
Case Report
Austin J Cancer Clin Res 2015;2(4): 1040.
Metaplastic Gastric Mucosa Mimicking a Gastric Heterotropia in a Small Intestine of Patient Presenting with Recurrent Subocclusive Episodes
Gupta P¹, Shabnam N¹, Tiwari N¹, Mahendru V² and Srivastava AN¹*
¹Department of Pathology, Era’s Lucknow Medical College & Hospital, India
²Department of Surgery, Era’s Lucknow Medical College & Hospital, India
*Corresponding author: Srivastava AN, Department of Pathology, Era’s Lucknow Medical College & Hospital, Lucknow, India.
Received: June 15, 2015; Accepted: June 30, 2015; Published: July 04, 2015
Introduction
Heterotropia means presence of normal tissue at an abnormal position. Abnormal embryological development presents as congenitally present heterotrophic tissue. Gastric heterotropia are mostly seen in duodenum but very rarely in small intestine [1]. Isolated cases of heterotopic gastric mucosa have been reported at all levels of the alimentary tract from the oesophagus to the rectum. Gastric heterotropias commonly occur in duodenum, esophagus and rectum but presence of heterotrophic tissue rest in ileum and jejunum is a very rare finding. Metaplasia is a change in one type of fully developed tissue to another differentiated tissue usually due to sustained inflammation and its complication [2]. It may either be acquired metaplasia as in Barrett’s esophagus or a true gastric heterotropia of congenital origin as in Meckel’s Diverticulum. The biggest diagnostic confusion is of a simple true congenital gastric heterotropia being misdiagnosed as a gastric metaplasia [3].
A patient with heterotropias might present with a spectrum of symptoms, from asymptomatic to ulcers in to intestinal obstructions. Intussusception, perforation, bleeding and pain are common complications with heterotropias. Generally gastric heterotropias are flat lesions with mild plate like elevations that are missed radiologically [4]. We report a case of a 40 year old male who presented with subacute intestinal obstruction. He was diagnosed as a case of focal ileal gastric heterotropia as a cause of this partial obstruction.
Case Presentation
A 40 yr old male presented to the emergency with acute abdominal pain and inability to pass stool or flatus. On examination his abdomen was soft on palpation and rapid bowel sounds were heard on auscultation. His PR examination showed empty rectum. His vitals and other systems were within normal limits. The patient was taken up for emergency exploratory laparotomy under GA. On opening the bowel, strictures and adhesion in a part of small intestine was seen and a segment was sent for histopathology. All his other blood investigations were within normal limits. Unfortunately no USG findings were available as this was a case of emergency laparotomy. Grossly a segment of small intestine was received (Figure 1). Cut surface shows focal sharply marginated slightly elevated area with haphazard convoluted thickened mucosal rugosities different from surrounding intestinal mucosa which shows transverse well oriented grayish white mucosal rugosities. Lumen proximal to this was dilated with partially atrophied mucosa. Histopathologically, section from the lumen showed scattered mucinous glands both above and below the muscularis mucosa surrounded by irregularly oriented smooth muscle cells. Overlying mucosa showed partially flattened villi lined by columnar cells with scattered goblet cells (Figures 2a,2b). Dense chronic inflammatory infiltrate was seen extending up the muscularis layer. Focal areas showed dilated lymphatics and congested blood vessels (Figure 3). These glands below the muscularis were PAS positive and Alcian blue negative, which confirmed the neutral mucin in these glands suggesting a foveolar epithelium of gastric mucosa (Figures 2c,2d). Overlying small intestinal mucosa showed goblet cells with Alcian blue positivity (Figure 2c). No gastric glands or chief cells or parietal cells were seen. A diagnosis of Ectopic gastric foveolar mucosa was made as a cause of stricture with intestinal obstruction. Therefore it was concluded that this gastric mucosa was of metaplastic etiology.
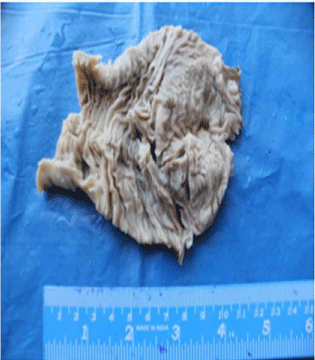
Figure 1: Intestine show circumscribed foci of haphazardly arranged
convoluted gastric type mucosa.
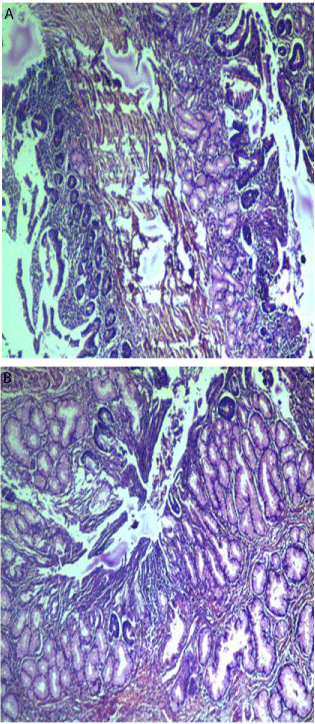
Figure 2a,2b: Lobules of mucinous glands lying below the small intestinal
epithelium.
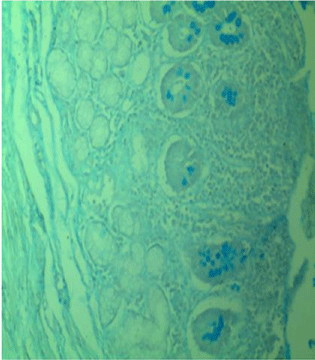
Figure 2c: Alcian blue negative mucinous glands.
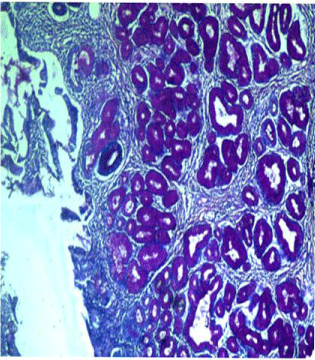
Figure 2d: PAS positive mucinous glands.
Discussion
Gastric heterotropia of the intestinal tract is an occasional, incidental, gross or microscopic finding at surgery or autopsy. It is most frequently seen as an acquired metaplastic change resembling antral mucosa in response to inflammatory bowel diseases such as regional enteritis [3]. The biology of this entity has been charecterised as hyperplasia of primitive gut epithelium overtime [5]. It is very important to differentiate a benign heterotropia from a metaplastic change, which is the biggest pitfall in the diagnosis of heterotropias, which a pathologist is faced with in daily practice.
Gastric heterotropias have been commonly seen in esophagus as inlet patches, duodenum, gallbladder, Meckel’s diverticulum etc [6]. Heterotropias are simply developmental anomalies. Heterotropic gastric tissue consists of full thickness of specialized gastric glands comprising chief cells, parietal cells and foveolar epithelium. A heterotropia presents as perfect tissue island, a metaplasia involves partial thickness of tissue and they intermingle with native tissue as is seen in our case favouring a metaplastic tissue [7].
Embryological development of esophagus and stomach occurs at approximately the 4th week of gestation. The esophagus gets divided into the ventral respiratory portion and the dorsal food pipe. The stomach develops as a saccular fusiform structure which undergoes rotation as it develops. Developmental errors in the above steps lead to heterotropias [8]. Wacrenier et al. and Soule explained the origin of heterotropias by elucidating that these arise from the primitive gut epithelium, which becomes separated from the primordial stomach and undergoes hyperplasia overtime due to unknown reasons. Origin of heterotropias from the metaplasia of pluripotent endodermal cells of foregut has been proposed by Skandalakis et al. Vitellointestinal duct has also been proposed as site of origin in a study by Abel et al. Ability of endodermal cells to undergo hyperplasia in the gut due to physical movement of gastric epithelia have also been proposed as a cause.IHC shows p21, p27 and cyclin D all cell cycle regulators to be positive in foveolar epithelium [9].
The cause of gastric heterotropia is unknown but it most likely represents a developmental error since, embryologically, the epithelium of the esophagus, stomach, and small bowel is derived from morphologically similar cells. The stimulus for differentiation and proliferation of these cells into a mucosa typical for a distinct and different region of the gastrointestinal tract is unknown [3]. In a study done by Carlei et al. metabolic and functional activity of gastric heterotrophic mucosa regarding production of acid and mucin is identical to that of normal gastric mucosa [10,11].
A metaplasia is an acquired condition where a change in one type of mature epithelium to another takes place. The biggest diagnostic dilemma faced is in differentiating a metaplasia an abnormal regenerative process as exemplified by pyloric metaplasia where we see group of fundic glands from a heterotropia [12]. However in this case we could not find a fully developed fundic mucosa.
Conclusion
Gastric heterotropia is one of the confusing diagnoses for a pathologist as differentiating it from a metaplasia is a challenge. Discussion of such a rare but important entity and better methods of confirmatory diagnosis is the need for the hour.
References
- Lambert MP, Heller DS, Bethel C. Extensive gastric heterotopia of the small intestine resulting in massive gastrointestinal bleeding, bowel perforation and death: report of a case and review of the literature. Pediatr Dev Pathol. 2000; 3: 277-280.
- Bhattacharya B, Jakate S, Saclarides TJ, Keshavarzian A. Gastric heterotopia presenting as a mass in jejunum. Arch Pathol Lab Med. 2003; 127: 506-507.
- Nawaz K, Graham DY, Fechner RE, Eiband JM. Gastric heterotopia in the ileum with ulceration and chronic bleeding. Gastroenterology. 1974; 66: 113-117.
- Smithuis RH, Vos CG. Heterotopic gastric mucosa in the duodenal bulb: relationship to peptic ulcer. AJR Am J Roentgenol. 1989; 152: 59-61.
- Philip A, Varnholt H, Michael V, Prasad R, Moriarty KP. Giant polypoid gastric heterotopia of the jejunum presenting with intermittent intussusception. J Laparoendosc Adv surg Tech. 2007; 17: 120-124.
- Steele SR, Mullenix PS, Martin MJ, Ormseth E, Weppler E, Graham J, et al. Heterotopic gastric mucosa of the anus: a case report and review of the literature. Am Surg. 2004; 70: 715-719.
- Mann NS, Mann SK, Rachut E. Heterotopic gastric tissue in the duodenal bulb. J Clin Gastroenterol. 2000; 30: 303-306.
- Srinivasan R, Loewenstine H, Mayle JE. Sessile polypoid gastric heterotopia of rectum: a report of 2 cases and review of the literature. Arch Pathol Lab Med. 1999; 123: 222-224.
- Martínez A, Decanini-Terán O, Soria-Céspedes D. Polypoid and hyperplastic heterotopic gastric mucosa in the jejunum as a cause of recurrent subocclusive episodes. Ann Gastroenterol. 2013; 26: 184.
- Kestemberg A, Mariño G, de Lima E, Garcia FT, Carrascal E, Arredondo JL. Gastric heterotopic mucosa in the rectum with Helicobacter pylori-like organisms: a rare cause of rectal bleeding. Int J Colorectal Dis. 1993; 8: 9-12.
- Carlei F, Pietroletti R, Lomanto D, Barsotti P, Crescenzi A, Pistoia MA, et al. Heterotopic gastric mucosa of the rectum--characterization of endocrine and mucin-producing cells by immunocytochemistry and lectin histochemistry. Report of a case. Dis Colon Rectum. 1989; 32: 159-164.
- Lessells AM, Martin DF. Heterotopic gastric mucosa in the duodenum. J Clin Pathol. 1982; 35: 591-595.