
Case Report
Austin J Clin Case Rep. 2015;2(2): 1072.
Splenic Abscess in Primary Hyperparathyroidism
N K Agrawal*, Naresh Bansal, Saket Kant, Anupam Kumar, Shruti Sharma, Ved Prakash, Jayshree Swain, Anand Kumar and S K Singh
Department of Endocrinology and Metabolism Institute of Medical Sciences Banaras Hindu University, India
*Corresponding author: Agrawal N K, Department of Endocrinology and Metabolism Institute of Medical Sciences Banaras Hindu University, India
Received: September 04, 2014; Accepted: April 23, 2015; Published: May 15, 2015
Abstract
We report a case of a 46 yr old lady presenting with proximal muscle weakness and fractures on trivial trauma secondary to a parathyroid adenoma followed by acute renal failure. She was managed conservatively and underwent surgery for parathyroid adenoma. Post operatively, she later developed Hungry Bone Syndrome for which she was given Calcium along with Rocaltrol. She later developed a Splenic Abscess that was drained leading to complete recovery. This is a rare case report of Splenic abscess in a patient with primary hyperparathyroidism.
Keywords: Primary Hyperparathyroidism, Hypercalcemia, Hungry Bone Syndrome, Splenic Abscess
Case Summary
A 46 year-old lady was admitted to the hospital because of Primary Hyperparathyroidism. She was well, until about two years back, when she reported easy fatigability, Arthralgias involving both large and small joints and gradually progressive proximal muscle weakness with no associated swelling of the joints or neck swelling. Four months earlier she slipped while walking and fractured both her hips and hence reported to the hospital for the same. Laboratory studies were performed which revealed high serum calcium (14.3 mg%), low phosphorus levels (2.2 mg%) and raised alkaline phosphatise (2715IU/L) for which she was referred to endocrine section. Other parameters revealed pancytopenia (hemoglobin 8 g%, total leucocyte count 2600/cmm, platelet count 60,000/cmm, normocytic normochromic anaemia), normal liver and renal function tests and sonography of the abdomen. iPTH was found to be raised (1903 pg/ml). Ultrasound of the neck revealed hypoechoic oval soft tissue mass lesion posterior to right lobe of thyroid. She initially refused surgery and Cinacalcet was unaffordable but 2 months later she reported to the hospital with anasarca and decreased urine output. Investigations at that time revealed Anaemia (Hb 8.6 g%), Azotemia (Blood Urea 190 mg%, Serum Creatinine 5.4 mg%) and persistently raised serum calcium and low phosphorus. She recovered from acute renal failure following one session of Hemodialysis and appropriate intravenous fluids. Right Parathyroidectomy was done and during the post operative period, she developed clinical and biochemical features of hypocalcemia and hypophosphatemia. The postoperative albumin-adjusted serum calcium and phosphorus levels were 6.5 mg/dl (N, 8.5–10.2 mg/dl) and 3.0 mg/dl (N, 2.5–4.5 mg/dl), respectively (Hungry Bone Syndrome). iPTH was found to be 36.3 pg/ml with low 24hrs urinary calcium and phosphorus. She was treated with calcium gluconate along with Rocaltrol. Further during the course of hospitalisation she developed persistent unexplained breathlessness, tachypnoea and arterial blood gas analysis revealing metabolic acidosis. She developed minimal left sided pleural effusion and splenomegaly. Pleurocentesis was suggestive of exudative effusion with predominance of mesothelial cells. Ultrasonography and Computed tomographic scan of Chest and Abdomen revealed Pleural effusion and a large splenic abscess with no other significant abnormality. Her liver function tests, hepatitis serology, HIV test and work up for Tuberculosis were found to be negative. Two - D Echocardiography was normal and did not reveal any evidence of vegetations. She was managed with successful percutaneous drainage of the splenic abscess. Aspirated fluid from the abscess and blood cultures was sterile. She recovered completely and during follow up was found to have normal serum calcium and phosphorus levels.
Discussion
This patient, a diagnosed case of Primary Hyperparathyroidism with Parathyroid adenoma had presented with Pre renal acute renal failure following sepsis and dehydration. She improved with dialytic support and surgery for parathyroid adenoma. Later development of breathlessness with localised findings on chest examination and persistent metabolic acidosis was secondary to subsequent development of splenic abscess. Successful management of the splenic abscess by percutaneous drainage ameliorated the above findings,
Use of drugs like Rocaltriol has been documented to cause splenic abscess even in absence of predisposing causes like hemoglobinopathies [4,5], other hematologic disorders (eg, polycythemia vera [5], essential thrombocythemia [8], myeloid leukaemia, trauma, atrial fibrillation or infective endocarditis [3,7]. In the present case, rocaltrol was not given at time of development of features of splenic abscess. Pancytopenia seen in this case was secondary to marrow fibrosis which is known to occur in hyperparathyroidism [2]. Anemia in PHPT is multifactorial, and marrow fibrosis is one of the causes. The underlying mechanism of marrow fibrosis is likely to be related to elevated levels of intact PTH (iPTH). Leucopenia, thrombocytopenia and marrow fibrosis in patients with symptomatic PHPT improve after curative parathyroidectomy. There has only been one case report earlier of splenic abscess without any risk factors with Primary Hyperparathyroidism [1].
Laboratory Data
Date
23/07/12
17/08/12
10/09/12
15/09/12
Hemoglobin
8
9.1
9.0
9.8
Total Leucocyte Count
2600
13,800
9600
7500
Differential Count
P80L15
P78L15
P78L10
P65L24
Platelet
60,000/cmm
2.12 lac
1.72 lac
3.1 lac
MCV
77.1
Blood Urea
146
50
41
22
Serum Creatinine
4.01
1.4
1.4
1.2
Serum Calcium
11.8
6.5
7.0
8.8
Serum Phosphorus
3.6
1.95
1.8
3.5
Serum ALP
1392
2923
876
Serum Albumin
3-65g/dl
iPTH
1903
36.3pg/ml
Ultrasound Abdomen
Mild Hepato splenomegaly renal parenchymal disease
Large Splenic abscess
Ultrasound Neck
Hypoechoic oval mass posterior to right lobe of thyroid
CT Abdomen
Large Splenic abscess
2D ECHO
Normal
Urinary Ca/P/Cr
18 / 26 / 8.2
Table 1: Text here.
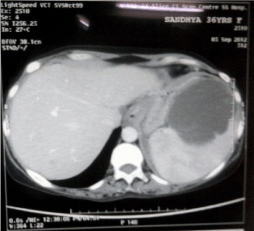
Figure 1: CT Scan showing Splenic Abscess.
Therapy of choice is parathyroidectomy and if refused by the patient cinacalcet can be used [12] although not a definitive answer. In poor patients we have limited in therapeutic options. This patient was later convinced for surgery.
In conclusion, pancytopenia may be a feature of Primary Hyperparathyroidism. The management of hyperparathyroidism may improve leucopenia and thrombocytopenia without significant improvement in anaemia. Splenic abscess may present in a patient with pancytopenia associated with Hyperparathyroidism which should be investigated. Only large splenic abscesses require surgical intervention, however splenectomy may not be necessary in all cases.
References
- C V Nadarajah, I Saif, S A Asghar. An Unusual Cause of Septicemia. Acute Medicine. 2011; 10: 26-28.
- Bhadada SK, Sridhar S, Ahluwalia J, Bhansali A, Malhotra P, Behera A, et al. Anemia and Thrombocytopenia Improves after Curative Parathyroidectomy in a Patient of Primary Hyperparathyroidism (PHPT). J Clin Endocrinol Metab. 2012; 97.
- Bayer AS, Bolger AF, Taubert KA, Wilson W, Steckelberg J, Karchmer AW, et al. Diagnosis and management of infective endocarditis and its complications. Circulation. 1998; 98: 2936-2948.
- Chiang IS, Lin TJ, Chiang IC, Tsai MS. Splenic abscesses: review of 29 cases. Kaohsiung J Med Sci .2003; 19: 510-515.
- Chulay JD, Lankerani MR. Splenic abscess: Report of 10 cases and review of the literature. Am J Med. 1976; 61: 513-522.
- Chang KC, Chuah SK, Changchien CS, Tsai TL, Lu SN, Chiu YC, et al. Clinical characteristics and prognostic factors of splenic abscess: A review of 67 cases in a single medical center of Taiwan. World J Gastroenterol. 2006; 12: 460-464.
- Kim HS, Cho MS, Hwang SH, Ma SK, Kim SW, Kim NH, et al. Splenic abscess associated with endocarditis in a patient on hemodialysis: A case report. J Korean Med Sci. 2005; 20: 313-315.
- Smith MD Jr, Nio M, Camel JE, Sato JK, Atkinson JB. Management of splenic abscess in immunocompromised children. J Pediatr Surg. 1993; 28: 823-826.
- Swamy TK, Balachandar TG, Chandramohan SM, Manohara G, Ali MA. Splenic abscess in a HIV patient. Trop Gastroenterol. 1995; 16: 29-31.
- Piplani S, Ramakrishna, Nandi B, Ganjoo RK, Madan R, Chander BN. Two cases of salmonella splenic abscess. Med J Armed Force India .2006; 62: 77-78.
- Murray AW, Macgregor AB. A case of multiple splenic abscesses managed non-operatively. J R Coll Surg Edinb. 2000; 45: 189-191.
- Marotta V, Di Somma C, Rubino M, Sciammarella C, Del Prete M, Marciello F, et al. Potential role of cinacalcet hydrochloride in sporadic primary hyperparathyroidism without surgery indication. Endocrine. 2014.