Research Article
Austin Orthop. 2018; 3(1): 1009.
The Surgical Treatment of Lumbar Brucellar Spondylitis Byposterior Approach
Tian Ye and Xining Y*
Department of Orthopaedics, the First Affiliated Hospital of Hebei North University, Zhangjiakou, China
*Corresponding author: Xining Y, Department of Orthopaedics, the First Affiliated Hospital of Hebei North University, Zhangjiakou, China
Received: April 17, 2018; Accepted: May 21, 2018; Published: May 28, 2018
Abstract
Objective: This study investigate the effect of surgical treatment of lumbar spondylitis, which used posterior approach to remove the lesion, graft the bone between transverse process and used nail rod system to make Internal fixation.
Methods: From February 2011 to April 2017, 62 cases of lumbar brucellar spondylitis were analyzed retrospectively in the No. 1 Affiliated Hospital of Hebei North University in Zhangjiakou City, Hebei Province, China. Including 37 male and 25 female patients aged 24 to 61; average age was (42.8±1.5). With an average duration of 4-28 months, average month was (6.6±1.8). All the patients have the history of contact the source of animal, impurity diet history or other pathogen exposure history. The result of X-ray, CT, MRI, c-reactive protein and blood sedimentation, Rose Bengal Plate Agglutination test (RBPT) and Standard tube Agglutination Test (SAT) check were positive. The outcome also conforms to National Health and Family Planning Commission of the People`s Republic of China WS 269-2007 brucellosis diagnostic criteria and principles of treatment. Preoperative, doxycycline + rifampicin + sulfamethoxazole were used for 56 days. Next, Surgical treatment was performed by using posterior approach to remove the lesion, graft the bone between transverse process and used nail rod system to make Internal fixation. Post-operative, the antibulimia drugs was used again until the C-reactive protein, blood pressure, RBPT test and the SAT test were negative. Furthermore, other 2 weeks medication should be used necessary. During drugs oral therapy time, the monitoring indexes of related infections were dynamically rechecked to monitor liver and kidney function. Visual Analogue Scale (VAS) was used to assess the degree of lower limb pain and lower back pain and Oswestry Disability Index (ODI) was used to assess the degree of recovery of waist function, Frankel spinal cord injury classification method was used to determine the recovery of spinal cord function.
Results: The operation time was 165-235 min, averaging (175.3±22.1) min. Intra operative bleeding was 260~510ml, averaging (338.3±75.9) ml. The length of hospitalization was 8~14 days, on average (11.99±3.25) days. No intra operative vascular injury or spinal cord injury. The incisions were healed well. The follow-up postoperative was more than 12 months, averaging month is 18.2±4.5. The infection symptoms disappeared. After 3 months, the blood sedimentation and other infection indexes were returned to normal. The result of X-ray examination showed that bone healing was obtained in transverse process between 3~12 months, and the fusion time of bone graft was 7~11 months, average month is (8.4±1.2). After 3 months, 6 months and 12 months follow-up, VAS score points was (3.05±0.65), (1.88±0.55) and (0.31±0.42) respectively. Compared with preoperative points (6.67±1.85), which were significantly lower. The results was statistically significant (P=0.012); the classification of Frankel spinal cord injury was significantly better than before (P=0.022). The ODI functional disorder index was (21.15±5.35), (12.26±4.55) and (5.31±3.12), lower than preoperative significantly (37.87±4.85), and the results were statistically significant (P=0.031).
Conclusions: We could remove the lesion, graft the bone between transverse process and use nail rod system to make internal fixation by posterior approach, thoroughly remove the lesion which was granulation tissue or abscess of lumbar spine or around the spinal canal. For the vertebral canal and nerve root canal, a complete decompression cam is created. After using nail rod system to make internal fixation, the lumbar spine could have an immediately stabilized. This method could recover the normal physiological protuberance of lumbar spine and prevent the instability occur in lumbar spine. For lumbar Brucella spondylitis, combine with long time oral therapy and posterior approach operation was an effective treatment method.
Keywords: Brucellosis; Surgical Treatment; Spondylitis; Lumbar Spine
Introduction
Spinal Brucellosis was a kind of spine infection that occurred in the spinal joint space or the surrounding tissues of spine. The illness triggered inflammation that present in vertebral body or spinal intervertebral discs. It was commonly known as Brucellar Spondylitis (BS) [1-4]. According to the report of Turgut et al. [5], the morbidity of lumbar BS was 68%. Drug oral therapy was the primary way to treat BS, but when it occurred: intractable pain in the spine lesion; large and unabsorbable abscess or lumbar muscle abscess; spinal cord or nerve root compression; spinal instability or other local symptoms was not ameliorated. Surgical treatment was scientific and reasonable [1, 6-10]. This was a clinical research that about 62 cases of lumbar BS patients, which in our hospital from February 2011 to April 2017, and the report was as follows.
Data and Methods
This group had 62 cases, 37 male, 25 female, age 24-61 years old, average age was (42.8±1.5). All cases had the contact history with epidemic animal, history of unclean diet or other contact history with pathogenic bacteria. 24 cases of which were in epidemic area. The onset time was 4 to 28 months, average (6.6±1.8) months. The disease onset occult, progress was slow, with different degrees of clinical symptoms, such as: Fever, night sweats, fatigue, lower back pain or sensory abnormalities, etc. There were 39 cases, which had spinal cord, cauda equina or nerve root compression; meanwhile all this 39 cases had varying degrees of numbness, radiative pain, local tenderness, percussion pain, reflex or anal sphincter dysfunction. The lymphatic system and genitourinary infection existed on 21 cases. All patients were successfully treated with surgery, no death or other unexpected result, and postoperative follow-up was over 12 months, average month was (18.2±4.5).
Imaging examination
All 62 cases underwent X-ray, CT, and MRI before the surgery. The results showed that 55 patients (88.70%) were affected by two vertebral bodies, and the others were affected by three or more vertebral bodies.
X-ray showed: The intervertebral space of 38 cases became extremely small, and the density of which increased, the images of which also changed. The articular surfaces of 12 cases had bone destruction, which happened to the intervertebral joints with lesions. There were 43 cases, which showed can cellated bone erosion in the periphery of the vertebral body, and different degrees of bone sclerosis existed at the edge of the vertebral body. Among them, 7 cases had the change that named bird’s mouth shape, i.e. in another way, a compact unstructured shadow had emerged. 10 cases had happened zygapophyseal joint bone destruction, which near the lesion. This change affected the stability of the spine; large bone destruction occurred in 6 cases, which destroyed the range over 1.5cm2; visible lumbar muscles shadow or the soft tissue shadow around the vertebrae presented around the lumbar muscles.
CT showed: There were 38 cases which showed bone destruction in the intervertebral disc, which affected the articular surface. The articular surface was altered by hardening and hyperplasia, and bone destruction was found in the central part of the lesion. In 43 cases, the bone destruction of vertebral body occurred a kind of changed named “lacing vertebra”, that was, there were different sclerosis bands around the bone destruction lesion, and new bone destruction were seen in the hyperplasia of the new bone. There were 18 cases which showed this kind of change in the zygapophyseal joint. There were 17 cases which periosteum of vertebral body occurred “lips” change. That was imaging findings of periosteal calcification; 15 cases, which transverse process area appeared hyperplasia structure changed, just like a hat on it; there were 22 cases, which bone destruction of vertebral body connected with the soft tissue shadow of the vertebra. The boundary of the soft tissue was clear, but the structure was irregular, and the lateral lumbar muscle was extruded.
The MRI showed: The intervertebral space of 38 cases became extremely small, and the disc of the vertebra was a signal of inflammatory change, bone destruction occurred in the terminal plate of vertebral body; There were 42 cases, which edge of the vertebral body had an can cellated bone erosion, and bone marrow edema was observed in the vertebral body. In 22 cases, we found an MRI signal that had irregular abscesses on the lateral structure of the vertebra; In 39 cases, it was found that the epidural abscess of the spinal canal was altered, the damaged intervertebral disc or the proliferative inflammatory granulation tissue, and the corresponding plane spinal cord or cauda equina and nerve root were compressed.
Laboratory examination
In the 62 cases in this group, Erythrocyte Sedimentation Rate (ESR) increased and C - reactive Protein (CRP) increased, ESR was 30~110mm/h, CPR was 48~115mg/L. There were 18 positive cases of Rose Bengal Plate Agglutination test (RBPT), 54 cases were positive in Standard tube Agglutination Test (SAT). All examinations were conducted in accordance with WS 269-2007 “brucellosis diagnostic criteria and principles of treatment”. Patients with preoperative fever were examined by Brucella bacteriology during the fever, 39 cases of which were tested for blood culture and 10 were positive. 23 cases were tested for bone marrow culture and 8 positive cases. During the operation time, there were 44 cases that the contents of the lesion had been cultured, and 22 cases were positive.
Treatment method
Preoperative preparation: All the patients undergoing the operation had been treated with oral therapy: Doxycycline, rifampicin, sulfamethoxazole. The treatment time was more than 2 weeks. The systemic symptoms improved, but the local symptoms did not improve significantly. There was one or more of the following situations:
1. Intractable pain in the lesion of the lumbar spine;
2. The abscess of the vertebra or the abscess of the lumbar was not absorbed or changed;
3. The spinal cord or the nerve root pressure;
4. Local symptoms did not improve;
5. Unstable spine. Preoperative, the ECG, laboratory examination and imaging examination should be checked.
All checks were perfect and no surgical contraindications. Surgical treatment was performed to remove the lesion completely.
Surgical methods: Our operation chose general anesthesia, tracheal intubation, and prone position, posterior and middle approach of the spine. Layer by layer, cut the skin and subcutaneous tissue. The spinal muscle and paraspinal soft tissue were separated. Let the spinous process of the vertebral body, vertebral plate, zygapophyseal joint could be seen. To enlarge the surgical field of vision, to focus on the lesion vertebral body, and to the upper and lower part of the vertebral body, a vision of the distance of the vertebral body was revealed. C-arm X-ray machine perspective. At the vertebral pedicle of the three vertebral bodies, centered on the diseased vertebral body. Placed the pedicle screw accurately. (if intraoperative findings: Pathological changes of the vertebral body bone destruction was not serious, less bone hyperplasia sclerosis and vertebral arch root transpedicular bone was better, we used the pedicle screws, after daub streptomycin powder, nailing directly; if intraoperative findings: the vertebral body was damaged severely and the spine was unstable. We performed pedicle screw fixation over the diseased vertebral body.) We began to clear pathological changes of the vertebral body lesions, when the spine was fixed and the structure of it was stable. Next, bone graft was performed between transverse processes of diseased vertebral bodies. C-arm X-ray machine perspective. Removed both sides vertebral plate of the diseased vertebral body to expand and decompress the spinal canal. After the spinal cord, epidural sac or nerve root of the corresponding segment of the vertebral body were exposed clearly and accurately, used surgical instruments carefully to remove the inflammatory tissue and pus from the spinal canal. If it was in front of the spinal cord, in front of the epidural, the posterior longitudinal ligament, or the lumbar spinal nerve root, there was a limited and enclosed inflammatory granulomatosis or abscess. Incised the pericardial membrane carefully. Remove the inflammatory granuloma or abscess. Moderately stretch the cauda equina or nerve root. Exposed the posterior margin of the lesion or the nerve root canal. Removed the bone destruction area of the posterior edge of the vertebral body or the nerve-root canal thoroughly. Moderately stretched the cauda equine to make the gaps of the lesion spine visible. Remove part of the vertebral lesion fiber ring. When the surgical field showed clearly, shave the fibrous ring and nucleus pulposus of the lesion spine thoroughly. At the same time, the damaged cartilage plates need to be removed. In the case of a significant hardening of the vertebral bone, it is required to remove the hardened transsexual bone, until the wound had blood ooze. In this group, there were 7 patients with paraspinal abscess. We had a partial resection of the transverse process of the lesion spine first. The surgical field was well exposed. With the help of C-arm X-ray machine, Use a multiangle and different size of spoon to curette the lesion. Removed the abscess or inflammatory granulomatous tissue and bone destruction carefully, which was at the anterior or para vertebrae of the vertebral body. Use pressure hemostatic or bipolar coagulator to stop bleeding. Rinse the area with saline again and again. The intervertebral disc endoscope was placed into the intervertebral space and a view was observed to assess how the diseased tissue was removed. If it was necessary, removed the residual lesion once again. Used the bone file to polish the transverse process of the vertebral body until the wound bleeding. When the lesion occurred in the center of the spine body or the lesion bone which was removed over 1cm3. You could crush the severed lamina and then blend in with a 1g of streptomycin, plant to the bone defect. When bone grafting was insufficient, it was a feasible option to select the autologous iliac bone graft. Rinsed the wound with more than 3000ml of gentamicin rinsing saline. Then, placed 1 or 2 drainage tubes and close the wound layer by layer.
Post-operative treatment: Postoperative nursing of spinal surgery was performed, and antibiotics were used for 3~5 days to prevent postoperative infection. Nutrition should be strengthened. During this time, liver and kidney function should be monitored. Post-operative, all cases were requested to lie in bed absolutely for 5~7days.The drainage was in the flat position. When the cases had a 24-hour drainage rate <50ml, the drainage could be removed. We would get the stitches out 2 weeks Post-operative. Post-operative 3~4 weeks, patients could be able to walk with a protective waist. Instruct patients to exercise the upper back on the bed. Increase the intensity of the activity gradually. We chose the oral therapy that doxycycline + rifampicin + sulfamethoxazole when the operation was finished until the C-reactive protein, ESR, RBPT and SAT was negative, and the oral therapy continued for 2 weeks.
Evaluation of surgical effect
1 year post-operative, the X-ray examination was reviewed at 3 month, 6 month and 12 month. The fusion of bone grafts and the fixation system were mastered. We used the VAS score to assess the degree of lower extremity pain and lower back pain, the Frankel spinal cord injury classification method to determine the recovery of spinal cord function and the ODI functional disability index to assess the degree of labor recovery.
Statistical analysis
SPSS 20.0 software was used to make statistical analysis. Patient’s age, duration time, operation time, length of hospital stay for measurement data and normally distributed, with x̅±s; VAS score and ODI index were compared with single factor analysis of variance. The rank sum test was used for the classification of Frankel spinal cord injury. P < 0.05 was considered statistically significant.
Results
There were no major vascular injuries or spinal cord injury in this group. The posterior lesion was removed clearly. The operation time was 165~235 min, average time is (175.3±22.1). The amount of in traoperative bleeding was 260~510ml, average (338.3±75.9) ml. The length of hospitalization was 8~14days, average (11.99±3.25). The wound was healed very well. There were 5 cases of fever, the highest was 38.50C. The anti-infection oral therapy was applied again. After three to five days, the body temperature was back to normal. 14 days later, the stitches were recovered. The wound was healed well. Postoperative follow-up of all cases was over 12 months, average 18.2±4.5 months. There were no complications such as recurrence of lesion, formation of sinus tract, incision infection or internal fixation failure. The symptoms of infection were all disappeared. From 3 to 12 months, all patients should have X-ray examination. The result showed that the bone graft fusion was very well. The fusion time of bone grafting was 7~11 months, average (8.4±1.2) months. The fixed system position was good. There was no looseness or breakage. 3 months, 6 months and 12 months later, the grade of Frankel spinal cord injury was significantly better than before (P=0.022) (Table 1). The VAS score was (3.05±0.65), (1.88±0.55) and (0.31±0.22). Compared with the score that preoperative (6.67±1.85). It reduced statistically. The comparison results were statistically significant (P=0.012). The ODI dysfunction index was (21.15±5.35), (12.26±4.55) and (5.31±3.12), and compared with the preoperative period (37.87±4.85). The comparison results were statistically significant (P=0.031) (Table 2) (Figure 1 and 2).
Time
B
C
D
E
Preoperative
0
16
45
2
3 months
0
5
25
32
6 months
0
4
16
42
Last follow-up
0
0
11
51
Table 1: Frankel spinal cord injury grading scale (n=62) before and after operation.
Time
VAS
ODI
Preoperative
6.67±1.85
37.87±4.85
3 months
3.05±0.65
21.15±5.35
6 months
1.88±0.55
12.26±4.55
12 months
0.31±0.22
5.31±3.12
F
2.24
2.56
P
0.012
0.031
Table 2: VAS score and ODI index (n=62) before and after operation.
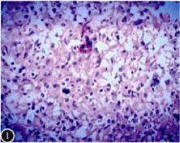
Figure 1: Histopathological examination of the lesion showed cell proliferation,
proliferative nodules and granulomatous formation, with intracellular
mononuclear cells, lymphocytes, neutrophils, eosinophilic infiltrates, and a
nodular lesion composed of epithelial cells (HE staining, x 200).
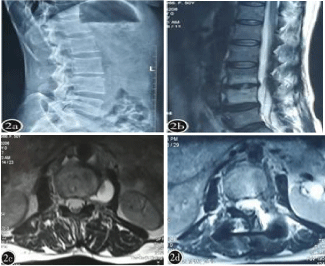
Figure 2: 50-year-old female patient. Main complaint: Low back pain and
limited waist activity, low heat for 2 months.
2a: Preoperative X-ray examination indicated: L3/4 vertebral space was
damaged and narrow.
2b: Preoperative MRI examination sagittal image indicated: L3,
L4 vertebral body and L3/4 intervertebral disc were damaged, and the
intervertebral space had abscess. The abscess was oppressive to the cauda
equina.
2c: Preoperative MRI axial image show: L3/4 damaged intervertebral disc
and paraspinal abscess cause nerve root canal stenosis, and narrow nerve
root canal compression of nerve roots.
2d: Postoperative MRI axial image show: L3/4 parabasal abscess had
been removed, and the nerve root canal had been decompressed thoroughly.
Discussion
Indications of lumbar BS surgery
Lumbar BS was a secondary infection of the spine of the lumbar vertebrae, which had been caused by a pathogen invasion of the lumbar vertebrae [5]. Reported that the incidence of lumbar vertebrae was 68%. The primary treatment for lumbar BS was still based on oral therapy. Most of the patients, after conservative treatment, could get effective treatment effect [4,5,11]. However, it was often because of the patient’s localized symptoms that could not be lifted or relieved, surgical treatment was necessary. For example: The infection causes growth of granulomatous tissue or an abscess to invade a spinal canal. It was a neurological condition for cauda nerve, nerve root, or spinal cord, which leads to neurological symptoms; there was a large unabsorbable lesion around the vertebral body; there was a continuous stimulation to the surrounding normal tissue; the stability of the spine was affected. Surgical treatment was a necessary treatment for lumbar BS when it developed to a certain stage [12,13]. Yang Xining et al [14], which classified into one or more of the following situations, the surgical treatment was necessary:
1. A large abscess or psoas abscess which could not be absorbed;
2. A spinal abscess or an inflammatory granuloma;
3. The intractable pain caused by the destruction of the disc;
4. The lesion of the vertebral body or the zygapophyseal joint affects the stability of the spine;
5. Indus, nerve roots, or spinal cord compression;
6. A mixed infection with other bacteria. With the improvement of the people’s living standards, patients had higher standards of quality of life when the surgical treatment was done.
Surgical operation as an significant treatment method that could quickly and accurately remove the lesions, relieve the clinical symptoms, restore the stability of the lumbar spine, and satisfy the treatment desire of the patients with lumbar spine, which was an ideal treatment choice.
Surgical approach selection of lumbar BS
For the surgical treatment of lumbar BS, our concept was: Removed the lesion completely; removed the decompressions which existed in spinal canal; orthodontic spine correction; intertransverse bone grafting, and strong internal fixation system. The idea was not only to restore the biomechanical stability of the spine, but also to eradicate the lesion. This was a better recovery for the spinal function. The traditional surgical approach for lumbar spine involves: Forward entry, front and back roads, and rear route.
The above two kinds of surgical methods that including the anterior approach: The lesion was cleared thoroughly. We could have a direct vision during operation time. But, disadvantages were equally obvious. The anterior approach was performed with an oblique incision on one or both sides of the abdomen. Surgical approach should pass the external oblique machine, internal oblique muscle, the transverse abdominal muscle and psoas major. The operating area, which was in the back of the peritoneum, affected the inferior arterial artery, the vein and the vagus in front of the spine. It required very high surgical techniques. At the same time, there was a possibility of a larger injury. The spinal fixation of anterior approach had limitations on the recovery of lumbar stability, especially for patients with kyphosis, and the effect of correction and postoperative prevention of deformity was not ideal [15]. The combined operation of the anterior and posterior approaches had the following problems: The anterior surgical injury was large, the surgical fixation was much longer, the patient lumbar activity was limited after the operation, and the degeneration of the adjacent vertebral body was accelerated [16].
In comparison, the posterior approach was more suitable for the disease. The posterior surgery only removed the spinal muscle and the part of the vertebral body. It was more accurate, less invasive, less affected to normal tissue. At the same time, the structure and stability of the spinal posterior column could be instead of by a nail stick system, the forward was guaranteed by bone graft fusion.
The advantages of posterior lesion removal, intervertebral bone grafting, and nail stick system fixation
The advantages of posterior approach were shown in the following aspects: 1) It was better to restore the stability of the lumbar spine. Through the fixation of the nail rod system, the spine reposition and orthopedics were performed well, the physiological curvature of the spine was restored, and the possibility of kyphosis was reduced. After the decompression of vertebral plate and the enlargement of the nerve root canal, the stability of the posterior column of the spine was provided, and the stability of the three columns was guaranteed. 2) Post-operative, the injury of tissue was small, the operation difficulty was low, and the injury of important tissue was not easy to occur. The physiological structure of the lumbar spine determined that during the surgical procedure, a moderate caudal nerve or root pull of the nerve root would not result in significant postoperative neurologic symptoms or neurological root pain symptoms. And the safety of this operation was also confirmed by Fei qi [17]. 3) The removal of the abscess and proliferating tissues next to or in front of the spinal column. With use of the spoon which had various sizes and multiple angles and other advanced spinal surgical instruments, the posterior approach could have the surgical results just like anterior approach. If necessary, remove a small amount of vertebral transverse process to expand the surgical field, which could help remove the focus thoroughly. This was a feasible scheme.
Conclusion
For patients, who had lumbar BS, combine oral therapy and surgical treatment, which could remove the diseased tissue or abscess completely. The operation could fully decompress the spinal canal and nerve root canal. At the same time, the fixation of the rod system could guarantee an immediate stability of the lumbar spine. To restore and maintain the normal physiological curvature of the lumbar spine, prevent postoperative lumbar spine deformity or other lumbar instability. In a word, the surgical treatment, that used posterior approach to remove the lesion, graft the bone between transverse process and used nail rod system to make internal fixation, was an effective method for lumbar spine BS.
References
- Lim KB, Kwak YG, Kim DY. Back pain secondary to Brucella spondylitis in the lumbar region. Ann Rehabil Med. 2012; 36: 282-286.
- Ulu-Kilic A, Karakas A, Erdem H, Gulsun S, Elald N, Alabay S, et al. Update on treatment options for spinal brucellosis. Clin Microbiol Infect. 2014; 20: 75-82.
- Bagheri AB, Ahmadi K, Chokan NM, Abbasi B, Akhavan R, Bolvardi E, et al. The diagnostic value of MRI in Brucella spondylitis with comparison to clinical and laboratory findings. Acta Inform Med. 2016; 24: 107-110.
- Smailnejad Gangi SM, Hasanjani Roushan MR, Janmohammadi N. Outcomes of treatment in 50 cases with spinal brucellosis in Babol. Northern Iran. Infect Dev Ctries. 2012; 6: 654-659.
- Turgut M, Turgut AT, Koşar U. Spinalbrucellosis: Turkish experience based on 452 cases published during the last century. Acta Neurochir. 2006; 148: 1033-1044.
- Passias PG, Ma Y, Chiu YL, et al. Comparative safety of simultaneous and anterior and posterior spinal surgery. Spinal. 2012; 37: 247-255.
- Selim Sözen, Cemal Üstün, Hasan Baki Altinsoy. Paosa abscess secondary to Brucellosis. Med J Bakirköy. 2011; 7: 79-81.
- Mousa AM, Bahar RH, Araj GF, Koshy TS, Muhtaseb SA, al-Mudallal DS, et al. Neurological complications of Brucella spondylitis. Acta Neurol Scand. 1990; 81: 16-23.
- Katonis P, Tzermiadianos M, Gikas A. Surgical treatment of spinal brucellosis. Clin Orthop Relat Res. 2006; 444: 66-72.
- Xinming YANG, Xianyong MENG, Changbo HU, et al. Diagnostic and surgical treatment of Brucella spondylitis. 2016; 9: 308-316.
- Yang Xinming, Wei Shi, Wangle Yaoyi. Imaging Classfication and Clinical Significance of Brucellosis Spondylitis. Spine. 2014; 3: 172-177.
- Ioannou S, Karadima D, Pneumaticos S, Athanasiou H, Pontikis J, Zormpala A, et al. Efficacy of prolonged antimicrobial chemotherapy for brucellar spondylodiscitis. Clin Microbiol Infect. 2011; 17: 756-762.
- Mailtan Maimaiti, TIAN Juan, SHENG Weibin, et al. Diagnosis and surgical treatment of the Brucellar spondylitis. Chinese Journal of Orthopaedics. 2012; 32: 323-330.
- YANG Xinming, MENG Xianyong, ZHANGYing, et al. Treatment of the brucellar spondylitis in the thoracic and lumbar vertebrae by surgery. Chinese Journal of Spine and Spinal Cord. 2012; 22: 600-606.
- Jain AK, Dhammi IK, Jain S, et al. Simultaneously anterior decompression and posterior instrumentation by extra pleural retroperitoneal approach in thoracolumbar lesions. Indian J Orthop. 2010; 44: 409-416.
- ZHANG Guojun, YAN Guofei, LAO Eli, et al. A combined surgical treatment of lumbar brucellar spondylitis with anterior and posterior approach. Hebei Medicine. 2013; 19: 585-587.
- FEI Qi, YANG Yong, Jin jun LI, et al. A case of incomplete paraplegia of brucellar spondylitis and a review of the literature. Chinese Journal for Clinicians. 2014; 42: 48-50.