
Research Article
Austin J Clin Cardiolog. 2023; 9(2): 1106.
Associations between High Sensitivity Troponin in the Emergency Department and Diagnosis of Myocarditis
Giladi E1,3*#; Ratzon R2,3#; Arow Z1,3; Losin I1,3; Omelchenko A1,3; Pereg D1,3; Assali A1,3; Arnson Y1,3
¹Department of Cardiology, Meir Medical Center, Tel Aviv University, Tel Aviv, Israel
²Department of Emergency Medicine, Meir Medical Center, Kfar Saba, Israel
³Sackler Faculty of Medicine, Tel Aviv University, Tel Aviv, Israel
*Corresponding author: Giladi Ela Department of Cardiology, Meir Medical Center, 59 Tshernichovsky, Kfar Saba, Israel. Tel: +972-9-7472587; Fax: +972-9-7472812 Email: elafi@clalit.org.il
#These authors contributed equally to this work.
Received: June 26, 2023 Accepted: July 25, 2023 Published: August 01, 2023
Abstract
Background: The diagnosis of myocarditis is challenging, and typically relies on clinical presentation, non-invasive imaging, and serum biomarkers. We examine if implementation of hsTnT has affected recognition of myocarditis and patient outcomes.
Methods: Retrospective analysis of >18-year-old patients diagnosed with myocarditis in Meir Medical Center since January 2000 to the end of April 2020. Patients were divided based on their diagnosis date - up to January 2014, for which there was a regular troponin test (REG group) and starting February 2014 for which there was a hsTnT test (HS group). We examined the difference in the rate of myocarditis diagnosis, mortality, and hospitalizations due to heart failure.
Results: We identified 262 patients who were diagnosed with myocarditis. There were no significant differences between the groups. After the implementation of hsTnT there was a two-fold increase in the diagnosis rate (0.0366 vs. 0.0625 cases per day; P<0.0001). The REG group presented with more ST changes (51% vs. 29%; p=0.006) and less cases of normal heart function (69% vs. 79%; P=0.048). There was a higher mortality rate in HS group (6 deaths vs. 2; p=0.011).
Conclusions: hsTnT test leads to increase in myocarditis diagnosis and allows for diagnosing more mild case.
Keywords: Myocarditis; Troponin; Diagnosis; Prognosis
Introduction
Myocarditis is a potentially life-threatening inflammatory condition of the myocardium which most often occurs secondary to an infection but can also be immune-mediated due to exposure to toxic substances. Myocarditis is an uncommon and likely underdiagnosed condition which presents with a wide range of cardiac and extra-cardiac symptoms [1,2]. The incidence of myocarditis is difficult to determine as Endomyocardial Biopsy (EMB), the diagnostic gold standard, is seldom used [3,4]. The Global Burden of Disease study reported an incidence of 22 cases of myocarditis per 100,000 patients based on International Classification of Diseases (ICD) codes on hospital discharge documentation between 1990 and 2013 [5].
Myocarditis prognosis is variable and varies by disease cause and severity. When complicated by Left Ventricular (LV) dysfunction, Heart Failure (HF) or arrhythmia it is associated with a poor prognosis [6]. Most of the available data relies on small series, animal experimental models and case reports [7,8].
Given the lack of consensus regarding the role of EMB and the excellent prognosis of patients with mild uncomplicated myocarditis, a recent agreement statement recommends that EMB be reserved for patients who are likely to have specific myocardial disorders associated with worse prognoses and specific treatment recommendations [9]. Cardiac troponins are sensitive of myocyte injury in patients with clinically suspected myocarditis. However, they are non-specific and when normal do not exclude myocarditis [10,11]. In the past few years, highly sensitive troponin tests allow detection of minimal increase in serum troponin levels and can possibly identify more patients with myocarditis. A small study by Ukena et al. demonstrated that high sensitive troponin-T (hsTnT) is a predictive marker for the diagnosis of acute myocarditis with a sensitivity of 83% and specificity of 80% using a cutoff of 50 ng/L [12].
Highly sensitive troponin test had become feasible at our medical center Since February 1st, 2014. The aims of this study were to detect trends in myocarditis diagnosis with the use of hsTnT, and to determine if different lab studies led to any difference in the clinical characterization and prognosis of the patients diagnosed with myocarditis.
Methods
Study Design
A retrospective single center cohort study. The cohort included patients newly diagnosed with acute myocarditis at Meir Medical Center between January 1st, 2000, and April 30th, 2020. The source of data was Meir Medical Center's computerized records which contain all the medical information, including imaging studies, obtained during an emergency room visit, hospital admissions and outpatient follow-up. Potentially eligible patients were identified by screening for patients with an ICD-9 diagnosis or an imaging report of myocarditis. Eligibility criteria were age 18 years or older and newly diagnosed myocarditis with a positive troponin test. Patients younger than 18 and those with missing data were censored from the cohort.
Clinical diagnosis of acute myocarditis was based on constellation of signs and symptoms, Electrocardiogram (ECG) findings and cardiac biomarkers typically seen in myocarditis, with exclusion of acute coronary syndrome.
All relevant cases were manually retrieved and examined. Baseline characteristics collected were demographic data, lab studies including baseline troponin, cardiovascular risk factors (diabetes mellitus, hypertension, dyslipidemia and smoking), presenting symptoms and vital signs at admission (Table 1). Positive troponin tests were defined as >0.1 mg/L (100 ng/L) for the "regular" troponin test (REG group) and >14 ng/L (0.014 mg/L) for the hsTnT test (HS group).
Troponin REG
Troponin HS
P - value
N=121
N=141
Age (mean, sd)
37.2 ± 13.06
36.5 ± 14.6
0.685
Gender
Male
(100)83%
(117)83%
0.916
Female
(41)17%
(24)17%
0.916
N. of Cardiovascular risk factors*
0
(100)83%
(116)82%
0.687
1
(13)11%
(18)13%
0.503
2
(7)6%
(3)2%
0.138
3
(0)0%
(4)3%
0.045
Smoking
(15)12%
(20)14%
0.672
Normal LVEF (%)
(83)69%
(111)79%
0.048
Peak troponin (ng/L)
1053.49
999.68
0.701
ECG
N=85
N=75
ST - Changes
(44)51%
(22)29%
0.006
T- Wave Inversion
(29)34%
(34)45%
0.151
*Cardiovascular risk factors: Diabetes, Hypertension, Dyslipidaemia
LVEF= left ventricular ejection fraction
Table 1: Baseline characteristics.
ECG strips were examined for ST segment deviation or T wave abnormalities. Echocardiography findings include biventricular function and evidence of pericardial effusion. Radiological characteristics of myocarditis were determined from reports of all available cardiac MRI studies. Due to the different periods in which cases were collected, follow-up was limited to 6 years in both groups. Patients were followed for repeated admissions due to heart failure and for all-cause mortality.
Statistical Methods
The Patients were grouped by date of admission and type of troponin test used upon diagnosis. The first group was composed of patients diagnosed with myocarditis between January 1st, 2000, and January 31st, 2014, in the REG group and the second group was composed of patients diagnosed with myocarditis from February 1st, 2014, to April 30th, 2020 in the HS group.
The primary outcome was myocarditis diagnosis rate after HS-troponin test employment in the emergency room setting. Secondary outcomes were the mild myocarditis cases diagnosed (normal LV function and no cardiac sequela), hospitalization for heart failure and overall mortality.
Data are presented as median (Inter-Quartile Range [IQR]) for continuous variables and frequency (%) for categorical variables. Baseline characteristics between patients were compared using two-sample t-test was used for continuous data and a χ2 test, for categorical data. The cumulative incidence of the primary outcome over follow-up period and corresponding 95% Confidence Intervals (CI) was calculated for each group with death as competing risk and comparison of the two groups using logrank test. Clinically statistical significance was determined as P<0.005. Statistical analysis was performed using the SPSS software (version 25, SPSS Inc., Chicago IL).
The study was approved by the Institutional Ethics Committees in accordance with the Declaration of Helsinki.
Results
The study cohort included 262 consecutive patients newly diagnosed with acute myocarditis. The REG included 121 patients; HS group included 141 patients. Clinical characteristics, risk factors and demographic features are presented in Table 1. Mean age was 37.2±13.6 years in the REG group and 36.5±14.62 in HS group (p=0.685), most of patients were male (83% in the two groups). Mean troponin values were 1053.49±944.78 in REG group and 999.68±1264.23 ng/L in HS group (p=0.701).
Myocarditis Diagnosis Rate
Using hsTnT, there was a nearly two-fold increase in the incidence rate of myocarditis (0.063 patients per day, a patient every 16 days and 0.037 patients per day- a patient every 27 days, respectively), with statistically significance of P<0.001 (95% CI 0.014%-0.038%).
Clinical and Prognosis Outcomes
Only 50% of patients in each group had complete ECG data. Higher degree of ST segment changes were observed in REG group, 51% vs. 29% (44/87 patients and 22/75 patients respectively), p=0.006, as presented in figure 1. No significant difference was found in T wave abnormalities between the groups (P=0.151). Patients in the HS group patients had higher rates of normal LV function in echocardiography. Of 141 patients in HS group, 111 patients (79%) had normal LV function compared to 83 of 121 patients (69%) in REG group, p=0.048 (Figure 2). During follow-up period, only 3 patients were subjected to recurrent hospitalization due to exacerbation of heart failure, of which 1 in REG group and 2 in HS group, with no statistical significance. Eight patients have died during follow-up, with higher all-cause mortality rate in HS group (6/140 patients) compared with REG group (2/121 patients), with P=0.011 (Figure 3).
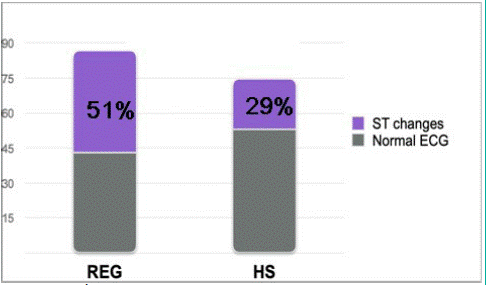
Figure 1: Changers in ECG. ECG changes in REG and HS groups
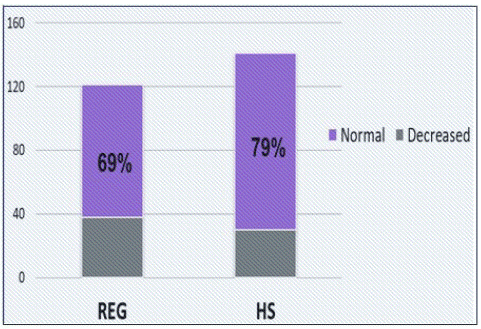
Figure 2: LV Function. LV function (%) in REG and HS groups
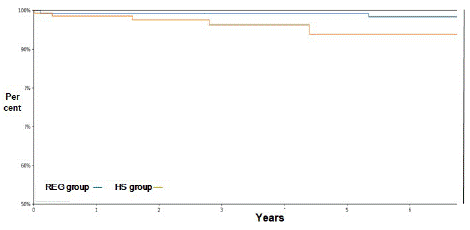
Figure 3: Kaplan-Meier curve for mortality. Mortality rates in REG (yellow line) and HS (blue line) groups
Discussion
Our research shows that the use of hsTnT in the ER results in improved identification rates of myocarditis. The improved recognition rate led to identification of comparatively less severe cases with intact LV function. The patients’ demographics and clinical features were comparable across the groups, with male gender predominance. There was no significant difference regarding cardiovascular risk factors and smokers between the groups. These figures were comparable with previous reports of acute myocarditis [14,15]. Young adults are most frequently affected. The mean age of adult patients with myocarditis has been reported to range from 20 to 51 years [16,17].
The diagnosis of myocarditis did not result in an increased occurrence of cardiac complications during the follow-up duration. This correlates with previous publications mentioned patients presenting with acute myocarditis and preserved left ventricular function have a good prognosis with a high rate of spontaneous improvement without sequelae [13,14]. Nevertheless, in up to 30% of patients with biopsy-proven myocarditis, progression to Dilated Cardiomyopathy (DCM) can occur and is associated with a poor prognosis [4].
Myocarditis is a challenging diagnosis, mainly as there is no pathognomonic clinical presentation, and the disease may present as a variety of non-inflammatory myocardial conditions. Myocarditis has a wide diversity of clinical manifestations, which may range from subclinical to fulminant heart failure.
The gold standard for the diagnosis of myocarditis is the EMB. According to the Dallas criteria, acute myocarditis is defined as the histologic evidence of lymphocytic infiltrates in association with myocyte necrosis [18]. However, subjected to sampling error, variation in expert interpretation, alteration with other markers of viral infection and immune activation in the heart, EBM seldom is used in clinical routine, and is usually reserved for selected cases with severe or rapidly progressive symptoms [1]. Thus, the diagnosis is commonly established by clinical presentation, cardiac biomarkers, and noninvasive imaging findings. Cardiac MRI is a beneficial tool for the diagnosis of myocarditis, with high sensitivity and specificity. This modality can detect intracellular and interstitial edema, capillary leakage and hyperemia that support the diagnosis of myocarditis (Lake Louis criteria) and in severe cases cellular necrosis and interstitial fibrosis. Based on the Lake Louis criteria, myocarditis can be predicted with a diagnostic accuracy of 78% [19]. In our study, however, cardiac MRI was only attainable during later period, and for only a small number of patients (12, 8.5%). In REG group there were no patients diagnosed with the assistance of MRI.
In patients with a history suggestive of myocarditis, an increased cardiac troponin implies myocardial injury, particularly when measured with an assay with high precision. Experimental and clinical studies suggest that serum hsTnT can be a useful diagnostic tool early in the course of myocarditis [20,21]. Cardiac biomarkers in fulminant myocarditis can reach levels similar to those in patients with transmural myocardial infarctions caused by epicardial coronary occlusions [2]. Multiple mechanisms are causative of cardiac troponin leakage in these situations, not solely restricted to irreversible cardiomyocyte necrosis. Potential pathways also include increased left–ventricular filling pressures with subsequent myocardial wall stress, toxicity from inflammatory cytokines, oxidative stress, catecholamine excess and direct cellular damage. However, an absence in hsTnT rise does not rule out myocarditis [22]. Observational studies had failed to prove a significant correlation between the magnitude of troponin measured and prognosis [23-25].
In our study, the mean troponin-T peak in the REG group was 1053.49 ng/L compared with 999.68 ng/L in the HS group. Like previous reports, we could not find a correlation with maximal troponin levels and mortality. This points towards the significance of troponin as a diagnostic rather than prognostic tool.
Despite the common use of ECG as an available screening tool, the sensitivity for myocarditis is merely 47%. The most frequently seen ECG findings are nonspecific T-wave changes. Occasionally, the ECG changes may mimic acute myocardial infarction or pericarditis with ST-segment elevation, ST-segment depression, PR depression, and pathologic Q waves [26,27]. In recent studies, QRS prolongation was an independent negative predictor for survival, while Q-waves and repolarization abnormalities were unrelated to outcome or inflammatory histological features on EMB [28]. In referral populations, new-onset supraventricular or ventricular arrhythmias occur in up to 55% of patients [29], they are often non-sustained and rarely cause hemodynamic compromise. The occurrence of abnormal QRS complexes, axis deviation, or new left bundle branch block is associated with higher rates of mortality or cardiac transplantation [15,26,30].
In our study, more ST changes were present in the REG group than the HS group (51% and 29%, respectively), and no differences were noted in T wave changes. It should be mentioned that measuring QRS interval or T wavelength was not possible due to physical lack of ECG stripes from 20-year-old files, and only ECG reports were available.
Echocardiography is important for evaluation of myocardial damage and heart failure, and for assessment of ventricular thrombi and pericardial effusion. Nevertheless, there are no specific echocardiographic features of myocarditis. Segmental or global wall motion abnormalities are non-specific and can masquerade as myocardial infarction. Patients with fulminant myocarditis tend to present with a non-dilated, thickened, and a hypocontractile left ventricle, whereas patients with mild myocarditis usually present with normal wall thickness. Right ventricular dysfunction is rare but an important predictor of mortality or cardiac transplantation [31].
The REG group of patients included more patients with ECG changes and a higher fraction of patients with left ventricular dysfunction on echocardiography. Thus, it is assumed that HS troponin test had increased the diagnosis rate of patients with mild myocarditis that is not reflected by ECG or echocardiographic findings.
There were more mortality cases in the HS group compared to REG group (6/140 vs. 2/121 patients respectively). This could be partially explained by underdiagnosed patients that were not included in the REG group. Our study had several limitations. First, it is of retrospective nature, which is prone to selection bias. Second, myocarditis diagnosis was also debatable.
Myocarditis is traditionally defined by lymphocytic infiltrated in association with myocyte necrosis not characteristic for ischemic damage [32]. The diagnosis of myocarditis in this study was based on clinical suspicion, evidence of myocardial injury, and the exclusion of an acute coronary event. It could be that events identified as myocarditis were in fact atherosclerotic heart disease without significant coronary stenosis, and vice versa, thus a more accurate diagnosis might have affected study results. Third, the study expands over a period of 20 years, during this time some of the documentation was manually retrieved, which may have led to emitting of undiagnosed cases. Some patient files had only partial data, such as a single troponin test, and that could impact peak troponin calculations. Different follow up periods could have also affected outcomes for recurrent hospitalizations. Fourth, the study was conducted in a single center in Israel, clinical practice may vary from different centers in Israel and other countries.
Conclusion
hsTnT test in suspected myocarditis cases can increase the diagnostic yield and allow detection of more mild cases. More data is necessary to establish its prognostic value.
Author Statements
Acknowledgments
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript. The authors have no relevant financial or non-financial interests to disclose.
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Dr. Reut Ratzon and Dr. Ela Giladi. The first draft of the manuscript was written by Dr. Ela Giladi and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. The authors affirm that human research participants provided informed consent for publication.
References
- Blauwet LA, Cooper LT. Myocarditis. Prog Cardiovasc Dis. 2010; 52: 274-88.
- Kociol RD, Cooper LT, Fang JC, Moslehi JJ, Pang PS, et al. Recognition and initial management of fulminant myocarditis: A scientific statement from the American Heart Association. Circulation. 2020; 141: e69-92.
- Richardson P, McKenna W, Bristow M, Maisch B, Mautner B, et al. Report of the 1995 World Health Organization/International Society and Federation of Cardiology Task Force on the Definition and Classification of cardiomyopathies. Circulation. 1996; 93: 841-2.
- Kindermann I, Barth C, Mahfoud F, Ukena C, Lenski M, et al. Update on myocarditis. J Am Coll Cardiol. 2012; 59: 779-92.
- Global Burden of Disease Study 2013 Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015; 386: 743-800.
- Ammirati E, Cipriani M, Moro C, Raineri C, Pini D, et al. Clinical presentation and outcome in a contemporary cohort of patients with acute myocarditis: multicenter Lombardy registry. Circulation. 2018; 138: 1088-99.
- Caforio AL, Marcolongo R, Basso C, Iliceto S. Clinical presentation and diagnosis of myocarditis. Heart. 2015; 101: 1332-44.
- Caforio ALP, Malipiero G, Marcolongo R, Iliceto S. Myocarditis: A clinical overview. Curr Cardiol Rep. 2017; 19: 63.
- Cooper LT, Baughman KL, Feldman AM, Frustaci A, Jessup M, et al. The role of endomyocardial biopsy in the management of cardiovascular disease: a scientific statement from the American Heart Association, the American College of Cardiology, and the European Society of Cardiology. Circulation. 2007; 116: 2216-33.
- Heymans S. Myocarditis and heart failure: need for better diagnostic, predictive, and therapeutic tools. Eur Heart J. 2007; 28: 1279-80.
- Lauer B, Niederau C, Kühl U, Schannwell M, Pauschinger M, et al. Cardiac troponin T in patients with clinically suspected myocarditis. J Am Coll Cardiol. 1997; 30: 1354-9.
- Ukena C, Kindermann M, Mahfoud F, Geisel J, Lepper PM, et al. Diagnostic and prognostic validity of different biomarkers in patients with suspected myocarditis. Clin Res Cardiol. 2014; 103: 743-51.
- Anzini M, Merlo M, Sabbadini G, Barbati G, Finocchiaro G, et al. Long-term evolution and prognostic stratification of biopsy-proven active myocarditis. Circulation. 2013; 128: 2384-94.
- Caforio AL, Calabrese F, Angelini A, Tona F, Vinci A, et al. A prospective study of biopsy-proven myocarditis: prognostic relevance of clinical and aetiopathogenetic features at diagnosis. Eur Heart J. 2007; 28: 1326-33.
- Magnani JW, Danik HJ, Dec GW Jr, DiSalvo TG. Survival in biopsy-proven myocarditis: a long-term retrospective analysis of the histopathologic, clinical, and hemodynamic predictors. Am Heart J. 2006; 151: 463-70.
- Cooper LT Jr, Berry GJ, Shabetai R. Idiopathic giant-cell myocarditis--natural history and treatment. Multicenter giant cell myocarditis study group investigators. N Engl J Med. 1997; 336: 1860-6.
- Kytö V, Saukko P, Lignitz E, Schwesinger G, Henn V, et al. Diagnosis and presentation of fatal myocarditis. Hum Pathol. 2005; 36: 1003-7.
- Aretz HT, Billingham ME, Edwards WD, Factor SM, Fallon JT, et al. Myocarditis. A histopathologic definition and classification. Am J Cardiovasc Pathol. 1987; 1: 3-14.
- Friedrich MG, Sechtem U, Schulz-Menger J, Holmvang G, Alakija P, et al. Cardiovascular magnetic resonance in myocarditis: a JACC White Paper. J Am Coll Cardiol. 2009; 53: 1475-87.
- Bachmaier K, Mair J, Offner F, Pummerer C, Neu N. Serum cardiac troponin T and creatine kinase-MB elevations in murine autoimmune myocarditis. Circulation. 1995; 92: 1927-32.
- Smith SC, Ladenson JH, Mason JW, Jaffe AS. Elevations of cardiac troponin I associated with myocarditis. Experimental and clinical correlates. Circulation. 1997; 95: 163-8.
- Jani SM, Nallamothu BK, Cooper LT, Smith A, Fazel R. Beating, fast and slow. N Engl J Med. 2017; 377: 72-8.
- Gilotra NA, Minkove N, Bennett MK, Tedford RJ, Steenbergen C, et al. Lack of relationship between serum cardiac troponin I level and giant cell myocarditis diagnosis and outcomes. J Card Fail. 2016; 22: 583-5.
- Aquaro GD, Perfetti M, Camastra G, Monti L, Dellegrottaglie S, et al. Cardiac MR with late gadolinium enhancement in acute myocarditis with preserved systolic function: ITAMY study. J Am Coll Cardiol. 2017; 70: 1977-87.
- Eggers KM, Lindahl B. Application of cardiac troponin in cardiovascular diseases other than acute coronary syndrome. Clin Chem. 2017; 63: 223-35.
- Morgera T, Di Lenarda A, Dreas L, Pinamonti B, Humar F, et al. Electrocardiography of myocarditis revisited: clinical and prognostic significance of electrocardiographic changes. Am Heart J. 1992; 124: 455-67.
- Dec GW Jr, Waldman H, Southern J, Fallon JT, Hutter AM Jr, et al. Viral myocarditis mimicking acute myocardial infarction. J Am Coll Cardiol. 1992; 20: 85-9.
- Ukena C, Mahfoud F, Kindermann I, Kandolf R, Kindermann M, et al. Prognostic electrocardiographic parameters in patients with suspected myocarditis. Eur J Heart Fail. 2011; 13: 398-405.
- Kühl U, Pauschinger M, Seeberg B, Lassner D, Noutsias M, et al. Viral persistence in the myocardium is associated with progressive cardiac dysfunction. Circulation. 2005; 112: 1965-70.
- Nakashima H, Katayama T, Ishizaki M, Takeno M, Honda Y, et al. Q wave and non-Q wave myocarditis with special reference to clinical significance. Jpn Heart J. 1998; 39: 763-74.
- Hazebroek MR, Everaerts K, Heymans S. Diagnostic approach of myocarditis: strike the golden mean. Neth Heart J. 2014; 22: 80-4.
- Guglin M, Nallamshetty L. Myocarditis: diagnosis and treatment. Curr Treat Options Cardiovasc Med. 2012; 14: 637-51.