Case Report
Austin J Clin Case Rep. 2014;1(4): 1018.
Microprolactinoma in a Woman with Sheehan’s Syndrome
Deepti Jain*
Department of Obstetrics and Gynecology, Chhotu Ram Hospital, India
*Corresponding author: Deepti Jain, Department of Obstetrics and Gynecology, Chhotu Ram Hospital, 10, 11 Huda complex, Rohtak, Haryana, India
Received: May 20, 2014; Accepted: June 20, 2014; Published: June 23, 2014
Abstract
A 24 year old woman presented with amenorrhoea and inability to conceive. One and a half year back she had an episode of massive antepartum haemorrhage. Endocrinal work up revealed deficiency of gonadotrophins, central hypothyroidism and paradoxically a very high level of serum prolactin, thus diagnosed as a case of Sheehan’s syndrome with hyperprolactinemia. Magnetic resonance imaging revealed a microadenoma of the pituitary gland. She was treated with thyroxine replacement, dopamine agonist cabergoline and cyclic estrogen and progesterone therapy. Ovulation was augmented with clomiphene citrate. She conceived and a small for gestational age baby was delivered with no apparent anomalies. Postnatally she had adequate lactation contrary to most women with postpartum hypopitiutarism.
Keywords: Sheehan’s Syndrome; Hyperprolactinemia; Gonadotrophins Microprolactinoma
Abbreviations
TSH: Thyroid stimulating hormone; MRI: Magnetic Resonance Imaging; T3: Tri-iodo Thyronine; T4: Thyroxine
Case Presentation
A 24year old woman presented on 8th Jan 2010, with secondary amenorrhoea and inability to conceive for the last one and a half year. She had an episode of ante partum haemorhage at 30 weeks of pregnancy, 2 years back. She was rushed to the nearest tertiary care centre where she delivered a preterm fresh still born fetus. Two units of blood transfusion had to be given to combat the hypovolemic shock.
After this episode she started having acyclic menses, occurring after prolonged periods of time, followed by secondary amenorrhea. She had periods once following a course of medroxy progesterone acetate.
Later on, repeated administration of medroxy progesterone failed to induce a withdrawal bleed.
Investigations
Since progesterone challenge test was already negative, Endocrinal workup was begun (Table 1).
Pelvic ultrasonography was done, which revealed that the uterus was of normal size .However, endometrial thickness was only 1.6mm, suggesting marked estrogen deficiency.
Name
Patient� value
Normal� range
Serum Luteinizing Hormone
4.30 �iu/ml
1.90 � 16.90 �iu/ml
Follicle Stimulating Hormone
7.51 �iu/ml
2.50 � 10.20 �iu/ml
Tri-iodo thyronine T3
80.20ng/dl
60 � 181 ng/dl
Thyroxine T4
3.10 ng/dl
4.50 � 12.60 ng/dl
Thyroid stimulating hormone, TSH
37.08 �iu/ml
.35 � 5.50 �iu/ml
S. Estradiol
31.93pg/ml
40 � 410 pg/ml
Growth hormone
5.28ng/ml
< 0.01 � 10.00ng/ml
Random Blood Sugar
85ng/dl
<140 ng/dl
Serum Prolactin
241ng/ml
2.80 � 29.20ng/ml
Table 1
Differential diagnosis
As amenorrhoea and infertility occurred following obstetric haemorrhage and since Serum estradiol level was below 40pg/ml, with normal follicle stimulating and luteinizing hormones, a diagnosis of postpartum hypopituitarism or Sheehan’s syndrome was considered. Thyroxine T4 level was low and thyroid stimulating hormone TSH was raised suggesting hypothyroidism. Paradoxically, serum prolactin was very high 241ng/ml and hence a magnetic resonance imaging was performed.
Finding on MRI are as given below:
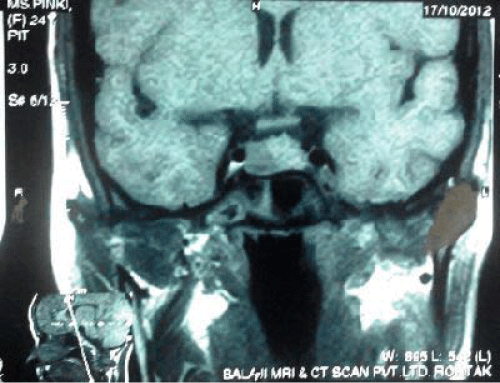
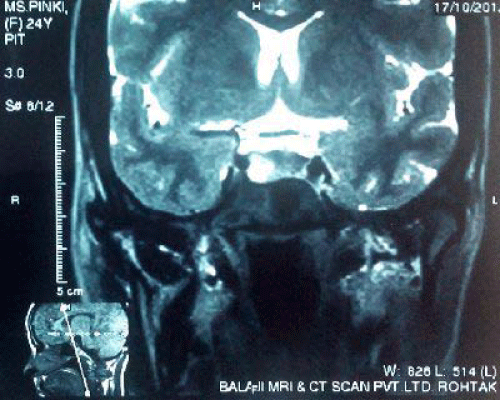
- Focal lesion in peripheral zone of pituitary gland on right side appearing hypointense on T1W and hyper intense on T2W image. This measures 8×8×8.5 mm in size. No suprasellar extension of lesion is seen. Pituitary stalk is diverted to left side.
- Sellar floor is normal.
- Posterior pituitary bright spot normal.
- Suprasellar cistern, chiasma and hypothalamus are normal.
Impression
Focal lesion seen in peripheral region of pituitary gland on right side suggesting micro adenoma (Figure 1,2). Hence a final diagnosis of Sheehan’s syndrome with prolactin secreting micro adenoma was made.
Figure 1: MRI T1W coronal image showing hypointense lesion in pitiutary.
Figure 2: MRI T2W Coronal image shows a hyperintense lesion with no suprasellar extension
Treatment
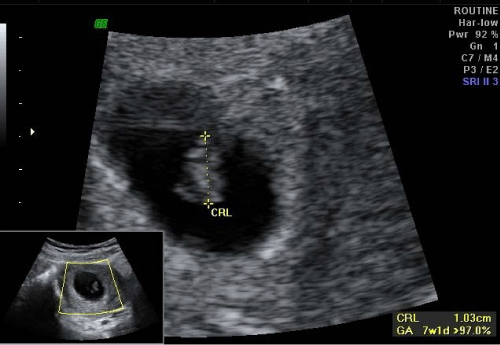
On October 17, 2012 the women was put on L-thyroxine 50mg and cabergoline 0.5 mg twice a week. She was also started with ethinyl estradiol 2mg for 28 days and medroxy progesterone 10 mg once daily for last ten days, for two consecutive cycles. Calcium and Vitamin D supplements were also added. The patient started menstruating with cyclic estrogen and progesterone after one month of therapy. Day 2 investigations after about 6 weeks of therapy revealed that thyroid stimulating hormone value was 6.79 miu / ml and Serum prolactin level had decreased to 2.32 ng / ml. Thyroxine dose was increased to 62.5 mcg. After completion of two cycles of estrogen and progesterone, clomiphene citrate 50 mg was begun from day 2 of cycle. She conceived in the second cycle with clomiphene citrate 37.5 mg and a viable seven weeks fetus was visualized on March 16, 2013 (Figure 3). Cabergoline was stopped as soon as Elisa test for pregnancy was positive. TSH was measured every 4 to 6 weeks and thyroxine dose carefully adjusted to keep TSH below 2miu / ml in 1st trimester and below 3 miu / ml after first trimester. The dose of thyroxine increased from a prepregnant value of 62.5 mg to 112.5 mg just before delivery.
Figure 3: Ultrasound Scan showing 7 weeks viable pregnancy.
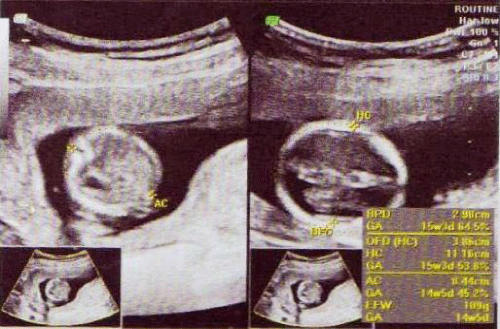
The woman remained normotensive during pregnancy and no glucose intolerance was observed. An anomaly scan at fifteen weeks revealed a healthy fetus with no anomalies (Figure 4). However intrauterine growth retardation was observed and on Sept 26, 2013, i.e. at 34 weeks 2 days, preterm delivery occurred. A 1.3 kg small for gestational age baby was delivered, was shifted to neonatal intensive care unit and the baby recovered in ten days. Breast feeding was begun and lactation was effective with adequate milk production.
Figure 4: Anomaly Scan at 15 weeks.
Discussion
Sheehan’s Syndrome is a devastating disease which occurs following serious obstetric haemorrhage, often requiring blood transfusion. The probable etiology is an infraction of the enlarged pituitary gland of pregnancy, occurring due to massive haemorrhage, resulting in panhypopituitarism or partial hormone deficiency.
In a recent study Growth hormone and prolactin deficiency were seen in 90-100% of cases [1]. Cortisol, gonadotrophin and thyroid stimulating hormones were found to be decreased in 50-100% cases [1]. Diabetes insipidus has also been reported by some authors, though very rare in only 5% cases [1]. Acute cortisol deficiency can result in circulatory collapse and mortality if not detected. Deficiency of pituitary hormones results in loss of reproductive function, genital atrophy, loss of bone mineral density, weakness, debility, and premature ageing.
In our patient there was deficiency of gonadotrophins, evidenced by low levels of estradiol. Thyroxine level was low with a high thyroid stimulating hormone suggesting central hypothyroidism. Other authors too have reported central hypothyroidism in Sheehan’s Syndrome with low T3 and low T4 levels and moderately elevated TSH levels [1]. The high level of TSH is due to increased sialylation (a form of glycosylation) which reduces its metabolic clearance leading to increased half life. However this glycosylated TSH has reduced biological activity.
Contrary to the commonly seen very low levels of prolactin in Sheehan’s Syndrome, hyperprolactinemia was present in this woman. Only 3 reports of Sheehan’s Syndrome with hyperprolactinemia have appeared in literature till date [2-4]. In a case report of Sheehan’s syndrome from Srinagar Valley in India hyperprolactinemia was associated with low cortisol and low thyroxine levels [4]. Sheehan’s syndrome with hyperprolactinemia has been seen in another report but there a scan of the sellar region was normal [3]. Empty sella in 70% cases and partially empty sella in 30% cases are seen on magnetic resonance imaging in most women with Sheehan’s syndrome. These MRI findings in pituitary gland evolve in a time dependent manner following haemorrhage.
Contrary to Empty Sella Sign, a microadenoma in the pituitary gland was visualized in our patient, which has made this case a very unique and rare presentation of Sheehan’s Syndrome, probably the first one ever reported.
Infertility in hypopitiutarism generally is managed with hormone replacement. Estrogen and progesterone are given cyclically to raise estrogen levels and reverse genital atrophy. Human menopausal gonadotrophins are given to induce ovulation in Sheehan’s syndrome with gonadotrophin deficiency. High doses of Human menopausal gonadotrophins were used by us in a case, with successful conception and a good neonatal outcome [5]. However here in the present case after hyperprolactinemia was reversed with cabergoline and euthyroid status was achieved, ovulation could easily be induced with a small dose of clomiphene citrate. Considering that cabergoline is still not validated to be safe in 1st trimester, it was stopped when Elisa test for pregnancy became positive. Since there are no reports suggesting enlargement of microadenoma during pregnancy, the patient was observed for headache, vomiting and cabergoline was not started even after 16 weeks. The hypothyroid status worsened considerably as pregnancy advanced. The presence of intrauterine growth retardation was a significant observation. Most women with Sheehan’s syndrome have severe lactation failure after delivery [5]. However, here milk production was abundant, probably because lactotroph cells of pituitary gland were preserved.
Conclusion
Sheehan’s Syndrome or postpartum hypopituitarism needs to be recognized early and adequate hormone replacement done to prevent further morbidity and restore reproductive function. Hyperprolactinemia with microprolactinoma in the pituitary gland in Sheehan’s presentation was a very surprising observation which is being highlighted with this presentation.
References
- Shivaprasad C. Sheehan's syndrome: Newer advances. Indian J Endocrinol Metab. 2011; 15 Suppl 3: S203-207.
- Stacpoole PW, Kandell TW, Fisher WR. Primary empty sella, hyperprolactinemia, and isolated ACTH deficiency after postpartum hemorrhage. Am J Med. 1983; 74: 905-908.
- Kelestimur F. Hyperprolactinemia in a patient with Sheehan's syndrome. South Med J. 1992; 85: 1008-1010.
- Bashir Laway, Bashir Mir, Ganie Mohd, Mir Shahnaz, Gojwari Tariq, Kotwani Suman, et al. Hyperprolactinemia in a patient with Sheehan’s syndrome. Turkish Journal of Endocrinology and Metabolism. 2010; 14: 47-49.
- Jain D. A ray of hope for a woman with Sheehan's syndrome. BMJ Case Rep. 2013; 2013.