
Case Report
Austin J Clin Case Rep. 2019; 6(1): 1138.
Xanthogranulomatous Pyelonephritis the Great Imitator: A Case Report with Literature Review
Iloughmane Z¹*, Echchachoui H¹, Bennani Smires F¹, E¹ Ghazi M¹, Zerrik M¹, Ait Oufkir M², Tbouda M³, Toufga Z4, Oukabli M³ and Chemsi M¹
¹Aeromedical Expertise Center, Military Hospital Mohammed v Rabat, Morocco
²National Center of Reproductive Health, Hospital Ibn Sina, Rabat, Morocco
³Department of Pathology, Military Hospital Mohammed v Rabat, Morocco
4Department of Radiology, Military Hospital Mohammed v Rabat, Morocco
*Corresponding author: Iloughmane Zakaria, Aeromedical Expertise Center, Military Hospital Mohammed v Rabat, Morocco
Received: January 02, 2019; Accepted: January 30, 2019; Published: February 06, 2019
Abstract
Xanthogranulomatous pyelonephritis is a rare form of chronic pyelonephritis, which frequently has a pseudotumoral appearance, we report the case of a 50-year-old postmenopausal woman with a history of recurrent urinary tract infections, admitted for asthenia, prolonged fever (39°C) and importat weight loss, the medical imagerie revealed a mass of the right kidney. The radiological aspect of the mass led us to a pseudotumoral pyelonephritis which motivated a percutaneous scanner-guided biopsy which showed an inflammatory infiltrate composed of a variable number of xanthomatous histiocytes with neutrophils, lymphocytes, plasma cells, and multinucleated giant cells, confirming the diagnonis of Xanthogranulomatous pyelonephritis, the treatment was a nephrectomy.
Xanthogranulomatous pyelonephritis affects females more often than males, the most common symptoms are flank or abdominal pain, lower urinary tract symptoms, fever, palpable mass, and weight loss. Biological results showed leukocytosis and anemia. Urine cultures most often reveal Escherichia coli and Proteus mirabilis. Radiological criteria can direct the diagnosis specially for the focal form, but only the histological findings confirms the diagnosis, showing a granulomatous inflammatory infiltrate composed of xanthomatous histiocytes, and multinucleated giant cells. Both antibiotics and surgery can be treatment options depending on the patient’s disease status.
Keywords: Kidney; Xanthogranulomatous pyelonephritis; Chronic pyelonephritis
Abbreviations
XGPN: Xanthogranulomatous Pyelonephritis
Introduction
Xanthogranulomatous pyelonephritis (XGPN) is an uncommon chronic destructive granulomatous process of renal parenchyma, called the “great imitator” because of its clinical and radiological findings miming other neoplastic and inflammatory renal diseases, There are two anatomic forms of XGPN: the diffuse form, which is the most frequent, and the pseudo-tumoural form (or focal form), By this case we remind the rarity of the Xanthogranulomatous pyelonephritis and the difficulty of establishing the diagnosis and choosing the ideal treatment between conservative and radical surgery [1,2].
Case Presentation
A 50-year-old postmenopausal woman with a history of recurrent urinary tract infections, admitted for asthenia, prolonged fever (39°C) and importat weight loss, the physical examination found a right lumbar contact. The hematologic evaluation showed the presence of leukocytosis at 18,000cells/mm3, 64% of which was neutrophilic, an increased C-reactive protein at 313mg/dl, ferritinemia at 8590ng/ml, and fibrinogen increased at 8.37g/l. Renal function was maintained with uremia at 0.13g/l and serum creatinemia at 5mg/l, Urinalysis revealed a multi-sensitive Escherichia coli.
Renal ultrasound revealed a right hypoechoic renal mass without pyelocalicar dilatation or clearly visible obstacle image, Computed tomography showed a right renal lesion of irregular contours hypo dense enhanced heterogeneously, measuring 34x30 mm (Figure 1).
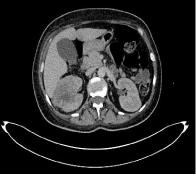
Figure 1: Axial section of an abdominal CT with contrast injection showing a
right renal lesion of irregular contours hypo dense enhanced heterogeneously
measuring 34x30 mm.
Magnetic resonance imaging performed in the context of a renal tumor objectified a T1 hyposignal lesion with a small heterogeneously enhanced fatty area (Figure 2). The radiological aspect of the mass led us to a pseudotumoral pelimiyelonephritis which motivated a percutaneous scanner-guided biopsy, which showed a granulomatous inflammatory infiltrate composed of neutrophils, lymphocytes, plasma cells, xanthomatous histiocytes compatible with a xanthogranulomatous pyelonephritis (Figure 3).
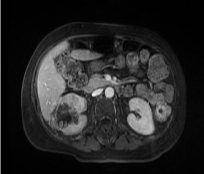
Figure 2: Axial section of T1-weighted abdominal MRI with fat saturation and
contrast injection showing a T1 hyposignal lesion with a small heterogeneously
enhanced fatty area.
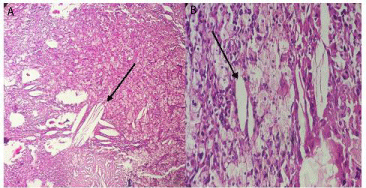
Figure 3: Histological section of the biopsy with high magnification x200
(A) and x400 (B), showing numerous foamy histiocytes surrounding lipids
crystals (black arrow).
The patient has been proposed for surgeons for a possible nephrectomy, the postoperative follow-ups were simple with a good clinical evolution.
Discussion
XGPN is a chronic granulomatous inflammation of renal parenchyma, described for the first time by Schlagenhaufen in 1916 and classified In 1978 by Elder and Malek, There are two anatomic forms of XGPN: the diffuse form, which is the most frequent, and the pseudo-tumoural form (or focal form) [1].
XGPN occurs specialy in middle-aged women, with male to female ratio ranging up to 1/6 in some series [3,4].
The most common symptoms revealing the XGPN are flank or abdominal pain, lower urinary tract symptoms, hematuria, fever, palpable mass and weight loss.
The laboratory findings showed stigmas of infection including predominantly neutrophilic leukocytosis, elevation of the C-reactive protein, sedimentation rate and fibrinogen. The urinary culture is sterile in 54% of cases, in case of urinary infection, Escherichia coli and Proteus mirabilis are the most frequently found germs [5,6].
The diagnosis of xanthogranulomatous pyelonephritis is mainly histopathological, but some radiological criteria can direct it specially for the focal form and which generally poses a problem of diagnosis with renal tumors, the Computed tomography findings of diffuse XGPN include hydronephrosis (90.9%), renal calculus (72.7%), pyonephrosis (45.5%), intraparenchymatous collection (45.5%), cortical renal atrophy (45.5%), nonfunctioning kidney (36.4%), abscess (36.4%) and perinephric fat accumulation (18.2%) [7].
Renal ultrasound can visualize nonspecific abnormalities: enlarged and heterogeneous kidneys. The appearance of “hydropyonéphrose” is sometimes evocative, with multiple hypoechoic or anechoic formations within the renal parenchyma [7,8].
Intravenous urography found non-specific abnormalities: lithiasis (38%), hydronephrosis, syndrome mass (62%), decrease renal excretion, or even mute kidney in diffuse forms essentially (27%), associated tract anomaly excretory [5,7,9].
The magnetic resonance imaging often indicated in the context of the assessment of a renal tumor, makes it possible to objectify a hypersignal in T1- and T2-weighted sequences comparable to that of the subcutaneous tissues, and this thanks to the lipidic richness of macrophage cells contained in xanthomatous granulomas [7,10].
The final diagnosis should be determined by the histopathological examination findings, showing an inflammatory infiltrate composed of a variable number of xanthomatous histiocytes with foamy cytoplasm, neutrophils, lymphocytes, plasma cells, and multinucleated giant cells, In addition, a variable degree of renal tubular atrophy can be observed. It is thought that XGPN is a morphologic variant of chronic pyelonephritis, but differs from it with the abundant infiltrate of foam cells, which are macrophages containing lipids [9,11].
The immunohistochemistry study can play an essential role in the differential diagnosis, lipid-laden xanthomatous cells may mimic the clear cells of Renal Cell Carcinoma, Xanthogranulomatous pyelonephritis is diffusely positive for CD68. Renal cell carcinoma is usually positive for CD10 and epithelial membrane antigen. Vimentin can stain positive for both [11].
The management differs for diffuse and focal forms. Total nephrectomy is the standard of treatment in diffuse forms, but both radical and partial nephrectomies are technically difficult because of inflammation of tissues around kidney, Focal XGPN or bilateral XGPN can also be treated with antibiotics if the diagnosis is established with histologic features of biopsy or combined clinical and cytologic features, Medical treatment avoids a decaying surgery and offers nephron-sparing, the main problem is to confirm this diagnosis and exclude renal cancer. Preoperative and postoperative broad-spectrum antibiotics and symptomatic management are also key factors for successful management. The prognosis is considered to be good after treatment [12,13].
Conclusion
Xanthogranulomatous pyelonephritis is a rare form of chronic pyelonephritis in which the impact of obstructive lithiasis and of urinary infections is proven. Its symptomatology mimics other chronic renal diseases. The diagnosis is difficult, evoked by the tomodensitometry, the intravenous urography and ultrasound, confirmed by magnetic resonance imaging and especially by histopathological examination of nephrectomy.
References
- Li L, Parwani AV. Xanthogranulomatous pyelonephritis. Arch Pathol Lab Med. 2011; 135: 671–674.
- Chlif M, Chakroun M, Ben Rhouma S, Ben Chehid MA, Sellami A, Gargouri M, et al. Xanthogranulomatous pyelonephritis presenting as a pseudotumour. N Can Urol Assoc J. 2016; 10: E36–E40.
- Kim SW, Yoon BI, Ha US, et al. Xanthogranulomatous pyelonephritis: Clinical experience with 21 cases. J Infect Chemother. 2013; 19: 1221–1224.
- Korkes F, Favoretto L, Bróglio M, Silva CA, Castro MG, Perez DC. Xanthogranulomatous Pyelonephritis: Clinical Experience with 41 Cases. Urology. 2008; 71: 178–180.
- Malek RS, Elder JC. Xanthogranulomatous pyelonephritis: a critical analysis of 26 cases and of the literature. J Urol. 1978; 119: 589-593.
- Huisman TK, Sands JP. Focal xanthogranulomatous pyelonephritis associated with renal cell carcinoma. Urology. 1992; 39: 281-284.
- Loffroy R, Varbédian O, Guiu B, Delgal A, Michel F, Cercueil JP, et al. La pyélonéphrite xanthogranulomateuse: principaux aspects en imagerie. Progrès En Urologie. 2008; 18: 266–274.
- Tiu CM, Chou YH, Chiou HJ, Lo CB, Yang JY, Chen KK, et al. Sonographic features of xanthogranulomatous pyelonephritis. J Clin Ultrasound. 2001; 29: 279-285.
- Mohanty A, Kim O. Nonfunctional right kidney in a 50-year-old woman: Xanthogranulomatous pyelonephritis. Arch Pathol Lab Med. 2005; 129: e209–e211.
- Verswijvel G, Oyen R, Van Poppel H, Roskams T. Xanthogranulomatous pyelonephritis: MRI findings in the diffuse and the focal type. Eur Radiol. 2000; 10: 586-589.
- Reul O, Waltregny D, Boverie J, de Leval J, Andrianne R. Pseudotumoral xanthogranulomatous pyelonephritis: diagnosis with percutaneous biopsy and success of conservative treatment. Prog Urol. 2001; 11: 1274-1276.
- Bingöl-Kologlu M, Ciftçi AO, Senocak ME. Xanthogranulomatous pyelonephritis in children: Diagnostic and therapeutic aspects. Eur J Pediatr Surg. 2002; 12: 42–48.
- Tsai KH, Lai MY, Shen SH, Yang AH, Su NW, Ng YY. Bilateral xanthogranulomatous pyelonephritis. J Chin Med Assoc. 2008; 71: 310–314.