Case Report
Austin J Clin Case Rep. 2014;1(6): 1030.
“Pus Somewhere, Pus Nowhere Else, Pus above the Diaphragm”-Pediatric Pericarditis Puzzling Professionals
Govani DR1, Scott V2, Kumar H3, Patel RR4, Patel RV5* and Vaghela SV6
1Medical Student, University of Birmingham Medical School, UK
2Department of Ped Surgery, Royal Alexandra Children’s Hospital, Brighton, UK
3Department of Ped Surgery, Patan Academy of Health Sciences, Nepal
4Department of Pediatrics (AM), Saurashtra University, India
5Department of Ped Surgery, Saurashtra University, India
6Department of Cardiothoracic Surgery, Saurashtra University, India
*Corresponding author: Patel RV, Department of Surgery, Postgraduate Institute of Child Health and Research and KT Children Government Hospital, Saurashtra University, Rajkot 360001, Gujarat, India
Received: June 28, 2014; Accepted: July 22, 2014; Published: July 24, 2014
Abstract
A case of acute septicaemia in an 18-month-old girl is presented in whom the general surgical approach of the classic aphorism ‘pus somewhere, pus nowhere else, pus under the diaphragm’ proved nothing but a distraction. The child had several professionals involved in her care and multiple investigations including chest and abdominal radiographs, ultrasound scans, and a computerised axial tomogram of the torso failed to detect the problem. She also underwent 3 operative procedures including a diagnostic laparoscopy with incidental appendectomy, exploratory laparotomy with mesenteric lymph node biopsy and insertion of a central line by a general surgeon and a second line insertion. In total she received 4 general anesthetics under continuous EKG monitoring. She was given courses of multiple antibiotic combinations without clinical improvement. She was finally referred to us at the children hospital with cardiac services to rule out a cardiac cause after 2 weeks of investigation and unsuccessful treatment. In addition to classic clinical, laboratory, EKG and imaging investigations done earlier showing clear features of gross pericarditis, she underwent an echocardiogram which confirmed gross purulent pericarditis. This responded well to percutaneous image guided drainage under antibiotic cover. This case highlights changing trends of infections at very young age and that the classic general surgery aphorism may not be applicable to this group of patients. Moreover, this case is a reminder of the dictum that a child should not be considered a miniature form of the adult and general surgical principles may not be applicable to them. It demonstrates that younger children need special expertise and although several professionals from various specialities even with a pediatric interest were involved and numerous investigations were performed, centred on the abdomen, the team was cognitively blocked to look at the evidence on the other side of the diaphragm- the eyes cannot see what the mind does not know. Even the pediatric team had difficulty identifying the problem as cardiology services were based at the cardiac hospital on a different geographical site; hence team did not have routine exposure and practice. It highlights the fact that patient safety and quality of care is still lacking in developing countries even in the twenty first century due to obscure referral pathways, lack of specialist services and geographical isolation.
Keywords: Bacterial; Children; Pericarditis; Pericardiocentesis; Echocardiography; Diaphragm
Introduction
The symptoms and signs of infection at the lower and upper age limits of life, in the pediatric and geriatric populations, are frequently nonspecific. In general surgery, it is recommended to remember the well-known aphorism of “pus somewhere, pus nowhere else, and pus under the diaphragm” [1-3]. Our case is a strong reminder of the facts that it could be above the diaphragm and that what the mind does not know the eyes cannot see.
Case Presentation
An 18-month-old girl presented with an acute infectious illness of short duration of 5 days, characterised by the non specific symptoms of a runny nose, high swinging pyrexia and rigors associated with anorexia, reduced oral intake and irritability. She was seen by her family doctor and diagnosed with an acute viral illness and given oral analgesics and amoxicillin to which she did not respond. She had one episode of vomiting and diarrhoea in these 5 days of acute severe illness.
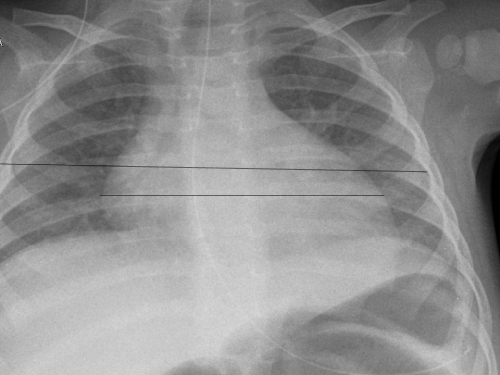
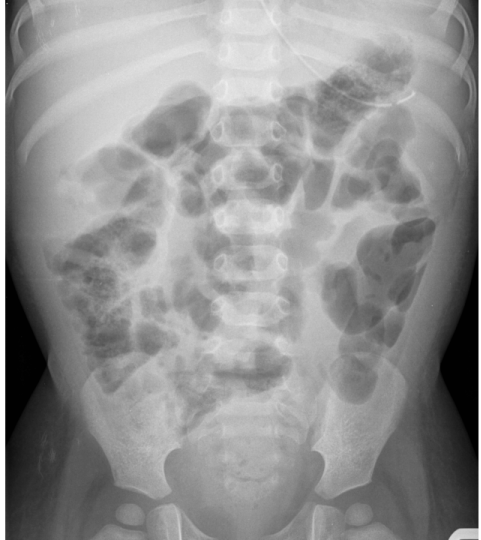
She was subsequently admitted to the district hospital. She was unwell, pale, febrile, tachycardic and tachypneic. Her chest was clear and her abdomen soft and non-tender. Urine dipstick and microscopy was normal. Laboratory investigations including renal and liver functions were normal but the inflammatory markers were raised with a C-reactive protein (CRP) of 307 mg/L, white cell count 24.4 X 109/L, polymorphs 19.82X109/L and hemoglobin of 89 G/L. All bacteriological investigations, including lumbar puncture for cerebrospinal fluid (CSF), urine, stool, and blood and swab cultures were negative. A chest radiograph showed clear lung fields and although an enlarged cardiac shadow and increased cardiothoracic ratio are clearly evident, it was reported to be normal (Figure 1). Abdominal radiograph showed features of febrile ileus (Figure 2).
Figure 1 : Chest radiograph showing clear lung fields and enlarged cardiac shadow. Note increased cardiothoracic ratio.
Figure 2 : Abdominal radiograph showing features of ileus
The child was started on triple antibiotics and given intravenous fluid to which she responded marginally. The pediatric team realised that she was at high risk of serious illness and referred her to the pediatric team at a tertiary center. The referral was rejected on the basis that the child was not intubated or ventilated and the local hospital was advised to continue treatment with antibiotics. Gravely concerned for the child’s welfare and determined to ensure the child’s transfer to a tertiary unit, a referral was made to the pediatric surgical division at the Department of Surgery. An opinion was sought to exclude an acute abdomen with peritonitis although there were minimal clinical features.
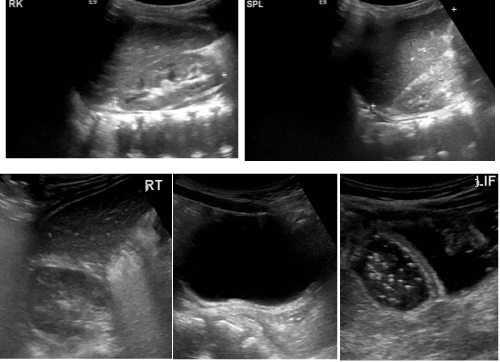
Upon arrival at the tertiary hospital the child was pyrexial but her abdomen was full, very soft and non-tender without any signs of acute peritonism or peritonitis. She was seen by the ad hoc consultant pediatric surgeon and one with a pediatric and anesthetic interest and was not considered to have an acute surgical abdomen. She had an ultrasound scan of her abdomen which showed no abnormality (Figure 3). Her parents were updated.
Figure 3: Abdominal ultrasound showing normal upper and lower abdominal structures.
At this point the pediatric surgeon decided to refer the child to the pediatric cardiology team to rule out endocarditis or a similar cardiac pathology. The pediatric cardiology department was at yet another hospital, the team there insisted on the local pediatric team being involved first and an internal referral was made.
The head of surgical services, a general surgeon, was on call. He considered it as per the classic dictum in surgery that pus somewhere, pus nowhere else, pus under the diaphragm. He immediately booked the case for surgery, did not personally examine the child or consider alternatives given the child’s young age and the child proceeded to surgery. A discussion was held between the pediatrician, the surgeon with pediatric surgical interest and the anesthetist, at whom the head of surgery insisted that this was a surgical case and declined pediatric medical input.
The child’s parents were once again updated, this time being informed that their daughter likely had peritonitis due to appendicitis and required surgery. She proceeded to the operating room and underwent an examination under anesthetic which failed to reveal an appendix mass or similar, followed by a diagnostic laparoscopy.
At laparoscopy, the appendix appeared normal; there was no free fluid in the abdomen and no other pathology was noted. The appendix was removed. Post operatively she continued to have pyrexia and a pediatric medical opinion was once again sought on the 3rd post-operative day as she was not making any progress. As a result her antibiotics were changed to cover a broader range of pathogens (tazocin and gentamycin).
She continued to have high inflammatory markers (CRP 286 mg/L, white cell count 19.2X109/L) despite a further change to antibiotics (piperacilin and tazocin). She was seen by another pediatrician on 5th post-operative day for an opinion which concluded that there was no obvious medical cause for her illness.
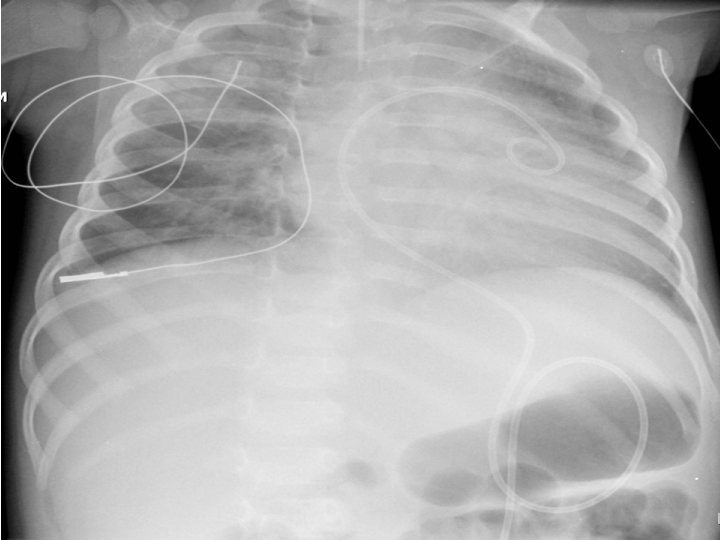
In view of the lack of a medical explanation for the sepsis the child underwent an exploratory laparotomy and insertion of central line on the 5th post-operative day under the care of the general surgeon. A complete flank to flank laparotomy was normal. There were a few lymph nodes in the small bowel mesentery which were biopsied and histology showed only reactive hyperplasia. Unfortunately the insertion of a central line, not guided by ultrasound, in to the right subclavian vein was complicated by a pneumothorax and clinical deterioration (Figure 4). An internal jugular vein line was successfully inserted by anesthetic team and the pneumothorax responded to conservative measures.
Figure 4: Chest radiograph showing right sided pneumothorax. Note elevated right hemidiaphragm and shift of mediastinum.
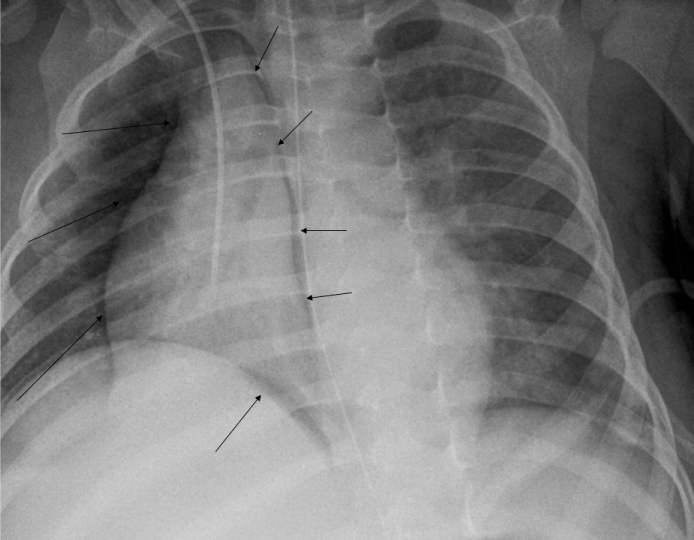
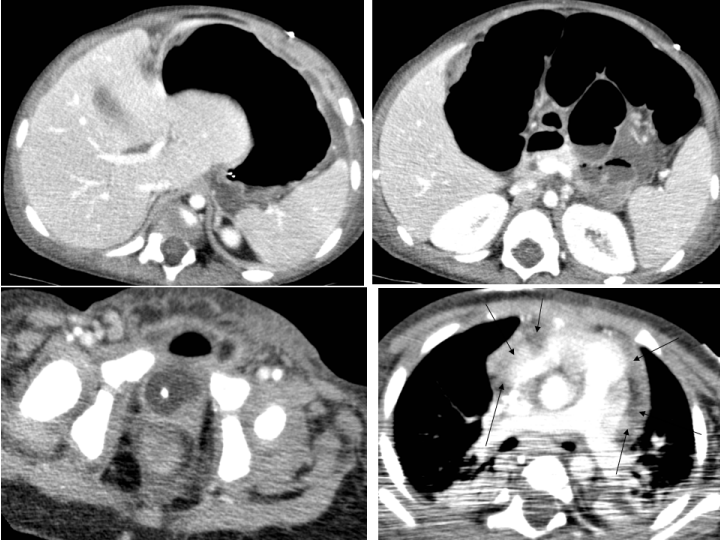
A CAT scan of abdomen and lower thorax under general anesthesia was requested by the general surgeon, again focusing on the search for sepsis within the abdominal cavity. It was reported to show no intra-abdominal pathology except an ileus but also noted left lower lobe collapse and atelectasis of right lung base. The pericardial effusion present on these images was not commented upon; presumably the radiologist was also focused on the abdomen (Figure 5). A further central line for parenteral feeding was inserted under general anesthesia on the 9th day of admission.
Figure 5: CT scans showing bilateral basal collapse of the lung and gross pericardial collection (multiple arrows).
Despite multiple antibiotics the child continued to have swinging pyrexia and sepsis. Two weeks after the initial admission, she was referred to the cardiology department to exclude a cardiac cause of her febrile illness. The classic tell tale features of prodromal viral illness, swinging pyrexia with rigors, tachycardia and tachypneia, seated position with leaning forward, impalpable cardiac impulse, clear audible high pitched pericardial rub, widened concave saddle shaped ST elevation in all leads except AVR and V1, low voltage complexes of variable axis on EKG, review of chest radiograph , ultrasound and CAT scans by our team gave an on the spot diagnosis of pericarditis even before the echocardiogram was done. The echocardiogram revealed an acute pericarditis with a pericardial collection. This was drained by percutaneous pericardiocentesis and catheter drainage under antibiotic cover (Figure 6). The pus was sent for urgent Gram, acid-fast and fungal staining and culture but this failed to identify an organism and although she was referred to immunologist, all tests were normal. She made a good recovery and was allowed home after 3 weeks of admission. At her 3 month follow up appointment she was well and discharged with a cautionary note of lifelong risk of adhesive bowel obstruction due to laparotomy.
Figure 6: Post procedure chest radiograph. Note pericardial drain in situ.
Discussion
Acute pyogenic pericarditis in children is rare but nearly always fatal if untreated [4]. It is usually metastatic resulting as a complication of an infection elsewhere in the body and subsequently spread hematogenously or via lymphatics from the mediastinum or lung [5]. Pre-existing cardiac anomalies, pericardial effusion, septic foci, immunomodulation, chronic disease and previous heart surgery or chest trauma may predispose or complicate pyogenic pericarditis. The typical presentation is that of acute fulminating infectious illness of short duration with high swinging temperatures not responding to intravenous antibiotics [6].
Early detection is the key. Characteristic clinical features (as detailed above), laboratory investigations showing florid septicaemia, EKG criteria and imaging should help. Our patient had several chest and abdominal radiographs, ultrasounds and even a CAT scan. Signs of the pericardial effusion were present on each of them but the focus remained on the abdomen. The child was reviewed by general pediatricians and anesthetists but did not have formal 12 lead EKG at any point. She underwent 4 procedures under general anesthesia with continuous EKG monitoring and these traces should have raised the possibility of pericarditis had they been scrutinised carefully.
Percutaneous pericardiocentesis with or without irrigation of the pericardial cavity combined with effective systemic antibiotic therapy is mandatory (a combination of an antistaphylococcal antibiotic and an aminoglycoside, followed by tailored antibiotic therapy according to the results of pericardial fluid and blood cultures) [7]. This was all that was required in our case. Intrapericardial instillation of antibiotics may additionally be required. Frequent irrigation of the pericardial sac by urokinase or streptokinase, using large catheters, may help to drain thick purulent exudate8. Thoracoscopic or open surgical drainage through sub-xiphoid pericardiotomy may be more appropriate in some cases [9].Pericardiectomy is required in cases in which there are dense adhesions, loculations, thick purulent effusion, recurrence of tamponade, persistent infection, and progression to constriction [7-9].
Surgical mortality up to 8% has been reported for pericardiectomy combined with antibiotic treatment but the total mortality is higher. Mortality in treated patients is 40% in adults and up to 77% in recent reports and in children mostly due to generalised toxaemia, septicaemia, cardiac tamponade and constriction [3,4,10].
This child’s care was compromised by a number of factors and multiple opportunities to improve the quality of treatment were missed. A lack of multidisciplinary working and geographical isolation encouraged clinicians to manage this case independently of other specialist colleagues. The initial referring clinicians were hampered by the failure of the tertiary center to accept this unwell child. An unwise decision was therefore taken to transfer this child for a surgical opinion despite lacking clinical signs, the course of this child illness was then set.
This not only delayed the diagnosis but subjected the child to multiple unnecessary interventions, which could have been life threatening. It also encouraged the tunnel vision attitude that resulted in two explorations of the abdomen with negative results and a CAT scan of the abdomen when the cause of the sepsis was already visible on simple imaging. Whilst it may have been entirely reasonable to perform the initial laparoscopy and even to remove the normal appearing appendix would be debatable, consideration should be given to the decision to proceed with an exploratory laparotomy so soon after a thorough laparoscopy, performed by a surgeon experienced in these techniques, and without further imaging prior to surgery. Even after this second surgery there was considerable delay in seeking specialist opinions to detect the cause of the sepsis which clearly was not the abdomen.
Fortunately this patient has had positive outcome from a potentially fatal condition but lessons must be learned and referral pathways strengthened to ensure that other children who present with unusual pathologies receive the specialist care they require at the earliest opportunity.
Acknowledgement
We are grateful to the general surgical, pediatric, anesthesiology and radiology teams of the district general hospital for their referral of this patient to us for further investigations and treatment. We are grateful to Dr Nayan Kalavadia MD, Consultant Pediatric Intensivist, Dr Anil Patel MD, Consultant Acute Care Pediatrician, Dr G M Faldu MD, Consultant Pediatric Anesthetist, Dr Sudhir Bhimani, Consultant Pediatric Cardiologist, Dr J T Faldu, Consultant Pediatric Pathologist and Dr Kailas Dalsania MD, Consultant Pediatric Interventional Radiologist for their help and expertise in treating this complicated patient successfully.
References
- Thompson J. The peritoneum, omentum, mesentry and retroperitoneal space. William NS, Bulstrode CJK, O’Connell PR, editors. In: Bailey and Love’s short practice of surgery, Hodder Arnold. 2008:991-1008.
- Galloway AC, Anderson RV, Grossi EA, Spencer FC, Colin SB. Acquired heart disease. In Schwartz SI, Shives GT, Spencer FC, Daly JM, Fisher JE, Galloway AC, editors. In: Principles of surgery. McGraw-Hill, New York. 1999:845-908.
- Parry A. Miscellaneous cardiac diseases. Morris PJ, Wood WC, editors. In: Oxford textbook of surgery. Oxford Press. 2008: 2421-2432.
- Lema LE. Surgical management of pyopericardium. East Afr Med J. 1993; 70: 140-142.
- Greeengard J, Hoffman SJ. Pericarditis simulating an acute condition of the abdomen. Arch Surg. 1933; 26: 623-632.
- BOLES ET Jr, HOSIER DM. Abdominal pain in acute myocarditis and pericarditis. Am J Dis Child. 1963; 105: 70-76.
- Goodman LJ. Purulent Pericarditis. Curr Treat Options Cardiovasc Med. 2000; 2: 343-350.
- Ustünsoy H, Celkan MA, Sivrikoz MC, Kazaz H, Kilinç M. Intrapericardial fibrinolytic therapy in purulent pericarditis. Eur J Cardiothorac Surg. 2002; 22: 373-376.
- Sagristà-Sauleda J, Barrabés JA, Permanyer-Miralda G, Soler-Soler J. Purulent pericarditis: review of a 20-year experience in a general hospital. J Am Coll Cardiol. 1993; 22: 1661-1665.
- Keersmaekers T, Elshot SR, Sergeant PT. Primary bacterial pericarditis. Acta Cardiol. 2002; 57: 387-389.