
Special Issue - Coronary Artery Disease
Austin J Clin Cardiolog. 2021; 7(2): 1077.
The Effects of Combined Same Session Aerobic and Resistance Training on Physical Performance in Coronary Artery Disease Patients: Protocol Comparison
Clavario P1, Barbara C1, Porcile A1, Russo C1, Zappulla T1, Capurroa E1, Cornero T1, Ferrari Aggradi C1, Mäkikallio T3 and Hautala AJ2,3*
¹Cardiac Rehabilitation Center of Genoa, Azienda Sanitaria Locale, ASL 3 Genovese, Genoa, Italy
²Faculty of Sports and Health Sciences, University of Jyväskylä, Finland
³Cardiovascular Research Group, Division of Cardiology, Oulu University Hospital, University of Oulu, Finland
*Corresponding author: Hautala AJ, Faculty of Sports and Health Sciences, University of Jyväskylä, PO Box 35, FI-40014 University of Jyväskylä, Finland
Received: May 25, 2021; Accepted: June 12, 2021; Published: June 19, 2021
Abstract
Aerobic training is included to cardiac rehabilitation programs together with resistance training. The effects of combined aerobic and resistance training performed in a same session with different protocols on peak aerobic capacity (VO2peak) and maximal dynamic strength (1RM: one repetition maximum) are not well known. We compared the effectiveness of two different combined aerobic and resistance training programs for 12 weeks performed three times in a week in stable Coronary Artery Disease (CAD) patients (n=30) who had previously performed aerobic training only. The patients were randomized to High Volume- Low Intensity Group (HLG) or Low Volume-High Intensity Group (LHG). Both groups performed laboratory controlled aerobic exercise first (60min, 80% of lactate threshold) followed by six major muscle group resistance exercises (HLG: 30-35% of 1RM, 3 sets, 12 repetitions) or (LHG: 60-70% of 1RM, 3 sets, 6 repetitions). VO2peak remained at the baseline level for whole study group (23 ± 6 vs. 24 ± 7 ml·kg-1·min-1, p=0.380) and the responses did not differ between the HLG and LHG (p=0.891). Muscle strength increased when analyzed as one group for both upper (Push Up; 24 ± 8 vs. 30 ± 7 kg, p <0.0001) and lower body (Leg Extension; 20 ± 6 vs. 27 ± 6 kg, p <0.0001) with no difference between subgroups (p=0.240 and p=0.504, respectively). As conclusion, combined aerobic and resistance training in the same training session for 12 weeks improved maximal strength independently of the intensity of resistance training. These results highlight the importance of regular resistance training, even at moderate intensity, for CAD patients in terms of physical performance and independent living.
Keywords: Coronary heart disease; Combined aerobic and resistance training; Rehabilitation
Abbreviations
VO2peak: Peak Aerobic Capacity; 1RM: One Repetition Maximum; CAD: Coronary Artery Disease; HLG: High Volume-Low Intensity Group; LHG: Low Volume-High Intensity Group; CR: Cardiac Rehabilitation; NYHA: New York Heart Association Functional Classification; RPE: Perceived Ratings of Exertion
Introduction
A comprehensive patient-tailored Cardiac Rehabilitation (CR) programs have shown to improve the patient’s physical, psychological and social condition [1,2]. Multidisciplinary CR approach focuses on patient education, nutritional counseling, modification of the risk factors, psychosocial management, individually tailored exercise training and the overall well-being of patients [3-5]. Exercise as a main component in CR reduces cardiac mortality, hospital readmission [6,7], anxiety [8] and has shown to be cost-effective for health care [9]. Therefore, exercise-based CR should be referred to an early program [10] soon after the discharge for patients with acute coronary syndrome, cardiac surgery, or percutaneous intervention to maximize health benefits [11,12].
Aerobic training is widely included to CR programs together with resistance training [1]. Combined aerobic and resistance training versus aerobic training alone in coronary artery disease patients has shown to be more effective in improving body composition, maximal muscle strength and cardiorespiratory fitness with equally safe compared to aerobic training only [13]. Furthermore, for cardiorespiratory fitness, longer session duration and shorter postcoronary artery disease period are associated with better outcome, whereas for muscle strength, higher training volume, longer postcoronary artery disease period and younger age are associated with better outcome. Additionally, no significant difference has been shown in effect expressed as maximal aerobic capacity or muscle strength between training for ≤12 weeks and >12 weeks, training ≤2 days per week and ≥3 days, and with moderate and high intensity of aerobic and resistance training [14].
Both exercise training modalities performed in same session has shown to induce clinically relevant fitness improvements in older adults [15,16]. Therefore, we compared if combined aerobic and strength training performed in the same session three times in a week for 12 weeks will increase physical performance further compared to previously perform aerobic training only in stable Coronary Artery Disease patients (CAD). Since the debate as to what dynamic strength training intensities should actually be applied [17], we compared the effectiveness of two different combined aerobic and strength training program protocols (HLG: High Volume-Low Intensity Group vs. LHS: Low Volume-High Intensity Group) on peak aerobic capacity and maximal muscle strength of upper and lower body.
Materials and Methods
Subjects and study protocol
Volunteer individuals with diagnosis of coronary artery disease were recruited from a consecutive series of patients from the Cardiac Rehabilitation Center of Genoa (Azienda Sanitaria Locale ASL 3, Genoa, Italy) from January 2019 through May 2019. All of those patients were stable and medicated according to medical guidelines, and included to the study according to the following criteria: New York Heart Association (NYHA) Functional Classification class I, no scheduled or emergency procedure for bypass surgery, no unstable angina pectoris, no severe peripheral atherosclerosis, non-smokers, no diabetic retinopathy or neuropathy, or inability to perform regular exercises, e.g. due to severe musculoskeletal problems. Additionally, all patients reported exercise training background with at least three months of aerobic training at least two times in a week and no resistance training previously. The study was carried out according to the Declaration of Helsinki, accepted in the local Ethics Committee of the Liguria Region (study number 11559), and all the subjects gave written informed consent.
Combined aerobic and resistance training intervention
Individuals (n=30) willing to participate were randomized to high volume-low intensity group (HLG, n=15) or low volumehigh intensity group (LHG, n=15) and were invited to the Cardiac Rehabilitation Center of Genoa (Italy) to start the laboratory controlled 12 weeks exercise training program, which included three exercise sessions on a week. During the intervention, three times a week they visited our Cardiac Rehab gym equipped with aerobic (Monark Exercise AB, Vansbro, Sweden) and air resistance exercise devices (HUR Oy, Kokkola, Finland), where they were individually guided by a physical therapist. The study outflow is presented in Figure 1.
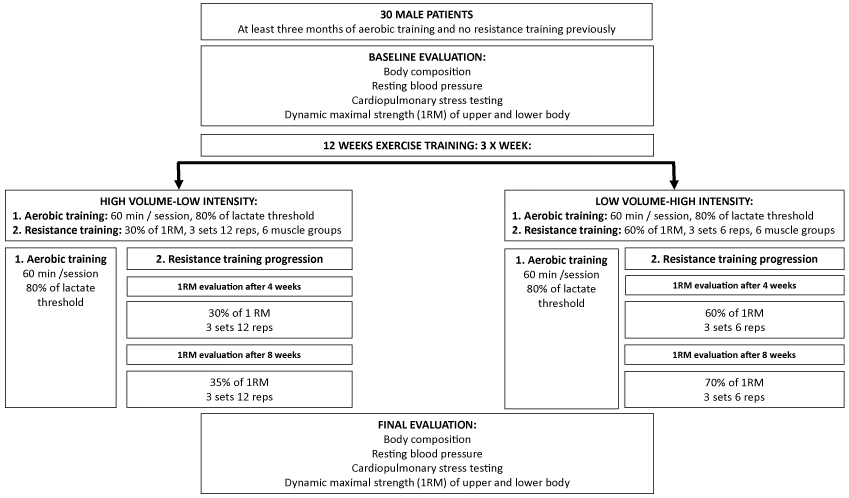
Figure 1: Study design for protocol comparison.
The exercise training was planned and modified according to the cardiac rehabilitation guidelines [18-20]. During the 12 weeks exercise training intervention, in each exercise session, both groups performed laboratory controlled aerobic exercise of 60min first including 5min warm-up and 5min cool down first. We decided to start each session with aerobic exercise, since the patients were familiar and experienced with this kind exercise. The intensity of aerobic exercise was defined according to peak aerobic capacity test results targeting to the level of 80% of lactate threshold in Watts, and controlled by physiotherapist during exercise. Aerobic exercise was followed by six major muscle group resistance exercises (for the lower extremity: leg extension/flexion and abduction/adduction; for the upper extremity: push-up/pull-down). Resistance training load was determined for each muscle groups according to the results of the maximal dynamic strength testing (1RM: One Repetition Maximum). The progression of resistance training was confirmed after four and eight weeks by defining new 1RM values to be used to continue training. Resistance training prescription for the HLG was defined as 30-35% of 1RM, 3 sets and 12 repetitions and for the LHG: 60-70% of 1RM, 3 sets and 6 repetitions (Figure 1).
The Perceived Ratings of Exertion (RPE) scale [21] from scale 0 to 10 was used in the end of each exercise session to evaluate the average intensity of a single exercise session. Average realized training load was assessed by calculating training load (RPE x duration of exercise session), described earlier [22].
Assessment of peak aerobic exercise capacity
All the patients performed a symptom-limited maximal exercise test on a bicycle ergometer (Monark Exercise AB, Vansbro, Sweden) for assessment of peak aerobic capacity (VO2peak) using the COSMED system for cardiorespiratory exercise testing (Quark CPET, COSMED, Rome, Italy). One of four possible ramp protocol was selected (10, 15, 20, 25 watt/min) based on weight in order to reach the maximal possible oxygen consumption in 10 to 12 minutes. Standard 12-lead electrocardiograms and blood pressure measurements were obtained at rest, every 3 minutes during exercise, at peak exercise and for 5 minutes during the recovery phase. The test was considered maximal if the respiratory exchange ratio was above 1.1 and/or if peak heart rate was above 85% of predicted maximal heart rate. The lactate threshold was identified for each subject using both the V-slope and ventilator equivalent methods. VO2peak was defined as the highest 20-seconds average of VO2 during the last minute of exercise test.
Assessment of maximal dynamic muscle strength
Maximal dynamic muscle strength (kg) for each muscle groups was tested with air resistance equipment (HUR Oy, Kokkola, Finland), which replaces the weight plates traditionally used in weight stack machines with a pneumatic system of resistance. Maximal dynamic strength was assessed to find the maximum load with which a subject was able to perform 3-5 repetitions for each muscle groups. From these loads the expected 1RM was estimated by using Brzycki’s formula [23] integrated to HUR SmartTouch software.
Measurements of patient characteristics
Body composition was assessed by measurements of weight and body mass index. Blood pressure was measured in a supine position after a 10min resting period. Smoking status, history of acute myocardial infarction, revascularization and medication were defined from the hospital registry and standard questionnaires. Left ventricular systolic function was assessed using 2-D echocardiography (Vivid 7, GE Healthcare, Wauwatosa, WI, USA).
Statistical analyses
The results are expressed as means (SD). The normal Gaussian data distribution was verified by the Kolmogorov-Smirnov goodnessof- fit test. The changes in measured parameters for the whole study group was analyzed by using paired-samples t-test. The differences in responses within the HLG and LHG protocol groups after the training intervention were analyzed by General Linear Model (GLM) procedure for main effect. One-way ANOVA was used to compare the groups at baseline and after intervention if the main effect in GLM <0.05. A chi-square test was used to compare categorical parameters. Statistical analyses of the data were performed with SPSS software (IBM SPSS 26, SPSS Inc., Chicago, Illinois, USA). A P value of <0.05 was considered significant.
Results
Baseline demographics and clinical characteristics of the study participants are illustrated in Table 1. The average of realized exercise training load did not differ between the HLG and LHG groups (TRIMP for the HLG 890 ± 210 and for the LHG 987 ± 402, p=0.530). Similarly, there were no difference in average RPE (p=0.903) asked after each exercise session for the HLG (4.8 ± 1.1) and LHG (4.8 ± 0.9), average duration (min) of a training sessions in a week (HLG 188 ± 35 vs. LHG 206 ± 51, p=0.396) or average number of realized exercise training sessions (HLG 2.1 ± 0.4 vs. LHG 2.1 ± 0.5, p=0.972). During the 12 weeks intervention, six patients in the HLG and none in the LHG group dropped out from the study. More specifically, in the HLG group the reasons for interruption were loss of interest [4], loss of time mainly because of work duties [1] or health-related problems [1].
HLG (n=9)
LHG (n=15)
P-value
Age (years)
66 ± 7
68 ± 8
0.485
BMI (kg/m2)
29 ± 2
27 ± 3
0.295
SBP Rest (mmHg)
116 ± 15
120 ± 13
0.53
DBP Rest (mmHg)
67 ± 7
68 ± 7
0.65
Ejection Fraction
Normal
5
11
0.212
Lower
4
4
Betablockade User
Yes
9
13
0.511
No
0
2
PCI
Yes
2
7
0.21
No
7
8
CABG
Yes
3
4
0.539
No
6
11
Diabetes
Yes
1
4
0.614
No
8
11
Heart Failure
Yes
4
4
0.412
No
5
11
Valve Replacement
Yes
2
2
0.615
No
7
13
Values are means ± SD or the number of subjects (proportion); Ejection fraction >60 was considered as normal; BMI: Body Mass Index; SBP: Systolic Blood Pressure; DBP: Diastolic Blood Pressure; PCI: Percutaneous Coronary Intervention; CABG: Coronary Artery Bypass Grafting.
Table 1: Patient characteristics for High Volume-Low Intensity (HLG) and Low Volume-High Intensity (LHG) and exercise training groups.
VO2peak remained at same level for the whole study group (23 ± 6 vs. 24 ± 7 ml·kg-1·min-1, p=0.380, Table 2) and there was no difference in response between the HLG and LHG showing 3% increase of VO2peak for both groups (p=0.891, Figure 2A). Muscle strength increased markedly when analyzed as one group for both upper (e.g. 35% increase in 1RM Push Up; 24 ± 8 vs. 30 ± 7 kg, p <0.0001) and lower body (e.g. 50% increase in 1RM Leg Extension; 20 ± 6 vs. 27 ± 6 kg, p <0.0001). The responses did not differ between the groups for Push Up or Leg Extension (p=0.240 and p=0.504, respectively, Figure 2B and 2C). There was no difference between the groups in responses of strength gain in other muscle groups (p=ns for all).
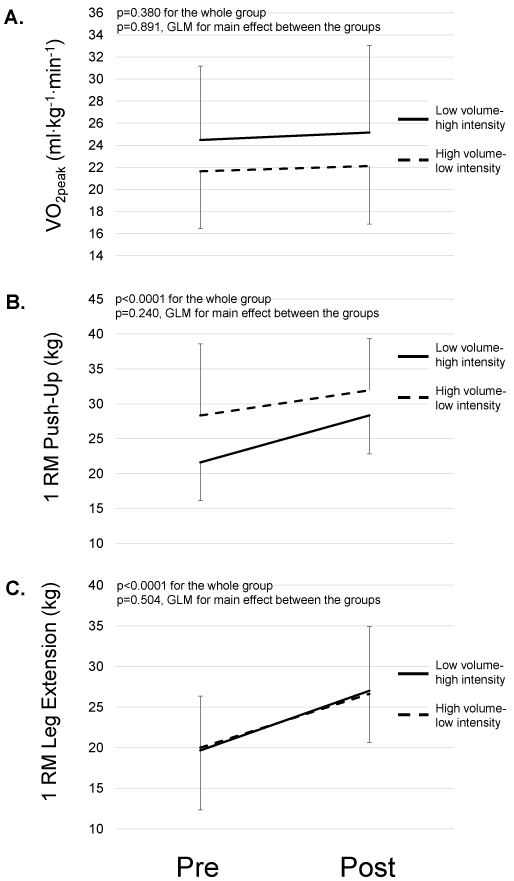
Figure 2: Effects of 12 weeks exercise-based cardiac rehabilitation with two
different protocols performing combined aerobic and resistance training in the
same session on (A) peak aerobic capacity (VO2peak), (B) maximal dynamic
strength of upper body (1RM of Push Up) and (C) maximal dynamic strength
of lower body (1RM of Leg Extension).
Pre
Post
P-value
BMI (kg/m2)
28 ± 3
28 ± 3
0.649
SBP rest (mmHg)
119 ± 14
119 ± 11
0.588
DBP rest (mmHg)
68 ± 7
70 ± 8
0.029
VO2peak (ml/kg-1/min-1)
23 ± 6
24 ± 7
0.38
1 RM Push Up (kg)
24 ± 8
30 ± 7
<0.0001
1 RM Pull Down (kg)
36 ± 8
47 ± 8
<0.0001
1 RM Leg Extension (kg)
20 ± 6
27 ± 6
<0.0001
1 RM Leg Flexion (kg)
25 ± 5
31 ± 5
<0.0001
1 RM Abduction (kg)
25 ± 6
31 ± 6
<0.0001
1 RM Adduction (kg)
27 ± 5
32 ± 5
<0.0001
Values are means ± SD or the number of subjects (proportion); BMI: Body Mass Index; SBP: Systolic Blood Pressure; DBP: Diastolic Blood Pressure; VO2peak: Peak Aerobic Exercise Capacity; RM: Repetition Maximum.
Table 2: Results of twelve weeks of exercise training for the whole study group (n=24).
Discussion
The present study demonstrated that combined aerobic and resistance exercises in the same session performed regularly at weekly basis for 12 twelve weeks, maintained cardiorespiratory fitness at the baseline level in stable coronary artery disease patients who had previous aerobic training background but no resistance training. Instead, maximal dynamic strength for upper and lower body increased markedly. Combined aerobic and strength exercises in the same training session improved maximal strength independently of the high or low intensity of strength training. These results may highlight the importance of dynamic strength training even at low intensity level (30-35% of 1RM) to increase maximal upper and lower body strength for aged cardiac patients highlighting physical performance and independent living.
The combination of aerobic and strength training in the elderly is the optimum strategy to improve both neuromuscular and cardiorespiratory functions and, consequently, to maintain functional capacity during aging [24]. Recent meta-analysis confirmed that combined training strategy induced gains in VO2peak, muscle strength, and hypertrophy in patients with coronary artery disease [14]. When adjusting combined aerobic and resistance training performed in the same exercise session with apparently healthy adults over 50 years, clear and functionally relevant beneficial effects for combined training performed in the same session on VO2peak, 6min walking test and 30s chair stand when compared with no-exercise controls were observed. Additionally, there was a small beneficial effect for combined training when compared to aerobic training only for VO2peak [15]. However, the effectiveness of combined aerobic and resistance training in the same exercise session with different training protocols has not been widely studied earlier in cardiac patients.
We observed minimal or no change in VO2peak with our patients independent of high or low resistance training protocol performed (about 3% increase for both groups). It may be partly explained by the fact that our patients had previous background for aerobic training and the volume and intensity of aerobic training during intervention was quite similar compared to earlier, consequently, maintaining VO2peak at same level. It is also noteworthy that combined training had small-to-moderately beneficial effects on VO2peak when compared to aerobic training only in healthy subjects expressed as average absolute increase of 0.8ml·kg-1·min-1 [15], which is well in line with our cardiac patients obtaining VO2peak gain at average level of 0.6ml·kg-1·min-1. It could be argued, that different intra-session exercise order may effect on VO2peak response. Exercise order was earlier studied among 26 apparently healthy elderly men about 65 years, who were divided into two concurrent training groups: strength prior to or after aerobic training for 12 weeks, three times per week performing both exercise types in the same training session. VO2peak increased for both groups showing increase of about 2.1ml·kg-1·min-1, with no difference between groups. However, 1RM of Leg Extension increased more (change about 24kg) when performing strength prior to aerobic exercise (change about 15kg) [25]. In the present study, we observed minor non-significant increase in VO2peak for both high volume-low intensity group and low volume-high intensity group and clear maximal muscle strength gain of upper and lower body for both groups, but we did not change the intra-session order, which may have an influence for the results.
Muscle weakness is prominent in patients with coronary artery disease compared with aged- matched healthy individuals [26]. The prognostic value for muscular fitness is well recognized, for example an increase of 10% in muscle strength has shown to be associated with reductions of 23% and 34% in all-cause and cardiovascular mortality among patients with coronary artery disease patients who were hospitalized for acute coronary syndrome or coronary artery bypass grafting [27]. Therefore, we feel that our results are well in line supporting the idea that combined aerobic and resistance training can substantially contribute to increasing life expectancy in cardiac patients by maintaining peak aerobic capacity and increasing muscle strength. Additionally, these exercise induced benefits can also be positively associated with cost-effectiveness related with less risk of subsequent events and hospitalization providing an evidence based strategy for policy-makers [9,28]. In the present study, the dropout rate from the exercise training program of 12 weeks (20%) was on about a similar level as in some previous studies. One of our previous exercise-based cardiac rehabilitation study of a two-year intervention in coronary artery patients with and without type 2 diabetes, showed the dropout rate about 37% [29]. Similarly, Marzolini et al. [30] demonstrated that non-completion of a 12-month cardiac rehabilitation program averaged 32%. However, in the present study all the dropouts were in HLG and none in the LHG. It could be speculated, if the long duration of single exercise sessions may partly explain the dropout rate because a lack of motivation for four subjects. However, there was no difference in average time spend in exercise session between groups (HLG 89min vs. LHG 98) and average RPE values in the end of exercise (4.8 for both groups) showed that training sessions were well tolerated. In addition, no adverse events were reported during the intervention.
Strengths of this study were that the all exercise sessions were laboratory controlled and realized well according to training prescription. Despite the recognized underutilization of cardiac rehabilitation worldwide [31], our patients were already adapted regular aerobic training in their weekly routine and were willing to add resistance training to their training regimen. Therefore, overall understanding about the benefits of training were well accepted which may helped our patients to get used to this new program of combined aerobic and resistance training in the same session. We understand that the patient sample in our study is small, selected, and included only men, which can limit generalizability to a broader population of coronary artery disease patients especially for individuals with significant co-morbidities. Furthermore, since we did not have a control group, considerable uncertainty remains regarding the effectiveness of same-session combined exercise training compared with aerobic or strength training performed alone or with control group included. Further experimental work is needed to address this deficiency of knowledge and to establish superiority between different training approaches. Future studies may also address the modifying effects of exercise programming variables such as volume and intensity on training outcomes to optimize the prescription of combined training interventions at the individual level.
Conclusion
The present protocol comparison evaluation of exercise-based cardiac rehabilitation shows that combined aerobic and resistance exercises in the same training session for three months maintained cardiorespiratory fitness at baseline level, but increased markedly maximal dynamic strength of upper and lower body. When comparing high volume-low intensity group to low volume-high intensity group, cardiorespiratory fitness remained at the same baseline level for both groups, but there was a clear similar increase of maximal dynamic strength for upper and lower body for both groups. These results may highlight the importance of regular resistance training of big muscle groups, even at moderate intensity (30-35% of 1RM), for aged cardiac patients in terms of physical performance for daily activities, independent living and quality of life.
References
- Ambrosetti M, Abreu A, Corra U, Davos CH, Hansen D, Frederix I, et al. Secondary prevention through comprehensive cardiovascular rehabilitation: From knowledge to implementation. 2020 update. A position paper from the Secondary Prevention and Rehabilitation Section of the European Association of Preventive Cardiology. Eur J Prev Cardiol. 2020: 2047487320913379.
- Halasz G, Piepoli MF. Focus on cardiovascular rehabilitation and exercise training. Eur J Prev Cardiol. 2020; 27: 1683-1687.
- Kotseva K, De Backer G, De Bacquer D, Ryden L, Hoes A, Grobbee D, et al. Lifestyle and impact on cardiovascular risk factor control in coronary patients across 27 countries: Results from the European Society of Cardiology ESC-EORP EUROASPIRE V registry. Eur J Prev Cardiol. 2019: 2047487318825350.
- Laukkanen JA. Cardiac rehabilitation: why is it an underused therapy? Eur Heart J. 2015; 36: 1500-1501.
- Piepoli MF, Abreu A, Albus C, Ambrosetti M, Brotons C, Catapano AL, et al. Update on cardiovascular prevention in clinical practice: A position paper of the European Association of Preventive Cardiology of the European Society of Cardiology. Eur J Prev Cardiol. 2020; 27: 181-205.
- Anderson L, Oldridge N, Thompson DR, Zwisler AD, Rees K, Martin N, et al. Exercise-Based Cardiac Rehabilitation for Coronary Heart Disease: Cochrane Systematic Review and Meta-Analysis. J Am Coll Cardiol. 2016; 67: 1-12.
- Ades PA, Balady GJ, Berra K, Franklin BA, Froelicher V, Hamm LF, et al. The Journal of Cardiopulmonary Rehabilitation and Prevention at 40 Years and Its Role in the Evolution of Cardiac Rehabilitation. J Cardiopulm Rehabil Prev. 2020; 40: 2-8.
- Verschueren S, Eskes AM, Maaskant JM, Roest AM, Latour CHM, Op Reimer WS. The effect of exercise therapy on depressive and anxious symptoms in patients with ischemic heart disease: A systematic review. J Psychosom Res. 2018; 105: 80-91.
- Hautala AJ, Kiviniemi AM, Makikallio T, Koistinen P, Ryynanen OP, Martikainen JA, et al. Economic evaluation of exercise-based cardiac rehabilitation in patients with a recent acute coronary syndrome. Scand J Med Sci Sports. 2017; 27: 1395-1403.
- Piepoli MF, Corra U, Adamopoulos S, Benzer W, Bjarnason-Wehrens B, Cupples M, et al. Secondary prevention in the clinical management of patients with cardiovascular diseases. Core components, standards and outcome measures for referral and delivery: a policy statement from the cardiac rehabilitation section of the European Association for Cardiovascular Prevention & Rehabilitation. Endorsed by the Committee for Practice Guidelines of the European Society of Cardiology. Eur J Prev Cardiol. 2014; 21: 664-681.
- Pelliccia A, Sharma S, Gati S, Back M, Borjesson M, Caselli S, et al. 2020 ESC Guidelines on sports cardiology and exercise in patients with cardiovascular disease. Eur Heart J. 2020.
- Abreu A, Pesah E, Supervia M, Turk-Adawi K, Bjarnason-Wehrens B, Lopez- Jimenez F, et al. Cardiac rehabilitation availability and delivery in Europe: How does it differ by region and compare with other high-income countries? Endorsed by the European Association of Preventive Cardiology. Eur J Prev Cardiol. 2019; 26: 1131-1146.
- Marzolini S, Oh PI, Brooks D. Effect of combined aerobic and resistance training versus aerobic training alone in individuals with coronary artery disease: a meta-analysis. Eur J Prev Cardiol. 2012; 19: 81-94.
- Lee J, Lee R, Stone AJ. Combined Aerobic and Resistance Training for Peak Oxygen Uptake, Muscle Strength, and Hypertrophy after Coronary Artery Disease: a Systematic Review and Meta-Analysis. J Cardiovasc Transl Res. 2020; 13: 601-611.
- Hurst C, Weston KL, McLaren SJ, Weston M. The effects of same-session combined exercise training on cardiorespiratory and functional fitness in older adults: a systematic review and meta-analysis. Aging Clin Exp Res. 2019; 31: 1701-1717.
- Giallauria F, Cittadini A, Smart NA, Vigorito C. Resistance training and sarcopenia. Monaldi Arch Chest Dis. 2016; 84: 738.
- Hansen D, Abreu A, Doherty P, Voller H. Dynamic strength training intensity in cardiovascular rehabilitation: is it time to reconsider clinical practice? A systematic review. Eur J Prev Cardiol. 2019; 26: 1483-1492.
- Corra U, Piepoli MF, Carre F, Heuschmann P, Hoffmann U, Verschuren M, et al. Secondary prevention through cardiac rehabilitation: physical activity counselling and exercise training: key components of the position paper from the Cardiac Rehabilitation Section of the European Association of Cardiovascular Prevention and Rehabilitation. Eur Heart J. 2010; 31: 1967- 1974.
- Fletcher GF, Ades PA, Kligfield P, Arena R, Balady GJ, Bittner VA, et al. Exercise standards for testing and training: a scientific statement from the American Heart Association. Circulation. 2013; 128: 873-934.
- Bjarnason-Wehrens B. Recommendations for resistance exercise in cardiac rehabilitation: Do they need reconsideration? Eur J Prev Cardiol. 2019; 26: 1479-1482.
- Borg GA. Psychophysical bases of perceived exertion. Med Sci Sports Exerc. 1982; 14: 377-381.
- Foster C. Monitoring training in athletes with reference to overtraining syndrome. Med Sci Sports Exerc. 1998; 30: 1164-1168.
- Brzycki M. A Practical Approach to Strength Training: McGraw-Hill. 1998.
- Cadore EL, Izquierdo M. How to simultaneously optimize muscle strength, power, functional capacity, and cardiovascular gains in the elderly: an update. Age (Dordr). 2013; 35: 2329-2344.
- Cadore EL, Izquierdo M, Alberton CL, Pinto RS, Conceicao M, Cunha G, et al. Strength prior to endurance intra-session exercise sequence optimizes neuromuscular and cardiovascular gains in elderly men. Exp Gerontol. 2012; 47: 164-169.
- Gayda M, Merzouk A, Choquet D, Ahmaidi S. Assessment of skeletal muscle fatigue in men with coronary artery disease using surface electromyography during isometric contraction of quadriceps muscles. Arch Phys Med Rehabil. 2005; 86: 210-215.
- Kamiya K, Masuda T, Tanaka S, Hamazaki N, Matsue Y, Mezzani A, et al. Quadriceps Strength as a Predictor of Mortality in Coronary Artery Disease. Am J Med. 2015; 128: 1212-1219.
- Shields GE, Wells A, Doherty P, Heagerty A, Buck D, Davies LM. Costeffectiveness of cardiac rehabilitation: a systematic review. Heart. 2018; 104: 1403-1410.
- Karjalainen JJ, Kiviniemi AM, Hautala AJ, Piira OP, Lepojarvi ES, Peltola MA, et al. Determinants and prognostic value of cardiovascular autonomic function in coronary artery disease patients with and without type 2 diabetes. Diabetes Care. 2014; 37: 286-294.
- Marzolini S, Brooks D, Oh PI. Sex differences in completion of a 12-month cardiac rehabilitation programme: an analysis of 5922 women and men. Eur J Cardiovasc Prev Rehabil. 2008; 15: 698-703.
- Turk-Adawi K, Supervia M, Lopez-Jimenez F, Pesah E, Ding R, Britto RR, et al. Cardiac Rehabilitation Availability and Density around the Globe. E Clinical Medicine. 2019; 13: 31-45.