Abstract
Objective: Er:YAG laser etching is reported to have conflicting effects on adhesion to dentin. As ethanol has been proved to increase the infiltration capacity and adhesive performance of resins, this study was conducted to evaluate the effect of ethanol pretreatment on the Shear Bond Strength (SBS) of a self-etch adhesive to Er:YAG laser etched coronal and root dentin.
Methods: Forty extracted human premolars were ground flat exposing the coronal and root dentin surfaces, and randomly divided into four groups according to Er:YAG laser etching and ethanol pretreatment. The polished surfaces were either used as controls or etched with Er:YAG laser-80 mJ, 10 Hz, VSP (Fidelis III/Fotona) (n=20). Prior to adhesive application, the coronal and root dentin of 10 teeth from each group were pretreated with ethanol (100%) (n=10). Adper Easy One (3M ESPE) self-etch adhesive was applied to the specimens and composite resin blocks (Z250, 3M ESPE) were built using a jig (Ultradent). SBS was tested and the data were evaluated using one-way ANOVA, Tukey’s HSD test, and t-test (p=0.05).
Results: The Control/Ethanol group exhibited the highest values, which were significantly higher than those of the Er:YAG and Er:YAG/Ethanol groups for both coronal and root dentin (p<0.05). Comparison of two dentin substrates in the control groups did not show any significant differences (p>0.05). SBS to root dentin was higher in the Er:YAG group, whereas bonding to coronal dentin was higher in the Er:YAG/Ethanol group (p<0.05).
Conclusion: Adhesive performance of the self-etch adhesive to Er:YAG laser etched dentin was not improved by ethanol pretreatment.
Keywords: Ethanol; Self-Etch adhesive; Er:YAG laser etching; Coronal dentin; Root dentin
Introduction
With the growing demand for minimally invasive and esthetic dentistry applications, many of the current restorative procedures are based on adhesive techniques, which have been constantly improved to obtain more effective bonding between restorative materials and dental substrates [1]. For this purpose, the focus of studies has shifted to find new bonding techniques, new adhesive materials, and alternative instruments that can better prepare the tooth tissues for bonding procedures.
The pretreatment of dental tissues prior to adhesive procedures is an important step that directly affects the clinical success of the restorations. Hence, new instruments such as dental lasers have been recommended as alternative tools to conventional methods. Among the various types of lasers currently available, the erbium: yttrium aluminum garnet (Er:YAG) laser is one of the highest recommended types of laser for hard tissue applications, as its wavelength (2.94 μm) coincides with the main absorption band of water (~3.0 μm) and it is well absorbed by hydroxyapatite [2]. The use of the Er:YAG laser for dentin pretreatment (Er:YAG laser etching) was reported to yield a microretentive surface with open dentin tubules, which are considered ideal for adhesion [3-5]. However, although some studies report that laser irradiation has no or a slight effect on dentin bonding, most researchers have concluded that laser irradiation impairs the resin bond strength to dentin [6-8]. Some authors have speculated that the lack of adhesive resin infiltration was the main explanation for the low bond strength of bonding agents to laser irradiated dentin [9,10]. In addition, studies in the literature present the results of current adhesive systems that were developed to act on the tooth substrate prepared by conventional techniques [8,10-12]. Thus, the effect of Er:YAG laser etching in combination with new adhesion strategies and adhesive systems on bonding to dentin remains to be clarified.
Parallel to the evolution of new instruments, many efforts have also been directed towards formulating new adhesive systems that are easier, faster, and more user-friendly. For this purpose, self-etch adhesives with a reduced number of bonding steps were introduced. The most recent type combining all the components into the liquid is referred to as a “one-step self-etch” adhesive system [13]. One-step self-etch adhesives are recommended to ensure maximum adhesion through the mechanism of improved monomer penetration into the tooth substrate as well as improved wet ability of the tooth surface via the resin components [14]. These systems not only lessen the clinical application time, but also significantly reduce technique-sensitivity and the risk of making errors during application and manipulation as the infiltration of resin occurs simultaneously with the self-etching process, by which the risk of discrepancy between both processes is much lower [14].
In the basics of dentin bonding, water that fills the intrafibrillar and interfibrillar spaces after apatite dissolution by acids should be totally displaced and infiltrated by the resin monomers to form a strong and durable “hybrid layer” [15]. Therefore, incomplete replacement of water during adhesive application leaves behind a hydrated collagen matrix that could adversely affect the adhesion to dentin [15]. However, to date, complete displacement of water from the interfibrillar compartment by contemporary dentin adhesives has not been reported [15]. The “ethanol wet-bonding” technique has been suggested to overcome this limitation, in which ethanol instead of water is used to support the demineralized dentin collagen matrix. In this technique, ethanol is used to chemically dehydrate the demineralized collagen matrix as it is a polar solvent with lower hydrogen bonding capacity than water. The resultant shrinkage of the collagen fibrils in the lateral dimension and reduction in hydrophilicity of the collagen matrix create wider interfibrillar spaces for hydrophobic resins to infiltrate the matrix more completely as a potential mechanism for better resin-dentin adhesion [16,17]. It was clearly demonstrated that ethanol increases the infiltration capacity and adhesive performance of adhesive resins [18,19].
Efficacy of adhesive systems is generally evaluated based on their ability to bond to coronal dentin. Nevertheless, the increasing age of the population, and developments in adhesive dentistry and periodontology significantly increased the demand for restoration of root dentin defects [20]. Since “ethanol wet bonding” is a promising technique and, to date, no available report has described the adhesion of self-etch adhesives to Er:YAG laser etched dentin regions in combination with ethanol pretreatment, the present study was conducted to evaluate the effect of ethanol pretreatment on Shear Bond Strength (SBS) of a one-step self-etch adhesive to Er:YAG laser etched coronal and root dentin. The hypotheses tested were: I) Er:YAG laser etching increases the bond strength of the onestep self-etch adhesive to coronal and root dentin regardless of the type of dentin and ethanol pretreatment; II) Ethanol pretreatment increases the bond strength of the one-step self-etch adhesive to dentin, regardless of the type of dentin and Er:YAG etching; III) There are no differences in bond strengths between different dentin regions (coronal or root) either with Er:YAG laser etching or ethanol pretreatment.
Materials and Methods
Table 1 shows the materials used in this study. Forty extracted intact human premolars were treated with a periodontal scaler to remove organic debris before being cleaned with water pumice slurry. Each tooth was examined under a stereomicroscope (Olympus SZ 61, Olympus Corporation, Tokyo, Japan) at ×40 magnification to eliminate those with cracks and hypoplastic defects. The superficial enamel and cementum were abraded from the buccal tooth surfaces with a 180-grit Silicon Carbide (SiC) paper under running water to expose both coronal and root dentin within the same tooth. The prepared surfaces were polished with 200-grit, 320-grit, and 400-grit SiC papers under copious water for 10 s each and, finally, with a 600- grit paper for 60 s, to create standard and clinically relevant smear layers. All specimens were examined under the stereomicroscope at ×40 magnification to ensure that no enamel and cementum remained and that no pulp had been exposed. Each tooth was then mounted in a Plexiglas mold with autopolymerizing acrylic resin (Metafast, Sun Medical, Moriyama, Japan) so that the flattened surface of the tooth was positioned parallel to the base. The specimens were then placed in distilled water to reduce the temperature from the exothermic reaction of the embedding resin. After ultrasonic cleaning with distilled water for 3 min to remove debris, the surfaces were washed and dried with oil-free compressed air. The teeth were randomly divided into four groups according to Er:YAG laser etching and ethanol pretreatment (n=10).
Materials
(Batch no #)
Composition
Manufacturer
Application procedure
Adper Easy One
(#2012204)
HEMA, Bis-GMA, methacrylated phosphoric esters, 1,6 hexanediol dimethacrylate, methacrylate functionalized polyalkenoic acid, silica filler, ethanol, water, initiators, stabilizers
3M ESPE,USA
Apply adhesive and leave for 20 s. Dry with air for 5 s and light cure for 10 s
Filtek Z250
(# 6020A3)
BiS-GMA, UDMA, BiS-EMA, TEGDMA, zirconia/silica fillers
3M ESPE,USA
Apply 1.5 mm thick increments. Light cure for 20 s
Table 1: Materials used in the study.
Control group
The specimens in this group received no pretreatment. Specimens with polished surfaces served as controls.
Control/Ethanol group
Specimens with polished surfaces were rinsed with absolute ethanol (100% ethanol) for 30 s and excess ethanol was removed from the specimens with filter paper in order to leave a moist, ethanolsaturated dentine surface [21].
Er:YAG group
A square of 3 × 3 mm was marked on the coronal and root dentin surfaces of each specimen to indicate the test site. The dentin surfaces were manually irradiated to simulate the clinical conditions, by scanning movements, perpendicular to the surface, in focus mode (approximately 1 mm away from the surface) with an Er:YAG laser (Fidelis III, Fotona Medical Lasers, Ljubljana, Slovenia) with the settings 10 Hz, 80 mJ, 100 μs pulse duration with air-water cooling, using an R14 handpiece.
Er:YAG/Ethanol group
After Er:YAG laser etching, the dentin surfaces were pretreated with absolute ethanol for 30 s and excess ethanol was removed from the specimens with filter paper as in the Control/Ethanol group.
Subsequently, a one-step self-etch adhesive (Adper Easy One/3M ESPE, St. Paul, MN, USA) was applied to the test sites of the specimens (middle third of the crown and the cervical third of the root) according to the manufacturers’ instructions. Following the adhesive procedures, a special Teflon jig (Ultradent, Salt Lake City, UT, USA) with an inner diameter of 2.3 mm and a height of 3 mm was attached to the prepared dentin surfaces and a resin composite (Filtek Z250, 3M ESPE, St. Paul, MN, USA, A3 shade) was placed in two increments (1.5 mm thick each). Each increment was light cured for 20 s (Elipar Free Light; 3M Espe, St. Paul, MN, USA). After curing, the Teflon jig surrounding the composite resin was carefully removed. The specimens were stored in distilled water at 37 °C for 24 h, and then loaded by a metal rod parallel with and close to the bonding interface at 1 mm/min in shear mode until rupture occurred, on an Instron Universal Testing Machine (Lloyd Instruments Ltd, Foreham, Hampshire, UK). SBS values were calculated as the ratio of fracture load to bonding area and are expressed in megapascals. The fractured surface of each specimen was examined with a stereomicroscope (Olympus SZ 61, Olympus Corporation, Tokyo, Japan) at ×30 magnification to determine the mode of failure. The failure mode was classified as adhesive (between dentin and adhesive or within adhesive), cohesive (within the composite or dentin), or mixed (combination of adhesive and cohesive failures). Selected samples of each experimental and control group that exhibited a representative failure mode and a SBS close to the average value were processed for Scanning Electron Microscope (SEM) evaluation. The authors employed common procedures for SEM specimen preparation, including rinsing with distilled water, fixation in a 2.5% gluteraldehyde in cacodylate buffer solution and dehydration in ascending concentrations of ethanol. Each sample was then mounted on aluminum stubs, sputter coated with gold and examined under SEM (JEOL 6400, JEOL, Tokyo, Japan).
The data obtained from the SBS testing were subjected to statistical analyses for differences among (one-way ANOVA, Tukey’s HSD tests) and within the groups (t-test). The calculations were conducted using SPSS 15.0 software for Windows (SPSS, Chicago, USA) and the level of significance was set at p<0.05 for all tests.
Results
Table 2 demonstrates the results of one-way ANOVA, Tukey’s HSD, and t-tests. The SBS of the control groups was significantly higher than that of the Er:YAG groups. The Control/Ethanol group exhibited the highest values, which were significantly higher than those of the Er:YAG and Er:YAG/Ethanol groups both on coronal and root dentin (p<0.05). Comparisons of two dentin substrates in the control groups did not show any significant difference (p>0.05). SBS to root dentin was higher than coronal dentin for the Er:YAG group, whereas bonding to coronal dentin was higher than root dentin for the Er:YAG/Ethanol group (p<0.05).
Groups
Coronal dentin
(n=10)
Root dentin
(n=10)
Coronal/Root Dentin Comparison within Groups
Control Group
11.5±6.5ab
10.7±3.5xy
p = 0.38
Control/Ethanol Group
15.6±6.4a
14.4±3.6x
p =0.51
Er:YAG Group
5.3±1.4c
6.9±2.9yz
p = 0.04
Er:YAG/Ethanol Group
7.7±2.8bc
5.2±1.8z
p =0.02
Data with the same superscripts are not statistically different. (p<0.05).
Table 2: The Mean ± SD Shear Bond Strength Values (MPa).
The failure mode distributions are presented in Table 3. The most frequently observed failures were adhesive in nature for all groups both for coronal and root dentin except for the Control/Ethanol coronal dentin subgroup, in which mixed failures were predominantly observed (Figures 1-4).
Groups
n
A (%)
M (%)
C (%)
Control Group
Coronal dentin
10
5 (50%)
4 (40%)
1 (10%)
Root dentin
10
9 (90%)
0 (0%)
1 (10%)
Control/Ethanol Group
Coronal dentin
10
2 (20%)
7 (70%)
1 (10%)
Root dentin
10
6 (60%)
2 (20%)
2 (20%)
Er:YAG Group
Coronal dentin
10
8 (80%)
2 (20%)
0 (0%)
Root dentin
10
8 (80%)
1 (10%)
1 (10%)
Er:YAG/Ethanol Group
Coronal dentin
10
8 (80%)
2 (20%)
0 (0%)
Root dentin
10
10 (100%)
0 (0%)
0 (0%)
Total
80
56 (70%)
18 (22.5%)
6 (7.5%)
A: Adhesive; M: Mixed; C: Cohesive
Table 3: Failure mode distributions of the specimens.
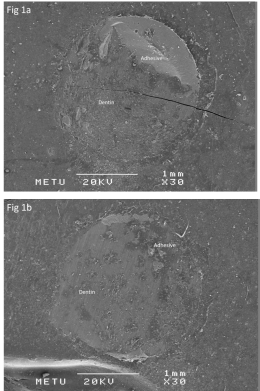
Figure 1: SEM micrographs of Control groups (X30). The specimens failed
adhesively at the resin dentin interface and within the adhesive both on
coronal (1a), and root dentin (1b).
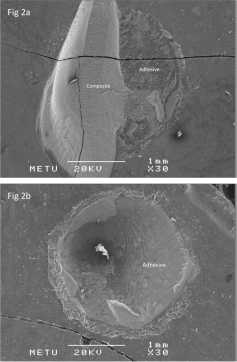
Figure 2: SEM micrographs of Control/Ethanol groups (X30). The interface
failed mixed adhesively within the adhesive and cohesively within the
composite on coronal dentin (2a); Failure within the adhesive was observed
on root dentin (2b).
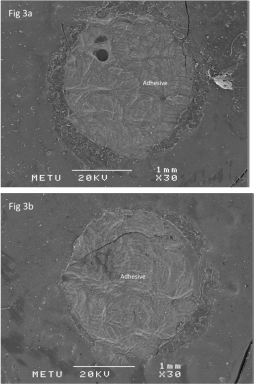
Figure 3: SEM micrographs of Er:YAG groups (X30). The interfaces failed
adhesively within the adhesive both on coronal (3a), and root dentin (3b).
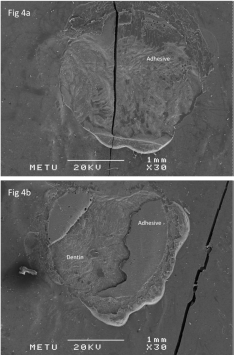
Figure 4: SEM micrographs of Er:YAG/Ethanol groups (X30). The interface
failed adhesively within the adhesive on coronal dentin (4a); whereas the
specimen failed adhesively at the resin dentin interface and within the
adhesive on root dentin (4b).
Discussion
Today one-step self-etch adhesives are the first choice of many clinicians due to their user-friendliness and reduced techniquesensitivity [13]. However, self-etch dental adhesives are a complex mixture of components including reactive monomers, an association of dissolved hydrophilic and hydrophobic monomers, cross linkers, initiators, and solvents. Although adhesives should ideally be formulated based on hydrophobic monomers of high molecular weight without additives such as water and solvents, monomers, hydrophilic resin diluents, and solvents are incorporated into these adhesives due to the necessity for adhesive to penetrate the microporosities of dentin [22]. Hydroxyethylmethacrylate (HEMA) is a widely used hydrophilic polar monomer that significantly improves adhesion by enhancing the wettability of dentin [23]. It also acts as a solvent and helps to prevent hydrophilic and hydrophobic phase separations [24,25]. Some co-solvents such as acetone, ethanol, or butanol are also included in these adhesives to provide organic molecules of lower polarity to enter a homogeneous phase [26]. The use of ethanol as co-solvent is reported to significantly increase the bond strength, as it allows more resin infiltration [27]. Based on previously reported data [26,27], Adper Easy One (3M ESPE, St. Paul, USA), a one-step self-etch adhesive that includes HEMA monomer and ethanol co-solvent, was used in this study.
Utilizing the Er:YAG laser etching settings suggested by the manufacturer and previous studies [8,11,28], the present study demonstrated that Er:YAG laser etching with the current settings decreased the bond strength of the one-step self-etch adhesive to coronal and root dentin, by which the first hypothesis was rejected. This finding was in accordance with the results reported by De Munck et al.. [4] and Van Meerbeek et al.. [3], which revealed that the microtensile bond strength of self-etch adhesive was significantly lower when the dentin surface was irradiated by Er:YAG laser with the parameters 80 mJ, 10 Hz. Ramos et al. [12] evaluated the effect of Er:YAG laser on SBS of different adhesives to dentin and concluded that Er:YAG laser irradiation with 80 mJ, 2 Hz adversely affected the bond strength of the self-etch adhesive used. De Oliveira et al. [9] investigated the micromorphology of resin–dentin interfaces using etch&rinse and self-etch adhesive systems on laser-treated dentin surfaces and they concluded that Er:YAG laser irradiation of dentin surfaces at 120 or 200 mJ/pulse resulted in morphological changes in the hybrid layer and resin tags for all the adhesives tested. They also reported poor resin infiltration into the peritubular dentin, and that the expected funnel-shape appearance at the entrance of dentin tubules was less evident following Er:YAG laser irradiation.
It is well known that the dentin surfaces are covered with a smear layer when prepared with burs or polishing papers [9]. As the self-etch adhesives are normally applied onto smear layer covered dentin, their mechanism is based on incorporating the smear layer into the hybrid layer [9]. The lack of smear layer after Er:YAG laser etching may be a reason for the decrease in SBS of the current one-step self-etch adhesive in this study. Moreover, the thermal collagen degradation, and morphological, compositional, and phase alterations, such as carbonate loss, formation of modified hydroxyapatite-like crystals, and increase in acid-resistance, after Er:YAG laser etching could also explain the impaired adhesion to dentin surfaces in this study [9,10,29].
For achieving better adhesion to Er:YAG laser irradiated tooth tissues, the adherent surfaces should be modified to create a more suitable host when using the current adhesive systems. Optimum wettability of solid surfaces and the infiltration capacity of the adhesive resins are of paramount importance in adhesion [30,31]. Ethanol-wet bonding was introduced to increase the wettability of the dentin surface, permitting the hydrophobic adhesive monomers to infiltrate into the collagen network and prevent phase separation [32,33]. There are limited data showing that ethanol-wet bonding increased the adhesion capacity of etch&rinse adhesive systems to coronal dentin [34]. However, it is difficult to compare the results of the present study with the literature as the dentin substrates, pretreatment procedures, and adhesive systems utilized are quite different [17,19,34]. This study is unique in evaluating the effect of ethanol pretreatment on SBS of a one-step self-etch adhesive to dentin either polished with SiC papers (control) or etched with Er:YAG laser. According to the findings of this study, the second hypothesis was rejected. Although an increase trend was observed in SBS of the Control/Ethanol group in comparison with the Control group, there were no significant differences within the Control and Er:YAG groups with ethanol pretreatment for coronal or root dentin.
The adhesion process depends not only on the adhesive systems and surface pretreatment procedures but also on the dental substrates [35]. In the last few decades, the age of the patient population has increased and individuals have a greater tendency to maintain their natural dentition throughout their entire life. Gingival recession and subsequent root exposure leading to root caries have become more prevalent in the population [36]. Clinically, the margins of many adhesive restorations on the root surface are thought to be positioned in cervical outer root dentin [37]. While the adhesion to coronal dentin is important, that to root dentin is also critical for the clinical performance of restorations partially or totally located below the cementoenamel junction [38]. However, only a few studies have been published comparing the adhesive properties of coronal and root dentin [39-41]. In a previous work, Fogel et al.. [39] reported that the permeability of root dentin was lower than that of coronal dentin, which might reduce hydrophilic resin infiltration capacity into the tissue and result in lower bond strength values in root dentin. Comparing regional tensile-bond strength, Yoshiyama et al. [40] demonstrated that bond strength to coronal dentin was significantly higher than that to cervical root dentin. They related the decreased bond strength in root dentin to the lower number and the narrower diameter of the dentinal tubules. Gurgan et al. [41] showed that the SBS of two-step self-etch adhesive to coronal dentin was higher than that to root dentin, although no significant difference was found for one-step self-etch adhesive between coronal and root dentin. The present study aimed to provide further information about the effect of current adhesive systems and surface treatment strategies on bond strength to coronal and root dentin regions. Although there were no significant differences between the SBS to coronal and root dentin regions with/without ethanol pretreatment in the control groups, the results of this study were in accordance with the literature for the Er:YAG/Ethanol group, which revealed higher SBS on coronal dentin [39,40]. Furthermore, the SBS to root dentin was significantly higher in the Er:YAG group. Thus the findings of this study refuted the third hypothesis.
It should be noted that only one representative one-step selfetch adhesive was used and only one set of irradiation parameters was tested in this study. Although the present findings might open a gateway, this in vitro study could not predict clinical performance under in vivo conditions, as the absence of dentin fluid in the extracted teeth may have influenced the bond strengths. Therefore, further in vitro and in vivo studies testing a greater variety of adhesive systems and different Er:YAG laser settings, and evaluating the resin-dentin interfaces are required.
Clinical Relevance
1. Er:YAG laser etching with the current settings impaired the SBS of the current one-step self-etch adhesive to coronal and root dentin surfaces and it could not be improved by ethanol pretreatment.
2. Ethanol pretreatment might have a positive effect on the adhesive performance of the self-etch adhesive to control (non laser etched) dentin regardless of dentin region.
3. The effects of Er:YAG laser etching and ethanol pretreatment might differ between coronal and root dentin surfaces.
References
- Ikemura K, Endo T. A review of our development of dental adhesives--effects of radical polymerization initiators and adhesive monomers on adhesion. Dent Mater J. 2010; 29: 109-121.
- Souza-Zaroni WC, Chinelatti MA, Delfino CS, Pecora JD, Palma-Dibb RG, Corona SA. Adhesion of a self-etching system to dental substrate prepared by Er:YAG laser or air abrasion. J Biomed Mater Res B Appl Biomater. 2008; 86: 321-329.
- Van Meerbeek B, De Munck J, Mattar D, Van Landuyt K, Lambrechts P. Microtensile bond strengths of an etch&rinse and self-etch adhesive to enamel and dentin as a function of surface treatment. Oper Dent. 2003; 28: 647-660.
- De Munck J, Van Meerbeek B, Yudhira R, Lambrechts P, Vanherle G. Microtensile bond strength of two adhesives to Erbium:YAG-lased vs. bur-cut enamel and dentin. Eur J Oral Sci. 2002; 110: 322-329.
- Firat E, Gurgan S, Gutknecht N. Microtensile bond strength of an etch-andrinse adhesive to enamel and dentin after Er:YAG laser pretreatment with different pulse durations. Lasers Med Sci. 2010.
- de Souza AE, Corona SA, Dibb RG, Borsatto MC, Pecora JD. Influence of Er:YAG laser on tensile bond strength of a self-etching system and a flowable resin in different dentin depths. J Dent. 2004; 32: 269-275.
- Ramos RP, Chimello DT, Chinelatti MA, Nonaka T, Pecora JD, Palma Dibb RG. Effect of Er:YAG laser on bond strength to dentin of a self-etching primer and two single-bottle adhesive systems. Lasers Surg Med. 2002; 31: 164- 170.
- Eguro T, Maeda T, Otsuki M, Nishimura Y, Katsuumi I, Tanaka H. Adhesion of Er: YAG laser-irradiated dentin and composite resins: application of various treatments on irradiated surface. Lasers Surg Med. 2002; 30: 267-272.
- de Oliveira MT, Arrais CA, Aranha AC, de Paula Eduardo C, Miyake K, Rueggeberg FA, et al. Micromorphology of resin-dentin interfaces using onebottle etch&rinse and self-etching adhesive systems on laser-treated dentin surfaces: a confocal laser scanning microscope analysis. Lasers Surg Med. 2010; 42: 662-670.
- Esteves-Oliveira M, Zezell DM, Apel C, Turbino ML, Aranha AC, Eduardo Cde P, et al. Bond strength of self-etching primer to bur cut, Er,Cr:YSGG, and Er: YAG lased dental surfaces. Photomed Laser Surg. 2007; 25: 373-380.
- Visuri SR, Gilbert JL, Wright DD, Wigdor HA, Walsh JT. Shear strength of composite bonded to Er:YAG laser-prepared dentin. J Dent Res. 1996; 75: 599-605.
- Ramos RP, Chinelatti MA, Chimello DT, Borsatto MC, Pecora JD, Palma- Dibb RG. Bonding of self-etching and total-etch systems to Er:YAG laserirradiated dentin. Tensile bond strength and scanning electron microscopy. Braz Dent J. 2004; 15: SI9-20.
- Peumans M, Kanumilli P, De Munck J, Van Landuyt K, Lambrechts P, Van Meerbeek B. Clinical effectiveness of contemporary adhesives: a systematic review of current clinical trials. Dent Mater. 2005; 21: 864-881.
- Van Meerbeek BVM, Inoue S, Yoshida Y, Peumans M, Lambrechts P, Vanherle G. Adhesives and cements to promote preservation dentistry. Oper Dent. 2001; 1: 119-144.
- Vaidyanathan TK, Vaidyanathan J. Recent advances in the theory and mechanism of adhesive resin bonding to dentin: a critical review. J Biomed Mater Res B Appl Biomater. 2009; 88: 558-578.
- Sadek FT, Pashley DH, Nishitani Y, Carrilho MR, Donnelly A, Ferrari M, et al. Application of hydrophobic resin adhesives to acid-etched dentin with an alternative wet bonding technique. J Biomed Mater Res A. 2008; 84: 19-29.
- Pashley DH, Tay FR, Carvalho RM, Rueggeberg FA, Agee KA, Carrilho M, et al. From dry bonding to water-wet bonding to ethanol-wet bonding. A review of the interactions between dentin matrix and solvated resins using a macromodel of the hybrid layer. Am J Dent. 2007; 20: 7-20.
- Nishitani Y, Yoshiyama M, Donnelly AM, Agee KA, Sword J, Tay FR, et al. Effects of resin hydrophilicity on dentin bond strength. J Dent Res. 2006; 85: 1016-1021.
- Hosaka K, Nishitani Y, Tagami J, Yoshiyama M, Brackett WW, Agee KA, et al. Durability of resin-dentin bonds to water- vs. ethanol-saturated dentin. J Dent Res. 2009; 88: 146-151.
- Proenca JP, Polido M, Osorio E, Erhardt MC, Aguilera FS, Garcia-Godoy F, et al. Dentin regional bond strength of self-etch and total-etch adhesive systems. Dent Mater. 2007; 23: 1542-1548.
- Kim J, Gu L, Breschi L, Tjaderhane L, Choi KK, Pashley DH, et al. Implication of ethanol wet-bonding in hybrid layer remineralization. J Dent Res. 2010; 89: 575-580.
- Erickson RL. Surface interactions of dentin adhesive materials. Oper Dent. 1992; 5: 81-94.
- Pashley DH, Ciucchi B, Sano H, Horner JA. Permeability of dentin to adhesive agents. Quintessence Int. 1993; 24: 618-631.
- Moszner N, Salz U, Zimmermann J. Chemical aspects of self-etching enameldentin adhesives: a systematic review. Dent Mater. 2005; 21: 895-910.
- Van Landuyt KL, Snauwaert J, Peumans M, De Munck J, Lambrechts P, Van Meerbeek B. The role of HEMA in one-step self-etch adhesives. Dent Mater. 2008; 24: 1412-1419.
- Van Landuyt KL, Snauwaert J, De Munck J, Peumans M, Yoshida Y, Poitevin A. et al. Systematic review of the chemical composition of contemporary dental adhesives. Biomaterials. 2007; 28: 3757-3785.
- Nikhil V, Singh V, Chaudhry S. Comparative evaluation of bond strength of three contemporary self-etch adhesives: An ex vivo study. Contemp Clin Dent. 2011; 2: 94-97.
- Burkes EJ, Hoke J, Gomes E,Wolbarsht M. Wet versus dry enamel ablation by Er:YAG laser. J Prosthet Dent. 1992; 67: 847-851.
- Dela Rosa A, Sarma AV, Le CQ, Jones RS, Fried D. Peripheral thermal and mechanical damage to dentin with microsecond and sub-microsecond 9.6 microm, 2.79 microm, and 0.355 microm laser pulses. Lasers Surg Med. 2004; 35: 214-228.
- Aguilar-Mendoza JA, Rosales-Leal JI, Rodriguez-Valverde MA, Gonzalez- Lopez S, Cabrerizo-Vilchez, MA. Wettability and bonding of self-etching dental adhesives. Influence of the smear layer. Dent Mater. 2008; 24: 994- 1000.
- Gregoire G, Dabsie F, Dieng-Sarr F, Akon B, Sharrock P. Solvent composition of one-step self-etch adhesives and dentine wettability. J Dent. 2011; 39: 30- 39.
- Becker TD, Agee KA, Joyce AP, Rueggeberg FA, Borke JL, Waller JL, et al. Infiltration/evaporation-induced shrinkage of demineralized dentin by solvated model adhesives. J Biomed Mater Res B Appl Biomater. 2007; 80: 156-165.
- Wang Y, Spencer P. Hybridization efficiency of the adhesive/dentin interface with wet bonding. J Dent Res. 2003; 82: 141-145.
- Huang X, Li L, Huang C, Du X. Effect of ethanol-wet bonding with hydrophobic adhesive on caries-affected dentine. Eur J Oral Sci. 2011; 119: 310-315.
- Osorio E, Toledano M, da Silveira BL, Osorio R. Effect of different surface treatments on In-Ceram Alumina roughness. An AFM study. J Dent. 2010; 38: 118-122.
- Yuan Y, Shimada Y, Ichinose S, Tagami J. Hybridization quality in cervical cementum and superficial dentin using current adhesives. Dent Mater. 2008; 24: 584-593.
- Kikushima D, Shimada Y, Foxton RM, Tagami J. Micro-shear bond strength of adhesive systems to cementum. Am J Dent. 2005; 18: 364-368.
- Tanaka S, Sugaya T, Kawanami M, Nodasaka Y, Yamamoto T, Noguchi H, et al. Hybrid layer seals the cementum/4-META/MMA-TBB resin interface. J Biomed Mater Res B Appl Biomater. 2007; 80: 140-145.
- Fogel HM, Marshall FJ, Pashley DH. Effects of distance from the pulp and thickness on the hydraulic conductance of human radicular dentin. J Dent Res. 1988; 67: 1381-1385.
- Yoshiyama M, Sano H, Ebisu S, Tagami J, Ciucchi B, Carvalho RM, et al. Regional strengths of bonding agents to cervical sclerotic root dentin. J Dent Res. 1996; 75: 1404-1413.
- Gurgan S, Firat E, Baysan A, Gutknecht N, Imazato S. Effects of ozone and ND: YAG laser pretreatment on bond strength of self-etch adhesives to coronal and root dentin. Photomed Laser Surg. 2010; 28: S3-9.
