Case Report
Austin J Clin Case Rep. 2014;1(3): 1015.
Primary Meibomian Gland Carcinomas: a Technical Challenge to Treat from Radiotherapist Perspective
Rakesh Kapoor*
Department of Radiation Oncology, Institute of Medical Education and Research, India
*Corresponding author: Rakesh Kapoor, Department of Radiation Oncology, Institute of Medical Education and Research, Chandigarh, India
Received: May 20, 2014; Accepted: June 12, 2014; Published: June 16, 2014
Summary
Meibomian gland carcinoma is a very rare malignancy which we commonly deal with. Because of its slow growing nature and its ability to masquerade as multiple benign conditions treating this tumour is a major therapeutic challenge from an oncologist perspective. Here we have shared our experience with three such cases.
Background
The sebaceous carcinoma is a very rare malignant neoplasm primarily found in the area of the eyelid. Most of these cases originate in the tarsal meibomian glands. Meibomian gland carcinoma is considered to be the second most common eyelid malignancy after basal cell carcinoma [1]. These tumours are slow growing which may initially look benign in appearance and simulates to a number of benign pathological conditions like chalazion, papilloma, seborrheic keratitis, keratoacanthoma etc. A delay in diagnosis, which can be attributed primarily to ability of this tumour to masquerade as more benign conditions, often leads to inappropriate management with increased morbidity and mortality rates. Here we describe three cases of primary meibomian gland carcinoma with different biological behavior and management.
Case summary I
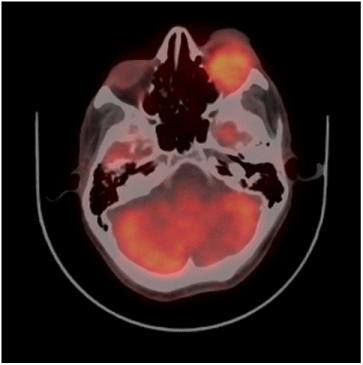
A 45 year old male patient presented with redness and watering of left eye for two months, painless progressive swelling of left eyelid since one month and mild decrease in vision in left eye for the same duration. On clinical examination a firm lobular pinkish mass was felt in the left lower eyelid involving bulbar conjunctiva. He underwent computed tomography of orbit which showed an enhancing mass lesion measuring 3.7x2.8x2.2 cm seen in inferolateral part of left orbit having ill defined fat planes with lateral rectus and inferior rectus muscles causing proptosis. PET-CT showed moderate FDG (SUV max 5.8) uptake in a well defined soft tissue lesion posterior to the globe. The mass was seen to extend both intra and extraconally. Loss of fat planes was noted with left lateral rectus and inferior rectus. Optic nerve was not visualized separately (Figure 1). Mild to moderate FDG uptake was also noted in bilateral cervical level II, right axillary and mediastinal lymph nodes. FDG avid lesions were also noted in lung, liver bilateral adrenal glands and multiple skeletal sites which were suggestive of widespread metastatic involvement. Fine needle aspiration cytology of the left infraorbital swelling came out to be meibomian gland carcinoma. In view of widespread disseminated disease patient has been given six cycles of chemotherapy based on Injection Paclitaxel 260 mg IV day 1 and injection Cisplatin 70 mg IV day 1 at three weekly intervals. He also received palliative local radiation to left eye 30 Gray in 10 fractions over two weeks. Patient is kept on follow up and leading a good quality of life for last six months.
Figure 1 :
Case summary II
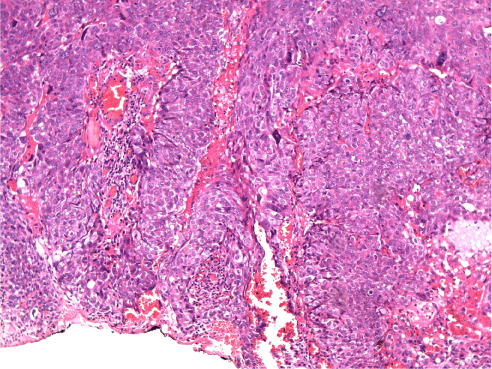
A 75 year old male patient presented with painless progressive swelling in the left upper eyelid for four months. On clinical examination a mass measuring 2x2 cm firm in consistency, with irregular surface was seen in the left upper eyelid. Rest of his medical examination was within normal limit. CECT orbit showed3.6x3.5 cm well defined heterogeneously enhancing soft tissue mass lesion was seen in superolateral extraconal compartment of left eye growing exophytically. He underwent excision of the upper eyelid mass with eyelid reconstruction. Histopathological examination revealed an ulcer measuring 2x2 cm in which tumour cells were arranged in sheets and lobules. The tumour cells had moderately pleomorphic vesicular nuclei, having prominent nucleoli and moderate amount of cytoplasm with vascularisation at places (Figure 2). Overall features were of meibomian gland carcinoma with distal resection margin involved by the tumour. He received post operative external beam radiotherapy 45 Gray in 15 fractions over 3 weeks period with electron beam in view of margin positivity. Pt is kept on follow up and he had clinically no evidence of disease.
Figure 2 :
Case summary III
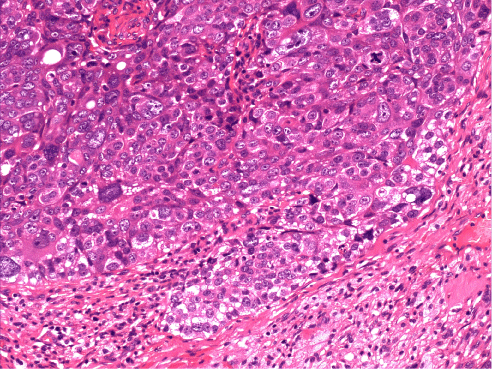
A 30 year old male presented with swelling in the lateral aspect of right lower eyelid since last four years. It was gradually progressive and was associated with mild pain. Wide local excision of mass was done four years back but it recurred since last three months. CECT orbit showed evidence of hypodense ill defined mass showing uniform enhancement seen predominantly at the lateral can thus, inferior part of preseptal compartment of eye with mild postseptal extension into the extraconal compartment lateral to lateral rectus showing ill defined fat planes with it and with the globe laterally. He was again operated and surgical pathology report showed infiltrating tumour composed of sheets and nest of tumour cells separated by fibrous tissue. The tumour cells show moderate nuclear pleomorphism and have moderate to abundant clear vacuolated cytoplasm (Figure3). Overall features were of meibomian gland carcinoma with resection limits, bone and lateral orbital wall involved by tumour. In view of positive resection margin patient had been given postoperative external beam radiotherapy 40 Gray in 20 fractions over four weeks with electrons. The disease again recurred after one year and underwent salvagesurgery in the form of right orbito-zygomatico maxillectomy with superficial parotidectomy with right neck sampling. Histopathology examination revealed poorly differentiated sebaceous carcinoma of right eyelid and meibomian gland involving lateral can thus of right eye, part of upper and lower conjunctiva, lacrimal gland and lateral rectus muscle. He was reirradiated with 3D conformal radiation 36 Gy in 20 fractions over four weeks. In view of high grade of tumour he received six cycles of chemotherapy based on Injection Ifosfamide 2 gm IV day1 to day 3 and Injection Cisplatin 30 mg day1 to day3 at three weekly intervals. After 6 months of follow up a repeat CECT head was done which revealed only bony defect in right frontal and zygomatic bone, right side maxillary sinus and greater wing of sphenoid with no evidence of growth.
Figure 3 :
Discussion
Meibomian glands are modified sebaceous glands present in the stroma of tarsal plate arranged vertically. They are about 30-40 in the upper lid and about 20-30 in the lower eyelid. Their secretions constitute the oily layer of the tear film [2]. Although sebaceous carcinoma has the potential to develop from any sebaceous glands in the body, it most commonly arises from the meibomian glands. Several large series confirmed that ocular sebaceous carcinomas arose from meibomian glands in 51-70% of cases examined, rest from gland of Zeiss and caruncle of orbit [2,3]. The clinical presentations of ocular sebaceous carcinomas are diverse and may delay an accurate diagnosis for months to years. It is a very slow growing tumour and commonly found in elderly population with female predisposition [1,3,4]. Mean age at diagnosis is mid sixties, however the tumour has been reported in children as young as 3-5 years old [1,2]. Upper eyelid lesions are two to three times more common than lower eyelid lesions probably reflecting the greater number of meibomian glands in the tarsal plate of the upper eyelid [2]. The most common clinical presentation is a small, erythematous or yellowish, slow growing deep seated papule or nodule on the upper eyelid that simulates a chalazion. Two important features differentiate meibomian carcinoma from other periocular malignancies. First, unlike single origin of other tumours, meibomian carcinomas appear to arise from multifocal origins. Second, unlike radial spread of basal cell and squamous cell carcinomas, meibomian gland carcinoma tends to spread superficially in a pattern known as pagetoid spread, which is a hallmark of this tumour. If pagetoid spread or intraepithelial spread on to the conjunctiva simulate to keratoconjunctivitis or blepharoconjunctivitis. Advanced cases with extensive pagetoid spread may result in loss of eyelid lashes, eyelid eversion, erosion and ulceration and gross ocular distortion. It is the pagetoid spread of the tumour that may confuse both clinician and the pathologist. The clinician may misdiagnose meibomian gland carcinoma as blepharoconjunctivitis and the pathologist as dysplasia [5,6]. Therefore we have to be very cautious in treating cases of recurrent blepharoconjunctivitis or chalazion not responding to treatment. Meibomian gland carcinomas can spread through direct, lymphatic or hematogenous route. The most common sites of spread are orbit, preauricular nodes, submandibulr nodes, and parotid gland. The less common sites of extension include cervical lymph nodes, lung, pleura, liver, brain, pericardium, lips, ethmoid sinus, or skull [7,8].
The therapy of choice for the meibomian carcinoma is primarily a surgical one. Radical surgical excision with frozen section by either a standard method or Moh’s micrographic surgery is the most common surgical procedure practiced. A subtotal or complete exenteration may be required in very large or recurrent tumours with spread to bulbar conjunctiva or orbital tissues. If there is evidence of regional lymph node involvement radical neck dissection along with partial parotidectomy should be performed [9]. Radiation therapy can be an alternative approach to surgical excision and may be considered as an adjunct to local surgery also. Radiotherapy as primary mode of treatment, has shown variable results in different studies [5,10]. Radiation is mainly reserved for patients who are not candidates for surgical procedures due to advanced age or disease, for palliation in widespread disease, and for patients who refuse exenteration for advanced local disease. Topical mitomycin C has been tried for pagetoid invasion of the conjunctiva by eyelid sebaceous gland carcinoma [11]. Cryotherapy is a useful adjunct to surgery in epibulbar and pagetoid extension of sebaceous gland, sparing exenteration. Probably our experience may throw some light in the management of meibomian gland carcinoma, which we rarely deal with.
References
- Ni C, Searl SS, Kuo PK, Chu FR, Chong CS, Albert DM, et al. Sebaceous cell carcinomas of the ocular adnexa. Int Ophthalmol Clin. 1982; 22: 23-61.
- Surgical Anatomy of the Orbit. Zide BM, Jelks GW, editors. New York: Raven Press. 1985: 35.
- Rao NA, Hidayat AA, McLean IW, Zimmerman LE. Sebaceous carcinomas of the ocular adnexa: A clinicopathologic study of 104 cases, with five-year follow-up data. Hum Pathol. 1982; 13: 113-122.
- Nelson BR, Hamlet KR, Gillard M, Railan D, Johnson TM. Sebaceous carcinoma. J Am Acad Dermatol. 1995; 33: 1-15.
- Shields JA, Demirci H, Marr BP, Eagle RC Jr, Shields CL. Sebaceous carcinoma of the eyelids: personal experience with 60 cases. Ophthalmology. 2004; 111: 2151-2157.
- Zürcher M, Hintschich CR, Garner A, Bunce C, Collin JR. Sebaceous carcinoma of the eyelid: a clinicopathological study. Br J Ophthalmol. 1998; 82: 1049-1055.
- Ni C, Kou PK. Meibomian gland carcinoma: A clinico-pathological study of 156 cases with long-period follows up of 100 cases. Jpn J Ophthalmol. 1979; 23: 388–401.
- Boniuk M, Zimmerman LE. Sebaceous carcinoma of the eyelid, eyebrow, caruncle, and orbit. Trans Am Acad Ophthalmol Otolaryngol. 1968; 72: 619-642.
- Wali UK, Al-Mujaini A. Sebaceous gland carcinoma of the eyelid. Oman J Ophthalmol. 2010; 3: 117-121.
- Hendley RL, Rieser JC, Cavanagh HD, Bodner BI, Waring GO 3rd. Primary radiation therapy for meibomian gland carcinoma. Am J Ophthalmol. 1979; 87: 206-209.
- Shields CL, Naseripour M, Shields JA, Eagle RC Jr. Topical mitomycin-C for pagetoid invasion of the conjunctiva by eyelid sebaceous gland carcinoma. Ophthalmology. 2002; 109: 2129-2133.