Abstract
Background: Children with Autism Spectrum Disorders (ASD) are at particular risk of impairment in social interaction, repetitive and stereotyped behaviors, and a poor quality of life. We tested whether applied behavior analysis intervention could, compared to a control condition, reduce repetitive and stereotyped behaviors, and increase social skills and thus enhance the quality of life among children with ASD.
Methods: Thirty children with ASD (mean age: 6.5 years) were randomly assigned either to applied behavior analysis intervention or to a control condition. All participants completed Gareth test on stereotypical behaviors, social communication, and interaction skills at the following time points: baseline, and six months later at completion of the intervention.
Findings: Stereotypical behaviors, social communication, and interaction skills improved over time from baseline to intervention completion, but more so in the applied behavior analysis intervention than in the control group. Compared to the control group, the applied behavior analysis intervention group reported had more positive scores.
Conclusion: The findings suggest that among children with ASD and compared to a control condition, applied behavior analysis intervention has the potential to improve symptoms of autism, thus contributing to their quality of life.
Keywords: Children; Autism spectrum disorder; Applied behavior analysis; Social skills; Stereotyped behavior
Introduction
Autism Spectrum Disorders (ASD) is a developmental disorder characterized by impairments in social interaction and communication, and behavioral deficits and limited behavioral patterns [1]. Moreover, people with ASD are likely to show a variety of comorbid disorders, including attention deficit and hyperactivity (ADHD), mental and motor retardation, and depression [2,3]. Further, children with ASD show delay in social, language, and symbolic game developments compared to healthy children. The global mean prevalence of ASD in the general population is 10 cases per 10 thousand and the diagnosis is most often made in child age. Moreover, recent study on the prevalence of ASD showed 1 in every 100 births [4].
Compared to the general population, children with ASD have shown behavior deficits such as stereotyped movements, aggression, and self-harm [5]. Further, they are in trouble for understanding and using the rules of social behavior [6,7], interactive gestures and non-verbal behavior [8-10], and motor coordination [9]. High or low sensitivity to auditory, olfactory, tactile, and visual stimuli has often been reported in children with ASD [11]. In addition, children with ASD have a more impaired motor function and are also less physically active than healthy children [12].
Further and based on previous studies, varieties of interventional programs have been used in promoting social development, and decreasing maladaptive behaviors in children with ASD. According to Green and colleagues [13] and Hess and colleagues [14], there are many approaches such as diets and vitamins, speech therapy, and music therapy in reduction of ASD symptoms. Some of these treatments or intervention programs have some positive effects on the development of children with ASD. Multimodal treatments including medication [15], physical activity interventions [16], sensory integration training [17], antidepressants, counseling, physical and occupational therapy are typically employed to alleviate the symptoms of ASD. However, although Applied Behavioral Analysis (ABA) intervention is commonly recommended [18], research regarding their potential as an alternative or add-on treatments is still in an early stage. ABA is derived of principles of behavior therapy, such as operant conditioning. ABA is the framework of a three-term contingency of operant conditioning, which includes the events that precede behavior, the behavior itself, and the stimuli that follow the behavior.
To decrease autistic symptoms, O Lovaas, T Smith and J McEachin [19] developed ABA training in people with ASD with parents engagement, and showed this technique has positive impacts on autistic symptoms. Participation of family members in the program is very important and the essential element of ABA technique [19]. For example, some studies found the effeteness of ABA intervention with parents engagement in children with ASD [20]. Furthermore, Anderson and colleagues showed that ABA training had a positive effect on children with ASD and they showed that more and sustained recovery was created in children who were trained for two years [21]. Previous studies found the positive effects of ABA training on children with ASD for 6 consecutive months compared with the control group. The results showed that this method was effective on symptoms of ASD in these children. However, in the some study, stereotypical behaviors, and social skills were not measured [22]. Therefore, the present study is aimed at behaviors and social skills as output.
In children with ASD, inadequate environmental stimuli and interventional programs were reported as the main reason for social development delays, reduced social engagement and poor behavior skills. Although previous studies have been conducted to improve these skills among children with ASD [14,22,23], further research is needed to determine the effects of intervention programs specifically regarding social and behavioral deficits. Additionally, knowledge of behavioral impairments of children with ASD is important for psychologists and occupational therapists. Most importantly, longterm interventions in children with ASD have been neglected in most studies and usually treatment methods were periodically and in the short-term. Moreover, in most studies children with ASD were not prepared to enter to schools after the intervention [22]. Accordingly, the main purpose of the present study was to examine the effects of a 6-months ABA training on stereotyped behaviors, and social skills in a sample of children with ASD, compared to a control condition.
The following two hypotheses were tested. First, based on previous research [23], we expected that participation in ABA training would be associated with a decrease in stereotypical behaviors over time compared to a control condition. Second, on the basis of previous studies [23] we expected that ABA training would lead to an increase in social skills over time compared to a control condition.
We believe that the ABA training intervention has the potential to help psychologists, parents and coaches improve social skills and motor control of children with ASD.
Method
Participants
A total of 30 children with ASD (mean age: 6.5 years; SD=2.17) took part in the present study. Inclusion criteria were: (1) children diagnosed with ASD; (2) age between 4 and 8 years; (3) a diagnosis of poor motor coordination (based on Movement Assessment Battery (MAB) criteria; Manual dexterity total ≤22), (4) the ability to follow a minimum of two-step instructions; (5) Getting a score from 75 to 115 in Gilliam Autism Rating Scale (GARS), (6) the ability to walk 10 meters without assistance and (7) parents signed written informed consent. Exclusion criteria were: (1) neuromusculoskeletal disorders or severe sensory impairments; (2) intake of arousal medications or substances; (3) orthopedic problems (orthopedic surgery one year before intervention); (4) injection of botulism toxin 6 months before intervention; (5) uncorrected visual impairment and (6) absenteeism in educational sessions (more than 2 sessions).
Procedure
Participants’ parents were fully informed about the aims and the procedure of the study, and the anonymous data handling. They all signed the written informed consent sheet and children gave their assent (verbally or by gesture) to participate in the present study. At baseline, stereotypical behaviors and social communication were tested. Next, the participating children were randomly assigned to one of the following conditions: 1) ABA training, and 2) control condition. The intervention lasted 6 months including three training sessions per week. Participants’ stereotypical behaviors and social communication were tested immediately after completion of the intervention (Figure 1). The Review Board of the Islamic Azad University (Urmia, Iran) approved the study, which was performed in accordance with the ethical principles laid down in the seventh and current edition (2013) of the Declaration of Helsinki.
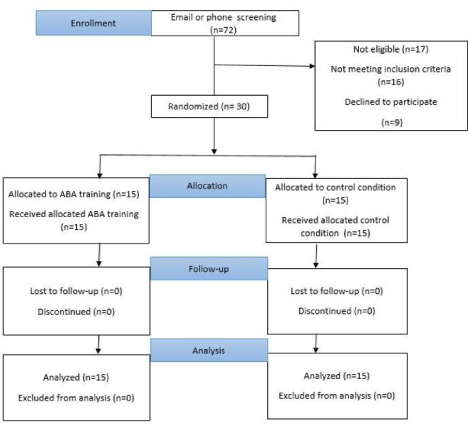
Figure 1: CONSORT participant flow diagram.
Instruments
Gilliam Autism Rating Scale (GARS): GARS test has been developed based on the definitions of Autism Society of America and the Psychiatric Association of America based on guidance from the statistical diagnostic manual of mental disorders. GARS have four sub-scales. Each subscale consists of 14 items. The first subscale is stereotype behavior that contains 1 to 14 items. This subtest describes cases of stereotyped behaviors, movement disorders, and strange behavior. The second sub-scale, which is communication skills, includes items 15 to 28. These items describe verbal and nonverbal behavior that signs of autism. Social interaction is the third sub-scale that includes statements 29 to 42. The items of this subscale assess the matters that can properly explain the events for the public. The fourth subscale is a developmental disorder that includes items 43 to 56. GARS test is suitable for people aged 3 to 22, which can be completed by parents and professionals at school or home. Studies indicate Cronbach Alpha of 90% for stereotypes behavior, 89% for communications, 93% for social interaction, 88% for developmental disorders, and 96% for symptoms of autism. The validity of the Persian version of this test is verified through comparison with different tests. based on Ahmadi and colleagues (2011) Cronbach’s alpha test in terms of stereotype behaviors, communication, social interaction, and developmental issues is, respectively 74%, 92%, 73%, 80%, and 89% for the overall reliability [24].
Intervention
The present intervention design was based on previous research [19,25]. At the beginning, basic adaptive skills towards language behavior, non-verbal and verbal skills, and imitation were considered. Then a basis is created for playing games using toys. After children have learned these skills, the second stage had started which was focused on teaching expressive language skills, short and simple word use, and interactive games with peers. Over time, the interventional programs were extended to homes and schools for 30 hours a week [26]. Applied behavior change was implemented based on individual training. Moreover, strengthening ABA changes was considered as one of the very important elements of this behavioral program. Based on children’s abilities, the intervention was considered according to four main steps: 1. introduction of behaviors, 2. skills behavior, 3. generalizing behavior, and 4. distinguishing behavior. In this perspective, training has begun by offering materials and educational content and then continues using the media and education or training program. In the next stage, children were guided to respond, and in the last stage, the children have received the outcome based on the answers provided. We have focused on learning in ABA intervention. The ABA reduced the probability of incorrect answers to a very low level. We have used several methods of guiding, reducing, and gradual reduction of guidance to reduce incorrect answers, and ultimately, reduces the overall capacity to respond incorrectly.
The control condition session was designed as an active control condition. Children assigned to the control condition met two times per week in small groups of six to nine participants for 6 consecutive months (duration: 45-60 minutes per session). During the meetings, children engaged in socio-therapeutic group events such as playing board games and checking blood pressure, which was organized by social workers and psychologists from the same hospital center.
Data analysis
Analyses of Variance (ANOVA) for repeated measures were performed with the factors Time (baseline, study end), Group (ABA training vs. controls), and Time by Group interaction, with stereotypical behaviors, social communication, and interaction skills as dependent variables. Post-hoc analyses were performed using Bonferroni corrections for p-values. Due to deviations from sphericity, the repeated measures ANOVAs were performed using Greenhouse- Geisser corrected degrees of freedom, though the original degrees of freedom are reported with the relevant Greenhouse-Geisser epsilon value (ε). For the interpretation of the ANOVAs, Cohen’s d effect sizes were reported. Effect sizes can be evaluated as trivial (0-0.19), small (0.20-0.49), medium (0.50-0.79) and large (≥0.80) (Cohen, 1992). The level of significance was set at p ≤0.05 across all analyses, and all statistics were processed using SPSS® 21.0 (IBM Corporation, Armonk, N.Y., USA) for Apple McIntosh®.
Results
All 40 children with ASD completed the baseline, and postintervention data assessment. All 15 children assigned to the intervention group participated in the planned 6 months of ABA training, and all 15 children assigned to the control condition participated in the 6 month control sessions. Table 1 provides an overview of the descriptive statistics for the outcome variables (autistic symptoms), separately for the intervention and control group, and the three measurement occasions (baseline, post-intervention). Furthermore, in Table 1, the results of the rANOVAs are displayed to examine whether the assessed outcome variables in the two groups develop differently.
Groups
Factors
ABA
Control
Group
Time
Time x Group interaction
N
15
15
M (SD)
M (SD)
F
ηp2
F
ηp2
F
ηp2
Stereotype behavior
24.96**
0.59
***133.49
0.61
38.51**
0.6
Baseline
31.30 (3.49)
29.60 (2.91)
Post-intervention
20.40 (3.77)
29.50 (3.02)
Communications symptoms
5.71*
0.31
29.11*
0.61
5.71*
0.66
Baseline
34.50 (2.01)
33.50 (1.95)
Post-intervention
29.50 (3.02)
31.70 (2.07)
Interactive behavior
42.62**
0.45
51.41**
0.51
34.05*
0.36
Baseline
30.40 (4.94)
34.10 (2.74)
Post-intervention
20.10 (6.19)
34.10 (2.76)
Note: ABA: Applied Behavior Analysis. Degrees of freedom: Group: (1, 17), Time: (1, 18), Time × Group (1, 38). *p<0.05. **p<0.01. ***p<0.001.
Table 1: Descriptive statistics for autism symptoms, separately for groups (ABA and control) and for each measurement point (baseline and post-intervention) and tests for time x group interaction effects.
Stereotype behaviors
Across the sample as a whole, the rANOVA revealed that stereotype behaviors decreased from baseline to study completion (significant Time effect; see Table 1). However, as shown by the significant Time by Group interaction, the significant effect of Time was primarily due to a reduction in stereotype behaviors in the ABA group, whereas scores remained nearly unchanged in the control group across all measurement time points (Figure 2). Effect size calculations (Cohen’s ds) showed that in the ABA group stereotype behavior scores declined substantially from baseline to post-intervention (large effect: d=0.93). Within the control group, stereotype behavior scores remained nearly unchanged from baseline to post-intervention (d=0.06). Effect size calculations comparing means of the ABA and the control group showed that stereotype behaviors scores were similar in the intervention and the control group at baseline (d=0.04), whereas the groups significantly differed at post-intervention (large effect: d=0.97).
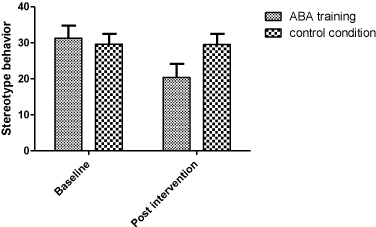
Figure 2: Stereotypes in the study groups at baseline and post-intervention.
Communications symptoms
As highlighted in Table 1, the rANOVA yielded that across the sample as a whole, communications symptoms decreased from baseline to post-intervention (significant Time effect). There was a marked increase in communications symptoms in the ABA group, whereas scores remained relatively unchanged in the control group. Accordingly, a significant Time by Group interaction was identified (Figure 3). Effect size calculations showed that within the ABA group, communications symptoms scores decreased substantially from baseline to post-intervention (large effect: d=0.88). Within the control group, communications symptoms scores remained nearly unchanged from baseline to post-intervention (d=0.10). Effect size calculations comparing means of the ABA and the control group showed that communications symptoms were similar in the intervention and the control group at baseline (d=0.05), whereas the groups significantly differed at post-intervention (large effect: d=0.92).
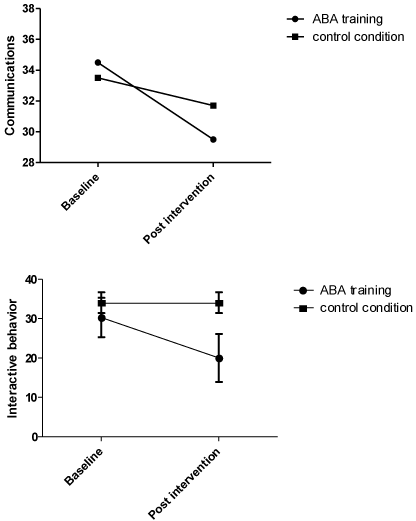
Figure 3: Above: The communication deficits in the study groups at baseline
and post-intervention. Below: The interactive behavior deficits in the study
groups at baseline and post-intervention.
Interactive behavior
The rANOVA points out that across the sample as a whole, interactive behavior symptom scores decreased from baseline to post-intervention (Figure 3). However, the significant Time effect was primarily due to a reduction in symptom severity in the ABA group; the scores of the control group remained at a similar level from baseline. Effect size calculations showed that within the ABA group, interactive behavior symptom scores decreased substantially from baseline to post-intervention (large effect: d=0.91). Within the control group, interactive behavior scores remained nearly a from baseline to post-intervention (d=0.06). Effect size calculations comparing means of the ABA and the control group showed that communications symptoms were similar in the intervention and the control group at baseline (d=0.09), whereas the groups significantly differed at post-intervention (large effect: d=0.89).
Discussion
The key findings of the present study were that among children with Autism Spectrum Disorders (ASD) a course of ABA lasting for 6 months reduced stereotype behaviors and autistic symptoms and improved social skills, compared to a control condition. The present findings add to the current literature in an important way in that ABA proved to be successfully applied to children with ASD. Such findings are relevant because children with ASD are at increased risk for depression and deprivation of school and to our knowledge, no thorough programs or consoling have so far been established for this specific problem to facilitate attending school.
Tow hypotheses were formulated, and each of these will now be considered. Our first hypothesis was that, compared to a control condition, ABA would reduce stereotypical behaviors over time, and this expectation was fully confirmed. Our second hypothesis anticipated similarly that, compared to a control condition, an ABA intervention would lead to reductions in social deficits. Moreover, this hypothesis was supported. The present results therefore concur with numerous previous studies [19,25,27].
The present study showed that an ABA method has positive effects on interactive behaviors, behavioral stereotypes, and communication skills. This finding is in accordance with K Bottema-Beutel, H Park and SY Kim [28] and G Green [29] findings which were concluded that undergoing ABA training has a positive impact on autistic behavior. Moreover, on the other hand, these findings contradict the findings of M Dionne and R Martini [30] about the role of game and education in children with ASD. In the same vein, Williams, Reddy, and Costall (2001) has been claimed that the implementation of intervention based on game might help in improving ASD symptoms.
The present finding also showed ABA intervention might improve behavior and social deficits. This finding is consistent with the findings of SL Harris and L Delmolino [31] about the effect of ABA on improving the performance of children with ASD. It is further consistent with the results of VK Jensen and LV Sinclair [32] in the treatment of children with ASD through ABA interventions at an early age.
The interpretation of the effectiveness of ABA training can be considered to be the type of intervention. There is evidence that children with ASD do not have sufficient ability to express their inner feeling and experiences verbally. Therefore, ABA training, which emphasizes the non-verbal consciousness of the body, game and physical activity and is performed by the active trainer and trainee, might be more beneficial to these individuals, compared to other verbal interventions such as psychological counseling. Most psychological counseling emphasizes verbal intervention. However, in the ABA training, using non-verbal techniques can have more effect on the behavior and social deficits aspects of children with ASD.
In general terms, our research allowed us to build on previous results, where it is considered that parental involvement in the therapeutic process can be of great help in increasing social and communication skills in children diagnosed with ASD.
Conclusion
Among children with ASD who have attended into the school, ABA had positive impacts on stereotypical behaviors, social communication, and interaction skills, when compared to a control condition. Our findings are important because children with ASD are at increased risk of developing psychological disorders, and because the study provides a viable means of facilitating the school attending of children with ASD.
References
- Bell CC. DSM-IV: diagnostic and statistical manual of mental disorders. Jama. 1994; 272: 828-829.
- Matson JL, Smith KR. Current status of intensive behavioral interventions for young children with autism and PDD-NOS. Research in Autism Spectrum Disorders. 2008: 2: 60-74.
- Wing L, Gould J, Gillberg C.Autism spectrum disorders in the DSM-V: better or worse than the DSM-IV? Research in developmental disabilities. 2011; 32: 768-773.
- Flamgan K. Drawing connections with autism. Dissertation]. America: Emporia State University. 2011.
- Watling RL, Dietz J. Immediate effect of Ayres’s sensory integration-based occupational therapy intervention on children with autism spectrum disorders. American Journal of Occupational Therapy. 2007; 61: 574-583.
- Wing L. Asperger’s syndrome: a clinical account. Psychological medicine. 1981; 11: 115-129.
- Wing L. Manifestations of social problems in high-functioning autistic people. In: High-functioning individuals with autism. Springer. 1992: 129-142.
- Ehlers S, Gillberg C. The epidemiology of Asperger syndrome: A total population study. Journal of child psychology and psychiatry. 1993; 34: 1327- 1350.
- Gillberg IC, Gillberg C. Asperger syndrome-some epidemiological considerations: a research note. Journal of child psychology and psychiatry. 1989; 30: 631-638.
- Szatmari P, Bremner R, Nagy J. Asperger’s syndrome: a review of clinical features. The Canadian Journal of Psychiatry. 1989; 34: 554-560.
- Dunn W, Myles BS, Orr S. Sensory processing issues associated with Asperger syndrome: A preliminary investigation. American Journal of Occupational Therapy. 2002; 56: 97-102.
- Rogers SJ, Ozonoff S. Annotation: What do we know about sensory dysfunction in autism? A critical review of the empirical evidence. Journal of Child Psychology and Psychiatry. 2005; 46: 1255-1268.
- Green VA, Pituch KA, Itchon J, Choi A, O’Reilly M, Sigafoos J. Internet survey of treatments used by parents of children with autism. Research in developmental disabilities. 2006; 27: 70-84.
- Hess KL, Morrier MJ, Heflin LJ, Ivey ML. Autism treatment survey: Services received by children with autism spectrum disorders in public school classrooms. Journal of autism and developmental disorders. 2008; 38: 961- 971.
- Manning-Courtney P, Murray D, Currans K, Johnson H, Bing N, Kroeger- Geoppinger K, et al. Autism spectrum disorders. Current problems in pediatric and adolescent health care. 2013; 43: 2-11.
- Ruggeri A, Dancel A, Johnson R, Sargent B. The effect of motor and physical activity intervention on motor outcomes of children with autism spectrum disorder: A systematic review. Autism. 2020; 24: 544-568.
- Schoen SA, Lane SJ, Mailloux Z, May-Benson T, Parham LD, Smith Roley S, et al. A systematic review of ayres sensory integration intervention for children with autism. Autism Research. 2019; 12: 6-19.
- Busch AJ, Webber SC, Brachaniec M, Bidonde J, Dal Bello-Haas V, et al. Exercise therapy for fibromyalgia. Current pain and headache reports. 2011; 15: 358.
- Lovaas O, Smith T, McEachin J. Long-term outcome for children with autism who received early intensive behavioral treatment. American Journal on Mental Retardation. 1993; 94: 359-372.
- Green G. Early behavioral intervention for autism: What does research tell us? 1996.
- Anderson SR, Avery DL, DiPietro EK, Edwards GL, Christian WP. Intensive home-based early intervention with autistic children. Education and treatment of children. 1987; 10: 352-366.
- Mohseni Ejiyeh A, Abedi A, Behnamnejad N. Effectiveness of Applied Behavior Analysis (ABA) for children with autism spectrum disorders in Iran, 2005-2013: a meta-analysis. Iranian Journal of Psychiatry and Clinical Psychology. 2015; 21: 17-25.
- Gonzalez-Aguero A, Vicente-Rodriguez G, Moreno LA, Guerra-Balic M, Ara I, Casajus JA. Health-related physical fitness in children and adolescents with Down syndrome and response to training. Scand J Med Sci Sports. 2010; 20: 716-724.
- Ahmadi S, Safari T, Hemmatian M, Khalili Z. The psychometric properties of Gilliam autism rating scale (GARS). Research in Cognitive and Behavioral Sciences. 2011; 1: 87-104.
- Virués-Ortega J: Applied behavior analytic intervention for autism in early childhood: Meta-analysis, meta-regression and dose–response metaanalysis of multiple outcomes. Clinical psychology review 2010, 30(4):387- 399.
- Corsello CM: Early intervention in autism. Infants & Young Children 2005, 18(2):74-85.
- Mohammadzaheri F, Koegel LK, Rezaee M, Rafiee SM: A randomized clinical trial comparison between pivotal response treatment (PRT) and structured applied behavior analysis (ABA) intervention for children with autism. Journal of autism and developmental disorders 2014, 44(11):2769-2777.
- Bottema-Beutel K, Park H, Kim SY: Commentary on social skills training curricula for individuals with ASD: Social interaction, authenticity, and stigma. Journal of autism and developmental disorders 2018, 48(3):953-964.
- Green G: Behavior analytic instruction for learners with autism: Advances in stimulus control technology. Focus on autism and other developmental disabilities 2001, 16(2):72-85.
- Dionne M, Martini R: Floor time play with a child with autism: A single-subject study. Canadian Journal of Occupational Therapy 2011, 78(3):196-203.
- Harris SL, Delmolino L: Applied behavior analysis: Its application in the treatment of autism and related disorders in young children. Infants & Young Children 2002, 14(3):11-17.
- Jensen VK, Sinclair LV: Treatment of autism in young children: Behavioral intervention and applied behavior analysis. Infants & Young Children 2002, 14(4):42-52.
