
Case Report
Austin J Clin Case Rep. 2017; 4(3): 1122.
Myocardial Infarction in the Setting of Unsuspected Thrombocytopenia
Ziffra J*, Samaddar S, Murray A and Tran P
Department of Cardiology, Mercy Medical Center – North Iowa, USA
*Corresponding author: Jeffrey Ziffra, Department of Cardiology, Mercy Medical Center – North Iowa, 1000 4th St. SW, Mason City, IA 50401, USA
Received: April 09, 2017; Accepted: July 20, 2017; Published: July 24, 2017
Abstract
Immune Thrombocytopenic Purpura is a rare disorder characterized by autoimmune destruction of platelets. Thrombus formation in coronary arteries with underlying atherosclerosis is at the hallmark of acute coronary syndrome. Immune Thrombocytopenic Purpura has rarely been implicated in cases of acute coronary syndrome which presents a treatment challenge laden with increased risks of both bleeding and thrombosis. We describe a case of a 42-year-old female with chronic Immune Thrombocytopenic Purpura who presented with a ST-Elevation myocardial infarction. After review of the literature, dual antiplatelet therapy has been implemented successfully with preferential angiogram by radial artery access and use of a bare-metal stent.
Keywords: Myocardial infarction; Immune thrombocytopenic purpura; Acute coronary syndrome
Introduction
Formation of an unstable thrombus in conjunction with atherosclerosis often precipitates acute coronary syndrome. Disorders including autoimmune thrombocytopenia are rare but have been reported to be associated with acute coronary syndrome. Given the need for antiplatelet therapy, this becomes a challenging medical conundrum. We describe a case of a 42-year-old female with a history of Immune ThrombocyticPurpura (ITP) who presents with an Inferior wall ST-Elevation Myocardial Infarction (STEMI). It is important for clinicians to recognize this challenging scenario to treat.
Case Presentation
We present the case of a 42-year-old female with a history of ITP status post splenectomy, history of preeclampsia with concern for HELLP syndrome, who presented to our facility with STEMI. The patient was transferred from an outside facility with STelevations in the inferior leads, minor ST-Elevations in the anterior leads on EKG (Figure 1). She was emergently taken to the cardiac catheterization lab with a very limited history and no laboratory data. In the cardiac catheterization lab she was found to have a 70% distal left anterior descending (LAD) artery stenosis and a right focal coronary artery (RCA) spasm (Figure 2,3). She received a successful percutaneous coronary intervention (PCI) of her LAD lesion with a 2.5 x 18 mm Bare Metal Stent. She also received intracoronary nitroglycerin, which resolved her focal RCA spasm. During the intervention, her labs returned for which she was found to be anemic and severely thrombocytopenic which was new compared to our last complete blood count. She was also found to have elevated lactate dehydrogenase and ferritin levels. A peripheral blood smear was performed which revealed spherocytes, shistocytes, polychromasia, basophilic stippling, Howell-jolly bodies, pappenheimer bodies and dimorphic population. After angiogram, she was transferred to a higher-level care facility for management of suspected Thrombotic ThrombocyticPurpura (TTP). Hematology was consulted for her thrombocytopenia and to rule out Disseminated Intravascular Coagulopathy, TTP, Hemolytic anemia or ITP.

Figure 1: EKG revealing minimal ST-Elevation in leads III and AVF
concerning for inferior wall infarction.
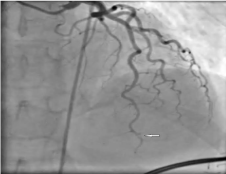
Figure 2: Distal 70% Left Anterior Descending Artery stenosis on angiogram.
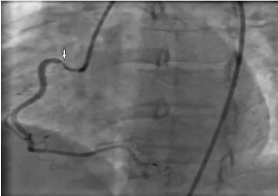
Figure 3: Right Coronary Artery Spasm which resolved on nitroglycerin.
The patient historically had a history of preeclampsia and HELLP syndrome. She was found to have ITP for which she was treated with steroids initially but ultimately a splenectomy was performed 12 years prior to admission. After splenectomy, she has complications with multiple infections. She had been on and off steroids for treatment of her chronic ITP. Upon presentation she was found to be methamphetamine positive in her urine. Further hematologic diagnosis revealed a mixed picture with signs of thrombotic microangiopathy and negative tests for Direct Antiglobulin Test (DAT) and ADAMTS13 mutations. After treatment with a steroid taper, she ultimately presented again to our facility from an outside emergency room for symptoms consistent with viral gastroenteritis where she was found to have thrombocytopenia with platelets were found at 28. She was not having any cardiac symptoms at that time but did stop taking her steroids. At this admission an echocardiogram was performed which displayed apical wall akinesis. Upon admission, she was hemodynamically stable. She was treated supportively with IV fluids, and her antiplatelet therapy and steroids were resumed.
Discussion
ITP is a rare autoimmune platelet disorder characterized by thrombocytopenia and mucocutanous bleeding. ITP is often a diagnosis of exclusion as there is a wide spectrum of disorders causing thrombocytopenia [1]. Acute coronary syndrome (ACS) is often precipitated by a platelet plug which forms, meets a cholesterol plaque and impedes blood flow to myocardium. Thrombocytopenia in ITP often has a paradoxical hypercoagulable state and the treatment often induces endothelial dysfunction and vasospasm as well. Few case reports have described STEMI in the setting of thrombocytopenia.
In treating for ACS, the treatment regimen consists of dual antiplatelet therapy (DAPT) that increases risks for bleeding. In patients with underlying thrombocytopenia, the risk for bleeding is multiplied. Access using the radial artery has been proposed to achieve easier hemostasis or the use of vascular closure devices. Bare metal stents are also preferred due to decreased duration of antiplatelet therapy [2,3]. Despite adequate medical therapy with appropriate duration of DAPT, these patients are still at high risk. Patients with ITP have been reported to have a higher risk of in stent thrombosis requiring repeat cardiac catheterization. Several cases have been reported with early in-stent restenosis in a short period of time requiring a repeat angiogram [4-7]. Generally GPiiB/iiiA inhibitors are avoided due to increased risk of bleeding however it has been reported to have successful uses in some case reports [8,9]. The first cases of ITP and ST-Elevation myocardial infarctions were reported to receive CABG however PCI has now proven to be a safe opportunity as well [2,10].
There have been no guidelines or recommendations on how to treat patients with this unique clinical presentation. Several case reports have suggested increasing platelet counts so as to reduce the risk of excess bleeding while giving antiplatelets [1]. Standard ACS medications including dual antiplatelet therapy and anticoagulant therapy is contraindicated when platelet counts drop below 30,000 [3]. Often in treatment of ITP, patients will often receive steroids, IVIg and if refractory, splenectomy [2]. IVIg has been proposed to increase risk of cardiac events however as it causes an increase in blood viscosity. This mechanism has been reported in 4 case studies while other literature supports its use successfully [11].
Although ITP quantitatively has a decreased amount of platelets, shorter bleeding times than would be expected have been reported. These new platelets are younger, larger and more active which may explain the presence of coexisting acute coronary syndromes in the settings of thrombocytopenia. ITP is an immune phenomenon in which autoantibodies attack platelets. It is proposed that these autoantibodies may attack the endothelium as well increasing the probability of thromboembolism [3]. Other medications to treat thrombocytopenia including Romiplostim also have been reported to increase thromboembolic risk [4].
Without any specific guidelines, we can look to previously reported cases and proposed theoretical mechanisms to help assist us in management. Shah A, et al. reports a case of a 42 year-old female with ITP who presented with ACS, received a bare metal stent and DAPT successfully but then returned the same day of discharge with in-stent restenosis and thrombus formation. At that time, the patient’s platelets were only slightly decreased. The patient presented again with a non-ST elevation myocardial infarction where the stent was found to be patent on angiogram. The patient continued on DAPT for 1 year’s duration and romiplostim. Li-Sha, et al. describe a case of a 75 year-old male with chronic ITP, and previous STEMI with stent placement who presented 5 years later with non ST-elevation myocardial infarction. The patient was found to have in-stent restenosis which was amenable to a cutting balloon. The patient was thrombocytopenic on presentation requiring platelet transfusion. 4 months later, the patient presented again with unstable angina and was found again to have a 99% restenosis in the same drug-eluting stent. These patients, despite adequate DAPT are at high risk for instent restenosis as well [5,7].
There are several invalidated proposed mechanisms described in the literature. As we know, thrombocytopenia is more often associated with bleeding rather than thrombosis however several case reports report an association with myocardial infarction, cerebrovascular event and venous thromboembolism. These complications are often found when the platelet counts begin to rise upon receiving treatment however. Shen, et al. proposes several theories such as the antibody reaction that attacks platelets may release small platelet particles than can precipitate thrombosis. As stated earlier, new platelets are larger and more active making them more likely to cause thrombosis. Autoantibodies targeting platelets may also nonselectively target coronary artery endothelium as well. Splenectomy, a treatment often reserved for refractory ITP can predispose to venous thromboembolism. Other treatments including steroids, danazol and IVIg treatments have been reported to increase blood viscosity platelet activation and/or vasospasm as well as cause arterial thrombosis [8]. Although splenectomy has been reported to be associated with thrombosis, there are no recommendations to perform this prophylactically. In general, the treatment of thrombocytopenia has to be done carefully due to a paradoxical increase in risk of thromboembolism.
We report the case of a 42-year-old female with chronic ITP status post splenectomy who had been on suppressive steroids in the past who presented with Inferior wall STEMI and found to have an LAD lesion with thrombus and a RCA spasm. The patient was found to be profoundly thrombocytopenic at time of her angiogram. A PCI was performed to her LAD and DAPT was maintained with further treatment of her thrombocytopenia. She presented again to us with a viral syndrome where DAPT was continued and steroids were given for thrombocytopenia. The patient continued to do well with these therapies. In reviewing the literature, the patient is at high risk for in-stent restenosis and treating her thrombocytopenia may worsen thrombosis. Treatment needs to be individualized and more research is needed in this subject to make guidelines to therapy.
References
- Neskovic AN, Stankovic I, Milicevic P, Aleksic A, Vlahovic-Stipac A, Calija B, et al. Primary PCI for acute myocardial infarction in a patient with idiopathic thrombocytopenic purpura. Herz. 2010; 35: 43-49.
- kDhillon S, Lee E, Fox J, Rachko M. Acute ST elevation myocardial infarction in patients with immune thrombocytopenia purpura: a case report. Cardiol Res. 2011; 2: 42-45.
- Zaid G, Dawod S, Rosenschein U. Immune thrombocytopenic purpura and myocardial infarction: a dilemma of management. Isr Med Assoc J. 2013; 15: 775.
- Rayoo R, Sharma N, van Gaal WJ. A Case of Acute Stent Thrombosis during Treatment with the Thrombopoietin Receptor Agonist Peptide-Romiplostim. Heart Lung and Circulation. 2012; 21: 182-184.
- Shah AH, Anderson RA, Khan AR, Kinnaird TD. Management of immune thrombocytic purpura and acute coronary syndrome: A double-edged sword! Hellenic Journal of Cardiology. 2016; 57: 273-276.
- Cines DB, Blanchette VS. Immune thrombocytopenic purpura. N Engl J Med. 2002; 346: 995-1008.
- Li-Sha G, Peng C, Yue-Chun L. Recurrent acute coronary syndrome and restenosis after percutaneous coronary intervention in a patient with idiopathic thrombocytopenic purpura: a case report and literature review. BMC Cardiovasc Disord. 2015; 15: 101.
- Campo G, Marchesini J, Fileti L, Tebaldi M, Ferrari R. Medical and interventional management of patients with severe thrombocytopenia undergoing percutaneous coronary intervention. Journal of Thrombosis and Haemostasis. 2012; 10: 153-156.
- Stouffer G A, Hirmerova J, Moll S, Rubery B, Napoli M, Ohman EM et al. Percutaneous coronary intervention in a patient with immune thrombocytopenia purpura. Catheterization and cardiovascular interventions. 2004; 61: 364-367.
- Russo A, Cannizzo M, Ghetti G, Barbaresi E, Filippini E, Specchia S, et al. Idiopathic thrombocytopenic purpura and coronary artery disease: comparison between coronary artery bypass grafting and percutaneous coronary intervention. Interact Cardiovasc Thorac Surg. 2011; 13: 153-157.
- Elkayam O, Paran D, Milo R, Davidovitz Y, Almoznino-Sarafian D, Zeltser D, et al. Acute myocardial infarction associated with high dose intravenous immunoglobulin infusion for autoimmune disorders. A study of four cases. Ann Rheum Dis 2000; 59: 77-77.