
Case Report
Austin J Clin Case Rep. 2015; 2(4): 1078.
Ileocecal Burkitt Lymphoma Following Chemotherapy and Radiotherapy for Rectum Cancer
Bazoukis G¹*, Fytrakis N¹, Boukas K¹, Spiliopoulou A¹, Florou K¹, Kaperda A¹, Thrappas J¹, Michelongona P², Fragkou A¹, Savvanis S¹ and Yalouris A¹
¹Department of Internal Medicine, General Hospital of Athens Elpis, Greece
²Department of Otorhinolaryngology, University Hospital of Patras, Greece
*Corresponding author: Bazoukis G, Department of Internal Medicine, General Hospital of Athens Elpis, Greece
Received: September 10, 2015; Accepted: November 02, 2015; Published: November 04, 2015
Abstract
Introduction: Burkitt lymphoma (BL) is an uncommon form of non-Hodgkin lymphoma in adults. It is a rapidly growing tumor with poor prognosis. The endemic form of the disease commonly appears with abdominal pain and symptoms of bowel obstruction. In our case we present a patient with ileocecal BL following chemotherapy and radiotherapy for rectum adenocarcinoma.
Case Presentation: A 56-years-old man presented at the emergency department complaining of atypical abdominal pain since a week. The medical history of the patient included rectum adenocarcinoma treated with low anterior resection followed by chemotherapy and radiotherapy. The clinical examination revealed a palpable abdominal mass at the right iliac region. Further exams revealed ileocecal BL.
Discussion: BL is a rare cause of abdominal pain in adults. Ileocecal region is commonly affected by the disease. Epstein Barr virus and HIV are the main risk factors for BL. The previous history of chemotherapy and radiotherapy could be potential risk factors for BL and must increase the clinical suspicion of the disease. Rapid initiation of appropriate treatment is the cornerstone for a better outcome.
Keywords: Burkitt lymphoma; Chemotherapy complications; Radiotherapy complications; Rectum adenocarcinoma; Ileocecal mass
Introduction
Burkitt lymphoma (BL) was first noted in African children by Dennis Burkitt in 1958 [1]. BL is a B-cell lymphoma with an extremely short doubling time and BL patients often present with bulky disease and a high tumor burden [2]. There are three clinical settings of the disease: endemic, sporadic and immunodeficiency-related [3]. In the non-endemic cases of BL, abdominal mass is a common finding at the first medical examination [4]. Similarly to other gastrointestinal (GI) lymphomas, extranodal BL appears more frequently in the stomach followed by small and large intestines, especially at the ileocecal area [2]. Other sites are bone marrow, liver, spleen, central nervous system and rarely skin, eyes, thyroid, bones and breasts [2,5]. The diagnosis of GI lymphoma is difficult because of the small size of biopsies and the confusion between the benign lymphoid proliferations of GI tract [3]. In our report we present a case of ileocecal BL in a patient with a previous history of rectum adenocarcinoma.
Case Presentation
A 56-years-old man from Albania who lived in Greece for the last ten years, presented at the emergency department complaining of atypical abdominal pain since a week with progressive worsening. The medical history of the patient included moderately differentiated adenocarcinoma of the rectum without metastasis diagnosed in 2005 treated with low anterior resection and colorectal anastomosis followed by chemotherapy and radiotherapy. Unfortunately, the exact medication that was followed was not clearly stated at his medical records. The clinical examination of the abdomen showed a palpable mass at the right iliac region. The only abnormal finding in laboratory exams was elevated LDH levels (809 IU/l [normal values: 81-225]) without anemia. The patient was HIV negative but was not tested for EBV antibodies. Chest x-ray was normal. Abdominal ultrasound failed to reveal any pathology. Abdominal CT scan after gastrografin per os, revealed a mass with soft tissue density that occupied almost all the lower abdomen in contact with the caecum and caused significant stenosis of its lumen as well as thickening of the greater omentum (omentum cake) (Figure 1). In Coloscopy a mass in the ileocecal region causing significant stenosis of the lumen was found (Figure 2). Histological examination showed infiltration of the intestinal mucosa by a high grade B cell non-Hodgkin lymphoma (NHL) with morphological and immunological characteristics of BL (CD20+, Ki-67 100%, BCL2-, CD3 -, C-MYC +). Unfortunately, our patient died before the results of the biopsy.
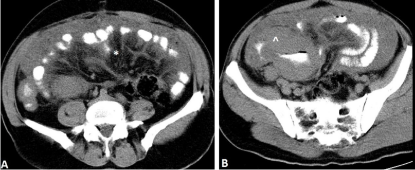
Figure 1: The computed tomography of the abdomen after gastrografin per
os, revealed thickening of the greater omentum (omentum cake) [symbolized
with * in figure A] and a mass with soft tissue density that occupied almost all
the lower abdomen in contact with the caecum caused significant stenosis of
the lumen [symbolized with ^ in figure B].
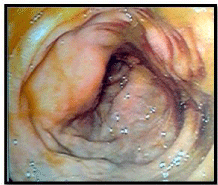
Figure 2: Endoscopic views showing a mass causing narrowing of the lumen
of the terminal ileum. Biopsies of the mass region were obtained.
Discussion
The GI tract is the most common site of extra nodal lymphoma accounting for 5%-20% of all cases [6-8]. On the other hand, primary GI lymphomas represent 5% to 10% of primary GI neoplasms [3]. Stomach is the most frequent position for GI lymphomas (50-60%) followed by small intestine (30%) and large intestine (10%) while oral and esophageal lymphomas are very rare [3,9]. Primary involvement of the Ileocecal region in NHL is rare with a frequency ranging from 11.5% to 37.1% of all intestinal NHLs and 2.4% to 22% of all GI tract NHLs [9]. The most frequent type of GI lymphomas is diffuse large B cell lymphomas [3,6,8]. Abdominal pain, anemia, anorexia, diarrhea, constipation, mass hemorrhage, B symptoms (fever, night sweats and weight loss) and elevated LDH consist the usual presentation of GI lymphomas [7,10]. Ileocecal lymphomas often present with complications such as intestinal obstruction and intussusceptions which require surgical intervention on an emergency basis [9,11]. BL is an uncommon form of NHL in adults, with an incidence of approximately 1200 patients per year in the United States [12]. The incidence rates of NHL are low in Albania for both men and women [13]. The endemic form of BL is most commonly seen in equatorial Africa with jaw and facial bone involvement [14]. The sporadic form of the disease most often appears as abdominal mass with bone marrow involvement [12]. Immunodeficiency-related BL cases present with nodal or extra nodal involvement with frequent bone marrow involvement [15]. BL usually presents as a bulky mass in the right lower quadrant [8]. However, atypical presentations of the disease have been reported [16-21]. Ileocecal area is a common region affected by sporadic BL [2,14]. In children, ileocecal BL can appear as acute appendicitis [22,23]. Risk factors for BL include Epstein Barr virus (EBV), malaria, HIV, low socioeconomic level and herbal exposure (Euphorbiaceae species) [14]. Patients with endemic type BL are EBV positive with a ratio of 95%, while this ratio is only 15% in patients with the sporadic-type [5]. Chemotherapy and radiotherapy for rectum cancer could be potential risk factors for secondary ileocecal BL [24-26]. On our patient, the time between finishing the treatment for rectum cancer and appearance of Burkitt lymphoma was about eight years. The definitive treatment of BL includes surgical procedures especially in cases of bowel obstruction and intensive chemotherapy. Radical resection before chemotherapy should be considered in early-stage ileocecal NHL to achieve a better survival [9]. CODOX-M/IVAC (Cyclophosphamide, vincristine, doxorubicin and high dose methotrexate, alternating with ifosfamide, etoposide, and cytarabine) and hyper-CVAD (modified fractioned Cyclophosphamide, vincristine, doxorubicin and dexamethasone) chemotherapy are commonly used to treat BL [27]. Rituximab, a recombinant antibody that targets CD20 on the surface of B lymphocytes, is often added to CODOX-M/IVAC and hyper-CVAD protocols [27,28].
Conclusion
BL is a rapidly growing tumor with poor prognosis. Regardless of the low frequency of sporadic BL in adults, the clinician must be highly suspected of the disease in any abdominal masses especially in the ileocecal region. The history of previous chemotherapy or radiotherapy could be a potential risk factor for the development of BL. Treatment should be initiated as soon as possible for accomplishing a better prognosis.
References
- Burkitt D. A sarcoma involving the jaws in African children. Br J Surg. 1958; 46: 218-223.
- Jang SJ, Yoon DH, Kim S, Yoon S, Kim DY, Park CS, et al. A unique pattern of extranodal involvement in Korean adults with sporadic Burkitt lymphoma: a single center experience. Ann Hematol. 2012; 91: 1917-1922.
- O'Malley DP, Goldstein NS, Banks PM. The recognition and classification of lymphoproliferative disorders of the gut. Hum Pathol. 2014; 45: 899-916.
- Kohno S, Ohshima K, Yoneda S, Kodama T, Shirakusa T, Kikuchi M. Clinicopathological analysis of 143 primary malignant lymphomas in the small and large intestines based on the new WHO classification. Histopathology. 2003; 43: 135-143.
- Kiresi D, Karabekmez LG, Koksal Y, Emlik D. A case of Burkitt lymphoma re-presenting as periportal hepatic and multiple organ infiltration. Clin Lymphoma Myeloma. 2008; 8: 59-61.
- Geramizadeh B, Keshtkar Jahromi M. Primary extra nodal gastrointestinal lymphoma: a single center experience from southern Iran - report of changing epidemiology. Arch Iran Med. 2014; 17: 638-639.
- Li M, Zhang S, Gu F, Xiao W, Yao J, Chao K, et al. Clinicopathological characteristics and prognostic factors of primary gastrointestinal lymphoma: a 22-year experience from South China. Int J Clin Exp Pathol. 2014; 7: 2718-2728.
- Ghimire P, Wu GY, Zhu L. Primary gastrointestinal lymphoma. World J Gastroenterol. 2011; 17: 697-707.
- Zhai L, Zhao Y, Lin L, Tian Y, Chen X, Huang H, et al. Non-Hodgkin's lymphoma involving the ileocecal region: a single-institution analysis of 46 cases in a Chinese population. J Clin Gastroenterol. 2012; 46: 509-514.
- Parente F, Anderloni A, Greco S, Zerbi P, Bianchi Porro G. Ileocecal Burkitt's lymphoma. Gastroenterology. 2004; 127: 8, 368.
- Szabo A, Farkas P, Laszlo A, Berczi L, Sperlagh M, Sugar I. [Ileocecal intussusception caused by Burkitt lymphoma, cause of mechanical ileus]. Magy Seb. 2003; 56: 116-119.
- Perkins AS, Friedberg JW. Burkitt lymphoma in adults. Hematology Am Soc Hematol Educ Program. 2008; 341-348.
- Ferlay J, Steliarova-Foucher E, Lortet-Tieulent J, Rosso S, Coebergh JW, Comber H, et al. Cancer incidence and mortality patterns in Europe: estimates for 40 countries in 2012. Eur J Cancer. 2013; 49: 1374-1403.
- Orem J, Mbidde EK, Lambert B, de Sanjose S, Weiderpass E. Burkitt's lymphoma in Africa, a review of the epidemiology and etiology. Afr Health Sci. 2007; 7: 166-175.
- Johnson DH, Reske T, Ruiz M. Case Report and Review of Immunodeficiency-Associated Burkitt Lymphoma. Clin Lymphoma Myeloma Leuk. 2015.
- Legault S, Couture C, Bourgault C, Bergeron S, Poirier P, Senechal M. Primary cardiac Burkitt-like lymphoma of the right atrium. Can J Cardiol. 2009; 25: 163-165.
- Mondal SK, Bera H, Mondal S, Samanta TK. Primary bilateral ovarian Burkitt's lymphoma in a six-year-old child: report of a rare malignancy. J Cancer Res Ther. 2014; 10: 755-757.
- Ziade F, von der Weid N, Beck-Popovic M, Nydegger A. Burkitts's lymphoma--an atypical presentation. BMC Pediatr. 2012; 12: 113.
- Tzachanis D, Dewar R, Luptakova K, Chang JD, Joyce RM. Primary cardiac burkitt lymphoma presenting with abdominal pain. Case Rep Hematol. 2014; 2014: 687598.
- Palakodeti S, Hoda K, Munroe CA. Perirectal Burkitt lymphoma presenting as an uncommon cause of lower gastrointestinal bleeding. Clin Gastroenterol Hepatol. 2014; 12: A23-24.
- Fadiora SO, Mabayoje VO, Aderoumu AO, Adeoti ML, Olatoke SA, Oguntola AS. Generalised Burkitt's lymphoma involving both breasts--a case report. West Afr J Med. 2005; 24: 280-282.
- Weledji EP, Ngowe MN, Abba JS. Burkitt's lymphoma masquerading as appendicitis--two case reports and review of the literature. World J Surg Oncol. 2014; 12: 187.
- Wang SM, Huang FC, Wu CH, Ko SF, Lee SY, Hsiao CC. Ileocecal Burkitt's lymphoma presenting as ileocolic intussusception with appendiceal invagination and acute appendicitis. J Formos Med Assoc. 2010; 109: 476-479.
- Krishnan B, Morgan GJ. Non-Hodgkin lymphoma secondary to cancer chemotherapy. Cancer Epidemiol Biomarkers Prev. 2007; 16: 377-380.
- Birgisson H, Pahlman L, Gunnarsson U, Glimelius B. Occurrence of second cancers in patients treated with radiotherapy for rectal cancer. J Clin Oncol. 2005; 23: 6126-6131.
- Hatami M, Whitney K, Goldberg GL. Primary bilateral ovarian and uterine Burkitt's lymphoma following chemotherapy for breast cancer. Arch Gynecol Obstet. 2010; 281: 697-702.
- Alwan F, He A, Montoto S, Kassam S, Mee M, Burns F, et al. Adding rituximab to CODOX-M/IVAC chemotherapy in the treatment of HIV-associated Burkitt lymphoma is safe when used with concurrent combination antiretroviral therapy. AIDS. 2015.
- Hong J, Kim SJ, Ahn JS, Song MK, Kim YR, Lee HS, et al. Treatment Outcomes of Rituximab Plus Hyper-CVAD in Korean Patients with Sporadic Burkitt or Burkitt-like Lymphoma: Results of a Multicenter Analysis. Cancer Res Treat. 2014.