
Case Report
J Cardiovasc Disord. 2016;3(1): 1024.
Multimodality Imaging of Left Ventricular Non- Compaction Cardiomyopathy Associated with Situs Inversus
Aradhya M, Manda Y, Vefali H, Agrawal S, Singh A, Sinha A and Shirani J*
Department of Cardiology, University of St. Luke’s University Health Network, USA
*Corresponding author: Shirani J, Department of Cardiology, University of St. Luke’s University Health Network, 801 Ostrum Street, Bethlehem, PA 18015, USA
Received: May 23, 2015; Accepted:November 27, 2016; Published: January 21, 2016
Abstract
Left Ventricular Non-Compaction Cardiomyopathy (LVNC) is characterized by hypertrabeculation and intratrabecular recesses. It has been mostly reported as an isolated entity, however, 1 in 8 cases of LVNC has been associated with various congenital heart defects. Whether such an association is genetically based or triggered by altered hemodynamic factors remains unsettled. We report a unique case of LVNC associated with situs inversus (dextrocardia with mirror image major visceral organs) in an adult. The patient’s clinical presentation (heart failure, left ventricular apical thrombus, atrial fibrillation and thromboembolic stroke) mandated a multimodality imaging approach to diagnosis and management. The role of cardiovascular imaging in evaluation of this complex heart disease is discussed.
Keywords: Left ventricular non-compaction; Situs inversus; Contrast echocardiography; Multimodality cardiac imaging
Introduction
Left Ventricular (LV) Non-Compaction Cardiomyopathy (LVNC) is a relatively rare cardiac disease characterized by prominent ventricular trabeculations and deep intertrabecular recesses on the luminal surface of the LV [1]. It is speculated that the ventricular hypertrabeculation is the result of intrauterine developmental arrest of the normal compaction process of the myocardium during the first trimester leading to the formation of a compacted and a noncompacted layer of myocardium. LVNC is considered to be a distinct primary genetic cardiomyopathy that can lead to systolic heart failure, thromboembolism, malignant arrhythmias and sudden cardiac death [2]. Although LVNC is often reported as an isolated entity, it has also been associated with other inherited and congenital heart diseases particularly Ebstein anomaly, aortic coarctation, tetralogy of Fallot, and uni- or bicuspid aortic valves [3,4]. We present a unique case of LVNC associated with situs inversus presenting with heart failure, left ventricular apical thrombus, atrial fibrillation and thromboembolic stroke studied by multimodality imaging.
Case Report
A 40-year-old man with known situs inversus presented with a 4 week history of worsening shortness of breath, palpitation and lower extremity edema. Physical examination showed signs of biventricular heart failure. Vital signs on presentation included: heart rate144 bpm, blood pressure 106/61 mmHg, respiratory rate 26 per minute and oxygen saturation 92% on 4 liters of oxygen via nasal cannula. Auscultation of the heart revealed irregular rhythm and no murmur. A right-sided 12-lead electrocardiogram showed atrial fibrillation with a rapid ventricular response (~170 bpm) and non-specific ST segment and T wave changes (Figure 1A). Chest X-ray showed dextrocardia and cardiomegaly, pulmonary venous congestion and bilateral pleural effusions (Figure 1B). Initial laboratory tests showed markedly increased liver enzymes and D-dimer (2310 ng/mL) as well as an elevated cardiac troponin I. Computed tomography of the chest with contrast showed situs inversus, cardiomegaly, and bilateral pleural effusion (Figures 2A and 2B). Transthoracic Echocardiogram (TTE) without and with contrast demonstrated a dilated Left Ventricle (LV) with moderately to severely reduced systolic function due to global hypokinesis, evidence of LVNC and large, partially mobile thrombiat the LV apex (Figures 3A,3B). The right ventricle was also dilated with reduced systolic function. No significant valvular disease was seen. After the initial management including anticoagulation, diuresis and rate control, normal sinus rhythm was resumed. Cardiac Magnetic Resonance (CMR) imaging then confirmed presence of LVNC involving the mid to distal anterior, septal and apical walls with complete resolution of apical thrombi (Figures 2C,2D). Invasive coronary angiography showed no significant obstructive disease and LV angiography demonstrated typical features of LVNC. Hospital course was complicated with cerebrovascular accident and acute renal injury with complete recovery. He was discharged with plans for follow up at the heart failure clinic and consideration of an implantable cardioverter defibrillator. A repeat contrast-enhanced TTE showed resolution of apical thrombi (Figure 3C). His family history was significant for premature coronary artery disease. There was no family history of heart failure, sudden cardiac death or congenital heart disease.
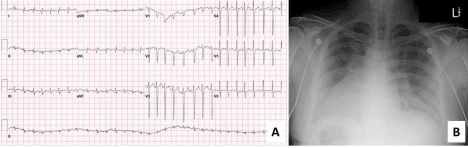
Figure 1: (A) ECG using right-sided chest leads shows atrial fibrillation
with rapid ventricular response, low voltage in limb leads, and late R wave
transition across percordial leads. (B) Portable anteroposterior chest x-ray
showing dextrocardia, pulmonary venous congestion, and right-sided gastric
air bubble consistent with situs inversus.
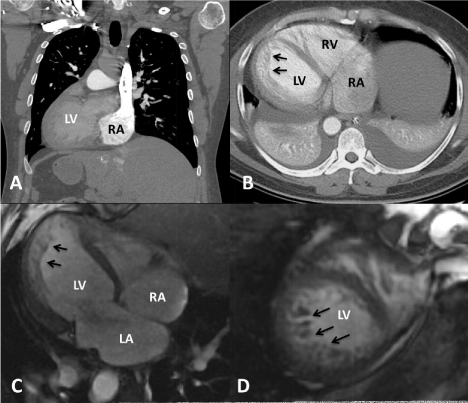
Figure 2: Chest computed tomography showing dextrocardia with situs
inversus on the sagittal view (A), and a dilated left ventricle with evidence of
non-compaction (arrows) on an axial view (B). Cardiac magnetic resonance
imaging also showed marked apical hypertrabeculations (arrows) consistent
with left ventricular non-compaction in long (C) and short (D) axis views.
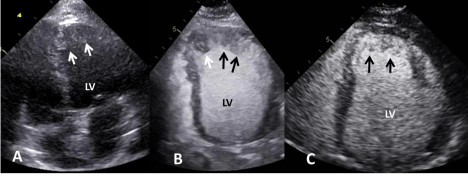
Figure 3: Transthoracic echocardiogram on admission (A,B) showing apical
thrombi (white arrows) and hypertrabeculation (black arrows) on unenhanced
(A) and contrast-enhanced (B) apical 4-chamber views. Follow up contrastenhanced
transthoracic echocardiogram showed resolution of apical thrombi
after anticoagulation and delineation of apical hypertrabeculation (arrows) in
an apical 4-chamber view (C).
Discussion
LVNC is now recognized as a genetic disease of the heart that can manifest itself as an isolated entity or in association with congenital cardiac anomalies [5]. The prevalence of LVNC in adults referred for echocardiography has ranged from 0.05% to 0.26% [3]. In one series, 12% of patients with LVNC had associated congenital cardiac defects including various forms of LV outflow tract abnormalities, Ebstein anomaly, tetralogy of Fallot, and double outlet right ventricle [4]. Despite such reports, it is yet unclear whether the association between LVNC and congenital heart disease is genetically based. In fact, some have speculated that abnormal hemodynamic characteristics during fetal life may be in part responsible for the development of LVNC in some patients with congenital heart defects [6]. In addition, the LVNC phenotype may at time be transiently manifested in highly-trained athletes, in patients with sickle cell anemia, and during pregnancy and may resolve completely after removal of the hemodynamic burden [7-9]. In the adult population, an association between LVNC and dextrocardia with situs solitus (dextroversion) has been reported in a 46 year old man with multiple cerebrovascular accidents [10] and in a 76 year old woman with dyspnea [11]. To our knowledge, an association between LVNC and situs inversus (dextrocardia with mirror image major visceral organs) has been only reported once before [12]. The latter, a 53 year old man with sinus node disease and LV systolic dysfunction was evaluated with TTE and transesophageal echocardiography and CMR imaging. Our patient presented with heart failure, LV apical thrombus, suspected pulmonary embolism, LV wall motion abnormality and cerebrovascular accident necessitating a multimodality imaging approach to anatomic and functional cardiac evaluation. Echocardiography, particularly when performed with contrast is an effective technique for diagnosis of LVNC [13]. In our experience, contrast echocardiography allows accurate delineation of the compacted and non-compacted myocardium obviates the need for color Doppler evaluation and allows clear identification of LV apical thrombi. In recent years, however, CMR imaging has significantly contributed to the accuracy of diagnosis of LVNC due to its superior resolution and recent establishment of unique imaging protocols and strict diagnostic criteria [14].
References
- Chin TK, Perloff JK, Williams RG, Jue K, Mohrmann R. Isolated noncompaction of left ventricular myocardium. A study of eight cases. Circulation. 1990; 82: 507-513.
- Maron BJ, Towbin JA, Thiene G, Antzelevitch C, Corrado D, Arnett D, et al. Contemporary definitions and classification of the cardiomyopathies: an American Heart Association Scientific Statement from the Council on Clinical Cardiology, Heart Failure and Transplantation Committee; Quality of Care and Outcomes Research and Functional Genomics and Translational Biology Interdisciplinary Working Groups; and Council on Epidemiology and Prevention. Circulation. 2006; 113: 1807-1816.
- Towbin JA, Lorts A, Jefferies JL. Left ventricular non-compaction cardiomyopathy. Lancet. 2015; 386: 813-825.
- Stähli BE, Gebhard C, Biaggi P, Klaassen S, Buechel EV, Attenhofer Jost CH, et al. Left ventricular non-compaction: prevalence in congenital heart disease. Int J Cardiol. 2013; 167: 2477-2481.
- Towbin JA. Inherited cardiomyopathies. Circ J. 2014; 78: 2347-2356.
- Bartram U, Bauer J, Schranz D. Primary noncompaction of the ventricular myocardium from the morphogenetic standpoint. Pediatr Cardiol. 2007; 28: 325-332.
- Gati S, Chandra N, Bennett RL, Reed M, Kervio G, Panoulas VF, et al. Increased left ventricular trabeculation in highly trained athletes: do we need more stringent criteria for the diagnosis of left ventricular non-compaction in athletes? Heart. 2013; 99: 401-408.
- Gati S, Papadakis M, Niekerk NV, Reed M, Yeghen T, Sharma S. Increased left ventricular trabeculation in individuals with sickle cell anaemia: physiology or pathology? Int J Cardiol. 2013; 168: 1658-1660.
- Gati S, Papadakis M, Papamichael ND, Zaidi A, Sheikh N, Reed M et al. Reversible de novo left ventricular trabeculations in pregnant women: implications for the diagnosis of left ventricular noncompaction in low-risk populations. Circulation. 2014; 130: 475-483.
- Friedman MA, Wiseman S, Haramati L, Gordon GM, Spevack DM. Noncompaction of the left ventricle in a patient with dextroversion. Eur J Echocardiogr. 2007; 8: 70-73.
- Baskurt M, Kalyoncuoglu M, Kucukoglu S. Noncompaction cardiomyopathy and dextroversion of the heart. Herz. 2011; 36: 33-36.
- Gonçalves LF, Souto FM, Faro FN, Mendonça Rde C, Oliveira JL, Sousa AC. Dextrocardia with situs inversus associated with non-compaction cardiomyopathy. Arq Bras Cardiol. 2013; 101: e33-36.
- Lampropoulos KM, Dounis VG, Aggeli C, Iliopoulos TA, Stefanadis C. Contrast echocardiography: contribution to diagnosis of left ventricular noncompaction cardiomyopathy. Hellenic J Cardiol. 2011; 52: 265-272.
- Choudhary P, Hsu CJ, Grieve S, Smillie C, Singarayar S, Semsarian C, et al. Improving the diagnosis of LV non-compaction with cardiac magnetic resonance imaging. Int J Cardiol. 2015; 181: 430-436.