Abstract
Background: Since December 2019, an outbreak of corona virus disease 2019(COVID-19), caused by the Severe Acute Respiratory Syndrome Corona Virus-2 (SARS-CoV-2) has widely and rapidly spread in China and around the world. Since 31 December 2019 and as of 30 April 2020, more than 25,000,000 cases of COVID-19 and 800,000 deaths have been reported. The grim epidemic has caused increasing public panic and mental health stress. Mental health is becoming an issue that cannot be ignored, while trying to control the outbreak. Cross sectional study was conducted to assess magnitude and factors associated depression among patients with COVID-19 in St. Peter Specialized Hospital Treatment Centers Addis Ababa, Ethiopia.
Methods: Institutional based cross-sectional study was conducted among 422 Patients with COVID-19 admitted at St. Peter Specialized Hospital COVID-19 treatment center. The Anxiety and Depression was assessed through face to face interviews by trained psychiatry nurses using 14-items Hospital Anxiety and Depression Scale (HADS).Correlates for depression & anxiety were assessed using a structured questionnaire and Oslo social support scale.
Result: A total of 373 participants were volunteer to be included in the study which makes the response rate88.4%. The mean age of the respondents was 37.46 (±SD=16.09) years. This study revealed that the Magnitude of Depression 36.5 % (136) and Anxiety 21.2 % (79) among COVID-19 patients. By using Multivariate (Anxiety) Logistic Regression, Patients who were Male (AOR 5.01, 95%CI (2.11, 11.87)), Housewife (AOR 11.43, 95%CI ( 2.67, 48.90)), Selfemployed (AOR 2.45,, 95%CI (1.07, 5.60)), having Diagnosed Chronic illness (AOR 2.56, 95%CI (1.19, 5.53)), having COVID-19 Symptoms for below 7 days and for 8-14 days ((AOR 3.21, 95%CI (1.21, 8.58)) & AOR 3.70, 95%CI (1.55, 8.84)) respectively) and those who had Poor/low Social Support (AOR 3.42, 95%CI (1.21, 9.63)) had Statistically Significant Association with Anxiety.
By using Multivariate (Depression) Logistic Regression, Patients who were 41 and above years of old (AOR 3.95, 95% CI (1.80, 8.69)), had Monthly Income of less than 1000 birr (AOR 2.99, 95%CI (1.11, 8.05)), Having COVID-19 Symptoms for 8-14 days (AOR 2.63, 95% CI (1.34, 5.17)) and who had Poor Social Support (AOR 3.13, 95% CI (1.34, 7.30)) were Statistically Significant Associated with Depression.
Conclusion: In the current study area the magnitude of depression and anxiety was high. Factors like sex, Job, having Diagnosed Chronic illness, Duration of COVID-19 symptom and social support with anxiety and factors such as age, income, duration of COVID-19 symptom and social support had statistically significant associated with depression.
Abbreviations
SPSS: Statistical Package for Social Science; WHO: World Health Organization; HADS-Hospital Anxiety and Depression Scale; NAT: Nucleic Acid Testing; COVID: Corona Virus Infectious Diseases; CT: Computed Tomography; COPD: Chronic Obstructive Pulmonary Disease; PSSS: Perceived Social Support Scale; SDS: Self Rating Depression Scale; SAS: Self Rating Anxiety Scale; GAD-7: Generalized Anxiety Disorder-7; PSQI: Pittsburgh Sleep Quality Index
Introduction
Background
The novel coronavirus (COVID-19) is a new infectious disease that is mainly transmitted by respiratory droplets and contact and is generally infectious to human beings [1]. On January 11, 2020, after pathogenic Nucleic Acid Testing (NAT), China reported 41 cases of pneumonia infected with the novel coronavirus (SARS-CoV-2) [2], for the first time in the world of human infection with the novel coronavirus. On January 30, 2020, the World Health Organization listed the novel coronavirus epidemic as a Public Health Emergency of International Concern (PHEIC) [3]. As of February 20, 2020, a total of 75, 465 confirmed cases and 2, 236 deaths have been reported in mainland China [4].WHO stated that there is a high risk of COVID-19 spreading to other countries around the world [5]. Now it becomes a major pandemic, once after it was detected in Wuhan, China, to clusters of cases in many countries of the world [6].
The symptoms of COVID-19 are non-specific, ranging from asymptomatic to severe pneumonia and death. Fever and cough are the most common clinical symptoms. Abnormal chest Computed Tomography (CT) has been used to diagnose 67.4-88.0 % cases of COVID-19, indicating that pneumonia is the most common manifestation of the disease [7-9]. The disease is rapidly spreading in areas with high population densities, including urban areas, camps and camp-like settings, and often overburdening weak health systems. It is now clear that the virus does not differentiate between setting and season. Without decisive action, massive outbreaks will happen around the world, because many countries have insufficient resources to augment health-care staff, and do not have enough space or the necessary supplies to treat the sick [6].
Mortality is higher in patients with hypertension, cardiac disease, diabetes mellitus, cancer, and COPD as well as elderly patients are more susceptible to severe disease and death, while children seem to have lower rates of infection and lower mortality. The approach to diagnosis is still very variable from region to region, country-tocountry, and even among different hospitals in the same city. The importance of a clinical pathway to implement the most effective and relevant diagnostic strategy is of critical importance to establish the control of this virus that is responsible for more and more deaths each day [10].
Currently, global statistics shows above 12 million people affected by covid-19 and In Ethiopia, more than 12,300 people are affected by covid-19, during the study period.
Statement of the problem
The evidences highlighted that depression and stress are interrelated to each other and the overlapping symptoms of these psychological problems can lead to a wide range of clinical and personal problems which negatively impact on the quality people’s overall life. Depression is an individual experience and a complex phenomenon as the feeling of despair is dominant [11]. Even if, the physicians of Filipinos chose adaptive coping in response to the COVID-19 outbreak there is low Psychiatric morbidity, which ranges 17.7% to 18.8% on the General Health Questionnaire (GHQ 28) [12]. Further, the survey that was conducted during the initial outbreak of COVID-19in China, reported 53.8% of respondents rated the psychological impact of the outbreak as moderate or severe; 16.5% as moderate to severe depressive symptoms; 28.8% as moderate to severe anxiety symptoms, and 8.1% reported moderate to severe stress levels [13]. The psychological fear is perhaps more intensified now compared to previous viral respiratory outbreaks, with increased air travel and enhanced global connectedness that make the spread of a pandemic much more effortless. Extensive media coverage of the epidemic can now influence the public’s psychological response to the infectious disease threat [14,15].
In addition, the systematic review mentioned that pooled prevalence anxiety, depression, acute stress disorder, burnout and post-traumatic stress disorder was 45%, 38%, 31%, 29%, and 19% respectively. Factorssuch as sociodemographic like younger age and female gender; social like lack of social support, social rejection or isolation, stigmatization; and occupational like working in a high risk environment (frontline staff), specific occupational roles ( nurse), and lower levels of specialized training, preparedness and job experience have an association with the likelihood of developing those problems [16,17].
Further, being a student, had specific physical symptoms and poor self-rated health status have significantly associated with a greater psychological impact of the outbreak and higher levels of stress, anxiety, and depression. Whereas, receiving specific up-to-date and accurate health information about treatment, local outbreak situation and taking particular precautionary measures (e.g., hand hygiene, wearing a mask) associated with a lower psychological impact of the outbreak and lower levelthese psychological problems [17].
Therefore, designing psychological interventions to improve mental health of the society during epidemics is essential. Raising people’s awareness about the measures taken by the government to counter the spread of rumors, applying optional to mandatory restrictions, and raising public awareness by providing information on the patients’ recovery process can reduce these psychological problems in society [18].
Deploying a mental health science perspective’ to the pandemic will also inform population-level behavior change initiatives aimed at reducing the spread of the virus. Ethiopia, being one of the developing countries trying to address the diverse needs of its people, is currently at the verge of the epidemic. The government is currently showing high commitment to contain the epidemic before it causes significant damage to the community by taking the actions like case identification, contact tracing, isolation and quarantine. To mitigate the spread of the disease, also it uses to the preventive measures like promoting social distancing and sanitary measures [19].
However, to our knowledge, most of the current studies related to this outbreak mainly focus on identifying the clinical or epidemiological characteristics of the infected cases, there is no relevant research examining the mental health burden on the COVID-19 on the general public in Ethiopia. So, in the present study, we aimed to explore the Prevalence and factors linked to Anxiety and Depression in Hospitalized patients with COVID-19. This study may draw more attention to the psychological state of patients with COVID-19, and assist health workers to provide more appropriate treatment and psychological interventions to improve mental and physical health of patients.
Literature reviews
Prevalence and associated factors of depression and anxiety: The cross-sectional study which was done among 144 patients with confirmed COVID19 who were Huoshenshan Hospital of Wuhan, China during the COVID-19 epidemic to explore the prevalence and factors linked to anxiety and depression by using the Hospital Anxiety and Depression Scale (HADS), and social support using the Perceived Social Support Scale (PSSS) reported that 34.72% and 28.47% patients with COVID-19 had symptoms of anxiety or depression, respectively. Further, those who had less social support were correlated with more anxious and depressive symptoms. Specifically factors like gender (β=1.446, p=0.034), older age (β=0.074, p=0.003), having less oxygen saturation (β=-2.140, p=0.049), and social support (β =-1.545, p=0.017) were associated with anxiety and age (β=0.084, p=0.001), family infection with SARS-CoV-2 (β=1.515, p=0.027) and social support (β=-2.236, p<0.001) were the factors associated with depression [20].
The study was done in the Second Affiliated Hospital of Harbin Medical University, by single-center cross-sectional study focused on measuring depression and anxiety using self-report scales. Linear regression was used to determine independent predictors for depression and anxiety. A total of 78 patients who were confirmed to have COVID-19 were enrolled in the study. Prevalence of depression and anxiety symptoms were diagnosed in 35.9% and 38.5% of the patients, respectively.
Multivariate linear regression analysis found female gender was an independent predictor for higher depression severity index. Having family members who were diagnose with COVID-19 and family members who died from COVID-19 were independently associated with higher depression severity index and anxiety score. Depression was assessed using the Zung Self-rating Depression Scale (SDS), consists of 20 items that measure symptoms of depression and Anxiety was assessed using the Zung Self-rating Anxiety Scale (SAS), is a 20-item self-report scale [4].
A cross-sectional study was conducted in southeastern China, including Sichuan Province, Chongqing City, Guizhou Province, and Yunnan Province, Data were collected using the Self-rating Anxiety Scale (SAS) and the self-rating depression scale (SDS) administered to 1593 respondents aged 18 years and above. The respondents were grouped as ‘affected group’ and ‘unaffected group’ on the basis of whether they or their families/colleagues/classmates/neighbors had been quarantined. So that, the prevalence of anxiety and depression was approximately 8.3% and 14.6%, respectively, and the prevalence in the affected group (12.9%, 22.4%) was significantly higher than that in the un-affected group (6.7%, 11.9%). Lower average household income, lower education level, having a higher self-evaluated level of knowledge, being more worried about being infected, having no psychological support, greater property damage, and lower selfperceived health condition were significant associated with higher scores on the SAS and SDS. People living in Chongqing had higher SAS and SDS scores than those living in Yunnan Province. Study was conducted from 4 Feb to 10 Feb 2020 [5].
The study was short review on the psychological effects of COVID-19 and its association with anxiety by using the electronic databases, including PubMed, Medline, Elsevier, and Science Direct as a source of data mentioned that 1210 participants from 194 cities in China answered an online questionnaire and 53.8% of these people experienced severe psychological impacts of the outbreak. Moreover, 16.5%, 28.8%, and 8.1% of the respondents reported moderate to severe levels of depression, anxiety, and stress, respectively [18].
A cross-sectional study which was conducted among 4872 Chinese citizens aged 18 years old to assess the prevalence of mental health problems and examine their association with social media exposure by using online survey was used to do rapid assessment, depression was assessed by the Chinese version of WHO-Five Well- Being Index (WHO-5) and anxiety was assessed by Chinese version of Generalized Anxiety Disorder scale (GAD-7)and finally described that the prevalence of depression, anxiety and Combination of Depression and Anxiety (CDA) was 48.3% (95% CI: 46.9-49.7 %), 22.6% (95% CI: 21.4-23.8 %) and 19.4% (95% CI: 18.3-20.6 %) respectively during COVID-19 outbreak in Wuhan, China. In addition more than 80% (95% CI: 80.9-83.1 %) of participants reported frequently exposed to Social Media (SME) and the frequently SME was positively associated with high odds of anxiety (OR=1.72, 95% CI: 1.31-2.26) and CDA (OR=1.91, 95% CI: 1.52-2.41) compared with less SME. Further, there are high prevalence of mental health problems, which positively associated with frequently SME during the COVID-19 outbreak [21].
A web-based cross-sectional survey was implemented to assess the population mental health burden during the epidemic, and to explore the potential influence factors, among 7, 236 & 24 self-selected volunteers to collect information about demographic information, COVID-19 related 25 knowledge, Generalized Anxiety Disorder-7 (GAD-7), Center for Epidemiology Scale 26 for Depression (CES-D), and Pittsburgh Sleep Quality Index (PSQI) reported that the overall prevalence of GAD, depressive 30 symptoms, and sleep quality were 35.1%, 20.1%, and 18.2%, respectively. Determinates such as young 31 years of aged peoples reported a higher prevalence of GAD and depressive symptoms than older 32 people (P<35 years) and times to focus on the COVID-19 (≥3 hours per day) 35 were associated with GAD, and healthcare workers were associated with poor sleep 36 quality. Generally, participants of young people, people who spent too much time on the 39 epidemic, and healthcare workers were at high risk for mental illness [22].
A review of the existing literature was conducted by using a search of the PubMed electronic database a total of 47 citations were retrieved to see the relation between COVID-19 and mental health summarized that symptoms of anxiety and depression was 16-28 % and self-reported stress was 8% that are common psychological reactions to the COVID-19 pandemic, and may be associated with disturbed sleep [23].
A web-based cross-sectional survey based on the Internet Survey on Emotional and Mental Health (ISEMH) was done to identify high-risk groups whose mental health conditions 7236 vulnerable to the COVID-19 outbreak by using anxiety symptoms, depressive symptoms, and sleep quality ongoing, online psychologicalrelated behavior survey of Chinese public, mentioned that the overall prevalence of anxiety symptoms, depressive symptoms, and poor sleep quality were 35.1%, 20.1%, and 18.2%, respectively. In addition, people aged <35 years reported a higher prevalence of anxiety symptoms and depressive symptoms than people aged ≥35 years. Healthcare workers/younger people who spent a high level of time (≥3 hours/day) had a particular higher prevalence of anxiety symptoms than in those who spent less time (<1 hours/day and 1-2 hours/day) on the outbreak. So, during the COVID-19 outbreak, healthcare workers and younger people were at an especially highrisk of displaying psychological impact when they spent too much time thinking about the outbreak [24].
Conceptual frame work: (Figure 1).
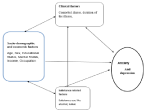
Figure 1: Schematic presentation of the Conceptual Framework developed from literature review.
Justification of the study: A number of studies have inter linked the depression and anxiety to patients with different disease. This study first reported the prevalence of anxiety anddepressioninpatientswithCOVID-19 during the epidemic. Therefore, in the present study, it is worthy of note that social support is one of the key factors linked to anxiety and depression for patients with COVID-19 and also medical workers as the major peer support that is of great significance to infected patients.
So the current study will add information regarding to Severity of Measurements and Associated Factors of anxiety and depression among covid-19 patients. It may also serve as a clinical reference to health care providers who work at psychiatric clinic to offer comprehensive care to their clients to minimize anxiety and depression and related complications and to early identify and treat anxiety and depression. It may also serve as a reference for future studies and to develop policies and plans.
Objectives
General objective
• To assess the Prevalence and Factors Associated with Depression and Anxiety of Hospitalized Patients with COVID-19 in St. Peter Specialized Hospital Treatment Centres Addis Ababa, Ethiopia, 2020 G.C
Specific objectives
• To determine the Magnitude of Depression among patients with covid-19
• To determine the Magnitude of Anxiety among patients with covid-19
• To identify factors Associated with Depression among patients with covid-19
• To identify factors Associated with Anxiety among patients with covid-19
Methods and Materials
Study setting and population
The study was institution based cross sectional design, conducted from June 1st to 15th of 2020 in St. Peter Specialized Hospital COVID-19 Treatment Centers Addis Ababa, Ethiopia. All adult patients (age ≥18) who had diagnoses of confirmed with covid-19 and those who were given their written consent to participate in the study were included in the sample. Critically ill patients were excluded from the study. Among 385patients who had admitted in St. Peter Specialized Hospital Treatment Center, 373 patients were recruited for the study. Study participants were included using purposive sampling technique.
Data collection
A structured questionnaire was used to collect the data on socio-demographic characteristics (age, sex, ethnicity, religion, education, occupation, and marital status). HADS was used to measure the anxiety and depression level among Admitted in the Hospital for COVID-19 disease. HADS is a 14-item questionnaire, commonly used to screen for depression and anxiety, 7 for anxiety and 7 for depression [14]. The scales used a cut off score for anxiety and depression ≥8 (30).It was validated in Ethiopia and internal consistency was 0.78 for anxiety, 0.76 for depression subscales and 0.87 for full scale. Social support was collected by Oslo 3-item social support scale, it has 3-item questionnaire commonly used to assess social support and it had been used in several studies, the sum score scale ranging from 3-14, which had three broad categories: “Poor Support” 3-8, “Moderate Support” 9-11 and “Strong Support” 12- 14. Data were collected by clinical nurses using pretested interviewer administered questionnaire.
Data processing and analysis
All questionnaires were checked for completeness and consistency of responses manually. After cleaning data was enter, in to EPI info version 7 then it was export to SPSS versions 20 for analysis. Descriptive statistics (frequencies and percentages) was used to explain the study participant in relation to study variables. Bivariate and multivariate analysis was used to determine the presences of statistically significant associations between the independent variables anxiety and depression. The strength of the association was presented by odds ratio and 95% confidence interval. A p-value of less than 0.05 on multivariate analyses was considered as statistically significant.
Ethical considerations
Ethical clearance was obtained from IRB ethical review board of St. Peter Specialized Hospital. After thoroughly discussing, the ultimate purpose and method of the study, a written consent will seek from St. Peter Specialized Hospital and Supporting Letter from MoH Clinical General Directorate Director. Informed verbal consent was obtained from each respondent. The respondents were informing that their inclusion in the study was voluntary and they are free to withdraw from the study if they are not willing to participate. If any question they do not want to answer they have the right to do so. To ensure confidentiality of respondents, their names were left out on the questionnaire. All interviews were individually to keep confidentiality. Based on the HADS, those who had symptoms of anxiety and depression were clinically further assessed on voluntary bases by referral to St. Peter Specialized Hospital psychiatric clinic/ unit for further diagnosis.
Results
Socio-demographic characteristics of the respondents
A total of 385 participants were included in the study, 373 volunteers, for a participation which makes the response rate 88.4%. After excluding the invalid questionnaires. The mean age of the respondents was 37.46(±SD =16.09) years. Among the respondents, the majority 157 (42.1%) were in age 30 years and below years, 220(59.0%) were male, 191 (51.2%) were married, 167 (44.8%) had secondary school education, 247 (66.2%) were orthodox religion members, 155 (41.6%) were employed at government institution and 177 (47.5%) had monthly income of above 2000 birr (Table 1).
Variables
Frequency
Percent (%)
Age
30 & below
157
42.1
31-40
109
29.2
41 & above
107
28.7
Sex
Male
220
59
Female
153
41
Marital status
Married
191
51.2
Single
159
42.6
Divorced
12
3.2
Widowed
11
2.9
Educational status
Primary school
64
17.2
Secondary school
167
44.8
Higher education
112
30
Unable to read and write
30
8
Religion
Orthodox
247
66.2
Muslim
52
13.9
Protestant
68
18.2
Catholic
3
0.8
Other
3
0.8
Job
Government
155
41.6
Jobless
53
14.2
Housewife
30
8
Student
18
4.8
Self
99
26.5
Other
18
4.8
Monthly income
1000 birr & below
112
30
1001-2000 birr
84
22.5
2001 & above
177
47.5
Table 1: Distribution of the socio demographic characteristics among patients Admitted in St. Peter Specialized Hospital COVID-19 Treatment Centers Addis Ababa, Ethiopia, 2020 EC.
Clinical, psychosocial and substance use characteristics of the respondent
Regarding to Clinical, Psychosocial and Substance use characteristics of the respondent, the majority 283 (75.9%) had no any diagnosed co-morbid illness, out of the 90 cases 34 (37.8%) of them had HTN as a co-morbid illness, 61 (67.8%) were lived for 6 months and above duration with the co-morbid illness and 55 (61.1%) were took a medication for more than a month. From all study participants, 210 (56.3%) of them had intermediate social support, 364 (97.6%) had no any history of tobacco use and 317 (85.0%) & 358 (96.0%) had no any history of alcohol and amphetamine use history respectively (Table 2).
Variables
Frequency
Percent (%)
Co-morbid illness
Yes
90
24.1
No
283
75.9
Types of co morbid illness
Diabetics
28
31.1
Renal disease
3
3.3
Liver disease
2
2.2
HIV infection
5
5.6
Schizophrenia
3
3.3
Epilepsy
2
2.2
HTN
34
37.8
Other
13
14.4
Duration of the illness
Equal to one month
22
24.4
2-3 month
3
3.3
4-5 month
4
4.4
6 month and above
61
67.8
Have you face an impact due to the illness
Yes
44
48.9
No
46
51.1
Treated for the same case previously
Yes
59
65.6
No
31
34.4
Take medication for more than one month
Yes
55
61.1
No
35
38.9
Social support
Low social support
77
20.6
Intermediate social support
210
56.3
Good social support
86
23.1
Tobacco use history
Yes
9
2.4
No
364
97.6
Alcohol use history
Yes
56
15
No
317
85
Amphetamine use history
Yes
15
4
No
358
96
Duration of COVID-19 symptoms
7 days & below
81
21.7
8-14 days
179
48
15 days and above
113
30.3
Table 2: Description of clinical, psychosocial factors among patients Admitted in St. Peter Specialized Hospital COVID-19 Treatment Centers Addis Ababa, Ethiopia, 2020 EC.
Explanatory Variables
Anxiety
COR,95%(CI)
AOR,95%(CI)
No
Yes
Age
30 & below
139
18
1
1
31-40
88
21
1.84 (0.93, 3.65)
1.44, (0.62, 3.33)
41 & above
67
40
4.61 (2.46, 8.64)*
2.16, (0.85, 5.51)
Sex
Male
163
57
2.08, (1.21, 3.58)*
5.01, (2.11, 11.87)**
Female
131
22
1
1
Marital status
Married
137
54
2.74 (1.56, 4.82)*
1.56, (0.71, 3.43)
Divorced
9
3
2.32 (0.58, 9.28)
2.71, (0.44, 16.58)
Widowed
9
2
1.54 (0.31, 7.67)
2.34, (0.14, 39.64)
Single
139
20
1
1
Job
Government
134
21
1
1
Jobless
36
17
3.01, (1.44, 6.30)*
2.74, (0.95, 7.90)
Housewife
16
14
5.58, (2.38, 13.09)*
11.43, (2.67, 48.90)**
Student
15
3
1.28, (0.34, 4.79)
2.62, (0.41, 16.64)
Self
75
24
2.04, (1.07, 3.91)*
2.45, (1.07, 5.60)**
Other
18
0
0.00, (0.00, 0.00)
0.000, (00, 00)
Income
1000 birr & below
79
33
1.97, (1.12, 3.45)*
1.57, (0.56, 4.38)
1001-2000 birr
69
15
1.02, (0.52, 2.02)
1.02, (0.43, 2.41)
2001 & above
146
31
1
1
Duration of COVID-19 SX
7 days & below
61
20
3.04, (1.36, 6.77)*
3.21, (1.21, 8.58)**
8-14 days
131
48
3.40, (1.68, 6.87)*
3.70, (1.55, 8.84)**
15 days and above
102
11
1
1
Diagnosed chronic illness
Yes
58
32
2.78, (1.63, 4.72)*
2.56, (1.19, 5.53)**
No
236
47
1
1
Social support
Low/poor
50
27
4.62, (2.01, 10.64)*
3.42, (1.21, 9.63)**
Medium/ intermediate
167
43
2.20, (1.02, 4.75)*
1.19, (0.47, 3.00)
High/good
77
9
1
1
*Significant association (p-value<0.05 in bivariate), **-significant association (p-value<0.05in multivariate analysis); Diagnosed chronic illness=DM, HTN, renal disease, liver diseases, Epilepsy, HIV/AIDS…
Table 3: Factors associated with Anxiety among patients Admitted in St. Peter Specialized Hospital COVID-19 Treatment Centers Addis Ababa, Ethiopia, 2020 EC.
Explanatory Variables
Depression
COR, 95%(CI)
AOR, 95%(CI)
No
Yes
Age
30 & below
117
40
1
1
31-40
76
33
1.27, (0.74, 2.19)
1.15, (0.58, 2.27)
41 & above
44
63
4.19, (2.47, 7.09)*
3.95, (1.80, 8.69)**
Educational level
Primary education
44
20
1.04, (0.54, 2.03)
.60, (0.24, 1.51)
Secondary school
104
63
1.39, (0.83, 2.31)
1.35, (0.72, 2.54)
Unable to read and write
11
19
3.96, (1.70, 9.22)*
1.28, (0.37, 4.42)
Higher education
78
34
1
1
Marital status
Married
105
86
2.28, (1.45, 3.59)*
0.99, (0.52, 1.93)
Divorced
10
2
0.56, (0.12, 2.65)
0.21, (0.03, 1.41)
Widowed
5
6
3.34, (0.97, 11.53)
2.80, (0.54, 14.49)
Single
117
42
1
1
Job
Government
109
46
1
1
Jobless
16
37
5.48, (2.78, 10.82)*
2.37, (0.98, 5.69)
Housewife
11
19
4.09, (1.81, 9.28)*
1.09, (0.32, 3.68)
Student
12
6
1.19, (0.42, 3.35)
0.46, (0.10, 2.04)
Self
76
23
0.72, (0.40, 1.28)
0.54, (0.27, 1.11)
Other
13
5
0.91, (0.31, 2.70)
0.16, (0.04, .72)
Income
1000 birr & below
49
63
3.27, (1.99, 5.37)*
2.99, (1.11, 8.05)**
1001-2000 birr
61
23
0.96, (0.37, 1.71)
0.76, (0.35, 1.64)
2001 & above
127
50
1
1
Duration of COVID-19 SX
7 days & below
52
29
1.62, (0.87, 3.00)
1.68, (0.77, 3.67)
8-14 days
101
78
2.24, (1.34, 3.75)*
2.63, (1.34, 5.17)**
15 days and above
84
29
1
1
Social support
Low/poor
38
39
3.39, (1.73, 6.62)*
3.13, (1.34, 7.30)**
Medium/ intermediate
133
77
1.91, (1.08, 3.39)*
1.54, (0.76, 3.11)
High/good
66
20
1
1
*Significant association (p-value<0.05 in bivariate), **-significant association (p-value<0.05in multivariate analysis); Diagnosed chronic illness = DM, HTN, renal disease, liver diseases, Epilepsy, HIV/AIDS…
Table 4: Factors associated with Depression among patients Admitted in St. Peter Specialized Hospital COVID-19 Treatment Centers Addis Ababa, Ethiopia, 2020 EC.
Magnitude of anxiety among COVID-19 patients
This study revealed that the magnitude of anxiety was 21.2% (95% CI 16.9, 25.2), among COVID-19 patients. (Figure 2).
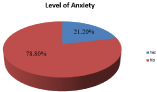
Figure 2: Magnitude of Anxiety among patients Admitted in St. Peter
Specialized Hospital COVID-19 Treatment Centers.
Magnitude of depression among COVID-19 patients
This study revealed that the Magnitude of Depression was 36.5% (95% CI 31.4, 41.3), among COVID-19 patients admitted at St. Peter Specialized Hospital (Figure 3).
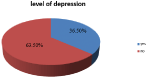
Figure 3: Magnitude of Depression among patients Admitted in St. Peter
Specialized Hospital COVID-19 Treatment Centers.
Factors associated with Anxiety and Depression among COVID-19 Patients Admitted at St. Peter Specialized Hospital
Bivariate analysis: For each Explanatory Variable, Bivariate Analysis was done and Socio-Demographic Factors Such as Age (being 41 and above year), Sex (being Male), Marital Status (Married), Job (being Housewife, Jobless & Self-employed), Monthly Income (having less than 1000birr); Clinical and Social Factors like having Diagnosed Chronic illness, Duration of COVID-19 Symptom (below 7 days &8-14 days) and Social Support (having Poor/low & Intermediate Social Support) were variables fulfilled the minimum requirement (p-value<0.05 significance level) for Anxiety and Factors such as Age (41 & above years), Educational Status (unable to read and write), Marital Status (Married), Job (Housewife & Jobless), Income (having less than 1000 birr), Duration of Symptom (8-14 days) and Social Support (Poor and Intermediate Support) were variables fulfilled the minimum requirement (p-value<0.05 significance level) for Depression for further Multivariate Logistic Analysis.
Multivariate logistic analysis: During the Multivariate Analysis; Sex (being Male), Job (being Housewife & Self-employed), having Diagnosed Chronic illness, Duration of COVID-19 Symptom (below 7 days & 8-14 days) and Social Support (having Poor/low & Intermediate Social Support) were Statistically Significant Associated with Anxiety. Factors such as Age (41 & above years), Income (having less than 1000 birr), Duration ofCOVID-19 Symptom (8-14 days) and Social Support (Poor Support) were Statistically Significant Associated with Depression during Multivariate Analysis.
By using Multivariate (Anxiety) Logistic Regression, Patients who were Male (AOR 5.01, 95% CI (2.11, 11.87)), Housewife (AOR 11.43, 95% CI (2.67, 48.90)), Self-employed (AOR 2.45,, 95% CI (1.07, 5.60)), having Diagnosed Chronic illness (AOR 2.56, 95% CI (1.19, 5.53)), having COVID-19 Symptoms for below 7 days and for 8-14 days ((AOR 3.21, 95%CI (1.21, 8.58)) & AOR 3.70, 95% CI (1.55, 8.84)) respectively) and those who had Poor/low Social Support (AOR 3.42, 95% CI (1.21, 9.63)) had Statistically Significant Association with Anxiety.
By using Multivariate (Depression) Logistic Regression, Patients who were 41 and above years of old (AOR 3.95, 95% CI (1.80, 8.69)), had Monthly Income of less than 1000 birr (AOR 2.99, 95% CI (1.11, 8.05)), Having COVID-19 Symptoms for 8-14 days (AOR 2.63, 95% CI (1.34, 5.17)) and who had Poor Social Support (AOR 3.13, 95% CI (1.34, 7.30)) were Statistically Significant Associated with Depression.
Discussion
Institution based cross sectional study was conducted to assess the Magnitude and factors associated with Anxiety and Depression among COVID-19 patients admitted in St. Peter Specialized Hospital.
Magnitude and factors associated with Anxiety among covid-19 patients
The study revealed that the prevalence of the current study’s finding for Anxiety was (21.20 %) lower than the study done in Huoshenshan Hospital of Wuhan, China which was 34.72% & Affiliated Hospital of Harbin Medical University which was 38.5%,but higher than the study conducted in southeastern China, including Sichuan Province, Chongqing City which was 12.9%.
The variation might be due to the difference in sample size and data collection toolin Huoshenshan Hospital of Wuhan was done among 144 patients [1] but the tool was similar, which was Hospital Anxiety and Depression Scale (HADS) [6], another study was done in Affiliated Hospital of Harbin Medical University (china) the difference in sample size and data collection tool, Anxiety was assessed using the Zung Self-rating Anxiety Scale (SAS) [4], is a 20-item self-report scale with a total of 78 patients [4]. The multivariate logistic regression analysis in the current study showed that some of the variables were significantly associated with anxiety. With respect to gender, being Male was 5.01 times more likely to have Anxiety than Females. The possible reason might be increased Exposure to acute life events, Gender Specific Roles and Higher Social Networks. The current result is smaller than the study conducted in Huoshenshan Hospital of Wuhan [13] & Affiliated Hospital of Harbin Medical University (china) but higher than the study conducted in southeastern China, including Sichuan Province, Chongqing City.
Job who were House wife & Self-employed had 11.43 and 2.45 times respectively more likely to have Anxiety as compared with those who were recruited at government institution. This might be due to a life-changing Disastrous experience, Exposed to New Environment, Economical Crises, apart from marketing or new process. This might be due to the difference in Role of female increase socio-demographic, culture [20].
In addition, having duration of COVID-19 symptoms for 7 days & below and8-14 days were 3.21 & 3.70 times respectively than more likely to have anxiety as compared with those who were duration of 15 & above. This might be due to the number of days, exposed to new pandemic infections which are difficult to understand and easily adopted and taking infectious protective equipment like mask& sanitizer frequently.
Regarding to social support, those who had poor social support were 3.42 times more likely to have anxiety than covid-19 patients who had good social support; this might be due to feeling of loneliness and lack of social interaction. The current result is higher than the study conducted in Huoshenshan Hospital of Wuhan, China [25].
Magnitude and factors associated with depression among COVID-19 patients
The study revealed that the prevalence of depression was 36.5%. Regarding the prevalence, the current study’s finding was similar with other studies carried out in Affiliated Hospital of Harbin Medical University (china) 35.9% [12]. However, the current study result is higher than the studies conducted in Huoshenshan Hospital of Wuhan, China which was 28.4% [26], in southeastern China, including Sichuan Province, Chongqing City which was 22.4% [25], in 194 cities in China which was 16.5% [12].
The variation might be due to the difference in sample size and data collection tool which was Zung Self-rating Depression Scale (SDS) [4] is a 20-item self-report scale with a total of 78 patients (4) Huoshenshan Hospital of Wuhan, China and in Affiliated Hospital of Harbin Medical University (china) by using short review on the psychological effects of COVID-19 and its association with anxiety& depression by using the electronic databases, including PubMed, Medline, Elsevier, and Science Direct as a source of data mentioned that 1210 participants.
The multivariate logistic regression analysis in the current study showed that some of the variables were significantly associated with Depression. With respect to age, those who were in the age interval of 41 & above years were 3.95 times more likely to have depression as compared than those who were 40 and below years old. The current result is similar with the study conducted in Huoshenshan Hospital of Wuhan [18].
Regarding to income, those who are 1000 & below were 2.99 times more likely to have depression respectively as compared to those who were 2001 & above. This might be due to lack of social interaction; unfamiliar types of the disease (pandemic) [25] lock down (stay home) problem of social support [12].
With respect to duration of covid-19 symptoms, patients who were manifested for 8-14 days were 2.63 times more likely to have depression as compared to those who had 15&above days of symptom. This might be due to being unfamiliar with the symptoms of the illness and fear of further complication. In addition, those who had poor social support were 3.13 times more likely to have depression as compared to those who had good social support. Having a strong family relationship has its own contribution in prevention as well as subsiding of depression symptoms.
Strength and Limitation of the Study
Limitation of the study
Among the limitation of this study, the fact related to the crosssectional design used, which simultaneously evaluate variables of the effect of interest and their associated factors, should be emphasized. Thus, it could not possible to identify whether influenced the associated factors or the outcome variable. Second, using invalidated tool to assess the substance related issues.
Conclusion and Recommendation
Conclusion
In the current study area, the magnitude of anxiety was (21.20%) high. It had statistically significant association with being age 41 & above, being male, house wife, self-employed, duration of COVID-19 Symptoms (below-7 & 8-14) and poor social support. Further the magnitude of depression was (36.5%) high. It had statistically significant association with older age (41 & above), income 1000 birr & below, duration of COVID-19 symptoms (8-14) and having poor social support.
Recommendations
To Amanuel mental Specialized Hospital (Ministry of Health In General):-
• The Ministry of Health should develop screening tools for anxiety and depression among patients that helps to early identifying cases among these pandemic.
• More attention should be given for Poor Social support.
• Good social interaction and suitable treatment environment should be created within the Hospital to prevent or minimize depression and anxiety due to stressful life events.
• Psychological related lessons should be given early at first Admitting prior the beginning of treatment & other care.
• Generally, early recognition of vulnerable factors associated with Anxiety and Depression among COVID-19 (Pandemic) patients is necessary to treat effectively.
Author Contributions
Conceived and designed the proposal: Performed the study: Analyzed the data: Wrote the paper.
Bizuayehu Assefa Dereseh (email: eldaza14@gmail.com ) Telephone-+251-911-480507 ,+251-900-571757).
Acknowledgement
First of all, I would like to thank to Amanuel Mental Health Specialized Hospital for their financial support to the accomplishment of this research thesis and their cooperation that they help me to get the data of current patients to determine sample size and their help during data collection time.
For my family members, Elenatal Bizuayehu, Dawit Bizuayehu and sr.zayed wored for their time. Additional, for minister of health clinical directorate director Yakop Seman for his valuable support.
Finally, I would like to thank my study participants for their participation in the study voluntarily, data collectors especially Sentayehu Birehan, Yonas wendu and St. Peter Specialized Hospital Research & Evidence Generation Department Staff.
References
- Special Expert Group for Control of the Epidemic of Novel Coronavirus Pneumonia of the Chinese Preventive Medicine Association. An update on the epidemiological characteristics of novel coronavirus pneumonia (COVID-19). Chinese Journal of Epidemiology. 2020; 139-144.
- Wuhan Municipal Health Committee. Report of Wuhan Municipal Health Committee on viral pneumonia of unknown cause.
- World Health Organization. Novel Coronavirus (2019-nCoV) Situation Report-11. 2020.
- Health Commission of the people’s Republic of China. Pneumonia situation in novel coronavirus infection. 2020.
- World health organization. Mental health and psychosocial considerations during the COVID-19 outbreak. 2020.
- United Nations Coordinated Appeal. Global Humanitarian Response Plan. Global HRP for COVID-19. 2020.
- Guan W-J, Ni Z-Y, Hu Y, Liang WH, Ou CQ, He JX, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020.
- Jiang G, Ren X, Liu Y, Liu W, Guo Z, Chen C, et al. Application and optimization of RTPCR in diagnosis of SARS-CoV-2 infection. Med Rxiv. 2020.
- Ai T, Yang Z, Hou H, Zhan C, Chen C, Lv W, et al. Correlation of chest CT and RTPCR testing in coronavirus disease 2019 (COVID-19) in China: a report of 1014 cases. Radiology 200642. 2020.
- Xu G, Yang Y, Du Y, Peng F, Hu P, Wang R, et al, Clinical Pathway for Early Diagnosis of COVID-19: Updates from Experience to Evidence-Based Practice, Clinical Reviews in Allergy & Immunology. 2020.
- Bayram N, Bilgel N. The prevalence and socio-demographic correlations of depression, anxiety and stress among a group of university students. Soc Psychiatry Psychiatr Epidemiol. 2008; 43: 667-672.
- Phua DH, Tang HK, Tham KY. Coping Responses of Emergency Physicians and Nurses to the 2003 Severe Acute Respiratory Syndrome Outbreak. Acad Emerg Med. 2005; 12: 322-328.
- Wang C, Pan R, Wan X, Tan Y, Xu L, Ho CS, et al. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int J Environ Res Public Health. 2020; 17: 1729.
- Rodin P, Ghersetti M, Oden T. Disentangling rhetorical subarenas of public health crisis communication: a study of the 2014-2015 Ebola outbreak in the news media and social media in Sweden. J Contingencies Crisis Manag. 2018; 27: 237-246.
- Tang L, Bie B, Park SE, Zhi D. Social media and outbreaks of emerging infectious diseases: a systematic review of literature. Am J Infect Control. 2018; 46: 962-972.
- Ricci-Cabello I, Meneses-Echave JF, Serrano-Ripoll MJ. Impact of Viral Epidemic Outbreaks on Mental Health of Healthcare Workers: A Rapid Systematic Review. med Rxiv preprint. 2020.
- Wang C, Pan R, Wan X, Tan Y, Xu L, Cyrus S, et al. Immediate Psychological Responses and Associated Factors during the Initial Stage of the 2019 Coronavirus Disease (COVID-19) Epidemic among the General Population in China. Int J Environ Res Public Health. 2020; 17: 1729.
- Fardin MA. COVID-19 and Anxiety: A Review of Psychological Impacts of Infectious Disease Outbreaks, Arch Clin Infect Dis. 2020: e102779.
- Ethiopia FMOH. National Comprehensive COVID19 Management Handbook FMOH. Ethiopia First edition. 2020.
- Kong X, Zheng K, Tang M, Kong F, Kong F, Zhou J, et al, Prevalence and Factors Associated with Depression and Anxiety of Hospitalized Patients with COVID-19, medRxiv preprint. 2020.
- GaoID J, Zheng P, Jia Y, Chen H, Mao Y, Chen S, et al. Mental health problems and social media exposure during COVID-19 outbreak. PLoS One. 2020; 15: e0231924.
- Holmes EA, O’Connor RC, Perry VH, Tracey I, Wessely S, Arseneault L, et al. Multidisciplinary research priorities for the COVID-19 pandemic: a call for action for mental health science. Lancet Psychiatry. 2020.
- Rajkumar RP. COVID-19 and mental health: A review of the existing literature, Asian Journal of Psychiatry. 2020; 52: 102066.
- Huang Y, Zhao N. Mental health burden for the public affected by the COVID-19 outbreak in China: Who will be the high-risk group?, Psychology, Health & Medicine. 2021.
- Gelaye B, Williams MA, Lemma S, Deyessaetal N. Validity of the Patient Health Questionnaire-9 for Depression Screening and Diagnosis in East Africa, Psychiatry Res. 2013; 210: 653-661.
- Dalgard OS, Dowrick C, Lehtinen V, Vazquez-Barquero JL, Casey P, Wilkinson G, et al. Negative life event, social support and gender difference in depression. Social psychiatry and psyciatric epidemiology. 2006; 42: 444-451.
