
Case Report
Austin J Clin Case Rep. 2015; 2(4): 1079.
Trimethoprim-Sulfamethoxazole Induced Rash, Febrile Neutropenia and Aseptic Meningoencephalitis
Vazquez de Lara F¹, Goins WP², Hernandez-Vila E³ and Hernandez-Vila EA³*
¹Department of Internal Medicine, Hospital Angeles Puebla, Mexico
¹Division of Infectious Diseases, Department of Medicine, Baylor College of Medicine, USA
³Department of Cardiology, Texas Heart Institute, USA
*Corresponding author: Eduardo Hernandez- Vila, Department of Cardiology, Texas Heart Institute, Houston, USA
Received: September 26, 2015; Accepted: October 30, 2015; Published: November 02, 2015
Abstract
Trimethoprim-sulfamethoxazole (TMP-SMX) is a commonly prescribed antibiotic that is associated with a number of adverse reactions that can be potentially life threatening. We report a case of a 30-year-old woman who presented with rash, febrile neutropenia and aseptic meningoencephalitis after finishing a course of TMP-SMX. To our knowledge, this is the first report of an otherwise healthy patient presenting with these conditions simultaneously.
Keywords: Trimethoprim-sulfamethoxazole combination; Aseptic meningitis; Aseptic meningoencephalitis; Febrile neutropenia; Exanthema
Case Presentation
A 30-year-old woman presented to the emergency department with a pruritic rash and fever. Six days before presentation she underwent augmentation mammoplasty and abdominoplasty. The patient was started on doxycycline and trimethoprim-sulfamethoxazole (TMPSMX) three days prior to surgery and continued it five days postoperatively because of a previous history of recurrent impetigo with methicillin-resistant Staphylococcus aureus. During her last day of taking the antibiotic she developed a diffuse rash, fever and chills.
On admission her temperature was 37.8 °C, blood pressure 108/73, pulse 115 beats per minute, respiratory rate 16 per minute, and oxygen saturation 99% on room air. The patient had no significant past medical history. She denied headaches, vision changes, nausea or vomiting. She complained only of mild constipation. Physical examination revealed a blanching patchy rash distributed primarily in the face, back, chest and abdomen (Figure.1). Incision sites were without erythema, swelling, fluctuance or drainage. The remainder of her examination was unremarkable. Laboratory analysis revealed mild thrombocytopenia and marked leukopenia of 0.5 x 10³ cells/μl (Reference: 3.4-10.8 x 10³ cells/μl) with an absolute neutrophil count (ANC) of 0.22 x 10³ cells/μl (Reference: 1.4–7.0 x 10³ cells/μl). HSV and VZV PCR from CSF and initial screening for CMV and influenza were negative. The patient was admitted with the diagnosis of febrile neutropenia for which she received cefepime, vancomycin, and one dose of filgrastim, a granulocyte colony-stimulating factor (G-CSF) analog. TMP-SMX had already been discontinued prior to hospital admission.
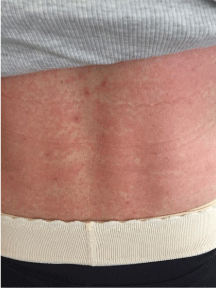
Figure 1: Photograph taken on the day of admission depicting the rash.
The patient developed a blanching and pruritic macular rash distributed
primarily in the face, back, chest and abdomen during her last day of taking
TMP-SMX.
On the second day of admission the neutropenia improved; however, the patient developed confusion, agitation, difficulty with expression, and fluent aphasia. She also complained of mild headache and neck pain. Neurologic examination showed orientation only to person and inability to follow two-step commands. Cranial nerve and fundoscopy examination were within normal limits, and no focal deficits were observed. Lumbar puncture revealed clear and colorless cerebrospinal fluid (CSF) with 6 WBCs/mm³ with lymphocyte predominance, increased protein of 263 mg/dL, and a normal glucose level. Cultures, bacterial latex agglutination test and cryptococcal antigen of the CSF were negative. Magnetic resonance imaging of the brain showed cerebral sulcal and cerebellar folial signal changes, as well as temporal lobe and white matter signal abnormalities consistent with meningoencephalitis (Figure.2).

Figure 2: Brain MRI taken on the 2nd hospital day when altered mental status
was observed. Brain MRI demonstrated nonspecific perivascular white
matter changes that can be seen in meningitis, meningoencephalitis, chronic
vascular disease, multiple sclerosis and vasculitis among other etiologies.
The patient was transferred to the medical intensive care unit; dexamethasone and intravenous acyclovir were started because of the concern of herpes simplex encephalitis. The fever and neutropenia resolved by the third day and the rash had almost completely disappeared. All cultures remained negative throughout the patient’s hospital stay. Her neurological symptoms gradually started to resolve on the next day after their onset. The patient was discharged on the sixth day of admission with complete resolution of all her symptoms.
Discussion
Trimethoprim-sulfamethoxazole is a combination antibiotic of the sulfonamide family that is very commonly prescribed despite having a wide variety of adverse effects [1]. These range from relatively mild gastrointestinal disturbances, such as nausea and vomiting, to more serious dermatologic, hematologic and central nervous system reactions [2-4]. We searched MEDLINE and MeSH databases utilizing the search terms trimethoprim-sulfamethoxazole combination, aseptic meningitis, aseptic meningoencephalitis, febrile neutropenia, and exanthema and we found no articles describing these three conditions presenting simultaneously in a patient.
Dermatologic reactions to TMP-SMX may occur in up to 4% of patients exposed to this drug. Approximately 75% of all untoward effects attributed to TMP-SMX are dermatologic, and these include toxic epidermal necrolysis and Stevens-Johnson syndrome [1,5]. Hematologic reactions include aplastic, hemolytic, and macrocytic anemias (particularly in the setting of folate deficiency); thrombocytopenia; leukopenia; and coagulation disorders [4,6].
Drug induced neutropenia is a serious condition that has been linked with almost every class of medications, including TMP-SMX. Neutropenia can be categorized as severe when the ANC is below 0.5 x 109 cells/L, and at this level the term drug induced agranulocytosis (DIA) is used [7]. Patients with DIA usually present with fever, chills and mylagia. If not treated promptly, DIA carries a great risk of developing septicemia [8]. Aggressive treatment of DIA with administration of broad-spectrum antibiotics and discontinuation of the offending agent is the mainstay of treatment, since this condition carries a mortality rate of 5% [8]. The use of G-CSF agents is controversial, and evidence-based recommendations are lacking. Nevertheless, its use has been advocated in high risk patients and those with a severely decreased ANC, due to the increased risk of morbidity and mortality that this condition confers [7]. In our case, the patient’s leukopenia promptly resolved after one dose of filgrastim during the first 24 hours after presentation, although it may not be effective in all cases [4].
Drug induced aseptic meningitis (DIAM) is a rare hypersensitivity reaction of the CNS that is associated with non-steroidal antiinflammatory drugs, immuno modulating agents and antibiotics. TMP-SMX is the most common antibiotic implicated in cases of aseptic meningitis and the diagnosis is always challenging [3]. The clinical presentation of aseptic meningitis is variable and difficult to differentiate from infectious meningitis. Patients may present with headache or neck pain, fever, nausea and vomiting. Generalized weakness and speech changes have also been reported, as well as neuropsychiatric alterations such as delirium and psychosis, particularly in the elderly population [9]. Other serious but less common neurologic manifestations include generalized tonic-clonic seizures, myoclonic jerks, unconsciousness and coma [3].
In order to appropriately diagnose DIAM, CSF analysis and imaging, such as computed tomography and MRI of the brain, are needed to rule out other potential causes. CSF usually contains moderately elevated WBC counts, markedly elevated protein levels with normal glucose and eosinophilic levels in most cases [3,10]. The term aseptic meningitis implies that a nonbacterial etiology is responsible for the meningeal inflammation. In order to make the diagnosis, CSF analysis must lack the classic signs of bacterial infection including a negative Gram stain and culture [11].
In our case, parasitic, viral and fungal etiologies of aseptic meningitis and encephalitis were reasonably excluded due to lack of risk factors and because all bacterial cultures and PCR viral studies were negative. The rapid recovery that our patient demonstrated was also more consistent with a drug-induced condition [3]. We also considered DRESS (drug rash with eosinophilia and systemic symptoms) syndrome and immune reconstitution inflammatory syndrome as alternative diagnoses. However, the absence of eosinophilia and the lack of evidence of an infectious etiology ruled these possibilities out [12,13].
Several mechanisms have been postulated by which TMPSMX produces many of these adverse reactions. Immune mediated idiosyncratic and classic hypersensitivity reactions, such as type II, III and IV, have been implicated in the cutaneous, hematologic and CNS abnormalities caused by this drug. This drug is well known to cross the blood brain barrier and this may contribute to its numerous neurological adverse effects [14]. Of note, acute elevations of IL-6 have been described in patients with signs of meningeal irritation, fever, malaise, head and backache [15,16]. In other cases the pathophysiology may not be as clear, and direct toxicity, immune complex deposition, induction of auto antibodies and oxidative stress have been postulated as the culprits in cases of thrombocytopenia, hemolysis and renal damage [10,17].
In summary, our patient presented with a diffuse blanching erythematous and pruritic rash, fever, and leukopenia. She developed altered mental status and signs of meningeal irritation within the first 24 hours of hospital admission with a clinical course most consistent with a drug-induced reaction. Generally well-tolerated, TMP-SMX has a long history of being useful in many clinical scenarios because of its low cost and effectiveness. However, clinicians should be aware of all the potential adverse reactions of this commonly prescribed antibiotic. Considering some of these may be life threatening, we believe careful monitoring is needed in all patients receiving this medication.
References
- Masters PA, O'Bryan TA, Zurlo J, Miller DQ, Joshi N. Trimethoprim-sulfamethoxazole revisited. Archives of internal medicine. 2003; 163: 402-410.
- Cairns B, Rich M. Fever, rash, and peeling skin. The Journal of family practice. 2011; 60: 9-12.
- Bruner KE, Coop CA, White KM. Trimethoprim-sulfamethoxazole-induced aseptic meningitis-not just another sulfa allergy. Annals of allergy, asthma & immunology: official publication of the American College of Allergy, Asthma, & Immunology. 2014; 113: 520-6.
- Kocak Z, Hatipoglu CA, Ertem G, Kinikli S, Tufan A, Irmak H, et al. Trimethoprim-sulfamethoxazole induced rash and fatal hematologic disorders. The Journal of infection. 2006; 52: 49-52.
- See S, Mumford JM. Trimethoprim/sulfamethoxazole-induced toxic epidermal necrolysis. The Annals of pharmacotherapy. 2001; 35: 694-697.
- Goodman LS, Gilman A, Brunton LL. Goodman & Gilman's manual of pharmacology and therapeutics. New York: McGraw-Hill Medica. 2008.
- Andres E, Maloisel F, Zimmer J. The role of haematopoietic growth factors granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor in the management of drug-induced agranulocytosis. British journal of haematology. 2010; 150: 3-8.
- Pick AM, Nystrom KK. Nonchemotherapy drug-induced neutropenia and agranulocytosis: could medications be the culprit? Journal of pharmacy practice. 2014; 27: 447-452.
- McCue JD, Zandt JR. Acute psychoses associated with the use of ciprofloxacin and trimethoprim-sulfamethoxazole. The American journal of medicine. 1991; 90: 528-529.
- Repplinger MD, Falk PM. Trimethoprim-sulfamethoxazole-induced aseptic meningitis. The American journal of emergency medicine. 2011; 29: 242 e3-5.
- Lockwood JR, Carr D. Drug-induced aseptic meningitis secondary to trimethoprim / sulfamethoxazole: a headache to be aware of. Cjem. 2014; 16: 421-424.
- Criado PR, Avancini J, Santi CG, Medrado AT, Rodrigues CE, de Carvalho JF. Drug reaction with eosinophilia and systemic symptoms (DRESS): a complex interaction of drugs, viruses and the immune system. The Israel Medical Association journal: IMAJ. 2012; 14: 577-582.
- Zaffiri L, Verma R, Struzzieri K, Monterroso J, Batts DH, Loehrke ME. Immune reconstitution inflammatory syndrome involving the central nervous system in a patient with HIV infection: a case report and review of literature. The new microbiologica. 2013; 36: 89-92.
- Wambulwa C, Bwayo S, Laiyemo AO, Lombardo F. Trimethoprim-sulfamethoxazole-induced aseptic meningitis. Journal of the National Medical Association. 2005; 97: 1725-8.
- Antonen J, Saha H, Hulkkonen J, Lumio J, Pasternack A, Hurme M. Increased in vitro production of interleukin 6 in response to Trimethoprim among persons with Trimethoprim induced systemic adverse reactions. The Journal of rheumatology. 1999; 26: 2585-2590.
- Antonen J, Hulkkonen J, Pasternack A, Hurme M. Interleukin 6 may be an important mediator of trimethoprim-induced systemic adverse reaction resembling aseptic meningitis. Archives of internal medicine. 2000; 160: 2066-2067.
- Ho JM, Juurlink DN. Considerations when prescribing trimethoprim-sulfamethoxazole. CMAJ: Canadian Medical Association journal = journal de l'Association medicale canadienne. 2011; 183: 1851-1858.