
Case Report
Austin J Clin Case Rep. 2017; 4(2): 1117.
Acute Pancreatitis: A Complication of Jejunostomy Tube
Ansari J, Anwar S and Agrawal S*
Department of Gastroenterology, Wright State University Boonshoft School of Medicine, USA
*Corresponding author: Agrawal S, Department of Gastroenterology, VA Medical Center, Wright State University,4100 W 3rd St, Dayton, OH 45428, USA
Received: January 10, 2017; Accepted: March 30, 2017; Published: April 10, 2017
Abstract
We have seen cases in the past where gastrostomy tube migration resulted in pancreatitis by obstruction of the sphincter of Oddi. We report a case of a 60-year-old male who presented to the hospital for malfunctioning jejunostomy tube. Patient had elevated lipase and liver enzymes on presentation. Endoscopic retrograde cholangiopancreatography confirmed extrinsic compression of ampulla of Vater by jejunostomy without filling defects in the biliary tree. After removal of the jejunostomy tube patient felt significantly better and was ultimately discharged.
Keywords: Acute obstructive pancreatitis; Jejunostomy tube; Common Bile Duct (CBD)
Introduction
Feeding tubes is the preferred root for long term feeding of patients who cannot be fed orally [1]. Acute Obstructive Pancreatitis (AOP) caused by gastrostomy tube migration and Sphincter of Oddi obstruction has been described in a few case reports previously. We describe a case of an elderly nursing home resident who presented with acute pancreatitis caused by extrinsic compression of Ampulla of Vater by a Jejunostomy Tube (JT). A comprehensive literature review was performed using medline and pubmed which revealed that no case thus far has been reported. This case serves to educate the importance of early recognition and management of this unusual complication.
Case Presentation
A 60 year-old male nursing home resident was sent to the hospital for evaluation of a malfunctioning JT. JT was placed earlier in the year for prolonged feeding after patient sustained a traumatic brain injury. Patient was non-verbal at baseline after his injury. His vital signs at the time of admission were normal. Abdominal exam was soft, non tender and JT flushed appropriately; however, some tension was noted when the tubing was withdrawn into the attachment device. Labs on admission revealed amylase 1519, lipase 971, AST 184, ALT 442, alkaline phosphatase 749, total bilirubin 1.0, and direct bilirubin 0.4. A CT scan without contrast was performed which revealed intrahepatic ductal dilatation, Common Bile Duct diameter (CBD) of 10 mm, and mild fat-stranding surrounding the pancreas. Gallbladder was normal without cholelithiasis. Endoscopic Retrograde Cholangiopancreatography was performed and the JT was found compressed across the ampulla with associated ulceration. An attempt to cannulate the CBD was unsuccessful. The JT was removed after balloon deflation. An endoscopic sphincterotomy was then performed and occlusion cholangiogram did not reveal any filling defects. Patient’s liver function test abnormalities gradually improved over the next few days and he was discharged back nursing home (Figure 1,2 and 3).
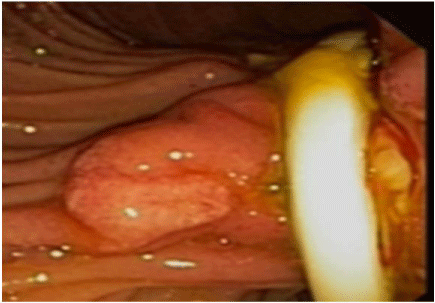
Figure 1: EGD showing ampullary region before the removal of Jejunostomy
Tube.
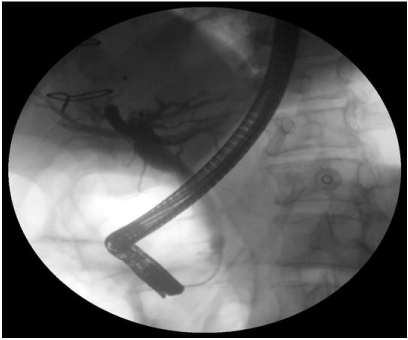
Figure 2: Cholangiogram revealing no filling defects.
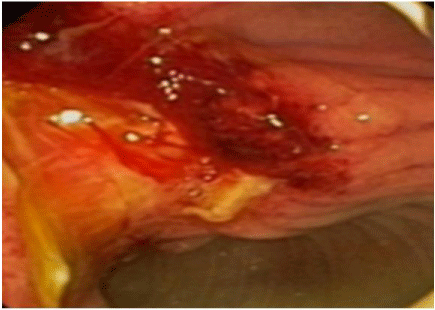
Figure 3: EGD showing ampullary region after removal of Jejunostomy tube.
Discussion
Enteral feeding is the preferred method of nutrition for patients who cannot maintain adequate nutrition orally and provides additional benefits such as gastrointestinal mucosal integrity and immuno-secretory function. Minimum Data Set (MDS) data from 2006 showed that only in New York State 8.1% of all nursing home residents were receiving enteral feedings. This data varies widely state-to-state [2]. There are different types of enteral feedings. Jejunostomy is a procedure by which a tube is situated in the lumen of the proximal jejunum [3]. It can be placed surgically or endoscopically. It is one of the common methods of enteral feeding. It is considered in patients after laparotomy, in which a complicated post-operative recovery is expected, those with a prolonged fasting period, those in a hypercatabolic state, or those who will subsequently need chemotherapy or radiotherapy.
J tube has been associated with complications, which can be broadly divided in to three categories: mechanical, gastrointestinal and metabolic. Some of the common complications include tube dislocation, obstruction or migration of the tube, cutaneous or intraabdominal abscesses, enterocutaneous fistulas, pneumatosis, occlusion, and intestinal ischemia. Other includes abdominal distension. Colic, constipation, nausea and vomiting [3,4]. In our review we were able to establish G-tubes as a recognized cause of AOP due to trauma to the sphincter of Oddi from wandering gastrostomy balloon. One study speculated the underlying mechanism for G-tube migration to be intestinal peristalsis, which carries the tube through the duodenum once it crosses the pyloric sphincter. The risk for migration is further increased if the tube is pushed too far upon its initial placement or if the external bumper securing the tube becomes loose, as this may cause the tube to be gradually pushed further into the abdominal cavity [5].
A review of the literature showed two cases where JT migrated in to the small intestine and subsequently came out of rectum 18 and 20 days later [6,7]. However no documented association between JT and acute pancreatitis was seen. Based on this patient’s endoscopic findings and resolution of pancreatic enzymes and liver function abnormalities after removal of JT, it is deduced that extrinsic compression of the biliary tract and inflammation of the sphincter of Oddi with subsequent obstruction of bile outflow caused pancreatitis directly due to the presence of a tightly wedged JT.
Conclusion
In the end we emphasize clinicians to be vigilant of this rare complication and have a strong index of suspicion of AOP secondary to JT when a patient with a JT presents with symptoms of acute pancreatitis.
References
- Brauner E, Kluger Y. Gastrostomy tube dislodgment acute pancreatitis. World J Emerg Surg. 2014; 9: 23.
- Gavi S, Hensley J, Cervo F, Nicastri C, Fields S. Management of feeding tube complications in the long-term care resident. Annals of Long-Term Care. 2008; 16: 28-32.
- Tapia J, Murguia R, Garcia G, de los Monteros PE, Oñate E. Jejunostomy: techniques, indications, and complications. World J Surg. 1999; 23: 596-602.
- Hoepffner N, Schröder O, Stein J. Enteral nutrition by endoscopic means; II. Complications and management. Z Gastroenterol. 2004; 42: 1393-1398.
- Bhargava A, Andrews C, Belforti R. Acute pancreatitis from gastrostomy tube migration in a nursing home resident. Annals of Long-Term Care: Clinical Care and Aging. 2011; 19: 25-27.
- Ozben V, Karatas A, Atasoy D, Simsek A, Sarigül R, Tortum OB. A rare complication of jejunostomy tube: Enteral migration. Turk J Gastroenterol. 2011; 22: 83-85.
- Bose AC, Shankar RR, Kate V, Ananthakrishnan N. Spontaneous antegrade enteral migration of feeding jejunostomy tube. Indian J Gastroenterol. 2005; 24: 74.