
Case Report
Austin J Clin Case Rep. 2019; 6(5): 1158.
An Extended Lithium Saga: Case Report
Matchett C* and Laura Maursetter DO
Division of Nephrology, Department of Medicine, University of Wisconsin School of Medicine and Public Health, Madison, WI, USA
*Corresponding author: Caroline Matchett, Division of Nephrology, Department of Medicine, University of Wisconsin School of Medicine and Public Health, 1685 Highland Avenue Madison, Madison, WI, 53792, USA
Received: November 25, 2019; Accepted: December 26, 2019; Published: December 31, 2019
Abstract
Lithium remains a drug of choice in the treatment of bipolar disorder, despite its extremely narrow therapeutic window. The toxic effects of lithium are well described, as is the use of intermittent hemodialysis (IHD) to remove lithium in patients with established toxicity. What remains elusive is the duration of therapy required to reduce lithium levels to therapeutic range (‹1.0mEq/L) following intoxication, especially when sustained-release preparations are ingested. We describe a case of acute on chronic lithium toxicity with an extended-release preparation that necessitated a total of 45 hours of IHD to normalize serum lithium levels (‹1mEq/L).
Keywords: Lithium; Toxicity; Extended-Release; Hemodialysis
Introduction
Lithium continues to be a preferred treatment for bipolar affective disorder [1]. Unfortunately, the therapeutic level of lithium (0.6–1.2 mEq/L) is extremely close to the toxic range. Lithium toxicity (levels ›1.5mEq/L) may manifest as gastrointestinal disturbances, cardiac arrhythmias, altered mentation, seizures or death [2,3].
Lithium is highly dialyzable due to its low molecular weight (6.94Da), negligible protein binding, and small volume of distribution (0.8-1.2 L/kg) [4]. The rapid reduction in serum lithium by intermittent hemodialysis (IHD) places it as the treatment of choice for cases of severe intoxication [4,5]. However, the appropriate duration of IHD for the treatment of lithium poisoning remains controversial. The literature is especially scarce in describing the time course of treatment when extended-release preparations are ingested. We report a case of acute on chronic intoxication with extendedrelease lithium that required prolonged IHD to achieve safe serum lithium levels.
Case Presentation
A 29-year old man with bipolar disorder who was chronically taking extended-release lithium carbonate presented to the emergency department 5 hours after an intentional overdose of 141g. On arrival, his temperature was 36.1°C, heart rate 115bpm, and blood pressure 170/94mmHg. Physical examination was limited due to significantly altered mentation, agitation, and emesis. Toxicology screening was negative for alcohol and illicit drugs. Initial laboratory values showed: sodium 146mmol/L, potassium 4mmol/L, BUN 13mg/dL, creatinine 0.87mg/dL, glucose 127mmol/L, white cell count 9.9×103/uL, hemoglobin 13.7g/dL platelets 338×103/uL and normal liver enzymes. Serum lithium level was 3.32mEq/L (therapeutic range 0.6–1.2 mEq/L). EKG demonstrated sinus tachycardia. Patient was intubated for airway protection and central venous access was obtained. An orogastric tube was placed and whole bowel irrigation with 3L polyethylene glycol was performed in an attempt to decrease gastrointestinal lithium absorption. The patient received a 2L normal saline bolus and then continued on 150mL/h with adequate urine output throughout. Nephrology consultation was obtained. Given that a repeat lithium level had decreased to 2.72mEq/L (8 hours after ingestion), the decision was made to hold the initiation of dialysis and continue to trend lithium levels. Hemodialysis was subsequently started (14 hours after ingestion) when serum lithium increased to 4.12mEq/L and repeat EKG revealed QTc prolongation.
The hemodialysis prescription included a high flux dialyzer with blood flows of 400mL/min and dialysate flows of 800mL/min through a 16 French right internal jugular catheter. There were no episodes of clotting reported and lithium levels were periodically checked (Figure 1). Plans were made to continue hemodialysis until a goal lithium of ‹1mEq/L was achieved.
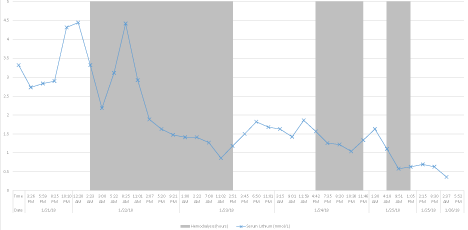
Figure 1: Effect of intermittent hemodialysis on lithium levels. Shaded are as represent hemodialysis sessions.
The patient’s serum lithium peaked at 4.44mEq/L (15 hours after ingestion). Thirty-six hours of continuous high-flux hemodialysis were required to normalize the patient’s lithium level (0.85mEq/L). Due to rebound lithium levels, two subsequent 4.5 hour hemodialysis sessions at 81 and 96 hours after ingestion were required to maintain a serum lithium concentration ‹1mEq/L. One hundred hours after the initial consumption, after whole bowel irrigation and 45 hours of hemodialysis, serum lithium levels were maintained ‹1mEq/L without further need for intervention.
Discussion
The use of IHD in the management of lithium overdose is well described; however, controversy over the duration of IHD required to reduce the plasma concentration to a safe level remains. Some authors report adequate clearance of lithium following one or two HD sessions [5]. More recently, experts advocate for extended hemodialysis until the lithium concentration remains below 1mEq/L for 6 to 8 hours [2,6]. Our patient required a total of 45 hours to normalize lithium levels (‹1mmol/L), lending support for the latter.
A range of factors requires consideration when deciding how to best manage lithium toxicity. Lithium’s oral bioavailability is ~80- 100% [7]. Immediate-release formulations are rapidly absorbed in the upper gastrointestinal tract with peak blood levels achieved within 1 to 2 hours. In contrast, extended-release (ER) formulations reach peak levels within 4 to 6 hours [2,5]. For both IR and ER formulations of lithium the elimination half-life is ~12-27 h; this may increase to upwards of 58h in chronic use due to the intracellular accumulation of the drug over time [2]. Relative to the rate at which it is eliminated from the body, lithium equilibrates between intracellular and extracellular compartments slowly [4]. This may result in multiple delayed peak concentrations following intoxication, which is likely what happened in our patient. It would be expected to have rebound of lithium levels after IHD but usually to a max of 50% of the predialysis level [8]. Our patient had significantly higher levels raising suspicion of alternative pharmacokinetics. ER preparations have the potential to form pharmacobezoars (mass of aggregated tablets in the GI tract) that can lead to prolonged and erratic drug absorption [4,9]. Although no investigation was done to assess for a bezoar in this patient, review raises suspicion that this was the source of continued lithium absorption, which required 45 hours of IHD to achieve control.
It imperative for practitioners to understand the pharmacokinetics of lithium and interpret lithium levels relative to both the time from ingestion and the formulation ingested. It is important to understand how ER formulations might alter predictions for duration of IHD therapy. Acute on chronic intoxications with ER formulations should be managed with caution; continuous drug monitoring and prolonged IHD sessions may be necessary to adequately remove the drug. In addition, the formation of medication bezoars is rare but can pose additional challenges in management. In this case, if the team would have stopped tracking lithium levels after the first decrease was noted, the outcome for this patient might have been different; instead, he was discharged without subsequent consequences.
References
- Lenox RH, et al. Neurobiology of lithium: an update. The Journal of clinical psychiatry. 1998; 59: 37-47.
- Okusa MD and LJ Crystal. Clinical manifestations and management of acute lithium intoxication. Am J Med. 1994; 97: 383-389.
- Ellenhorn MJ. Diagnosis and Treatment of Human Poisoning. Ellenhorn’s Medical Toxicology. 1997: 1880-1896.
- Baird-Gunning J, et al. Lithium Poisoning. J Intensive Care Med. 2017; 32: 249-263.
- Timmer RT and JM Sands. Lithium Intoxication. Journal of the American Society of Nephrology. 1999; 10: 666-674.
- Hansen HE and A Amdisen. Lithium intoxication. (Report of 23 cases and review of 100 cases from the literature). Q J Med. 1978; 47: 123-144.
- Girardi P, et al. Lithium in Bipolar Disorder: Optimizing Therapy Using Prolonged-Release Formulations. Drugs R D. 2016; 16: 293-302.
- Jacobsen D, et al. Lithium intoxication: pharmacokinetics during and after terminated hemodialysis in acute intoxications. J Toxicol Clin Toxicol. 1987; 25: 81-94.
- Thornley-Brown D, et al. Lithium Toxicity Associated with a Trichobezoar. Annals of Internal Medicine. 1992; 116: 739-740.