
Case Report
Austin J Clin Case Rep. 2015;2(3): 1074.
Twisted Huge Ovarian Cyst: The Clinical Lessons
Muwaffaq Mezeil Telfah*
Department of Surgery, College of Medicine, University of Mosul, Iraq
*Corresponding author: Muwaffaq Mezeil Telfah, Department of Surgery, College of Medicine, University of Mosul, Iraq
Received: September 13, 2014; Accepted: June 04, 2015; Published: June 06, 2015
Summary
A 30 year old woman presented to the surgical outpatient clinic with painless abdominal distension for the last six months. The patient had previous visits to the general practitioner who misinterpreted the case as a truncal obesity and reassurance was given. The basic clinical examination revealed an encysted intra-abdominal fluid occupying most of abdominal cavity. This clinical suspicion proved by imaging studies (Ultrasound and Computed Tomography) as encysted intra-abdominal fluid of unknown aetiology. The patient was given an elective appointment on the next available list. Meanwhile, she developed mild lower abdominal pain treated conservatively and advised to wait for surgery. On the day of surgery, she had normal vital signs and little abdominal physical signs. Per-operatively, a huge twisted right ovarian cystic lesion found treated by tubooophorectomy and delivered intact without spillage via long lower midline incision. The histopathology report revealed mucinous cystadenoma of ovary. The patient had smooth postoperative recovery and was well and pain free during the follow-up.
This case highlights the difficulties that may be encountered in the management of patients with abdominal distension due to encysted intra-abdominal fluid including potential misdiagnosis of the abdominal distension as an obesity. Also, It is a reminder about using basic clinical skills in diagnosing common disorders and taking all the necessary precautions to deal with suspicious intra-abdominal pathology.
Background
The presentations of intra-abdominal pathology are variable and represent a diagnostic challenge for physician [1]. However, back to basic principle is the gold standard to reveal the disease process. Basic clinical and operative skills usually lead to the diagnosis and ensure safe surgery. Every physician must be equipped with the clinical skills to detect intra-abdominal fluid collection and differentiate between encysted and free fluid utilising dull percussion notes, transmitted thrill and shifting dullness clinical tests [2].Occasionally, patients present to outpatient clinic with increasing abdominal distension which may be misinterpreted as a case of obesity. In such cases, all of aetiologies of abdominal distension namely the 6 Fs (Fetus, Flatus, Faeces, Fat, Fluid: free/encysted, large solid tumour e.g. Fibroid) should be considered in the differential diagnosis as a basic clinical knowledge [2]. The ovarian pathology is a common underlying cause for such clinical presentation (encysted intra-abdominal fluid) [3]. Ovarian cysts are a common cause of surgical procedures and hospitalizations among women worldwide. It has been reported that 5% to 10% of women will undergo surgery for an adnexal mass [1, 3]. This pathology should always be kept in mind during the assessment of women with abdominal distension at child bearing age. These pathologies should be treated urgently (preferably at the same admission) to avoid the development of serious complications such as twisting, haemorrhage and rupture [4]. The diagnosis of patients with encysted intra-abdominal fluid may be delayed and only diagnosed after surgical exploration for a vague abdominal mass without any clues to the surgeon whether it is benign or malignant mass.
During surgery, all surgeons should be vigilant and follow the standards of safe surgical skills in dealing with suspicious intraabdominal pathology especially when the pre-operative diagnosis is suspicious and the pathology is cystic. Accordingly, surgeons should be aware of more serious than simple pathology when encounter a huge cystic intra-abdominal pathology. It is important to remove the whole lesion intact without attempt of aspiration to prevent dissemination of fluid and implanting a secondary pathology. The reported case had a difficulty in establishing the initial diagnosis and developed serious complication while on the waiting list. Also, the case required a careful planning for safe surgical treatment.
Case Presentation
A recently married 30 year old woman presented to the outpatient clinic with abdominal distension for six months duration. She was well before marriage. She developed the abdominal distension gradually and it was completely painless. The patient had previous visits to her general practitioner about the condition but she was not investigated well and only received reassurance. She had a recent disturbance in her menstrual cycle (oligomenorrhea to menorrhagia) and had a missed period of three weeks at the time of presentation. Review of all other systems was normal and there were no relevant medical or surgical history. There was no similar cases in the family. Physical examination performed together with an input sought from a gynaecologist. The general examination was normal apart from hirsutism noted on the chin, body mass index (BMI) of 24.9 kg/m2 and hemodynamically stable. Local abdominal examination revealed a symmetrical gross abdominal distension (Figure 1,2), soft, dull percussion notes throughout the abdomen. A positive fluid thrill and negative shifting dullness suggesting encysted intra-abdominal fluid. There was no organomegaly. The bowel sound are positive but distant. Per-vaginal examination done with positive cervical excitation test.
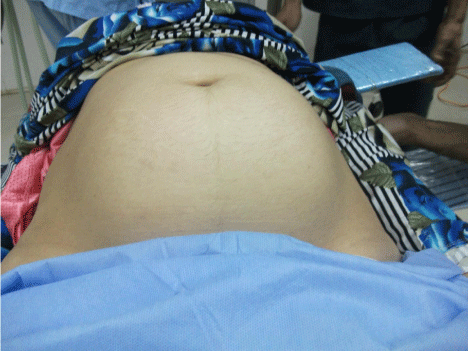
Figure 1: Gross Abdominal Distension ( Anterior View).
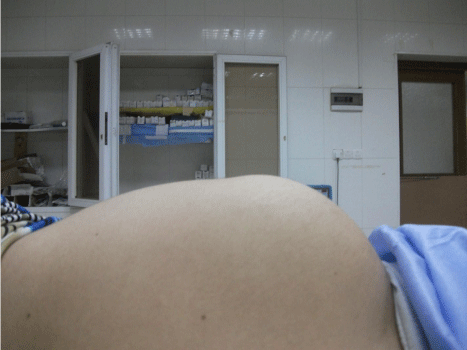
Figure 2: Gross abdominal Distension ( Lateral View ).
Investigations
Routine laboratory workup carried out. There was a negative pregnancy test ( Beta human chorionic gonadotrophine B-HCG), elevated tumor marker of CA125 level= 60 U/ml (elevated above normal range = less than 35). Normal other laboratory test. The full blood count and erythrocyte sedimentation rate (FBC & ESR) were: Hb: 11.4 gm/dl, WBC: 10*104 ,plat.: 200*104 and ESR: 10mm/hr. Liver functions were: TSB:8.2 Mmol/l , ALT & AST:13&20U/l, Alkaline Phosphatase:51 u/l and Total serum protein:62g/l. Renal functions: Urea: 4.8 mmol/l, Creatinine: 70Mmol/l, eelectrolytes: normal, General urine exam was normal. Fasting blood sugar: 5.4mmol/l, LDH: 150 U/l (Normal). Imaging studies performed such as Ultrasound scan and Computed Tomography (Figure 3) showed huge cystic lesion occupying most of the abdominal cavity with contradicting reports suggesting a range of intra-abdominal cystic diseases. No one of these imaging reports was confirmatory.
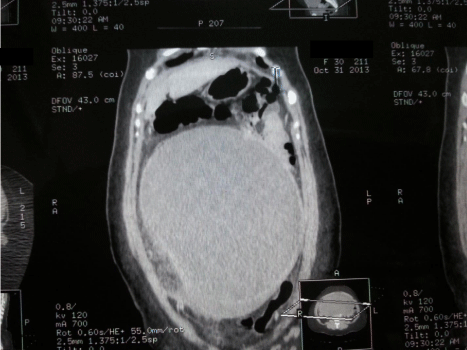
Figure 3: Computed Tomography CT Scan (Oblique Section) Showing Cystic
Lesion Occupying The Abdominal Cavity.
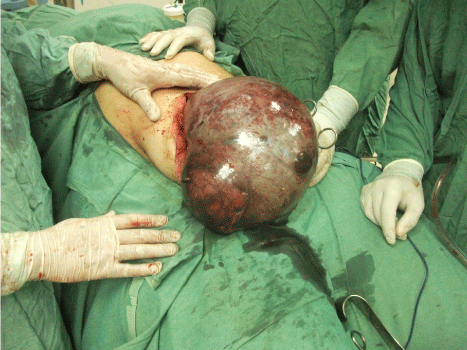
Figure 4: Intra-operative View of Huge Twisted Ovarian Pathology.
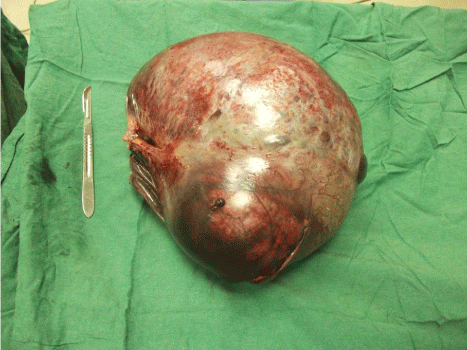
Figure 5: Mucinous Cyst-Adenoma of the Right Ovary (Weight : 7 Kg,
Dimensions: 50 cm x 30 cm x 25 cm).
Differential Diagnosis
Encysted intra-abdominal fluid could be due to:
- Ovarian cyst.
- Omental cyst.
- Mesenteric cyst.
- Encysted fluid of tuberculous (TB) peritonitis.
Treatment
The patient given an appointment for semi-elective surgery on the next available list (ten days ahead). Meanwhile, the patient developed lower abdominal pain which is mild in severity and the patient relatively stable. She visited her general practitioner again and she was given analgesics and reassurance. The patient was not referred back to her surgeon and was advised to wait for her date of surgery. However, on the day of surgery, the patient optimised for her elective surgery and exploration carried out as planned under general anaesthesia. The operative finding were surprising which required an extended lower midline incision. There was a huge right ovarian cystic, ugly looking lesion, dusky and twisted at its pedicle with haemorrhagic fluid in the pelvis to which right tubooophorectomy performed. The mass measured about 50 cm x 30 cm x 25 cm and weight 7.0 Kilogram (Figure 4,5). There was a normal left ovary and normal looking vermiform appendix. The presentation would mandate an emergency surgery rather than elective but how the patient tolerate such burden with hemodynamic stability is unexplained physiologically, pathologically and logically! Hence, we report this case.
Outcome and follow-up
She had a smooth postoperative recovery and discharged home after five days. The pathologist did aspiration of the mass and found a thick gelatinous material then dissection made to the mass to take samples from the wall. Histology confirmed a mucinous cystadenoma of the right ovary (benign tumour that arises from the surface epithelium of the ovary). She is well after one year of regular follow-up.
Discussion
Abdominal distension is a common presenting complaint to the surgeons. Systematic approach of evaluation is of paramount importance to have an accurate diagnosis. Encysted intra-abdominal fluid collection is a special challenging presentation which can be misinterpreted for any aetiology of abdominal distension [3]. It is frequently described that ovarian cysts can present as an overt abdominal distension to which basic physical examination will suggest the clinical diagnosis. Occasionally, ovarian cysts may be misdiagnosed as tense ascitis with diagnostic difficulties [5]. Our case had been misdiagnosed as a case of truncal obesity due to failure of application of basic clinical skills to detect intra-abdominal fluid and differentiate between encysted and free fluid. Huge ovarian cysts are liable to several complications such as torsion, haemorrhage and rupture [4]. In these patients, any new complaint should lower the threshold for early intervention to treat serious complications despite having normal vital signs especially in young patients with excellent physiological reserve and high threshold for pain [4]. Our case developed a twisted ovarian cyst while in the waiting list which passed un-noticed for unknown reason. This case is a lesson that young patients may have a high threshold of pain which enable them to tolerate twisting of huge cyst without hemodynamic instability. Equally important, patients with large, vague intra-abdominal cystic Lesion (encysted fluid) should have more active and urgent action (preferably intervention on the same admission) to avoid serious and life threatening complications. The management of vague intra-abdominal masses requires dynamic critical thinking which is an essential element of safe surgeons. Due to the fact that a disease process (Especially if cystic mass with malignant potential ) may be disseminated to other sites if ruptured during surgical removal, it is important to excise the lesion completely without rupture. The intraabdominal mass of the reported case retrospectively proved to be mucinous cyst-adenoma of ovary. Ovarian mucinous cystadenoma constitute 15 % of all ovarian tumours. It tends to be huge in size, multi-locular cyst with smooth outer and inner surfaces. Eighty percentage are benign, 10% are border-line and 10% are malignant [6]. As it is rich in mucinous fluid, its rupture can lead to mucin deposits on the peritoneum and results in pseudo-myxoma peritonei [7]. Every attempt was made to deliver the whole cystic lesion unruptured and excised totally even at expense of generous abdominal incision and its poor cosmetic results.
YE et al suggested in their review about managing giant ovarian pathologies that adequate removal of lesions with avoidance of accidental mass rupture is vital for safe surgery [8]. Hence, Any trial of aspiration must be prohibited in these doubtful cases to avoid a possible complication of pseudomyxoma peritonei in case of association with a mucinous ovarian tumour whether primary or more commonly secondary [9, 10]. This was applicable to our case who had vague cystic intra-abdominal mass together with elevated CA125 level, both of which suggestive of malignancy. However, CA-125 is unreliable in differentiating malignant from benign ovarian tumours in premenopausal women because of the increased rate of false positives and reduced specificity [11]. Cancer Antigen (CA) 125 levels require a cautious planning in patients without a notable tumour mass. Since an increased CA 125 level is a marker of ovarian cancer, a laparotomy is usually indicated to clarify the etiology. However, unnecessary explorations have been reported in the literature revealing no ovarian pathology in such patients [12].
Based on this concept, exploratory laparotomy performed for our patient which is proved retrospectively to be a benign mucinous cyst adenoma of the ovary to which all of the safety precautions applied and the lessons taken.
Learning Points/Take home messages
The clinical lessons learned from this case are:
- Abdominal distension is a common clinical scenario which needs careful systematic approach to verify the underlying cause.
- The basic clinical skills of dullness, positive fluid thrill and negative shifting dullness are the gold standard to detect encysted intra-abdominal fluid.
- Cystic intra-abdominal lesions should be dealt with urgently prior to development of more serious complications especially if new complaints developed.
- Cystic lesions specifically ovarian pathology should be removed safely without rupture even at expense of poor cosmetic results of large incisions.
- Aspiration of cystic lesions should be strongly discouraged especially in suspicious pathology to prevent development of secondary pathology.
Patient’s Perspective
The patient felt unlucky to have two delays in her management. First, when her GP was unable to detect the cyst early in the course of the disease when he misinterpreted the case as an obesity. Secondly, when no emergency action done upon detection of the cyst and more importantly when a little delay has subjected her life to constant threat. The situation has been explained to the patient as she has very unusual clinical presentation when she developed a complication in the cyst with little alarming signs.
References
- Sabiston DC, Townsend CM. Acute abdomen. Sabiston textbook of surgery: the biological basis of modern surgical practice. 18th ed. Philadelphia: Saunders/Elsevier; 2008; 1180–1196.
- Browse NL, Black J, Burnand KG, Thomas W EG. Browse's Introduction to the Symptoms and Signs of Surgical Diseases: Abdominal Distension. 4th ed. Oxford: Hodder Arnold;2005.
- Hilger, Wesley S, Magrina, Javier F, Magtibay, Paul M. Laparoscopic management of the adnexal mass. Clin Obstet Gynecol. 2006; 49: 535-548.
- Katz VL. Benign gynecologic lesions: vulva, vagina, cervix, uterus, oviduct, ovary. In: Katz VL, Lentz GM, Lobo RA, Gershenson DM, eds. Comprehensive Gynecology. 5th ed. Philadelphia, PA: Mosby; 2007; 419-471.
- Menahem S, Shvartzman P. Giant ovarian cyst mimicking ascites. J Fam Pract. 1994; 39: 479-481.
- Young RH: The ovary. In Sternberg's Diagnostic Surgical Pathology. Edited by Mills SE, Carter D, Greenson JK, Reuter E. Raven Press, NY; 2009; 2195.
- Buell-Gutbrod R, Gwin K. Pathologic diagnosis, origin, and natural history of pseudomyxoma peritonei. Am Soc Clin Oncol Educ Book 2013; 221–225.
- Long-Yun Ye, Jing Wang, DA- Ren Liu, Guo-Ping Ding and Li-ping. Management of giant ovarian teratoma: A case series and review of the literature. Oncol Lett. 2012; 4: 672–676.
- Rouzbahman M, Chetty R. Mucinous tumours of appendix and ovary: an overview and evaluation of current practice. J Clin Pathol. 2014; 67: 193-197.
- Dong Y, Li T, Zou W, et al. Pseudomyxoma peritonei: report of 11 cases with a literature review. Zhonghua Bing Li Xue Za Zhi. 2002; 31: 522-525.
- Sturgeon CM, Lai LC, Duffy MJ; Serum tumour markers: how to order and interpret them. BMJ. 2009; 339: b3527. doi: 10.1136/bmj.b3527.
- Sevinc A, Camci C, Turk HM, Buyukberber S. How to interpret serum CA 125 levels in patients with serosal involvement? A clinical dilemma. Oncology. 2003; 65: 1-6.