
Research Article
Austin J Biomed Eng. 2016; 3(1): 1034.
Temporal Response of Anterior Knee Laxity Following Strenuous Exercise
Starkel CD¹, Hawkins DA²* and Ashuckian ED³
¹Department of Mechanical and Aeronautical Engineering, University of California, USA
²Department of Neurobiology, Physiology and Behavior, University of California, USA
3Department of Biomedical Engineering, University of California, USA
*Corresponding author: Hawkins DA, Department of Neurobiology, Physiology, and Behavior, University of California - Davis, One Shields Avenue, College of Biological Sciences, USA
Received: April 27, 2016; Accepted: June 27, 2016; Published: June 29, 2016
Abstract
Routine Anterior Knee Laxity (AKL) testing of athletes can provide clinically relevant information about knee structural changes and has the potential to be prognostic for knee overuse injuries. However, for AKL to be prognostic, we must be able to discern normal AKL temporal responses following exercise from responses indicative of trauma. A Custom Knee Arthrometer (CKA) was constructed and used to quantify the temporal response and variability of AKL among thirty two young adults randomly assigned to an exercise (N=16) or control (N=16) group. Participants in the exercise group completed a 50 minute strenuous bout of lower extremity exercise. Their AKL was quantified immediately before, immediately after, every hour after for five hours, and 24 hours after the exercise. The 16 control participants were tested at similar times, but without exercising. Mean AKL did not change in the control group, but increased significantly in the exercise group (0.63 ± 0.87mm; p = 0.023) following exercise and returned to pre-exercise values within 1 hour postexercise. Individual AKL responses varied within the exercise group with two individuals (~12%) experiencing long lasting knee changes consistent with damage to knee structures. Damage accumulation may be a mechanism of non-contact Anterior Cruciate Ligament (ACL) injuries. Routine knee laxity testing using a biomedical device such as the CKA developed for this study provides a potential for detecting ACL changes and allowing sports medicine professionals to intervene to restore full ACL structural integrity and avoid damage accumulation and subsequent catastrophic rupture.
Keywords: ACL; Arthrometer; Injury prevention; Structural changes
Introduction
Injuries to the knee and specifically the Anterior Cruciate Ligament (ACL) have been described as an epidemic in youth sports. Estimates of the annual incidence of ACL injuries vary considerably, ranging from 80,000 to 250,000, with approximately 50% of these injuries occurring in athletes 15 to 25 years of age [1]. Approximately 70% of ACL injuries are non-contact in nature and occur during athletic activities that include cutting or landing tasks [2]. Non-contact ACL injuries have been studied extensively by many research groups, and there are multiple theories regarding the mechanisms of non-contact ACL injury. There is no consensus as to a single mechanism and the cause is most likely multi-factorial.
One potential mechanism of non-contact ACL injuries that could be affected by several factors (e.g. movement mechanics, anatomical structure) is overuse, defined as the repeated loading of a ligament and the subsequent mechanical breakdown characterized by a change in the ligament’s biomechanical properties such as stiffness and ultimate tensile load [3]. Repetitive submaximal loading of the ACL may cause microscopic damage to collagen fibrils or fibers, increasing the load on the remaining fibers and making the ligament more susceptible to failure [3,4]. Repetitive loading may also increase the production of inflammatory mediators and degradative enzymes which collectively may damage cells and contribute to overuse injuries [4,5]. The extent of damage sustained by the ACL in two different people performing the same repetitive task will likely vary due to individual differences in the magnitude of loading (caused by different anatomical structure and movement mechanics), and metabolic and inflammatory responses. Further, the extent of ACL damage that accumulates over multiple bouts of an activity will also vary between individuals and result in different structural changes to the ACL.
At 30 degrees of knee flexion, the ACL is the primary structural restraint to anterior translation of the tibia relative to the femur (defined as Anterior Knee Laxity (AKL)) [6,7] and therefore ACL structural changes can theoretically be quantified by changes in AKL. Clinicians exploit this idea to diagnose partial and complete tears of the ACL by performing various knee laxity tests. However, to our knowledge, no one has attempted to longitudinally use knee laxity testing to screen athletes for knee structural changes that could be prognostic of future catastrophic ACL injury.
For AKL to be prognostic for ACL injury, the resolution of the AKL measurement must be sufficient to detect clinically meaningful knee structural changes and the normal AKL day-to-day fluctuations and responses to exercise must be understood. The fact that some orthopaedic and sports medicine doctors can detect partial ACL tears from knee laxity exams, provides evidence that AKL measurement has the potential to provide clinically relevant longitudinal information about knee structural changes. We believe that we can resolve knee laxity changes of 0.5 mm and that this resolution has clinical significance. We can expect that a person having a normal knee laxity of 5 mm who performs activities that lead to 10% damage of the ACL cross sectional area without compromising the material properties of the remaining intact ACL would have a 10% increase in AKL. The AKL change would be larger if the material properties were also compromised in response to the activity. Recognition of the accumulation of 10% or more damage to an ACL can be clinically important and lead to intervention programs that reduce the incidence of non-contact ACL injuries.
To our knowledge, only six published studies have reported the temporal response of AKL following exercise [8-13]. These studies reported varying times ranging from 52 minutes to 5 hours for AKL to recover to pre-exercise values following exercise. Some of these studies briefly mentioned, but without explanation, that there were varied individual temporal responses not reflective of the mean response. Additional research to further characterize the temporal response of AKL post-exercise is needed to explore the potential for using AKL to detect subtle damage to knee structures that could potentially be prognostic for ACL injury.
The goal of this study was to determine if routine AKL screening has the potential to detect subtle knee changes reflective of damage accumulating in knee structures such as the ACL. The intent was not to quantify damage to specific knee structures, as this would be very challenging to do in-vivo, but rather to determine if AKL changes occur that are consistent with knee structural changes, and thus if more expensive and longitudinal studies to track AKL changes and ACL injuries are warranted.
We pursued three aims in this study. First, we tested the hypothesis that AKL increases during strenuous exercise in young adults. Results from this aspect of the study were compared to results from similar studies performed by others to demonstrate the validity of our AKL testing device and testing procedures. Second, we quantified the temporal response of AKL to strenuous exercise. This study provides improved time resolution of AKL measurements compared to previous studies and thus enhances our understanding of the temporal response of AKL following exercise. Third, we explored the variability in AKL changes and recovery times among young adults completing a strenuous bout of exercise to determine if any of the response were consistent with structural damage (i.e. AKL does not return to pre-exercise values). We hypothesized that a percentage of young adults who complete a strenuous bout of lower extremity exercise will experience lasting knee laxity changes consistent with subtle damage to knee structures.
Methods
Participants
Physically active, male and female, college-aged students 18-25 years of age participated in this study. Participants were excluded from participation if they were an intercollegiate athlete, a competitive club sport athlete, were sedentary, or had any injury or health condition that would prevent them from completing one hour of strenuous exercise. Participants were also excluded from the study if they had any previous knee injuries or had been diagnosed by a health care professional as being hypermobile.
Testing apparatus
All knee laxity measurements were made with a Custom Knee Arthrometer (CKA) developed in our institution’s Human Performance Laboratory (Figure 1). Commercially available knee arthrometers were evaluated prior to the start of this study and their resolution and precision were deemed inadequate for this study. Thus, the CKA was developed and used. The CKA was designed to acquire real time anterior and posterior force deformation data and consists of two force transducers (LC101-100 S Beam Load Cell, Omega Inc, Stamford, CT – accuracy, precision and resolution better than 0.62 N, 0.16 N, and 0.60 N respectively), two string potentiometers (SP1- 4 String Pot, Celesco, Chatsworth, CA - accuracy, precision and resolution better than 0.43mm, 0.11mm, and 0.20mm, respectively), a data acquisition laptop, a custom Lab VIEW virtual interface, and a rack and pinion force application system.
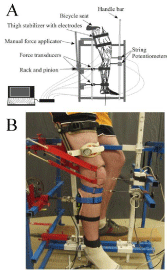
Figure 1: Schematic of the Custom Knee Arthrometer (CKA) (A) and typical
set up of a participant in the device (B), illustrating the force transducers,
string potentiometers, force application system and data acquisition laptop.
Test-retest variability of the device was assessed using data collected from 16 subjects. The intra-rater Intraclass Correlation Coefficient (ICC) [3,1] calculated for the CKA was 0.87. In contrast, the ICCs calculated for the KT 1000 (MED metric Corporation, San Diego, CA), a common device used to measure knee laxity, have ranged from 0.47 to 0.84 [14-19]. With an ICC of 0.87, the reliability of the knee arthrometer used in this study is appropriate for the aims of this study.
Testing protocol
The study was approved by our Institutional Review Board and prior to testing, written informed consent was obtained from all participants. Right knee AKL was measured for 32 participants (16 exercise, 16 controls) immediately before, immediately after, and every hour after the exercise session for five hours. A final laxity measurement was made approximately 24 hours post-exercise. Participants in the control group followed the same knee testing procedure and timeline, but did not participate in the exercise session. After the exercise session and between AKL testing sessions, participants were asked to work at a desk and allowed to walk briefly.
During AKL testing using the CKA, the participant sat on a bicycle seat with their right thigh constrained and several sensors (force transducers and string potentiometers) attached to their lower leg (Figure 1). Participants sat with their torso upright and their thigh securely strapped to a thigh support that maintained the knee in a position of 30 degrees of flexion (0 degrees being full extension). Before strapping the thigh to the thigh support, surface electrodes were applied to the skin over the vastus medialis and biceps femoris to monitor and collect Electromyogram (EMG) data. Prior to application of the electrodes, the skin was shaved (if necessary), abraded, and cleaned with an alcohol swab. Two cuffs attached to force transducers were then secured to the lower leg. Both transducers were positioned on the posterior aspect of the lower leg aligned perpendicular with the long axis; one attached approximately 10 cm distal of the knee, and the other attached just above the ankle. The lower leg was not supported vertically, thus creating a traction force at the knee, but was constrained by the ankle cuff in a horizontal plane. After securing the force transducers to the subject’s lower leg, the thigh strap was tightened until the subject felt constrained, but not to the point of discomfort.
After securing the thigh straps and force transducers, the string potentiometers were positioned and attached. The patellar brace was first centered over the participant’s patella and held firmly against the femoral condyles so that any motion of the brace represented movement of the condyles. The location of the brace was marked on the subject’s knee ensuring that the position could be replicated for all subsequent tests. The femur and tibial tuberosity string potentiometers were then secured to the attachment sites and adjusted so that the strings were parallel. After the subject was secured in the knee arthrometer, bicycle seat height and horizontal and vertical positions of the thigh constraint and force transducers were recorded to ensure the subject’s position in the device was consistent for all tests.
In each test, the lower leg was cyclically loaded 20 times while force and displacement were recorded. Cyclic anterior-posterior forces (200 N anterior and 50 N posterior) were manually applied via the rack and pinion system to the upper portion of the lower leg while the ankle was constrained. Each loading cycle was completed in approximately 2 seconds. Both the force applied to the upper leg and the force acting at the restraint just above the ankle were recorded with force transducers. The string potentiometers recorded the displacement of the femur and tibia in response to the loading.
Knee laxity was determined from the force and displacement data. The resultant horizontal force acting in structures of the knee (e.g. bones, ligaments, tendons) was equal to the sum of the forces recorded by the two force transducers. The displacement of the tibia relative to the femur was determined as the difference between the displacements of the tibial tuberosity and femoral condyles as recorded by the string potentiometers. The force-deformation response of the knee was plotted and anterior knee laxity for each cycle was calculated as the relative displacement of the tibia when the resultant force was 133 N, a common value used in various commercial knee laxity testing devices. The output of the CKA was the average anterior laxity value that was calculated for the final ten cycles.
Exercise protocol
The exercise group performed a 50 minute strenuous exercise protocol adapted from the Prevent Injuries and Enhance Performance (PEP) Program [20]. All exercise sessions were supervised by the researchers and took place on athletic fields at our institution. During the exercise session, subjects performed a 10 minute warmup, 10 minutes of strengthening exercises, 15 minutes of plyometric exercises, and 15 minutes of agility exercises. During the warmup, participants lightly jogged for 5 minutes and then performed five minutes of static and dynamic stretching exercises. During the strengthening, plyometric, and agility exercises, the subjects were asked to perform as many repetitions as possible in the allotted time period. Strengthening exercises included single leg toe raises, squats, walking overhead lunges, burpees, and skaters. Plyometric exercises included cone hops, squat jumps, tuck jumps, jumping rope, and mountain climbers. Agility exercises included a shuttle run with forward/backward running, a diagonal run, a weaving run (grapevine), cutting maneuvers, a square run, a bounding run, and a one-leg ladder drill.
The exercise session consisted of self-perceived high intensity efforts with brief periods of rest interspersed. Participants were instructed to perform at maximal intensity for each exercise. Extra rest was allowed if the subject requested it or was having difficulty completing the exercises at a high intensity level.
Statistical analysis
A mixed effects repeated measures ANOVA with an a priori significance level of 0.05 was used to determine the effects of exercise and time on AKL. Post hoc Dunnet’s method was used to make comparisons between the mean pre-exercise AKL (baseline) and all subsequent AKL measurements. All statistical analyses were performed using SAS software (Version 8, SAS Institute Inc., Cary, NC).
Results
Subject data
Participants were recruited into one of two groups for this study, controls (N=16, 8 females and 8 males) and exercise (N=16, 6 females and 10 males). All measurements were acquired by a single evaluator. Participants in the exercise and control groups averaged 21 (range 19-25) and 21 (range 18-25) years of age, respectively, with average masses of 67.7 ± 8.1 and 73.6 ± 13.5 kg, respectively, and heights of 172.2 ± 8.6 and 171.7 ± 9.0 cm, respectively (Table 1).
Controls (N=16)
Height (cm)
Mass (kg)
Age (years)
Mean
171.7
73.6
20.9
SD
9
13.5
1.8
Minimum
154.4
58.4
18
Maximum
187
98.2
25
Exercise Subjects (N=16)
Height (cm)
Mass (kg)
Age (years)
Mean
172.2
67.7
21.4
SD
8.63
8.1
1.9
Minimum
159
50.4
19
Maximum
187
82.9
25
Table 1: Descriptive data for study participants including height, mass and age.
Knee laxity data - Group results
Mean group laxity values did not vary with time for the control group, but were increased immediately post-exercise followed by a subsequent recovery for the exercise group (Figure 2). Group mean laxity values increased significantly from 3.39 ± 1.40 mm pre-exercise to 4.02 ± 1.10 mm immediately post-exercise (p = 0.023) in the exercise group (Figure 3). There was not a statistically significant difference between the pre-exercise and 1 hour or later post-exercise laxity values, indicating that mean anterior knee laxity had returned to its pre-exercise, baseline condition within one hour post-exercise.
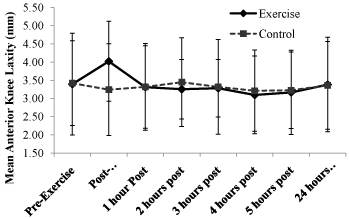
Figure 2: Temporal response of mean anterior knee laxity at 133 N for the
control and exercise groups. Mean group laxity values did not vary with
time for the control group, but increased than decreased post-exercise for
the exercise group. By one hour post-exercise, the exercise group’s mean
anterior knee laxity returned to the baselinepre-exercise condition.
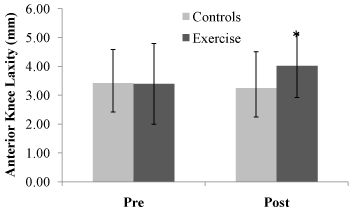
Figure 3: Mean (+ 1 std dev) Anterior Knee Laxity (AKL) for the control group
and the exercise group pre- and immediately post-exercise. The exercise
group demonstrated significantly increased laxity post-exercise (post-pre:
0.63 mm) compared to the control group (post-pre:-0.18 mm), *p<0.01. There
was no significant difference in AKL between the control and exercise groups
pre-exercise.
Knee laxity data - individual results
There were individual variations in knee laxity for both the control and exercise groups. The average standard deviation in knee laxity across time for individuals within the control group was 0.39 mm. For the exercise group, while mean anterior knee laxity increased with exercise and then returned to baseline within one hour post-exercise, there was a large variation in the temporal response among participants (Figure 4). Of the 16 exercise participants, 8 were termed ‘Increased Laxity’ (IL) responders and elicited the anticipated temporal response (increased laxity immediately post-exercise with an eventual return to baseline, pre-exercise laxity values). The remaining 8 exercise participants had varied temporal responses (defined as any response other than an immediate increase in laxity post-exercise followed by a return to baseline within the 5 hour testing window) and were termed ’Varied Laxity’ (VL) responders (Figure 5A-5C).
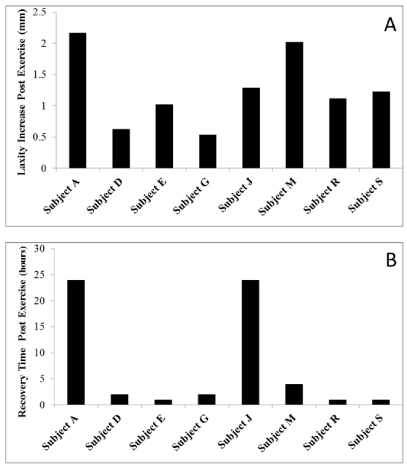
Figure 4: Of the “Increase Laxity” (IL) responders (N=8), there was a large
variation in the laxity increase (A) and recovery time post-exercise (B). The
mean increase immediately post-exercise was 1.25 mm or 63%, (SD = 0.59
mm, Range: 0.54 to 2.17 mm). 37.5% of the IL responders recovered within
1 hour post-exercise, another 25% recovered within 2 hours, another 12.5%
recovered within 5 hours, and the remaining 25% recovered by 24 hours postexercise.

Figure 5: Varied Anterior Knee Laxity (AKL) responses of the “Varied Laxity”
(VL) responders (N=8) following exercise. Three participants demonstrated
a decrease in laxity immediately post-exercise (A), three participants
demonstrated an increase in laxity immediately post-exercise, but then
recovered to laxity values below their pre-exercise condition (B), and two
participants had laxity values that increased immediately post-exercise but
did not recover within 24 hours (C).
Discussion
We found a significant increase in mean anterior knee laxity immediately post-exercise, supporting the results of previous studies and providing evidence that our testing device and methods are consistent with other methods described in the literature. To document normal fluctuations in laxity values throughout the day and identify laxity changes associated with exercise, a control group that did not participate in the exercise session was included in the testing protocol. Similar to results of other studies using control participants [2], no significant change in mean laxity was noted over the 24 hour testing period.
To our knowledge, only six published studies have attempted to quantify the recovery of knee laxity following exercise [8-13]. Stoller et al. reported an average torsional knee laxity increase of 14% following a 30 minute run, with an average recovery time of 52 minutes post-exercise [12]. Weisman et al. reported that valgus laxity increased between 7.4% and 22.8% (depending on the sport) following participation in basketball, downhill skiing, hockey, or soccer and that the laxity values returned to pre-exercise levels within 1 hour [13]. Johannsen et al. reported an average increase of 16% (1.4 mm) in anterior knee laxity immediately post-exercise and found that laxity values had not recovered when measured 30 minutes postexercise [8]. Nawata et al. reported an average increase of 33% (2.1 mm) in anterior knee laxity following a 30 minute run and found that laxity returned to the pre-exercise level within 1 hour post exercise [9]. Sakai et al. reported an average 47% increase (2.2mm) in anterior knee laxity following a 150 minute game style basketball practice. They found that the increased laxity returned to the pre-exercise level within 5 hours post-exercise, however laxity was only measured at 90 minutes post-exercise and again at 5 hours [11]. Nicholettos et al. reported an average 13.9% increase (1.0mm) in anterior knee laxity following open kinetic chain knee extensor exercise. The increased knee laxity did not return to baseline within 90 minutes post-exercise [10]. All six of these studies reported a significant increase in knee laxity immediately post exercise compared to baseline. We also found a significant increase in knee laxity immediately post exercise. Further, in agreement with previous work, excluding Sakai et al. and Nicholettos et al, we found that mean anterior knee laxity returned to pre-exercise levels within 1 hour post-exercise.
There were varied knee laxity temporal responses following exercise that are of considerable interest. Other investigators have noted varied knee laxity temporal responses following exercise, but they have given little recognition or attention to these responses. Steiner et al. reported that three knees in three basketball players and six knees in five distance runners demonstrated a decrease in total anterior-posterior laxity after exercise (average decrease, 0.5 cm or 9%) [21]. Sakai et al. reported an increase in laxity immediately postexercise, with mean laxity values at 5 hours post-exercise notably lower (1.6 mm) than the baseline, pre-exercise values [11].
Of the 16 exercise participants tested, 8 had a Varied Laxity (VL) response following exercise and 8 had the expected Increased Laxity (IL) response then recovery to pre-exercise levels. Of the VL responders, 3 demonstrated a decrease in laxity immediately postexercise (consistent with findings by Steiner et al.), 3 demonstrated an increase in laxity immediately post-exercise, but then recovered to laxity values below their pre-exercise condition (consistent with findings by Sakai et al.), and 2 had laxity values that increased immediately post-exercise but did not recover within 24 hours. The percentage of participants who had increased knee laxity that remained 24 hours after exercise (~12%, 2 of 16) is consistent with our hypothesis that a percentage of young adults who complete a strenuous bout of lower extremity exercise will experience lasting knee laxity changes consistent with subtle damage to knee structures.
We explored the effects of age, gender, anthropometrics, exercise intensity, fitness level, and outside temperature during the exercise session and found no differences between the VL and IL groups that could account for the varied laxity responses. These results highlight the varied temporal response of knee laxity following exercise, which represent the resultant effect of several possible responses (e.g. differences in creep recovery time, synovial fluid shifts, inflammation, chemical imbalances leading to fluid retention in muscle, hormone effects, muscle activation changes, and damage) that can vary between individuals. Determination of the exact mechanisms for the VL responses was beyond the scope of this study. However, the fact that there were VL responses consistent with knee structural changes that could be due to damage provides evidence that further investigation in this area is warranted. These results also highlight the importance of establishing a standard knee laxity measurement protocol that considers past activity and time if knee laxity is to be used as a prognostic tool for ACL injury.
While this study improves our understanding and resolution of the temporal response of AKL following exercise, addressing certain limitations and assumptions associated with both the measurement system and exercise protocol could improve future studies of the same nature. While the CKA was shown to have an intraclass correlation coefficient comparable to that of the KT-1000, this comparison was conducted on different subjects and with different testers, therefore limiting our ability to objectively compare the two devices. However, the ICC results for our device and tester provide evidence that the reliability of our testing was sufficient for the objectives of this study. Additional testing, such as x-ray imaging or cadaveric studies are necessary to truly evaluate the accuracy and precision of any knee laxity device. In addition to limitations associated with the measurement system, the exercise protocol introduced a few limitations and variables that were not explicitly accounted for in the analyses. The varied fitness levels of the participants resulted in large variations of intensities and effort levels. Participants were instructed to complete each exercise with maximal effort, however this was not monitored or controlled using heart rate data. Our intent was to identify the range of laxity changes that occur following intense training, but are not confident that we received an intense effort from all participants. Future testing on the effects of exercise on knee laxity may benefit from having a controlled exercise protocol such as a treadmill session where speed and time may be kept consistent between participants. While no correlations were found between the perceived intensity level and amount of laxity increase or recovery time, it is worthwhile to explore these relationships with a larger participant population and an objective, quantifiable exercise intensity level protocol. We did not evaluate the subjects’ leg strength or fitness level, but it would also be useful to explore the relationships between these quantities and knee laxity temporal responses.
Conclusion
In conclusion, a total of 32 participants, 16 exercise and 16 controls were tested to quantify the temporal response of the participants’ right knee laxity and explore the hypothesis that a percentage of young adults who complete a strenuous bout of lower extremity exercise will experience lasting knee laxity changes consistent with subtle damage to knee structures. In agreement with previous work, AKL did not change in the control group, but did change over time in the exercise group. The exercise group demonstrated a mean increase in AKL following exercise of 0.63 mm. Mean AKL returned to its baseline, pre-exercise value within 1 hour post-exercise. There were varied individual knee laxity temporal responses following exercise with some subjects experiencing laxity changes lasting longer than 24 hours, consistent with subtle damage to knee structures. We do not know if ACL damage actually occurred in these individuals, but the results are consistent with such a theory and warrant further investigation. The next logical step is to use imaging techniques to try and detect subtle trauma to the ACL in subjects who elicit a lasting knee laxity increase following strenuous exercise. Knee laxity measurements provide an exciting potential as a prognostic tool for ACL injury that is worthy of further exploration.
References
- Griffin LY, Albohm MJ, Arendt EA, Bahr R, Beynnon BD, Demaio M, et al. Understanding and preventing noncontact anterior cruciate ligament injuries: a review of the Hunt Valley II meeting, January 2005. Am J Sports Med. 2006; 34: 1512-1532.
- Hewett TE, Ford KR, Hoogenboom BJ, Myer GD. Understanding and preventing acl injuries: current biomechanical and epidemiologic considerations - update 2010. N Am J Sports Phys Ther. 2010; 5: 234-251.
- Jung HJ, Fisher MB, Woo SL. Role of biomechanics in the understanding of normal, injured, and healing ligaments and tendons. Sports Med Arthrosc Rehabil Ther Technol. 2009; 1: 9.
- Wang JH, Iosifidis MI, Fu FH. Biomechanical basis for tendinopathy. Clin Orthop Relat Res. 2006; 443: 320-332.
- Jelinsky SA, Lake SP, Archambault JM, Soslowsky LJ. Gene expression in rat supraspinatus tendon recovers from overuse with rest. Clin Orthop Relat Res. 2008; 466: 1612-1617.
- Butler DL, Noyes FR, Grood ES. Ligamentous restraints to anterior-posterior drawer in the human knee. A biomechanical study. J Bone Joint Surg Am. 1980; 62: 259-270.
- Woo SL, Hollis JM, Adams DJ, Lyon RM, Takai S. Tensile properties of the human femur-anterior cruciate ligament-tibia complex. The effects of specimen age and orientation. Am J Sports Med. 1991; 19: 217-225.
- Johannsen HV, Lind T, Jakobsen BW, Krøner K. Exercise-induced knee joint laxity in distance runners. Br J Sports Med. 1989; 23: 165-168.
- Nawata K, Teshima R, Morio Y, Hagino H, Enokida M, Yamamoto K. Anterior-posterior knee laxity increased by exercise. Quantitative evaluation of physiologic changes. Acta Orthop Scand. 1999; 70: 261-264.
- Nicholettos A, Barcellona MG, Morrissey MC. The immediate effects of open kinetic chain knee extensor exercise at different loads on knee anterior laxity in the uninjured. Knee. 2013; 20: 500-504.
- Sakai H, Tanaka S, Kurosawa H, Masujima A. The effect of exercise on anterior knee laxity in female basketball players. Int J Sports Med. 1992; 13: 552-554.
- Stoller DW, Markolf KL, Zager SA, Shoemaker SC. The effects of exercise, ice, and ultrasonography on torsional laxity of the knee. Clin Orthop Relat Res. 1983; 172-180.
- Weisman G, Pope MH, Johnson RJ. Cyclic loading in knee ligament injuries. Am J Sports Med. 1980; 8: 24-30.
- Hanten WP, Pace MB. Reliability of measuring anterior laxity of the knee joint using a knee ligament arthrometer. Phys Ther. 1987; 67: 357-359.
- Highgenboten CL, Jackson A, Meske NB. Genucom, KT-1000, and Stryker knee laxity measuring device comparisons. Device reproducibility and interdevice comparison in asymptomatic subjects. Am J Sports Med. 1989; 17: 743-746.
- Malcom LL, Daniel DM, Stone ML, Sachs R. The measurement of anterior knee laxity after ACL reconstructive surgery. Clin Orthop Relat Res. 1985; 35-41.
- Rowe A1, Wright S, Nyland J, Caborn DN, Kling R . Effects of a 2-hour cheerleading practice on dynamic postural stability, knee laxity, and hamstring extensibility. J Orthop Sports Phys Ther. 1999; 29: 455-462.
- Sailors ME, Keskula DR, Perrin DH. Effect of running on anterior knee laxity in collegiate-level female athletes after anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther. 1995; 21: 233–239.
- Wiertsema SH, van Hooff HJ, Migchelsen LA, Steultjens MP . Reliability of the KT1000 arthrometer and the Lachman test in patients with an ACL rupture. Knee. 2008; 15: 107-110.
- Gilchrist J MB, Melancon H, Ryan GW, Silvers HJ, Griffin LY, Watanabe DS, et al. A randomized controlled trial to prevent noncontact anterior cruciate ligament injury in female collegiate soccer players. Am J Sports Med. 2008; 36: 1476–1483.
- Steiner ME, Grana WA, Chillag K, Schelberg-Karnes E. The effect of exercise on anterior-posterior knee laxity. Am J Sports Med. 1986; 14: 24-29.