Research Article
Austin J Biomed Eng. 2014;1(1): 1005.
Understanding Postural Response of Parkinson’s Subjects Using Nonlinear Dynamics and Support Vector Machines
Amit Shukla1*, Ashutosh Mani2, Amit Bhattacharya2 and Fredy Revilla2
1Department of Mechanical and Mfg. Engg, Miami University, USA
2College of Medicine, University of Cincinnati, USA
*Corresponding author: :Amit Shukla, Department of Mechanical and Mfg. Engg, Miami University, Oxford, OH, 45056, USA.
Received: January 20, 2014; Accepted: February 24, 2014; Published: March 05, 2014
Abstract
Parkinson’s disease (PD) produces slowness, stiffness, tremor, shuffling gait and postural instability. This paper is to present an approach to classification and understanding of Parkinson’s patients using their postural response and analyzing it using a L2 norm metric in conjunction with support vector machines. Medication induced dyskinesia is a significant factor altering the postural response of Parkinson’s’ subjects. This paper demonstrates that classification accuracy can be significantly increased if dyskinesia and history of fall is carefully integrated in to the analysis. Long term goal of this research is toprovide an intelligent framework for automatic classification of the Parkinson’s’ subjects thus reducing the burden on clinical staff.
Introduction
More than 1 million people in North America are affected by Parkinson’s disease resulting in balance problems and falls. Postural instability and gait problems become resistant to pharmacologic therapy as the disease progresses. Furthermore, studies suggest that postural sway abnormalities are worsened by levodopa, the mainstay of therapy for PD. There is no proven treatment that slows or halts the progression of the disease [1]. Balance problems and resulting falls due to postural instability are a substantial cause of disability in patients with more advanced Parkinson’s disease [2]. They also contribute to mounting health care costs for society [3], [4]. Understanding falls can provide insight into the pathological mechanism for diagnostic and prognostic applications [5]. Recently, our group proposed the use of L2 norm as a metric for balance [6]. Clinical posture–graphic data on Parkinson’ subjects were analyzed using support vector machines in [7]. It was shown that dyskinesia clearly affects the collected postural data. This results in low classification accuracy using support vector machines. It was demonstrated that SVM is a useful tool and can complement the widely accepted (but very resource intensive) Unified Parkinson’s Disease Rating Scale (UPDRS) [8]. Current paper presents a classification of postural balance test data using Support Vector Machines (SVM) to identify the effect of medicine (levodopa) as well as dyskinesia. Novel aspects of present study include: first, effect of medication induced dyskinesia; second effect of history of falls and thirdly effect of compliant surface on the postural responsedata when analyzed using L2 norm metric using SVM algorithm. his work improves the application of SVM for classification by incorporating the effect of dyskinesia and test condition, while using L2 norm as a metric for balance.
The main objective of this paper is to present a classification method for Parkinson’s disease (PD) patients with respect to wearing–off of PD medication and medication–induced dyskinesia. The secondary objective was to explore the differences between PD patients with and without a history of falls with respect to L2 norm metric. The proposed classification method is based on Support Vector Machines, with L2 norm as the predictor variable.
L2 norm metric was calculated using the data from standard static posture graphic data (postural balance measurements done using force plate in two different conditions: Eyes Open on Firm Surface –EO and Eyes Open on Foam –FO).
Background
Many studies use simple models to represent human postural balance including [9] and [10]. A controlled inverted pendulum with proportional and derivative (PD) control, to stabilize the inherently unstable system, can be used to model human posture. One such model with intermittent control was analyzed in detail by [6]. Linear stability analysis can be used to obtain parametric stability boundary. In addition, the L2 norm of data can be obtained as a metric for quantification of postural response as defined by:
No scaling is performed with respect to the velocity or displacement terms of the measurement for estimation of these L2 norm values.
Clinical rationale for using L2 norm as the classifier variable High average L2 norm represents high energy content, while the smaller L2 norm shows a lower energy content. In clinical trials, it is well established that larger sway of human posture is usually indicative of impending instability. L2 norm clearly matches stability boundary as in [6]. Wearing off of PD medication (ON to OFF state transition) as well as medication induced dyskinesia are associated with higher postural sway [23,24]. Since L2 norm is indicative of energy content of postural sway, we hypothesized that L2 norm would serve as a good predictor for wearing–off of medication and dyskinesia.
Support Vector Machines: a classification tool A Support Vector Machine (SVM) [17–19] is a supervised machine learning algorithm that learns to distinguish between two groups of data based on a set of examples. The set of examples is known as the training set and each entry is marked as belonging to one of two classes. When the number of mutually exclusive classes is two, then the classification problem is referred to as a binary classification problem. The literature on classification of PD for computer aided diagnostics includes [20– 22] where SVM, Neural Network and Rotation Forrest Ensemble classifiers have been used with good outcome. In addition, its application to classification of PD using L2 norm of postural balance data was demonstrated in [7] based on work done in our group. This present paper is an extension where we demonstrate improvement in classification using SVM by considering the effect of dyskinesia as well as the test condition, specifically the influence of compliant surface (EO vs. FO condition).
Data Collection: Protocol and Processing
Posturography [12–14] is typically used to analyze the performance of the human balance system. In this study, postural sway (static posturography) is measured on a force plate platform system in two conditions: ON Medication (Levodopa) and OFF Medication (Levodopa) [15]. For the results presented in this paper, twenty four patients were evaluated before and after medication. Each patient underwent following testing protocols for the evaluation of their postural balance: First, Eyes Open on Force platform (a firm surface) (E0) and second, Eyes Open on Foam placed on Force platform (FO). EO test condition provides postural balance outcomes as a result of inputs from all three afferents (vision, proprioceptors and vestibular systems) necessary for maintenance of Postural balance. On the otherhand, FO test condition provides postural balance outcomes as a result of inputs from vision and vestibular system along with input from challenged (due to standing on Foam) proprioceptor system. Four trials were conducted for EO and two trials were conducted for FO condition for each patient. These test conditions are described in detail in [16]. The recorded data is processed to estimate anteriorposterior as well as mediolateral center of pressure trajectories. Each of the subjects is also evaluated by a trained Physician on Unified Parkinson’s Disease Rating Scale (UPDRS). To compare the effect of dyskinesia [23] on postural sway measurements, subjects wereclassified based on the presence of dyskinesia during the “ON” medication condition:“No Dyskinesia group” (ND) (n=11): Patients who had a rating of zero in the Modified Dyskinesia Scale for aminimum of 9 out of 12 trials during the “ON” medication condition and “Dyskinesia group” (DY) (n=13): Patients who had a rating ofone or greater in the Modified Dyskinesia Scale for a minimum of 9 out of 12 trials during the “ON” medication condition. All ratings were performed by a Movement Disorders Neurologist. The L2 Normis then used as a metric [6] to classify the data first based on stateof medicine (off medicine and on medicine) and then based ondyskinesia rating (DY or ND). Support Vector Machines were used for these classifications. In addition to the classification using SVM, we also explored differences between PD patients with and without a history of falls with respect to L2 norm metric.
Results and Observations
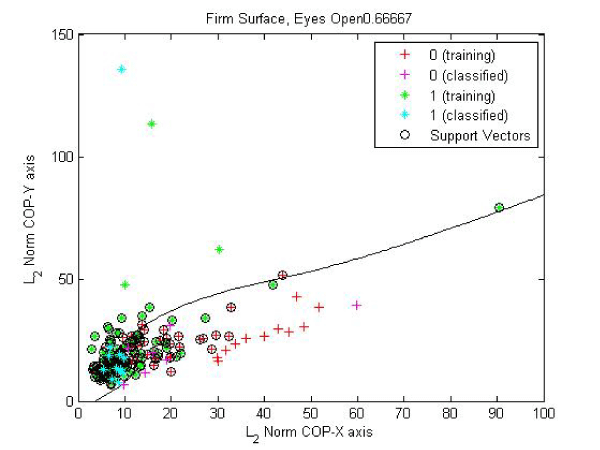
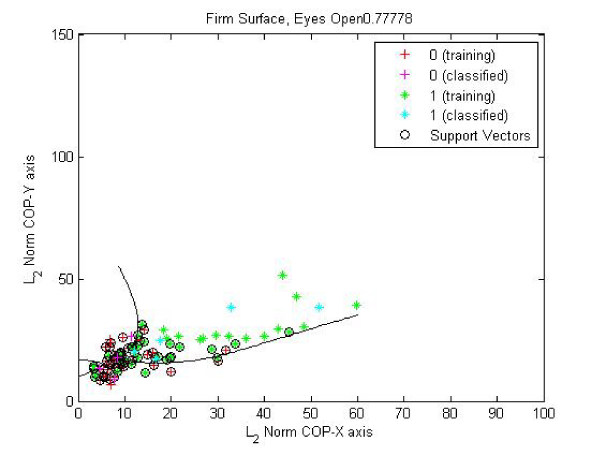
Classification with respect to medication condition and dyskinesia (SVM results) in this paper, we use 10% hold out cross validation on data for training the SVM using a polynomial kernel and employ soft margin hyper–plane for classification. A polynomial kernel function was used as it provided most accurate classification [7] for details. We performed cross–validation by randomly selecting 10% of the data as validation data set and using the rest 90% of the data for training the model. The model converged in all iterations. Success rate was used as the statistical metric to assess performance of SVM classification models. The success rate was calculated as follows: 100* (number of successful classifications) ⁄ (number of data points in validation data set). Figure 1, shows this process and the classification, for conditions A. Off medication condition is classified as “1” and on medication state is classified as “0”. The success rate of classification is approximately 64.5%, which is significant considering there is a wide range of demographics and inherent variability in the postural balance data between subjects and trials [Table 1]. Further, it is essential to note that this success rate in classification is replicated for each of the four test conditions [7]. It is widely noted that the medicine used to address Parkinson’s (levadopa) can cause tremors in the limbs resulting in dyskinesia. Some of these subjects have a tendency to demonstrate dyskinesia under medication (ON Med). This group is separated next and SVM methodology is utilized to estimate classification of subjects into those who exhibit dyskinesia and those who do not exhibit dyskinesia. The classification of subjects with dyskinesia when standing on a firm surface with eyes open is improved from 66% to 77% when considering the data related to on medication condition, as shown in Figure 2. Subjects with dyskinesia addition, EO condition, eyes open and firm surface, this difference is very significant (p=0.09) between faller and non–faller population of the subjects studied (Figure 3).
Figure 1: Svm: Training And Classification: Condition EO.
Figure 2: Svm: Training And Classification: Condition EO: Effect Of Dyskinesia: On Medication.
Data
Age(Yr)
Wt.(Kg)
Height(cm)
BOS(LxW)
Mean
61.6
171.6
82.6
26.4 x 34.9
SD
7.80
9.73
15.56
1.80 x 3.03
Min
42.8
152.6
56.2
23.6 x 26.3
Max
75.4
184.0
106.8
29.1 x 40.1
Table 1: Parkinson’s Patients: Demographics and Base of Support (BOS in cm x cm).
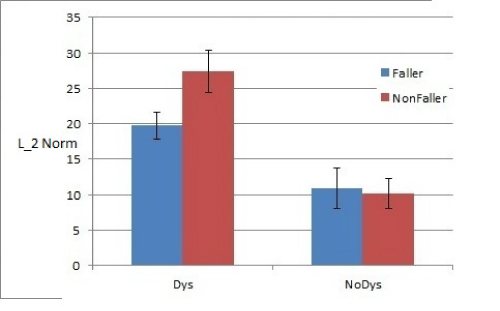
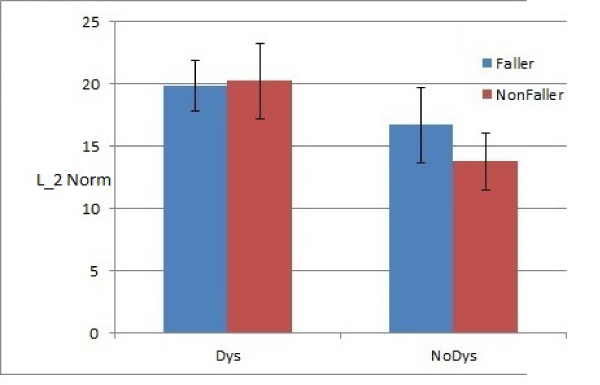
Figure 3: Comparison: Condition EO, History Of Fall: On Medication.
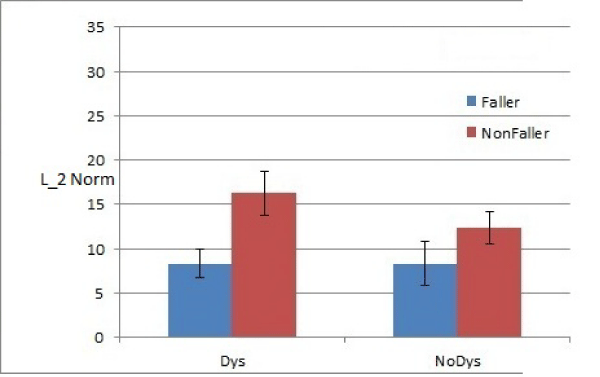
Figure 4: Comparison: Condition EO, History Of Fall: Off Medication.
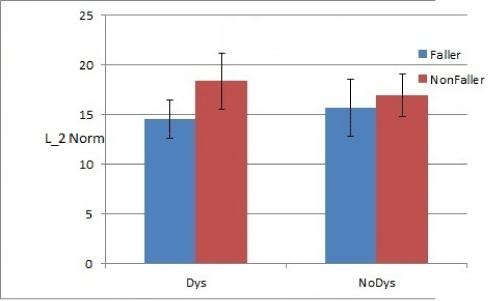
Figure 5: Comparison: Condition FO, History Of Fall: On Medication.
Figure 6: Comparison: Condition FO, History Of Fall: Off Medication.
The medication is assumed to be the primary cause of dyskinesia [11], hence as the subjects are off–medicine this difference is diminished (Figure 4). Using standard T–test, it is demonstrated that L2 norm can significantly differentiate between faller versus non–faller when tested under EO condition for subjects with no dyskinesia (p = 0.01). However, when the subjects are evaluated in condition FO, the effect of foam surface dominates. An increase in L2 norm is noticed for all subjects where most noticeable is the increase in the fallers who show dyskinesia under medicine (Figure 6). Similarly, as the subjects are taken off medication the effect of dyskinesia is eliminated and hence resulting in a drop in the corresponding L2 norm. In FO are classified as“1” and with no dyskinesia are classified as“0”. This result can be replicated for other test condition as outlined in [7]. In addition, it is observed that dyskinesia plays an essential role in altering the postural response [23].
Faller vs. non–faller PD patients with respect to L2 norm (standard T–test results) the history of fall combined with dyskinesia can provide a key insight into the postural stability of Parkinson’s subjects. To this effect, we separated fallers from non–fallers and also identified subjects who exhibited dyskinesia under medication condition. This analysis is shown in Figures (3–6). Each of the figures show means _ SEM for L2 norm for the associated test condition, dyskinesia rating and faller category. It is clear that subjects with dyskinesia have greater L2 norm as compared to subjects with no dyskinesia. In condition, ability of L2 norm to classify subjects into faller vs. non faller category is diminished for both on medication (p =0.21) and off medication conditions (p=0.47), for subjects with dyskinesia. Similartrends can be noted in the data which can be further explained if classification of subjects is done with the information regarding dyskinesia and history of falls associated with each subject.
Conclusion
Classification of postural balance data for subjects with dyskinesia and history of falls in Parkinson’s disease can be achieved using the described approach. It is noted that the classification percentage significantly improves (from 66% to 77%) if the data is separated for subjects with dyskinesia. In addition when we account for the history of falls a significant difference exists in the values of L2 norm. The result demonstrated is promising but would need to be further validated before clinical application of this technique can be fully justified. Future work related to this topic includes improving the classification accuracy by considering various features and metrics such as entropy, attractor dimension, as well as Lyapunov exponent. Long term goal of this project is to enable a diagnostic and prognostic capability for balance disorders related to Parkinson’s disease. This paper presents results which are a small step in that direction by contributing to understanding the role of test conditions and history of falls associated with the patients.
Acknowledgment
This research study was (partially) supported by the National Institute for Occupational Safety and Health Pilot Research Project Training Program of the University of Cincinnati Education and Research Center Grant T42⁄OH008432–05. In addition, this research is supported by the Miami University’s College of Engineering and Computing.
References
- Grimbergen YAM, Speelman AD, van der Marck MA, Schoon Y, Bloem BR. Gait, postural instability, and freezing. Parkinson’s disease. Olanow CW, Stocchi F, Lang AE, editors. In: Oxford: Blackwell Publishing Ltd. 2011.
- Bloem BR. Postural instability in Parkinson’s disease. Clin Neurol Neurosurg. 1992; 94: 41-45.
- LePen C, Wait S, Moutard-Martin F, Dujardin M, Ziégler M. Cost of illness and disease severity in a cohort of French patients with Parkinson’s disease. Pharmacoeconomics. 1999; 16: 59-69.
- Bloem BR, Grimbergen YA, Cramer M, Willemsen M, Zwinderman AH. Prospective assessment of falls in Parkinson’s disease. J Neurol. 2001; 248: 950-958.
- Peterka RJ. Sensorimotor integration in human postural control. J Neurophysiol. 2002; 88: 1097-1118.
- Willey C, Shukla A. L2 Norm as a Measure of Stability for a Postural Control Model. Proceedings of the 5th ASME Dynamic Systems and Controls Conference, Florida. 2012; 573-578
- Shukla A, Revilla F, Bhattacharya A. Classiication of Postural Balance in Parkinson’s Patients Using Support Vector Machines. Proceedings of the 6th IEEE/ASME Dynamics Systems and Control Conference, Stanford, CA, Oct 2013.
- Rocchi L, Chiari L, Horak FB. Effects of deep brain stimulation and levodopa on postural sway in Parkinson’s disease. J Neurol Neurosurg Psychiatry. 2002; 73: 267-274.
- Bottaro A, Yasutake Y, Nomura T, Casadio M, Morasso P. Bounded stability of the quiet standing posture: an intermittent control model. Hum Mov Sci. 2008; 27: 473-495.
- Asai Y, Tasaka Y, Nomura K, Nomura T, Casadio M. A model of postural control in quiet standing: robust compensation of delay-induced instability using intermittent activation of feedback control. PLoS One. 2009; 4: 6169.
- Nova IC, Perracini MR, Ferraz HB. Levodopa effect upon functional balance of Parkinson’s disease patients. Parkinsonism Relat Disord. 2004; 10: 411- 415.
- Horak F. Clinical Assessment of Balance Disorders. Gait and Posture 2006; 6: 76-84.
- Chung KA, Lobb BM, Nutt JG, McNames J, Horak F. Objective measurement of dyskinesia in Parkinson’s disease using a force plate. Mov Disord. 2010; 25: 602-608.
- Shumway-Cook A, Woollacott MH. Motor Control: Translating Research into Clinical Practice. New York: Lippincott, Williams and Wilkins; 2007.
- Contin M, Riva R, Baruzzi A, Albani F, Macri’ S. Postural stability in Parkinson’s disease: the effects of disease severity and acute levodopa dosing. Parkinsonism Relat Disord. 1996; 2: 29-33.
- Bhattacharya A, Morgan R, Shukla R, Ramakrishanan HK, Wang L. Non- invasive estimation of afferent inputs for postural stability under low levels of alcohol. Ann Biomed Eng. 1987; 15: 533-550.
- WWW D Umn Edu Math Technical Reports Technical Reports 2007 Tr 2009 Tr 2009 4 Pdf
- Scholkopf B, Smola A. Learning with Kernels. Cambridge: The MIT Press. 2002.
- Cristianini N, Shawe-Taylor J. An Introduction to Support Vector Machines. Cambridge: Cambridge University Press. 2000.
- Das R. A comparison of multiple classiication methods for diagnosis of Parkinson disease. Expert Systems with Applications. 2010; 37: 1568-1572
- Little MA, McSharry PE, Hunter EJ, Spielman J, Ramig LO. Suitability of dysphonia measurements for telemonitoring of Parkinson’s disease. IEEE Trans Biomed Eng. 2009; 56: 1015.
- Ozcift A. SVM feature selection based rotation forest ensemble classiiers to improve computer-aided diagnosis of Parkinson disease. J Med Syst. 2012; 36: 2141-2147.
- Armand S, Landis T, Sztajzel R, Burkhard PR. Dyskinesia-induced postural instability in Parkinson’s disease. Parkinsonism Relat Disord. 2009; 15: 359- 364.
- Revilla FJ, Larsh TR, Mani A, Duker AP, Cox C. Effect of dopaminergic medication on postural sway in advanced Parkinson’s disease. Front Neurol. 2013; 4: 202.