosis, occlusion, or excessive tortuosity. Many hospitals in China have mastered this technology. But because radial artery puncture often use 6F guiding catheter, it has strong back force. So it is not proper for patients with complex lesions and requiring simultaneous implantation of an intra aortic balloon pump or a temporary pacemaker catheter.
Prediction of the Trend of Interventional Therapy for Coronary Heart Disease
Standardized treatment
The number of patients with coronary heart disease is rising in China, which puts forward higher technical level for doctors and nurses who are engaged in the treatment of coronary heart disease [12]. Not only should we make innovation in the surgical equipment, but also formulate the appropriate treatment plan according to the different conditions of different patients. At present, the regionalization of technical level and nonstandard management in our country should be taken seriously. Therefore, preoperative preparation, operation, and postoperative rehabilitation should all be checked. And hospitals need strict and standardized management. The government also should increase investment in talent resources in backward areas. Only in this way can more patients with coronary heart disease benefit from the treatment.
Combination of interventional therapy and stem cell therapy
Stem cells have the potential to differentiate into various cells and can be collected from bone marrow or from cord blood. The introduced stem cells can regenerate necrotic cells, vascular endothelial cells, or smooth muscle cells and restore their function. The current study has shown that the mechanism of stem cell therapy for coronary heart disease is that it can differentiate into vascular endothelial cells, smooth muscle cells, myocardial cells, secrete cytokines and be fused with myocardial cells [13]. Through the stent, interventional treatment can help the recanalization of contracted coronary artery. If the interventional therapy combined with stem cells technique, not only can make the patients recover fast after operation, but also will not affect the health of patients in the stent removal operation after recover. It also can effectively prevent the occurrence of stent loss and other emergency situations.
The combination of interventional therapy and 3D printing technology
With the progressing of 3D imaging technology and materials engineering, 3D printing technology can now apply to medical practice, such as treatment of congenital heart disease [14]. Because of the difference in the shape and thickness of each person’s coronary artery, the existing stent is often unable to meet the needs of patients. 3D printing just can solve this problem [15], for example, according to the patient’s coronary artery image to design a suitable stent, then the success rate ofsurgery and postoperative survival will naturally increase. The Chinese University of Hong Kong and the University of Hong Kong have taken the lead in applying 3D printing technology to complex cardiac surgery in Hong Kong, which improves the effectiveness and safety of surgical treatment. They created highsimulated 3D silica gel software models of complex heart to assist in preoperative planning especially in working out individualized treatment plans for patients. The relevant case has been published in the medical journal Circulation Cardiovascular Interventions.
Conclusion
With the improvement of living standards, the incidence of coronary heart disease is increasing both in China and in the world. Despite the ongoing advances in coronary interventions, there are a number of problems that need to be addressed, such as the high rate of late thrombosis caused by long term use of antiplatelet drugs and the high costs of stent [16]. There is still a long way to go for interventional treatment for coronary artery disease. Today, with the rapid development of science and technology, it is an irreversible trend to form a comprehensive method to treat coronary heart disease. It is only by combining a variety of technologies that interventional therapy for coronary artery disease may undergo a qualitative leap.
References
- Hightower HB, Robin NH, Mikhail FM, Ambalavanan N. Array comparative genomic hybridisation testing in CHD. Cardiol Young. 2015; 25: 1155-1172.
- Braga F, Pasqualetti S, Ferraro S, Panteghini M. Hyperuricemia as risk factor for coronary heart disease incidence and mortality in the general population: a systematic review and meta-analysis. Clin Chem Lab Med. 2016; 54: 7-15.
- De feyter PJ, Foley D. Coronary stent implantation: a pamacea for the interventional cardiologist. Eur Heart J. 2000; 21: 1719-1726.
- Naqvi SY, Klein J, Saha T, McCormick DJ, Goldberg S. Comparison of Percutaneous Coronary Intervention Versus Coronary Artery Bypass Grafting for Unprotected Left Main Coronary Artery Disease. Am J Cardiol. 2017; 119: 520-527.
- Murphy MC, Hansell HN, Ward K, Shaw RE. Differences in symptoms during and post PTCA versus rotational ablation. Prog Cardiovasc Nurs. 1994; 9: 4-9.
- Gupta AK, Purkayastha S, Krishnamoorthy T. Percutaneous retrieval of intravascular broken catheter fragments. A novel technique using a balloon. Interv Neuroradiol. 2005; 11: 149-154.
- Minha S, Pichard AD, Waksman R. In-stent restenosis of drug-eluting stents. Future Cardiol. 2013; 9: 721-731.
- Maupas E, Lipiecki J, Levy R, Faurie B, Karsenty B, Moulichon ME, et al. Safety and efficacy outcomes of 3rd generation DES in an all-comer population of patients undergoing PCI: 12-month and 24-month results of the e-biomatrix French registry. Catheter Cardiovasc Interv. 2017.
- Xiaofeng Ye, Liang Lu, Kolewe ME, Park H, Larson BL, Kim ES, Freed LE. A biodegradable microvessel scaffold as a framework to enable vascular support of engineered tissues. Biomaterials. 2013; 34: 10007-10015.
- Du X, Pi Y, Dreyer RP, Jing Li, Xi Li, Nicholas SD, et al. The China Patientcentered Evaluative Assessment of Cardiac Events (PEACE) prospective study of percutaneous coronary intervention: study design. Catheter Cardiovasc Interv. 2016; 7: 212-221.
- He YP, Lu ZG, Gu YW, Pan JW, Gao MF, Wei M. Impact of multifactor intensive intervention on self management, risk factor control and outcome of post percutaneous transluminal coronary intervention patients. Chinese Journal of Cardiology. 2012; 40: 1037-1040.
- He P, Yang Y, Qiao S, Bo Xu, Min Yao, Yongjian Wu, et al. Comparison of short- and medium-term clinical outcomes between transradial approach and transfemoral approach in a high-volume PCI heart center in China. PLOS One. 2015.
- Wang SH. Application of stem cells in the treatment of coronary heart disease. Chin J Geriatr Heart Brain Vessel Dis. 2008; 10: 873-874.
- Wang QT, Wang YJ. Application of three-dimensional printing technology in the percutaneous coronary intervention field. China Medical Equipment. 2016; 13: 129-133.
- Gu Q, Tomaskovic-Crook E, Wallace GG, Crook JM. 3D bioprinting human induced pluripotent stem cell constructs for in situ cell proliferation and successive multilineage differentiation. Adv Healthc Mater. 2017.
- Teirstein P, Reilly JP. Late stent thrombosis in brachytherapy: the role of long-term antiplatelet therapy. J Invasive Cardiol. 2002; 14: 109-114.
