
Case Report
Austin J Clin Case Rep. 2020; 7(3): 1174.
Rare, Life Threatening, Treatment Dilemma: A Case Report of Hughes Stovin Syndrome
Assoufi N*, Maaroufi A, Elomri N, Smaali J, Charef A, Mekouar F, Jira M and Fatihi TJ
Department of Internal Medicine, Mohamed V Military Hospital, Faculty of Medical Sciences, University Mohammed V Rabat, Morocco
*Corresponding author: Naoufal Assoufi, Department of Internal Medicine, Mohamed V Military Hospital, Faculty of Medical Sciences, University Mohammed V Rabat, Morocco
Received: June 09, 2020; Accepted: October 09, 2020; Published: October 16, 2020
Abstract
Introduction: Hughes–Stovin Syndrome (HSS) is a rare clinical entity, which is characterized by peripheral venous thrombosis and multiple pulmonary artery aneurysms with potentially life-threatening complications.
Materials and Methods: We report a case of a 35 years old Moroccan military male with history of pulmonary tuberculosis treated 02 years ago and bipolar ulcer in his oral cavity and genital region who was presented to our service for mild abundance hemoptysis. Chest X ray showed opacity in the right lung field. Computed Tomography (CT) scan revealed bilateral multiple pulmonary artery aneurysms. Cardiac MRI was performed and showed the presence of a thrombosis of the right ventricle.
Hughes-Stovin syndrome was diagnosed, and high-dose of steroids (methylprednisolone) and immunosuppressant (cyclophosphamide) were administered. The hemoptysis was controlled with stabilization of the pulmonary aneurysms.
Conclusion: Our case shows a particular localization of thrombosis and the problem of treatment which keep to be a very difficult and hard decision especially when there is both a specific deep thrombosis and high risk pulmonary aneurysm.
Abbreviations
HSS: Hughes Stovin Syndrome; CT: Computed Tomography; MRI: Magnetic Resonance Imaging
Background
Hughes and Stovin had reported in 1959 four cases of deep vein thrombosis and multiple pulmonary artery aneurysms [1]. Since then this association caries the name of HSS (Hughes Stovin syndrome). It is a rare and life threatening clinical situation which affects almost men with only two women described in the literature [2].
The main cause of mortality in HSS is related the rupture of the pulmonary artery aneurysm which leads to a fatal hemoptysis [3-5]. This unpleasing and complicated situation for the patricians make the use of anticoagulant a very hard decision [1,6].
Case Report
A young morrocan military male of 35 years old with medical history of pulmonary tuberculosis treated 03 years ago has been admitted to our department for an isolated mild hemoptysis. He had a one year history of recurrent oral and genital ulceration. His physical examination was within normal limits). Contrast-enhanced CT scans of his chest demonstrated a bilateral pulmonary artery aneurysm (Figure 1). To asses extension of the disease a transthoracic echocardiography showed a mobile right ventricular mass. A cardiac MRI was subsequently done, which showed a 3.8 cm 1.6 cm right ventricular mass attached to his interventricular septum (Figure 2). An ophthalmologic examination of our patient showed no evidence of iritis or retinal vasculitis.
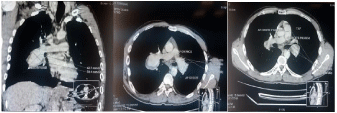
Figure 1: Contrast-enhanced CT scans of his chest demonstrated a bilateral pulmonary artery aneurysm.
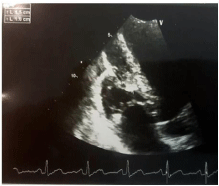
Figure 2: Transthoracic echocardiography showed a mobile right ventricular
mas.
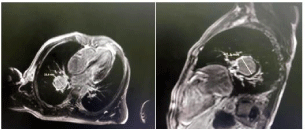
Figure 3: Cardiac MRI showed a right ventricular mass attached to his
interventricular septum.
He was thus diagnosed with Hughes-Stovin syndrome, which is a variant of Behcet’s disease.
A multidisciplinary discussion between the internists, thoracic surgeons and cardiovascular surgeons finally decided that anticoagulation therapy as well as any surgical or interventional therapy must be primarily avoided to initially. The patient underwent combined pulse therapy with methylprednisolone (1 g for three days) and cyclophosphamde (1 g per monthly) with 1 mg once a day of colchicine for initial management and stabilization of the aneurysms. No more hemoptysis has been recurred and the patient was discharged to be seen one month later for another pulse of cyclophosphamide.
Discussion
Hughes-Stovin syndrome is considered a variant of Behcet’s disease [7,8]. It classically affects young men aged between 12 and 40 years old, whom usually present with hemoptoic cough, dyspnea, chest pain and signs of pulmonary hypertension following history of deep venous thrombosis [1]. The cardiac thrombus mainly in the right ventricle keeps to be an exception in HSS [1,11].
Prevalence is unknown but less than 35 cases have been published in literature since its first description in 1959 by Hughes and Stovin [9].
The pathogenesis of Hughes-Stovin syndrome results from a vasculitis similar to that occurring in Behçet’s disease [1]. Vasculitis in Behçet’s disease particularly results in arterial occlusions, arterial aneurysms, venous occlusions, and varices [10], denoting systemic vessel involvement.
Hemoptysis keeps to be the main cause of death due the pulmonary aneurysm rupture in patient with Hughes Stovin syndrome.
As there are few cases published there is no treatment consensus for Hughes stovin syndrome. However, similar to the treatment protocols used in Behcet’s disease, treatment of Hughes-Stovin syndrome with steroids alone or in combination with immunosuppressant drugs, has been suggested [12]. It has been found that the use of immunosuppressant drugs, either corticosteroids or cytotoxic agents (a combination of cyclophosphamide and glucocorticoids), in patients with Hughes Stovin syndrome would have a positive impact on the stabilization of the pulmonary artery aneurysm walls [1,12] but not always useful in preventing disease progression particularly in the late stages of the disease [14].
If deep vein thrombosis, especially when it has a specific and particular localization, is present a therapeutic dilemma often occurs as regards the use of anticoagulants. This is what we had to deal with in our case where the patient has intracardiac thrombus. Anticoagulation may prevent the progression of thrombus and resolved it, but since it increases the risk of pulmonary aneurysm rupture which may lead to death with fatal hemoptysis, it is not recommended [6].
In our case, the first goal was to stabilize the wall of the aneurysms to reduce the risk of rebleeding. So we decided to avoid anticoagulation as well as any surgical or interventional therapy and to combine pulse therapy with methylprednisolone and cyclophosphamide as an initial management. This also agrees with the initial management protocol implemented by Umair K. and Taimur S [6].
Surgical resection of the affected segments of the lung has also been considered in cases of high risk rupture aneurysms limited to one segment or one lung [13]. But, the high morbidity and mortality associated with surgery, and the likelihood of multifocality and bilaterality of the pulmonary artery aneurysms at the time of diagnosis, makes transcatheter embolization an alternative to surgery as a life saving measure in many cases [1].
Conclusion
Our case shows a particular localization of thrombosis and the problem of treatment which keep to be a very difficult and hard decision especially when there is both a specific deep thrombosis and high risk pulmonary aneurysm.
References
- Weintraub JL, DeMayo R, Haskal ZJ, Scvir JS. Annual meeting film panel session: diagnosis and discussion of case 1: Hughes-Stovin syndrome. J Vasc Interv Radiol. 2001; 12: 53153-53154.
- Roberts DH, Jimenez JF, Golladay ES. Multiple pulmonary artery aneurysms and peripheral venous thromboses: the Hughes Stovin syndrome. Report of a case in a 12-year-old boy and a review of the literature. Pediatric Radiol. 1982; 12: 214-216.
- Ammann ME, Karnel F, Olbert F, Mayer K. Radiologic findings in the diagnosis of Hughes-Stovin syndrome. Ajr. 1991; 157: 1353-1354.
- Mahlo HR, Elsner K, Rieber A, Brambs HJ. New approach in the diagnosis of and therapy for Hughes-Stovin syndrome. Ajr. 1996; 167: 817-818.
- Yazici HFE. Mortality in Behçet’s syndrome. Clin Exp Rheumatol. 2008; 26: S138-S140.
- Umair Khalid, Taimur Saleem, Orphanet J. Hughes-Stovin Syndrome. Rare Dis. 2011; 6: 15.
- Bowman S, Honey M. Pulmonary arterial occlusions and aneurysms: a forme fruste of Behcet’s or Hughes-Stovin syndrome. British Heart Journal. 1990; 63: 66-68.
- Emad Y, Ragab Y, Shawki Ael H, Gheita T, El-Marakbi A, Salama MH. Hughes-Stovin syndrome: is it incomplete Behcet’s? Report of two cases and review of the literature. Clin Rheumatol. 2007; 26: 1993-1996.
- Hughes JP, Stovin PGI. Segmental pulmonary artery aneurysms with peripheral venous thrombosis. Br J Dis. 1959; 53: 19e27.
- Park JH, Han MC, Bettmann MA. Arterial manifestations of Behcet disease, AJR. 1984; 143: 821e -825e.
- Chalazonitis AN, Lachanis SB, Mitseas P, et al. Hughes-StovinSyndrome: a case report and review of the literature. Cases J. 2009; 2: 98.
- Lee J, Noh JW, Hwang JW, Kim H, Ahnn JK, Koh EM, et al. Successful cycophsphamide therapy with complete resolution of pulmonary artery aneurysm in Hughes Stovin syndrome patient. Clin Rheumatol. 2008; 27: 1455e-1458e.
- Durieux P, Bletry O, Huchon G, Wechsler B, Chretien J, Godeau P. Multiplepulmonary arterial aneurysms in Behcet’s disease and Hughes- Stovin syndrome. Am J Med. 1981; 71: 736e-741e.
- Tunaci M, Ozkorkmaz B, Tunaci A, Gul AEGBA. CT findings of pulmonaryartery aneurysms during treatment for Behcet’s disease. The AmericanJournal of Roentgenology, Radium Therapy and Nuclear Medicine. 1999; 172: 729-733.