Abstract
Objective: Pulmonary Artery Hypertension (PAH) is an independent risk factor for increased morbidity in Sickle Cell Disease (SCD) patients. Tricuspid Annular Plane Systolic Excursion (TAPSE) can be used as a surrogate measure for PAH. The objective of this study was to determine whether lower TAPSE values are associated with increased Emergency Department (ED) and hospital utilization.
Methods: TAPSE measurements were retrospectively obtained from bedside echocardiograms from a convenience sample of 28 SCD patients presenting to the ED with SCD pain. TAPSE was considered abnormal if <24.9mm, one standard deviation below the mean TAPSE for SCD patients. Medical records were reviewed to determine ED visits and hospital overnight stays over a two-year period. A t-test analysis and Pearson’s correlation were used for each variable.
Results: The initial sample included 28 SCD patient encounters. TAPSE measurements were abnormal in 5 patients and normal in 23 patients. The mean number of ED visits/year for the abnormal and normal TAPSE group were 23.00 and 16.87, respectively (p=0.57) with moderate negative linearity (p=0.03). The mean number of hospitalized days for abnormal and normal TAPSE groups was 108.8 and 59.6, respectively (p=0.10) with moderate negative linearity (p=0.07).
Conclusion: Lower TAPSE values (<24.9mm) in SCD patients were associated with higher ED and hospital utilization. If findings are replicated in larger studies, TAPSE may serve as a marker of morbidity in SCD patients presenting to the ED.
Keywords: Pulmonary artery hypertension; Tricuspid Annular Plane Systolic Excursion; Emergency Department
Introduction
Sickle Cell Disease (SCD) is a debilitating disease characterized by painful, unpredictable Vaso-Occlusive Episodes (VOEs) and chronic multi-organ damage [1]. SCD affects approximately 100,000 patients in the United States, with a disproportionate impact on underrepresented minorities [2,3]. SCD is associated with high healthcare utilization and costs and frequent Emergency Department (ED) visits [4-7]. Higher SCD-related ED utilization is associated with more severe disease and poorer outcomes [8,9].
Pulmonary Artery Hypertension (PAH) is a known complication of SCD, thought to be caused by chronic hypoxemia and vasoconstriction of the pulmonary vasculature due to chronic hemolysis [10]. PAH has been associated with higher SCD-related complications and greater hospitalization rates for SCD patients [10- 12]. Tricuspid Annular Plane Systolic Excursion (TAPSE) is a noninvasive echocardiographic assessment of right ventricular function that measures the longitudinal excursion of the tricuspid annulus, and it can be reliably measured by emergency medicine physicians with experience in echocardiography [13-15]. TAPSE is a strong prognostic factor for non-SCD patients with PAH [14-16], but its role in SCD remains unclear. SCD patients have higher mean baseline TAPSE measurements than non-SCD patients due to enlarged chamber sizes in this population [17,18], rather than better overall right ventricular functioning. We hypothesized that values lower than the baseline TAPSE value for SCD patients would be associated with increased morbidity in sickle cell patients.
To the best of our knowledge, this is the first study exploring the relationship between TAPSE and SCD-related ED visits and hospital utilization.
Materials and Methods
Study design and setting
This was a retrospective, observational study performed on a convenience sample of adult SCD patients presenting to the ED of a large, academic hospital with over 2,000 ED visits per year for SCDrelated complaints. The study was reviewed and approved by the Institutional Review Board of the University of Illinois at Chicago. Recruitment of patients occurred over three time periods during the summers of 2016, 2018 and 2019, based on availability of research personnel.
Selection of participants
Hemodynamically stable SCD patients who were 18 years or older presenting to the ED with a chief complaint of sickle cell VOE were included. Study participants were approached for participation after their initial ED evaluation and treatment plan was started for their pain.
Ultrasound protocol
Limited Bedside Echocardiograms (LBEs) were performed as part of a protocol for a separate study using a M4S-RS GE Vivid transducer by one of five emergency department providers (four attending physicians, one nurse practitioner) with at least one year of ultrasound fellowship training. Each LBE included at minimum an apical four chamber view, but other views were also obtained at the discretion of the sonographer. Echocardiograms were electronically stored for later analysis.
Methods of measurement
TAPSE was retrospectively measured from saved LBEs using GE Echopacs software by the principle investigator with at least one research associate present. Both the primary investigator and the research associate were blinded to the primary and secondary outcomes. Two separate TAPSE measurements were obtained from the echocardiograms. If there was a greater than 2mm variation in the first two measurements, a third measurement was obtained; the largest value was used for the analysis.
TAPSE measurements were considered abnormal if they were less than or equal to 24.9mm, a cut-off chosen because it is one standard deviation below the previously published mean TAPSE for SCD patients [17]. LBEs were excluded if the lateral tricuspid annulus could not be visualized throughout the entire cardiac cycle on the saved video clip.
Each subject’s medical record was reviewed for basic demographic information, hydroxyurea use, hemoglobin levels, and to determine ED visits, days hospitalized, and TAPSE measurement on prior echocardiograms over the 24-month period preceding enrollment date. Information was stored in REDCap, a web-based application for secure research databases.
Outcomes measured
The primary outcome measured was the mean number of ED visits per year. The secondary outcome was the total number of days in the hospital per year.
Primary and secondary data analysis
Patients were stratified into two distinct groups of normal (>24.9mm) and abnormal (<24.9mm) TAPSE measurements. The two groups were compared using unpaired t-tests (homoscedastic) for mean number of ED visits, overnight hospitals days, hemoglobin, and age using GraphPad.com, and confirmed in Microsoft Excel 2016. Pearson’s correlation coefficients with confidence intervals and Hedges’ g tests for effect size were calculated using socscistatistics. com. Chi-square test or Fischer’s exact tests were used to evaluate variables like sex and hydroxyurea use among the two groups.
Results
Characteristics of study subjects
Fifty-six patients were enrolled in this study. Fifty LBEs were performed on 49 patients. Thirty LBEs had adequate visualization of the lateral tricuspid annulus to obtain TAPSE measurements. The mean TAPSE measurement for the sample was 27.9mm, with 5 SCD patients in the abnormal TAPSE group and 23 SCD patients in the normal TAPSE group. Two were excluded from the analysis: one patient was visiting Chicago and had no prior records at the study institution and one patient had an artificial tricuspid valve. One patient was an extreme outlier of ED utilization with 114 ED visits, (i.e. >4 standard deviations from sample mean). Primary and secondary analyses were performed both with and without exclusion of the outlier. Twenty-six patients were included in the final analysis after exclusion of the extreme outlier.
All study participants included in the analysis were African American, including 14 females and 14 males. The majority of participants were hemoglobin phenotype SS (n=27) with a mean hemoglobin of 8.8g/dl and a mean age of 29 years old. There were no statistical differences between the abnormal and normal groups with regard to age, sex, hemoglobin, or hydroxyurea use. Twelve patients had echocardiograms documented in the 24 months prior to enrollment, two from abnormal TAPSE group, but none had TAPSE measurements or PAH mentioned on echocardiography report.
Primary and secondary analysis
The mean TAPSE values were 22mm and 29mm for the abnormal and normal TAPSE groups, respectively. The mean number of ED visits for abnormal and normal TAPSE groups were 23.00 and 16.87, respectively, p=0.57, 95% CI [-15.08,27.34]. TAPSE had a moderately negative correlation with number of ED visits, r(26)= -0.42, p=0.03, and the effect size was small with a Hedges’ g of 0.29. With the outlier excluded, the mean number of ED visits for the abnormal group was 23.00 and 12.00 for the normal TAPSE group, respectively, p=0.02, 95% CI= [1.72,20.28] (Table 1) with Hedges’ g of 1.24 indicating large effect size on the data. TAPSE measurements had a statistically significant negative correlation with the number of ED visits in this sample, r(24)= -0.53, p<0.01 (Figure 1).
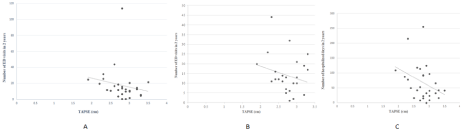
Figure 1: A) Number of ED visits in two years as a function of patients’ TAPSE values. B) Number of ED visits in two years as a function of patients’ TAPSE values with outlier excluded. C) Patients’ TAPSE values and their number of hospitalized days in two years.
Patients in the abnormal TAPSE group spent more days in the hospital compared to patients in the normal TAPSE group, with the mean number of days being 108.80 and 59.6, respectively. However, this finding was not statistically significant, p=0.10, 95% CI= [-7.89,106.27] (Table 1). The size of effect on this data set was fairly large though, with a Hedges’ g of 0.87. TAPSE had a moderate negative linear correlation with total days spent in the hospital in this sample, but it was not statistically significant r(26) = -0.35, p=0.07 (Figure 1). Exclusion of the outlier had minimal effect on the mean number of hospital stays, Pearson’s correlation coefficient, and effect size (Table 1).
Abnormal TAPSE <24.9mm
Normal TAPSE >24.9mm
p-value (abnormal vs. normal)
Number of patients (Total 28)
5
23
Mean TAPSE (SD)
22mm (0.19)
29mm (0.25)
<0.0001
Number of ED visits within 2 years - Mean (SD)
23 (7.48)
16.87 (23.06)
0.57
Number of overnight stays within 2 years - Mean (SD)
108.8 (63.55)
59.6 (57.44)
0.1
% High ED utilizers8
100%
82.60%
0.57
Age - Mean (SD)
33.4 (14.60)
35.48 (12.49)
0.75
Hgb - Mean (SD)
9.22 (1.87)
8.75 (2.06)
0.64
Hydroxyurea use
80%
56.50%
0.33
% Female
60
47.8
0.62
% Male
40
52.2
Table 1A: Characteristics of patients in each TAPSE group with outlier included.
Abnormal TAPSE <24.9mm
Normal TAPSE group minus outlier
p-value (abnormal vs. normal minus outlier)
Number of patients (Total 28)
5
21
Mean TAPSE (SD)
22mm (0.19)
28.9mm (0.22)
<0.0001
Number of ED visits within 2 years - Mean (SD)
23 (7.48)
12.00 (9.32)
0.02
Number of overnight stays within 2 years - Mean (SD)
108.8 (63.55)
58.90 (59.67)
0.11
% High ED utilizers8
100%
76.20%
0.55
Age - Mean (SD)
33.4 (14.60)
36.52 (12.58)
0.63
Hgb - Mean (SD)
9.22 (1.87)
8.63 (2.08)
0.57
Hydroxyurea use
80%
61.90%
0.44
% Female
60
52.4
0.76
% Male
40
47.6
Table 1B: Characteristics of patients in each TAPSE group with outlier excluded.
Limitations
This study was comprised of a convenience sample of patients enrolled at a single institution with retrospective TAPSE measurements, which limits the generalizability of the findings. Also, the study was likely underpowered. Study participants had higher ED and hospital utilization than the usual SCD patient population presenting to the ED, as well as overall lower TAPSE values [8], suggesting possible selection bias.
Most LBEs were performed by sonographers unaware that TAPSE would later be measured, possibly explaining why only 60% of LBEs had adequate visualization of the lateral tricuspid annulus [19-21]. Focused training may be needed before TAPSE is routinely measured on SCD patients in the ED.
Discussion
In our sample, TAPSE was inversely associated with both the number of ED visits and the number of days spent in the hospital, although the results were only significant after an extreme outlier was excluded. Larger studies are needed to determine if these correlations hold true [22-25].
PAH is a well-established risk factor for increased morbidity in SCD patients that must be measured either via right heart catheterization or indirectly estimated using Tricuspid Regurgitation Velocity (TRV) combined with an estimate of right atrial pressure; both methods require cardiology consultation. TAPSE can reliably be measured at the bedside without Doppler imaging from a single apical 4-chamber view [26,27].
If decreases in TAPSE prove an accurate indicator of morbidity in SCD, then TAPSE may be a useful risk stratification tool for SCD patients in the ED. TRV is sometimes abnormal for SCD patients during VOEs, then normalizes in steady state [28]. If the same is true for TAPSE, measurements in the ED can be compared to baseline outpatient measurements to determine if there is a change from steady state. A change from baseline TAPSE could indicate a more serious VOE similar to the way a drop in hemoglobin from baseline would.
Author Contributions
JC conceived the study and designed the methodology. HS, SM, and DG undertook recruitment of patients and managed data. HS, AR, and AH analyzed the data. JC, HS, and TK drafted the manuscript, and DG contributed to its revision. JC takes responsibility for the paper as a whole.
Acknowledgements
Thank you to Dr. Heather Prendergast, Dr. Wesley Eilbert, and Dr. Marina Del Rios for their support and contributions in editing this manuscript. We would also like to thank Dr. Leah Finkel, Dr. Pavitra Kotini-Shah, and Savannah Soppet for assisting with patient enrollment in the study and Mallory Hawksworth and Yaejin Park for assisting with data analysis. Lastly, we’d like to thank the Craig Fellowship program at the University Of Illinois College Of Medicine and the L@S GANAS program at the University of Illinois Chicago for their additional support.
References
- Platt OS, Brambilla DJ, Rosse WF, et al. Mortality In Sickle Cell Disease -- Life Expectancy and Risk Factors for Early Death. N Engl J Med. 1994; 330: 1639-1644.
- Chakravorty S, Williams TN. Sickle cell disease: a neglected chronic disease of increasing global health importance. Arch Dis Child. 2015; 100: 48-53.
- Loureiro MM, Rozenfeld S. Epidemiology of sickle cell disease hospital admissions in Brazil. Revista de Saúde Pública. 2005; 39.
- Yusuf HR, Atrash HK, Grosse SD, Parker CS, Grant AM. Emergency Department Visits Made by Patients with Sickle Cell Disease. American Journal of Preventive Medicine. 2010; 38: S536-S541.
- Okam MM, Shaykevich S, Ebert BL, Zaslavsky AM, Ayanian JZ. National Trends in Hospitalizations for Sickle Cell Disease in the United States Following the FDA Approval of Hydroxyurea, 1998-2008. Medical Care. 2014; 52: 612-618.
- Lanzkron S, Carroll CP, Haywood C. The burden of emergency department use for sickle-cell disease: An analysis of the national emergency department sample database. Am J Hematol. 2010; 85: 797-799.
- Shankar SM, Arbogast PG, Mitchel E, Cooper WO, Wang WC, Griffin MR. Medical care utilization and mortality in sickle cell disease: A populationbased study. Am J Hematol. 2005; 80: 262-270.
- Aisiku IP, Smith WR, McClish DK, et al. Comparisons of High Versus Low Emergency Department Utilizers in Sickle Cell Disease. Annals of Emergency Medicine. 2009; 53: 587-593.
- Carroll CP, Haywood C, Lanzkron S. Prediction of onset and course of high hospital utilization in sickle cell disease. Journal of Hospital Medicine. 2011; 6: 248-255.
- Gladwin MT, Sachdev V, Jison ML, et al. Pulmonary Hypertension as a Risk Factor for Death in Patients with Sickle Cell Disease. N Engl J Med. 2004; 350: 886-895.
- Agarwal M, Shah M, Patel B, et al. Association between Pulmonary Hypertension and Clinical Outcomes in Hospitalized Patients with Sickle Cell Disease. ATS Journals. 2018; 198: 534-537.
- Kanter J, Bhor M, Li X, Li F, Paulose J. High Healthcare Utilization in Adolescents with Sickle Cell Disease Prior to Transition to Adult Care: A Retrospective Study. Journal of Health Economics and Outcomes Research. 2019; 6.
- Daley J, Grotberg J, Pare J, et al. Emergency physician performed tricuspid annular plane systolic excursion in the evaluation of suspected pulmonary embolism. The American Journal of Emergency Medicine. 2017; 35: 106-111.
- Forfia PR, Fisher MR, Mathai SC, et al. Tricuspid Annular Displacement Predicts Survival in Pulmonary Hypertension. Am J Respir Crit Care Med. 2006; 174: 1034-1041.
- Alerhand S, Hickey SM. Tricuspid Annular Plane Systolic Excursion (TAPSE) for Risk Stratification and Prognostication of Patients with Pulmonary Embolism. The Journal of Emergency Medicine. 2019.
- Tello K, Axmann J, Ghofrani HA, et al. Relevance of the TAPSE/PASP ratio in pulmonary arterial hypertension. International Journal of Cardiology. 2018; 266: 229-235.
- Ramani GV, Edelman K, López-Candales A. Standard measures of right ventricular function assessment in adult patients with acute sickle cell crises. International Journal of Cardiology. 2009; 132: 448-450.
- Chiadika S, Lim-Fung M, Llanos-Chea F, et al. Echocardiographic parameters to identify sickle cell patients with cardio-pathology. Echocardiography. 2018; 35: 1271-1276.
- Dampier C, LeBeau P, Rhee S, et al. Health-Related Quality of Life in Adults with Sickle Cell Disease (SCD): A Report from the Comprehensive Sickle Cell Centers Clinical Trial Consortium. American Journal of Hematology. 2011; 86: 203-205.
- Brousseau D, Owens P, Mosso A, Panepinto J, Steiner C. Acute care utilization and rehospitalization for sickle cell disease. JAMA. 2010; 303: 1288-1294.
- Benenson I, Jadotte Y, Echevarria M. Factors influencing utilization of hospital services by adult sickle cell disease patients: a systematic review. JBI Database of Systematic Reviews and Implementation Reports. 2017; 15: 765-808.
- Epstein K, Yuen E, Riggio J, Ballas S, Moleski S. Utilization of the office, hospital and emergency department for adult sickle cell patients: a five-year study. Journal of the National Medical Association. 2006; 98: 1109-1113.
- Baum K, Dunn D, Gillian M. The Painful Crisis of Homozygous Sikcle Cell Disease: A study of risk factors. Archives of Internal Medicine. 1987; 147: 1231-1234.
- Wang W, Ware R, Miller S, et al. Hydroxycarbamide in very young children with sickle-cell anaemia: a multicentre, randomised, controlled trial (BABY HUG). The Lancet. 2011; 377: 1663-1672.
- Kushel M, Perry S, Bangsberg D, Clark R, Moss A. Emergency Department Use Among the Homeless and Marginally Housed: Results From a Community-Based Study. American Journal of Public Health. 2002; 92: 778- 784.
- Jaworsky D, Gadermann A, Duhoux A, et al. Residential Stability Reduces Unmet Health Care Needs and Emergency Department Utilization among a Cohort of Homeless and Vulnerably Housed Persons in Canada. Journal of Urban Health. 2016; 93: 666-681.
- Raven M, Billings J, Goldfrank L, Manheimer E, Gourevitch M. Medicaid Patients at High Risk for Frequent Hospital Admission: Real-Time Identification and Remediable Risks. Journal of Urban Health. 2009; 86: 230-241.
- Machado R, Mack AK, Martyr S, Barnett C, MacArthur P, Sachdev V. Severity of pulmonary hypertension during vaso-occlusive pain crisis and exercise in patients with sickle cell disease. Br J Haematol. 2007; 136: 319-325.
