
Research Article
J Bacteriol Mycol. 2016; 3(3): 1033.
Dermatophytic Disease: Report of A Tunisian Case Caused by a Sterile Dermatophyte Identified as Trichophyton Rubrum by ITS1 and ITS4 Sequencing
Ghazizadeh S¹*, Abedi J¹, Pourmatroud E¹, Raiisi F² and Lesanpezeshki M¹
¹Ob/Gyn Department Imam Khomeini Hospital, Tehran University of Medical Sciences, Iran
²Roozbeh Psychiatry Hospital, Tehran University of Medical Sciences, Iran
*Corresponding author: Ghazizadeh S, Tehran University of Medical Sciences, Imam Khomeini Hospital, Ob/Gyn Department, Tehran Iran
Received: June 23, 2016; Accepted: August 23, 2016; Published: August 25, 2016
Abstract
Objective: To compare the efficacy of 500Units vs. 250U botulinum toxin A (abobotulinumtoxinA) to treat severe vaginismus.
Method: 51 women with severe vaginismus who had not responded to conventional treatments recruited from Feb. 2007 to Feb.2008. Nine were excluded for not meeting inclusion criteria, 42 were randomly divided. The first group (n=21) received 500U. AbobotulinumtoxinA (BTA), the second group (n=21) received 250U. Patients filled out a sexual questionnaire and had a pelvic exam before the procedure, after one month they filled out same questionnaire; pelvic exam repeated at the same time. Main outcomes were improvement of sexual dysfunction. And relief of pelvic resistance
Result: Sexual dysfunction improved after injection of 500U. BTA (P value < 0.0001), Pelvic exam showed significant relaxation in both groups but more pronounced in the first group (P value < 0.0001). Libido remained unchanged. Fear from intercourse was 68.3% before the injection; it was relieved significantly in the first group (P value < 0.0001). Orgasm showed great improvement in the first group (P value < 0.02).
Conclusion: BTA in dose of 500Units is more effective than 250U. to treat severe vaginismus.
Keywords: Vaginismus; Botulinum toxin; Dyspareunia; AbobotulinumtoxinA
Introduction
The “vaginismus” term was first used in 1862 by Marion Sims to describe an involuntary contraction of the paravaginal muscles, ending in the nonconsummation of the marriage [1]. Vaginismus is defined according to DSM IV [2] as recurrent or persistent involuntary spasm of the musculature of the outer third of the vagina, which interferes with coitus and causes distress and interpersonal difficulty.
Severe spasm or tightening of the paravaginal muscles during attempted intercourse may vary from reflexive spasm of the pelvic muscles in response to attempted vaginal entry to voluntary muscle guarding in response to the expected or the repeated experience of pain [3]. In the severe forms of vaginismus, other muscles such as the abductors, the rectus abdominis, and the gluteus maximus may also be involved.
The new proposal for the 5th Diagnostic and Statistical Manual of Mental Disorders (DSM-5) is to discard the long-established differentiation between vaginismus and dyspareunia and to combine these two entities into one [4].
It may be primary (life-long), since first attempt of intercourse; or may be acquired (secondary), presented after an interval of painfree coital activity. In case of acquired type medical disorders such as vulvodynia or marital conflicts should be ruled out. Primary type is more common than acquired.
This involuntary spastic contraction is a reflex response that is stimulated by imagined, anticipated, or real attempts at vaginal penetration. In severe cases of vaginismus, the abductors of the thighs, the rectus abdominis, and the gluteus muscles also may be involved. Vaginismus may prevent intercourse in the most severe degrees, whilst in the milder ones it becomes a cause of dyspareunia [5]. Addar et al in a review of couples with unconsummated marriages found vaginismus as the primary cause in 63.9% of the cases [6]. Simonelli, et al. reported that by age 40, 7.8% of women reported vulvar pain [7].
Treatment of vaginismus is directed toward extinguishing the conditioned involuntary vaginal spasm. This can be accomplished by desensitization techniques that put a woman in control of relaxation of the musculature. Activities include Kegel exercises and inserting small objects (eg, dilator, syringe, finger) in and out of the vagina to teach that control of introital musculature can be voluntary and painless. Other approaches include sex therapy, hypnotherapy. Medications such as lubricants, anesthetic creams, propranolol, or alprazolam to reduce anxiety have been used effectively [8]; In a case series study we successfully used Botulinum toxin A to treat moderate to severe vaginismus [9]. Botulinum Toxin A (BTA) is a neurotoxin produced by Clostridium botulinum, a spore-forming anaerobic bacillus, which appears to affect only the presynaptic membrane of the neuromuscular junction in humans. Muscle inactivation persists until new fibrils grow from the nerve and form junction plates on new areas of the muscle-cell walls [10].
Renal, hepatic, or other diseases do not have any effect on the distribution or binding of botulinum toxin. This toxin is thought to be metabolized locally [10]. The minimum dose of toxin necessary to produce systemic toxicity is not known. However, by extrapolation of animal experiments, it is calculated that 160 vials of the drug would be needed to produce systemic symptoms of toxicity [10].
It was observed that botulinum toxin not only treated the neuromuscular disorders but that the associated pain appeared to be ameliorated. The total dose and frequency should be minimized in an effort to avoid development of antibodies; however, the incidence of antibody development is low (4%) [11].
The purpose of this study was to compare the efficacy of different doses of BTA (500U. vs. 250 U Dysport ) in severe cases of vaginismus.
Materials and Methods
According to the effectiveness of conventional treatment and our pilot study on botulinum toxin efficacy, for a level of significance of < 5% and power of 90%, sample size needed was estimated to be 30 patients, (15 in each group) we added 30% more in order to cover the lost to follow up. Study was registered as a clinical trial (NCT 00638066).
From February 2007 to February 2008, 51 women with severe vaginismus recruited for the study. All patients had tried different types of treatments such as behavior therapy technique, reverse Kegel exercise anesthetic creams, vaginal lubricants, but none of them were effective, Patients with vulvodynia or positive findings on the cotton swab test; vestibulodynia, and those with hymenal ring abnormality were excluded from the study. Also those with known contraindications to botulinum toxin; such as hypersensitivity to albumin, infection at the injection site, pregnancy; diseases of neuromuscular transmission; and coagulopathy or therapeutic anticoagulation were excluded. In addition they all received a psychiatrist consultation to rule out any underlying psychiatry problem. 51 patients participated, 9 excluded due to not meeting inclusion criteria. 42 patients randomly divided in two groups, there were no lost to follow up.
Written consent form was signed by the patients. They were randomly divided in two groups according to odd and even days; the first group received 500U. of botulinum toxin, while the second group received 250units.
The procedure was done in a day clinic unit, one vial of 500 units botulinum toxin type A (Dysport; Ipsen Ltd., United Kingdom) was diluted with either 2ml (500u/2cc solution No.1) or 4ml (250u/2cc solution No.2) of normal saline. Using a 23-gauge needle and insulin syringe; 2ml. of solution No. 1 or 2 was injected evenly into six sites, three on either side of the puborectalis muscle on the lateral wall of the vagina about 2-3 cm. above the hymen (Figure 1). Patients characteristically show involuntary spasm of these muscles during injection (Figure 2).
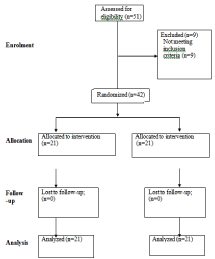
Figure 1: Consort statement flow diagram.
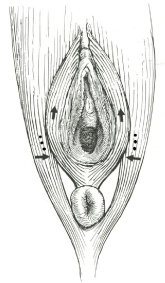
Figure 2: Contraction of the puborectalis muscle exerts some side to side
compression of the lower vagina. Black spots show sites of injections.
During this procedure oxygen was given via face mask (6-8 lit/ min) and SPO2 was monitored using pulse oximeter. In addition, light sedation was administered by midazolam and fentanyl ranging from 1-5mg and 50-150mg respectively. As some extent of muscular contraction was required to find the exact location of muscles; the sedation was not deep. Moreover, hymenectomy was performed for the patients having intact hymen. Finally a vaginal tampon was inserted for a few hours to stop bleeding. The patients were discharged on the same day.
Before the procedure all patients filled out Sexual Dysfunction Inventory (SDI) Questionnaire and had a pelvic exam by one gynecologist. One month later they filled out same questionnaire; pelvic exam repeated at the same time by the same gynecologist who was blinded to the randomization group.
The Statistical Package for the Social Sciences (SPSS) 15.0 was used to analyze the data. Analysis between two groups was done by Chi-square; analysis within each group performed by Wilcoxon Rank and McNemar tests. P ≤.05 was considered statistically significant.
Results
The mean age of the participants was 28.7 ±5.8 years (range 18- 40). The women were married for a mean of 5.4±5 months (range 1-25). Both groups were similar in terms of age (29.5±6.4 vs. 28±5.1 years; P>0.3) and duration of marriage (6±4.8 vs. 4.98±5.2; P>0.5). Intact hymen was found in 42.6% of the first group and 28.6% of the second group (P>0.07).
Results showed that, coital problems were greatly improved after injection of 500U BTA (P value <0.0001), although the second group also showed some improvement, but it did not reach statistical significance according to Table 1. Pelvic exam showed significant relaxation in both groups but more pronounced in the first group (P value <0.0001) (Table 2). Libido was unchanged after the injection (Table 3). Fear from intercourse was found in 68.3% of all patients before the injection; it was relieved significantly only in the first group (P value <0.0001) (Table 4). Orgasmic dysfunction also showed great improvement in the first group (P value <0.02) (Table 5).
Coitus
Before
After
P value
No coitus
painful
Normal
No coitus
painful
Normal
500U
10 (47.6%)
11(52.3%)
0 (0%)
2 (9.5%)
1 (4.8%)
18 (85.7%)
0.0001
250U
6 (28.6%)
15(71.4%)
0 (0%)
3 (14.3%)
7 (33.3%)
11 (52.4%)
0.45
Total
16(38.1%)
26(61.9%)
0 (0%)
5(11.9%)
8(19%)
29(69.0%)
Table 1: Frequency of coital problems before and after the injection.
P/Exam
Before
After
P Value
Impossible/ very painful
Possible/ mild pain
Impossible/very painful
Possible/ mild pain
500U
12(57.1%)
9(42.9%)
4(19%)
17(81%)
0.0001
250U
11(52.4%)
10(47.6%)
9(43%)
12(57%)
0.001
Total
23(54.8%)
19(45.2%)
13(31%)
29(69%)
Table 2: Pelvic exam before and after the injection.
Libido
Before
After
P Value
Decreased
Normal
Decreased
Normal
500U
6(28.6%)
15(74.1%)
4(19%)
17(81%)
0.48
250U
5(23.8)
16(76.2%)
6(28.6%)
15(71.4%)
0.56
Total
11(26.2)
31(73.8)
10(23.8%)
32(76.2%)
Table 3: Libido in two groups before and after the injection.
Fear
Before
After
P Value
Yes
No
Yes
No
500U
17 (85%)
3 (15%)
3 (14.3%)
18 (85.7%)
0.0001
250U
11 (52.4%)
10 (47.6%)
9 (42.9%)
12 (57.1%)
0.15
Total
28 (68.3%)
13 (31.7%)
12 (28.6%)
30 (71.4%)
Table 4: Fear from coitus before and after the injection.
Orgasm
Before
After
P value
No Orgasm al
Occasion
Always
No Orgasm
Occasional
Always
500U
8(40%)
7(35%)
5(25%)
3(14.3%)
5(23.8%)
13(61.9%)
0.02
250U
7(33.3%)
6(28.6%)
8(38.1%)
8(38.1%)
8(38.1%)
5(23.8%)
0.31
Total
15(36.6%)
13(31.7%)
13(31.7%)
11(26.2%)
13(31%0
18(42.9%)
Table 5: Orgasmic dysfunction before and after the injection.
Comparison between two groups showed that satisfactory coitus was achieved in the first group more significantly than the second group (p value<0.04) there was also less fear from intercourse in the first group (p value<0.04); orgasm was more common in the first group (p value<0.03). There was no difference between two groups in terms of pelvic exam discomfort and libido. There were no major complications during or after the injection. Two patients had a temporary constipation which was relieved in a few days. No patient reported fecal or urinary incontinence.
Discussion
The term “vaginismus” was originally used in 1862 by Dr. Marion Sims to describe a reflex- like contraction of the circumvaginal musculature, resulting in nonconsummation of marriage [12]. Management of vaginismus aims at helping the woman to regain voluntary control of her pelvic floor muscles. The treatment utilizes a behavioral method aimed at teaching relaxation of pelvic floor muscles together with a systematic desensitization of the fear of vaginal penetration. Surgical correction is almost never required and may be detrimental to achieving success [13]. Sex therapy is also effective but there is a correlation between duration of unconsummation, severity of vaginismus and success rate [14]. Sildenafil on demand therapy for 1-3 month has been reported to be successful [15]. Female partners of men with Erectile Dysfunction (ED) reported dyspareunia and vaginismus more frequently [16], ED can be secondary to these female problems.
Pacik, P.T. in his comprehensive study concluded that compared with other sexual pain disorders such as vulvodynia and vestibulodynia, the treatment of vaginismus has the highest success rate [17].
Our previous study demonstrated the effectiveness of botulinum toxin type A injection in the treatment of moderate and severe cases of vaginismus [9].
In a placebo controlled study of 13 patients, Shafik et al also reported complete response to botulinum toxin injection [18]. Brin and Vapnek reported a case of dyspareunia complicated with interstitial cystitis that was treated with injection of botulinum toxin at 2 consecutive sessions [19], Abbott and his colleagues showed that botulinum toxin type A is more effective than placebo at reducing pain and pelvic floor pressure in women with chronic pelvic pain and pelvic floor muscle spasm [20]. Botulinum toxin type A injected into the levator ani muscles of women with objective pelvic floor muscle spasm decreases pain symptoms and improves quality of life. These results were not influenced by dilution. In a retrospective study by Fageeh on six cases of severe vaginismus, four of which had a previous history of treatment failure, and two who were unresponsive to 4 months of conventional therapy. Five patients who received the Botox therapy had satisfactory intercourse on the same day of the treatment. One patient required a repeat injection after 2 months for recurrent vaginismus [21].
Bertolasi et al in their search identified 12 studies for review (including a randomized controlled trial) showing that BTA effectively reduces pain in chronic genital pain syndromes associated with pelvic floor spasm, helping to restore a normal sexual life [22]. A recent methanalysis by Ferreira, et al indicates that botulinum toxin is an effective therapeutic option for patients with vaginismus (pooled odds ratio of 8.723 with 95% confidence interval limits of 1.942 and 39.162, p = 0.005). This may hold particularly true in treatmentrefractory patients because most of the studies included in their meta-analysis have enrolled these subjects in their primary analysis [23]. BTA injections also seem to improve vulvodynia and vulvar vestibulitis [24,25].
In this study we compared the efficacy of two different doses of toxin (250U. vs. 500u.). There were no complications during or after the injection also no fecal or urinary incontinence was reported; only 2 patients had a temporary constipation. Libido was normal in most patients and remained unchanged after the injection.
Coital problems including fear from intercourse and orgasmic dysfunction were greatly improved after injection of 500U. BTA, the second group receiving 250U also showed some improvement, but it did not reach statistical significance. Although pelvic exam showed significant relaxation in both groups; it was more pronounced in the first group.
Conclusion
Intravaginal injection of botulinum toxin type A (Dysport) in dose of 500U is more effective than 250U to treat severe cases of vaginismus; in those who had received 500U of toxin sexual satisfaction also greatly improved.
References
- Sims JS. On vaginismus. Trans Obstet Soc Lond. 1861; 3: 356-367.
- Diagnostic and statistical manual of mental disorders. 4th ed: Washington, DC : American Psychiatric Association. 1994.
- Diagnostic and statistical manual of mental disorders. 5th ed: Arlington, VA, American Psychiatric Association. 2013.
- YM B. The DSM diagnostic criteria for vaginismus. Archives of Sexual Behavior. 2010; 39: 292-303.
- Graziottin A. Etiology and diagnosis of coital pain. J Endocrinol Invest. 2003; 26: 115-121.
- Addar MH. The unconsummated marriage: causes and management. Clin Exp Obstet Gynecol. 2004; 31: 279-281.
- Simonelli C, Eleuteri S, Petruccelli F, Rossi R. Female sexual pain disorders: dyspareunia and vaginismus. Current opinion in psychiatry. 2014; 27: 406-412.
- Baram DA. Sexuality, sexual dysfunction, and sexual assault. 14th ed. Baltimore (MD): Lippincott Williams & Wilkins. 2008.
- Ghazizadeh S, Nikzad M. Botulinum toxin in the treatment of refractory vaginismus. Obstet Gynecol. 2004; 104: 922-925.
- Dollery C. Therapeutic drugs. New York: Churchill Livingstone. 1999.
- Jankovic J, Schwartz K. Response and immunoresistance to botulinum toxin injections. Neurology. 1995; 45: 1743-1746.
- Lamont JA. Vaginismus. Am J Obstet Gynecol. 1978; 131: 633-636.
- Biswas A, Ratnam SS. Vaginismus and outcome of treatment. Ann Acad Med Singapore. 1995; 24: 755-758.
- Jeng CJ, Wang LR, Chou CS, Shen J, Tzeng CR. Management and outcome of primary vaginismus. J Sex Marital Ther. 2006; 32: 379-387.
- Ghanem H, Zaazaa A, Kamel I, Anis T, Salem A, El Guindi A. Short-term use of sildenafil in the treatment of unconsumated marriages. Int J Impot Res. 2006; 18: 52-54.
- Greenstein A, Abramov L, Matzkin H, Chen J. Sexual dysfunction in women partners of men with erectile dysfunction. Int J Impot Res. 2006; 18: 44-46.
- Pacik PT. Understanding and treating vaginismus: a multimodal approach. International urogynecology journal. 2014; 25: 1613-1620.
- Shafik A, El-Sibai O. Vaginismum: results of treatment with botulin toxin. J Obstet Gynaecol. 2000; 20: 300-302.
- Brin MF, Vapnek JM. Treatment of vaginismus with botulinum toxin injections. Lancet. 1997; 349: 252-253.
- Abbott JA, Jarvis SK, Lyons SD, Thomson A, TG V. Botulinum toxin type A for chronic pain and pelvic floor spasm in women: a randomized controlled trial. Obstet Gynecol. 2006; 108: 915-923.
- Fageeh WM. Different treatment modalities for refractory vaginismus in western Saudi Arabia. J Sex Med. 2011; 8: 1735-1739.
- Bertolasi L, Frasson E, Graziottin A. Botulinum Toxin Treatment of Pelvic Floor Disorders and Genital Pain in Women. Current Women's Health Reviews. 2008; 4: 180-187.
- Ferreira JR, Souza RP. Botulinum toxin for vaginismus treatment. Pharmacology. 2012; 89: 256-259.
- Bennani B, Raki S, Monnier G, Pelletier F, Humbert P. Botulinum toxin for vulvar vestibulitis. Ann Dermatol Venereol. 2006; 133: 807-808.
- Gunter J, Brewer A, Tawfik O. Botulinum toxin a for vulvodynia: a case report. The Journal of Pain. 2004; 5: 238-240.