Case Report
Austin J Clin Case Rep. 2014;1(3): 1013.
The Sinister Face of Tuberculosis
Haque S, Kim H, Cheruvu S and Olowokure OO*
Department of Internal Medicine and Hematology Oncology, University of Cincinnati, USA
*Corresponding author: Olowokure OO, Department of Internal Medicine and Hematology Oncology, University of Cincinnati, 234 Goodman Street, Cincinnati, OH 45219, USA
Received: May 30, 2014; Accepted: June 12, 2014; Published: June 14, 2014
Abstract
Tuberculosis (TB) still remains a deadly scourge in many developing countries and is re-emerging globally with a vengeance. In India, clinicians are encountering tuberculosis with varied manifestations, even in immunocompetent individuals. Adolescents are unique that they may manifest with primary or post-primary TB depending on their immune response. The simultaneous occurrence of primary and post primary TB in an immunocompetent adolescent is a rare presentation, as is highlighted in this case.
Keywords: Tuberculosis; Primary; Post-primary
Case Presentation
A 15-year old girl was admitted to our medical unit with 2-month history of high grade fever, cough with expectoration, anorexia and marked weight loss. There was no significant illness in the past and family history was not contributory. On examination she was cachexic and findings of consolidation in left infraclavicular and mammary region, with no evidence of peripheral lymphadenopathy or hepatosplenomegaly. No choroidal tubercles were demonstrable on fundus examination. Erythrocyte Sedimentation Rate (ESR) was elevated; 50mm/hour (Westergren method) and the Tuberculin test yielded an induration of 20 x 20 mm. Rest of the biochemical and hematological investigations were normal. Serology for Human Immunodeficiency Virus (HIV) was negative.
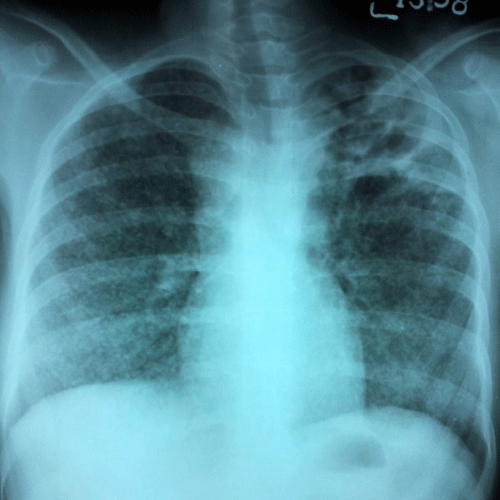
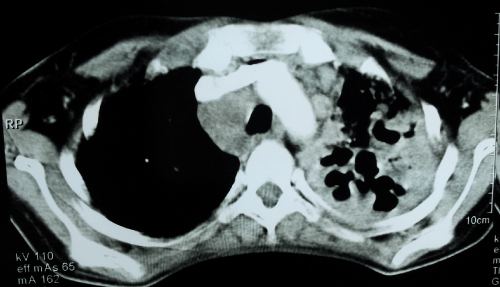
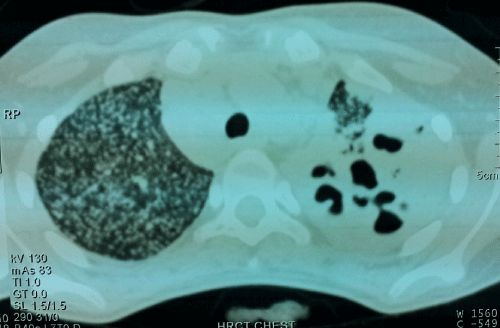
The chest radiograph (Figure 1) showed discrete, fine nodular densities implying miliary nodules diffusely in bilateral lungs, with consolidation and cavitation in left upper lobe in conjunction with mediastinal widening. Computed Tomography scan (CT) of thorax, axial section, showed consolidation with breakdown in left upper lobe, right paratracheal and prevascular lymphadenopathy (Figure 2a). High resolution images of lung window at the same level showed miliary nodules in bilateral upper lobes (Figure 2b). The sputum examination revealed typical Mycobacterium tuberculosis. Patient was started on anti-tubercular 4-drug combination therapy. Patient started showing signs of improvement, with the fever subsiding within two weeks of treatment.
Figure 1 :The chest radiograph shows miliary nodules diffusely in bilateral lungs, consolidation with cavitation in left upper lobe and mediastinal widening due to lymphadenopathy.
Figure 2a :Computed tomography (CT) of the thorax, axial section, at the level of upper lobes showing consolidation with breakdown in left upper lobe, right paratracheal and prevascular lymphadenopathy.
Figure 2b :High resolution images of the lung window showing miliary nodules in bilateral upper lobes.
Discussion
Tuberculosis is an infectious granulomatous disease caused by Mycobacterium tuberculosis, an acid-fast bacillus that is transmitted primarily via the respiratory route. Usually the primary focus is lungs and then the disease spreads secondarily to other organs. The disease may manifest as primary TB in children or become latent and then get reactivated in later life as post primary TB.
It is recognized that primary TB is primarily seen in children and presents either as mediastinal lymphadenopathy, parenchymal consolidation without upper lobe predilection / cavitation or as miliary TB and pleural effusion. In contrast, post primary is classically seen in adults, is more infectious, associated with upper lobe cavitation and absence of significant mediastinal lymphadenopathy. Although historically, these forms are distinct with unique clinical and radiological features, rarely overlapping characteristics between the two forms may be discernable.
TB is uncommon in adolescents and differs substantially from disease in younger children as they are more likely to be infectious and present symptomatically [1]. Clinical and radiographic findings may however mirror those of adults, with reactivation disease in lung apices [2], or of younger children, with intrathoracic adenopathy and higher rates of extrapulmonary disease than seen in adults [3]. Thus it may be often difficult to differentiate primary or post primary TB in adolescents as they may have common characteristics features of both.
Miliary disease is form of primary tuberculosis and traditionally has been observed more commonly in primary than post-primary disease. It is often observed in the immunocompromised individuals and generally has extra-pulmonary involvement. Among immunocompetent adults, miliary TB accounts for fewer than 2 per cent of all cases of TB [4-6]. Historically, miliary TB was considered a disease of infants and children, however currently, two peaks are evident, first in adolescence and young adults and second in elderly [4-6]. The inadequacy of effector T-cell response in containment of M. tuberculosis is considered responsible for progression to miliary TB, representing the Th2 end of spectrum [7- 8]. Conversely, cavitation occurs secondary to caseation necrosis and is a marker of body�s effective T- cell immune response, representing the Th1 end of spectrum. Cavitation in pulmonary TB represents reactivation of disease, as in post-primary tuberculosis [9,10]. Our immunocompetent patient had simultaneous occurrence of cavitatory lesions, miliary and mediastinal lymph-nodal tuberculosis, which represents a continuum of both primary and post-primary TB.
Host immune response status may be a better predictor of radiographic findings than classification by primary and post-primary TB [11]. It is important to emphasize that although cavitation, upper lobe involvement and sputum positivity are predominantly seen in post-primary TB, they may rarely be signs of active primary TB [11]. Infrequently, endobronchial spread in cavitatory TB may lead to air-space consolidation and diffuse parenchymal infiltrates typical of primary TB. In fact, quite unexpectedly, a recent study has demonstrated occurrence of upper lobe predilection and cavitation in healthy adolescents diagnosed with primary TB [12].
Learning points
- A high index of suspicion is required for diagnosing tuberculosis in adolescents.
- Simultaneous existence of miliary, mediastinal lymph-nodal and pulmonary tuberculosis cavitary lesions is very rare.
- High endemicity of tuberculosis in India and malnutrition may be responsible for this unusual presentation
References
- Cruz AT, Hwang KM, Birnbaum GD, Starke JR. Adolescents with tuberculosis: a review of 145 cases. Pediatr Infect Dis J. 2013; 32: 937-941.
- Sant'Anna CC, Schmidt CM, March Mde F, Pereira SM, Barreto ML. Radiologic findings of pulmonary tuberculosis in adolescents. Braz J Infect Dis. 2011; 15: 40-44.
- de Pontual L, Balu L, Ovetchkine P, Maury-Tisseron B, Lachassinne E, Cruaud P, et al. Tuberculosis in adolescents: A French retrospective study of 52 cases. Pediatr Infect Dis J. 2006; 25: 930-932.
- Sharma SK, Mohan A, Sharma A, Mitra DK. Miliary tuberculosis: new insights into an old disease. Lancet Infect Dis. 2005; 5: 415-430.
- Jacob JT, Mehta AK, Leonard MK. Acute forms of tuberculosis in adults. Am J Med. 2009; 122: 12-17.
- Hussain SF, Irfan M, Abbasi M, Anwer SS, Davidson S, Haqqee R, et al. Clinical characteristics of 110 miliary tuberculosis patients from a low HIV prevalence country. Int J Tuberc Lung Dis. 2004; 8: 493-499.
- Sharma PK, Saha PK, Singh A, Sharma SK, Ghosh B, Mitra DK, et al. FoxP3+ regulatory T cells suppress effector T-cell function at pathologic site in miliary tuberculosis. Am J Respir Crit Care Med. 2009; 179: 1061-1070.
- Sharma SK, Mitra DK, Balamurugan A, Pandey RM, Mehra NK. Cytokine polarization in miliary and pleural tuberculosis. J Clin Immunol. 2002; 22: 345-352.
- Jeong Y1, Lee KS. Pulmonary tuberculosis: up-to-date imaging and management. AJR Am J Roentgenol. 2008; 191: 834-844.
- Collins HL, Kaufmann SH. The many faces of host responses to tuberculosis. Immunology. 2001; 103: 1-9.
- Zawaideh M, Chao C, Poole P, Naheedy J. Primary tuberculosis in a malnourished adolescent. J Radiol Case Rep. 2012; 6: 1-8.
- Koh WJ, Jeong YJ, Kwon OJ, Kim HJ, Cho EH, Lew WJ, et al. Chest radiographic findings in primary pulmonary tuberculosis: observations from high school outbreaks. Korean J Radiol. 2010; 11: 612-617.