
Review Article
Austin Phys Med. 2019; 2(1): 1005.
Rehabilitation of Knee Arthroplasty
Khalfaoui S* and Abbassi EI M
¹Department of Physical Medicine and Rehabilitation of the Military Instruction Hospital Mohammed, Morocco
*Corresponding author: Khalfaoui S, Department of Physical Medicine and Rehabilitation of the Military Instruction Hospital Mohammed Assistant professor, V Rabat, Morocco
Received: April 23, 2019; Accepted: May 15, 2019; Published: May 22, 2019
Abstract
The knee arthroplasty is a surgical indication set in an analgesic and functional aim. Its success depend on a global reeducational support before and after surgery in which the patient plays a signification role in order to improve quality of life respecting the advises and instructions.
Keywords: Knee arthroplasty; Rehabilitation; Monitoring
Introduction
Osteoarthritis is a degenerative pathology inflammatory, due to the wear of cartilage present at the surfaces of sliding. Gradually, the different components of the knee joint irreversibly degrade causing painful stiffness and a reduction of the walking distance. The goal of total knee arthroplasty is to remove the pain, recover the joint mobility and resume activities of daily life in particular walking, transfers and stairs.
Rehabilitation after arthroplasty knee adapts to each patient according to his health status, background, abilities functional and especially its previous state before fitting the prosthesis. Its duration with the physiotherapist lasts a few weeks relayed by self-education that the patient must continue for up to 12 months Postoperative.
A study conducted by Eschalier has shown that the delivery of an information booklet concerning the overall care of knee osteoarthritis has no effect on improving knowledge and beliefs of the patient candidate to a total knee prosthesis [1]. In addition, the rehabilitation treatment preoperative encompassing physiotherapy and education has demonstrated its effectiveness in gonarthrosis [2]. The duration of hospitalization in the service of surgery was reduced by the improvement techniques of implantation of PTG, Medical control conditions and perioperative paramedical and economic imperatives.
In 1987, the transition to a center specialized rehabilitation after completion a PTG remained mandatory for Darnault et al. In order to improve the patient’s autonomy before returning to home [3]. In 1999, this choice was justified by the difficulties encountered in rehabilitation specialized as well as the need for a close medical supervision until the 18th postoperative day [4]. In 1992, it was demonstrated by a study by the Belgians, that the care early return allowed home two to three weeks [5]. The functional prognosis of arthroplasty total knee would depend on the quality of early rehabilitative management in surgery [6-8]. In the literature, we often report the interest and the positive effect of rehabilitation pre, peri and post-operative on the function and the quality of life [9].
In operated patients, able to return at home directly, the prescription of systematic physiotherapy is not recommended. However, it could facilitate trophic recovery and strength muscle as well as recovery functional.
It is therefore beneficial for these patients to prescribe a series of session physiotherapy for the purpose of improvement functional, according to the professionals of surgery and physical medicine and Rehabilitation.
Preoperative rehabilitation aims to alleviate pain, improve walking by increasing the walking distance, facilitate joint mobility of the knee, and to prepare for the surgical procedure.
The results obtained after an implantation of PTG are different despite a well-conducted surgical technique, good prosthetic implants and existence complications.
The functional result depends largely part of the anterior mobility of the knee, pre-operative muscle strength, the existence of risk factor without forget the voluntary mentality or not patient candidate for this surgery.
The decrease in muscle strength is a considerable factor because it is present from concrete way given the decline in activity physical caused by osteoarthritis; and the surgical procedure aggravates even more this loss of strength and voluntary contraction; hence the importance of emphasizing Analytical muscle and global preoperative by simple exercises, easy to achieve at home.
It is thus advisable to learn some exercises to be repeated at home twice day to walk type 20 minutes without pain, aerobics exercises, bike 10 minutes, muscle stretching, etc. [10-12].
After completion of the PTG implant, the purpose of surveillance is to detect post-operative complications and evaluate functional and clinical results.
She can be divided into 3 steps [13]:
1. During hospitalization in surgery
2. During rehabilitation functional
3. Long term.
During hospitalization in the orthopedic surgery service
The surgeon checks the presence of a mechanical compression as soon as you wake up patient, eliminates the sciatic nerve external poplitia by checking the sensitivity and motor skills, palpate peripheral pulses distal, without forgetting the loco-regional state of the knee as well as the general signs.
The Redon drain is removed to the second day if more flow, and the dressings are redone with supervision skin condition in search of a cicatricial disunion, dry necrosis or wet or possible infection.
Thromboembolic complications are clinically screened and prevented by anti-coagulant treatment covering four weeks postoperatively. The rehabilitation is started gradually, and in the case of a mobility deficit, an early mobilization under anesthesia general could be proposed.
Pain is a surveillance factor, which could disrupt the course of the functional rehabilitation protocol.
It must be taken care of early and preferably the day before anesthesia, as well as throughout the convalescence.
During functional rehabilitation [14]
It takes place classically in the reeducation center. Removal of staples or threads is made from J12 post-operative according to the cutaneous state and the scar (Figure 1). Cutaneous disorders gradually regress with the application of icing for ten minutes 5 to 6 times a day covering the skin by a towel to avoid the burn. The goal of rehabilitation is to get a knee, stable and painless.
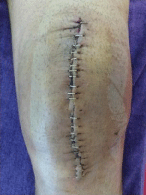
Figure 1: Staples in place.
Control with the surgeon is considered between the sixth and eighth week post-operative to ensure the absence of complications, evaluate the pain by the visual analog scale, measure the functional area of the knee and appreciate the quality of recovery of walking autonomous.
Long-term
One-year consultations, then all two to three years are planned, in order to establish a simple and reproducible score to compare the results so objective. Standard radiographs are also regularly requested looking for a misalignment, a wear of the polyethylene, positioning of implants and patella.
Life hygiene tips are renewed on the activities physical health and the prevention of septic complications likely to occur in case of local, locoregional infection or remotely.
Radio-clinical surveillance all three at five years after knee replacement surgery is considered of great importance allowing to:
1. Screen for subclinical complications objectified only at the radiography.
2. Monitor and evaluate the wear rate of the implant especially in the young operated.
3. Make the patient aware of different stages of the functional recovery [15]
Professional transmissions [16]
Before starting the protocol reeducation, the reeducator must have, in addition to the usual information at all rehabilitation treatment, an account operative rendering specifying:
• The reason for implantation.
• The date of the operative act.
• The type of prosthesis and its characteristics, basically if the patient has undergone a gesture on cruciate ligaments, if the patella has been retained or not, the amplitudes conceivable, the associated gestures, occurrence of a postoperative event immediate and counter indications and instructions to respect (support, mobilization articular ...) as well as preoperative data concerning pain, perimeter of walking and degree autonomy of the stairs.
Rehabilitation program [16]
Generally, re-education following an arthroplasty adapts to the global context of patient and his antecedents. After balance performed by the re educator, the program reeducation is established and divided into three steps:
The preoperative phase: about ten physiotherapy sessions is recommended, initiating a first contact of trust between the patient and physiotherapist, whose goal is:
1. Optimize the amplitudes articular
2. Strengthen all muscles stabilizers of the lower limb
3. Educate the patient to transfers, exercises, walking and activities superior walking aids techniques
4. Work breathing
5. Give an idea about the postoperative stage.
The acute phase: Preferably, before drain removal aimed essentially at:
1. Lower the pain threshold
2. Fight against cutanotropic disorders (Figure 2).
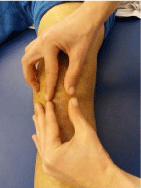
Figure 2: Work of the scar.
3. Mobilize the knee
4. Actively lock the knee discharge (Figure 3).
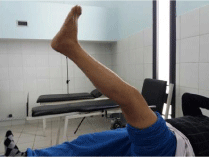
Figure 3: Active locking in discharge.
5. Reassure the patient on the plan functional.
Secondary phase: In addition to the objectives of the acute phase:
1. Control the pain
2. Tracking complications
3. Improve the gain of the amplitudes articular
4. Actively lock the knee charge
5. Work on balance and proprioception.
Rehabilitation techniques [16]
1. Massage: indicated to facilitate the contact with the patient, performed for circulatory purposes, decontracturing, and analgesic and preparatory to muscular work and proprioceptive (Figure 2).
2. Cryotherapy: isolated or compressive to fight inflammation, effusion intra-articular and especially the pain.
3. Antalgic electrostimulation: can to be associated for an analgesic purpose postoperatively.
4. Excito-motor electrostimulation: In association with techniques, manual muscular awakening to promote the lifting of amazement muscle and recovery of the Muscular force (Figures 4-7).
We use an electrical signal, symmetrical at zero average with:
• A frequency of 8 to 20 Hz for stimulate the fibers I and 20 to 40 Hz for fibers II and III
• A pulse duration between 200 and 400μs
• A stimulation duration of 20 to 30 minutes
• A rest period of 40 to 60 minutes.
1. Manual passive mobilization: essential technique by remaining in infra pain with the realization postures in extension and in bending (Figures 4,5).
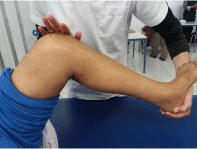
Figure 4: Manual passive mobilization.
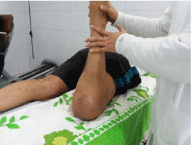
Figure 5: Manual posture in flexion.
2. Continuous passive mobilization by arthromotor: installed early post-operative by respecting the hygienic conditions and the healing procedure, always associated with passive mobilization manual, hence obtaining a progressive flexion according to the patient tolerance and instructions of the surgeon (Figure 8).
3. Auto-passive mobilization: completing the use of the arthromotor (Figure 9).
4. Active mobilization: in all its forms forms: free, helped and resisted. He this is a reinforcement progressive muscular, analytical and overall of all the muscles of the inferior member (Figures 6,7 and 10).
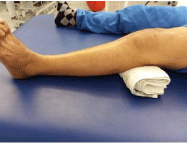
Figure 6: Isometric strengthening of the quadriceps on cushion or balloon.
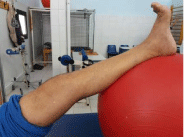
Figure 7: Isometric strengthening of the quadriceps on cushion or balloon.
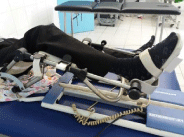
Figure 8: Continuous passive mobilization.
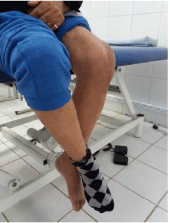
Figure 9: Self-posture in flexion.
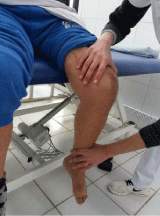
Figure 10: Reinforcement by contracted released.
5. Myo-feedback: useful for improve the control of the muscle contraction.
6. Reprogramming sensitivomotor or proprioceptive: started early in landfill then in charge, bipodal then
7. Unipodal, on stable ground then accident with and without help techniques, with stimulations applied at the scapular level, pelvic and at the knees (Figures 11-14).
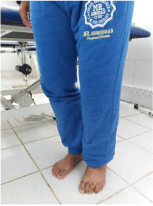
Figure 11: Bipodal support.
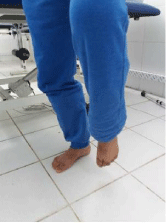
Figure 1: Unipodal support.
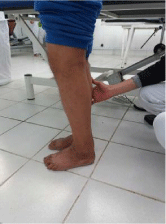
Figure 13: Work of balance.
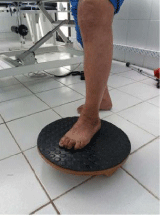
Figure 14: Proprioception work.
8. Functional work: ambulation, transfer and balance (Figures 15,16).
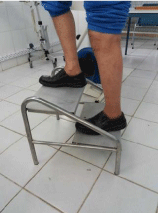
Figure 15: Climbing stairs.
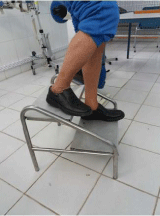
Figure 16: Descent of the stairs.
9. Balneotherapy: where the mobilization passive, active, strengthening muscular, proprioception and are carried out in immersion.
Two tests simple, easy to perform, can evaluate the functional abilities of the patient enjoying muscle strength and allowing the doctor dealing with detecting a possible deficiency justifying an extension of the rehabilitation treatment.
• Timed up and go test: get up from a chair, walk three meters then come back to sit down.
• Chair rise test: to stand up and sit on a chair five times hands crossed.
• 10. Therapeutic education of patient:
• Make the patient aware of the need to prevent avoidable complications,
• Learn and know the gestures prohibited and restrictions functional
• Respect the instructions of the surgeon, o Consider changing his lifestyle (walking, stairs, heavy load port, high heels, prolonged standing ...) o Involve his entourage in the management and postoperative management.
Follow-up criteria: [16]
1. Structural: pain, mobility, muscle strength, edema.
2. Functional:
• Walk: walking distance, walking speed, quality and walk diagram.
• Bipodal and unipodal balance
• Superior walking activities: transfer and stairs.
• Quality of life: use validated scale allows objectifying indicators functional and quality of life patient.
Conclusion
The total knee replacement prosthesis goal of relieving the patient on the plane pain and improve its mobility and its transfers. Pre and postoperative rehabilitation is an integral part of taking in charge of this arthroplasty, to optimize the results hoped. The patient should, in turn, participate in the favorable evolution of its quality of life by respecting the advice and applying the instructions prescribed by its various stakeholders.
References
- Eschalier B, Descamps S, Pereira B, Girard MG, Boisgard S, Coudeyre E. Evaluation of a preoperative therapeutic education approach before total knee arthroplasty. Journal of Epidemiology and Public Health. 2012; 558: 117-125.
- Coudeyre E, Jardin C, Givron P, Ribinik P, Revel M, Rannou F. Could preoperative rehabilitation modify postoperative outcomes after total hip and knee arthroplasty? Elaboration of French clinical practice guidelines. Ann Readapt Med Phys. 2007; 50: 189-97.
- Darnault A. Rehabilitation of the total knee prosthesis. Cah kinesither. 1987; 126: 40-53.
- Darnault AHJ, Breton G, Daniel F, Griffon A. Rehabilitation after total knee arthroplasty and its difficulties. Rheumatology. 1999; 51: 5-6.
- De Nayer FPE. Total knee arthroplasty. Ann Kinesither. 1992; 19: 205-208.
- Cheyron C. About the management of physiotherapy of 102 total knee prostheses at the Croix-Saint-Simon hospital. KS. 2003; 432: 5-12.
- Fritsch CZY, Leyvraz PF. Rehabilitation after total knee prosthesis retaining the posterior cruciate ligament. Rheumatology. 1994; 46: 71-75.
- Kumar P, Mc Pherson E, Dorr L, Wan Z, Baldwin K. Rehabilitation after total knee arthroplasty: a comparaison of 2 rehabilitation techniques. Clin Orthop Relat Res. 1996; 331: 93-101.
- Genet F, Mascard E, Coudeyre E, Revel M, Rannou F. Interest of an outpatient physiotherapy prescription at the exit of the surgery department after the installation of a total knee prosthesis? Elaborations of French recommendations for clinical practice. Annals of Rehabilitation and Physical Medicine. 2007; 50: 783-792.
- Bonnim M, Laurent JR, Paratte S, Zadegan F. What can be done after PTG, osteotomy and PUC? 83rd SOFCOT congress. 2007.
- Cazenave A, Cartier P. Unicompartmental prosthesis marmor evolution genesis-In “first-line knee arthroplasty: clinical experience”. Ed SAURAMPS Medical. 2008; 155-162.
- Duffy GP, Crowder AR, Trousdale RR. Cemented total knee arthroplasty for patients 55 years old or younger. J Arthroplasty. 1997; 12: 49.
- Gedda M, Gouilly P. Criteria for follow-up in rehabilitation and orientation in outpatient or follow-up care or rehabilitation after total knee arthroplasty. Chinese Siter Rev. 2009; 89: 21-23.
- Husted H, Hansen HC, Holm G, Bach-Dal C, Rud K, Andersen KL. What determine length of stay after total hip and knee arthroplasty? A national wide study in Denmark. Arch Orthop Trauma Surg. 2010; 130: 263-268.
- Ong PH, Pua YH. A prediction model for length of stay after total and unicompartimental knee replacement. J Bone Joint J. 2013; 70: 88-96.
- HAS: Professional recommendations. Criteria for follow-up in rehabilitation and orientation in ambulatory or SSR after total knee arthroplasty. January 2008.