
Case Report
Austin J Clin Case Rep. 2020; 7(5): 1183.
Severe Orbital Cellulitis Complicating Facial Malignant Staphylococcal Infection
Chabbar Imane*, Serghini Louai, Ouazzani Bahia and Berraho Amina
Ophthalmology B, Ibn-Sina University Hospital, Morocco
*Corresponding author: Imane Chabbar, Ophthalmology B, Ibn-Sina University Hospital, Morocco
Received: October 27, 2020; Accepted: November 12, 2020; Published: November 19, 2020
Abstract
Orbital cellulitis represents a major ophthalmological emergency. Malignant staphylococcal infection of the face is a rare cause of orbital cellulitis. It is the consequence of the infectious process extension to the orbital tissues with serious loco-regional and general complications. We report a case of a young diabetic child, presenting an inflammatory exophthalmos of the left eye with purulent secretions with a history of manipulation of a facial boil followed by swelling of the left side of face, occurring in a febrile context. The ophthalmological examination showed preseptal and orbital cellulitis complicating malignant staphylococcal infection of the face. Orbito-cerebral CT scan showed a left orbital abscess with exophthalmos and left facial cellulitis. An urgent hospitalization and parenteral antibiotherapy was immediately started. Clinical improvement under treatment was noted without functional recovery. We emphasize the importance of early diagnosis and urgent treatment of orbital cellulitis before the stage of irreversible complications.
Keywords: orbital cellulitis, malignant staphylococcal infection of the face, management, blindness
Introduction
Malignant staphylococcal infection of the face is a serious skin disease. It can occur following a manipulation of a facial boil. It is revealed by a rapidly diffuse cellulitis of the face [1]. Its extension is frequent towards the orbital cellular tissues causing a serious orbital cellulitis of unpredictable evolution and threatening the visual or even vital prognosis.
We report a case of severe orbital cellulitis in a young child occurring after neglected malignant staphylococcal infection of face and we emphasize the importance of early diagnosis and urgent treatment before the stage of complications.
Case Report
We report a case of a young male child, 14 years old, diabetic since the age of 12 years treated by insulin injection therapy with poorly controlled type 2 diabetes. He was presented to the ophthalmological emergency for an inflammatory exophthalmos of the left eye with purulent secretions. The interrogation revealed the appearance of a boil of nasal localization 15 days previously, followed by a progressive installation of a facial swelling after a boil manipulation with a fever and reduced general condition.
On ophthalmological examination, the visual acuity of the left eye was no light perception. We noted an inflammatory eyelid edema with purulent secretions, chemosis, irreducible exophthalmos and ophthalmoplegia with afferent pupillary deficit (Figure 1). The fundus examination was difficult. The examination of the face noted an inflammatory swelling of the frontal and left side, painful on palpation. On general examination, the child was feverish at 39.5° with reduced general condition.
Orbito-cerebral CT scan revealed a left preseptal and orbital cellulitis complicated by an orbital abscess with exophthalmos (Figure 2a, b), and left facial cellulitis with frontal purulent collection (Figure 3a, b).
The diagnosis of orbital cellulitis complicating malignant staphylococcal infection of the face was retained on clinical and radiological arguments. An urgent medical treatment was started without waiting for microbiological analysis, based on parenteral antibiotherapy: Ceftriaxone 2g and Gentamicin 160 mg, puncture-drainage of the purulent collection and glycaemic control. A bolus of corticotherapy was indicated after obtaining apyrexia and controlling the infection. Local treatments, antibiotic eye drops and lubricants were prescribed to protect the cornea from exposure and secondary infection. The course after treatment was marked by the regression of inflammatory edema and exophthalmos. However, the evolution of visual function was unfavorable with optic atrophy and permanent blindness (Figure 4a, b, c).
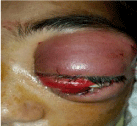
Figure 1: Photo of the left eye showing eyelid edema, chemosis, inflammatory
exophthalmos, ophthalmoplegia and purulent secretions + inflammatory
swelling of the left side of the face.
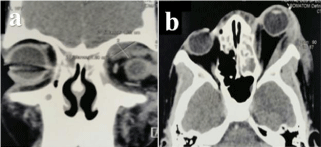
Figure 2 2 (a, b): Orbito-cerebral CT scan showing (a) a left orbital abscess
and (b) a left exophthalmos.

Figure 3 (a, b): Orbito-cerebral CT scan showing left facial cellulitis with left
frontal purulent collection.
Discussion
Malignant staphylococcal infection of the face is a serious skin disease. It can occur following a manipulation of a facial boil, more rarely a stye, a scrape, an infected insect bite or a dental infection [1,2]. It is mainly due to staphylococcus aureus, severe pathogen bacteria due to its virulence and resistance to antibiotics [3]. Factors favoring this condition are dominated by untimely manipulation of a facial boil, poor hygiene, diabetes, iron deficiency and primitive or acquired immune deficits [4]. It is revealed by a rapidly diffuse cellulitis of the face, with a reddish-purple and painful “staphylococcal” infiltration [3,4]. The extension is frequent towards orbital cellular tissues causing a severe orbital cellulitis of unpredictable evolution with protrusion of the eyeball [5]. The risk of cavernous sinus thrombophlebitis is significant with ophthalmoplegia and meningoencephalitis [6].
In the classic case, the irritated boil undergoes an extensive push and becomes protruding and painful. Very quickly, the swelling invades the face. The malignant staphylococcal infiltration is established: The cheek is swollen, the eyelids are oedematous, the palpebral cleft is closed with significant chemosis [1-4]. The infectious process thus reaches the preseptal and postseptal space of the orbit, causing severe orbital cellulitis. The evolution of orbital cellulitis is unpredictable. In some cases, the eyeball may be spared for a long time, while in other cases, despite prompt and appropriate treatment, visual function may be threatened and lead to blindness [7]. In addition, blindness remains a potentially serious complication of orbital infection. It can be the consequence of a mechanical optic neuropathy by elevation of the intra orbital pressure and/or a vascular origin by ischemia, central retinal artery occlusion, thrombophlebitis and/or an inflammatory origin (infectious neuritis) [8]. Appropriate and urgent management helps prevent progression to blindness. It includes, on the one hand, a meticulous general and ophthalmological examination and, on the other hand, an adapted imaging based on orbito-cerebral CT scan; necessary for the therapeutic approach decision [9,10].

Figure 4 (a, b, c): Photos showing the evolution (a) after abscess puncture
and 2 days of antibiotherapy (b) after 3 weeks (c) optic atrophy at the fundus
eye examination.
This case was a real challenge. The therapeutic management was particularly difficult given the young age of the patient, the existence of diabetic comorbidity and the delayed diagnosis until the stage of ocular complications, justifying then the poor functional result despite the regression of infectious and inflammatory phenomena.
Conclusion
Orbital cellulitis is a serious ophthalmological emergency. The infectious invasion of the orbit is most often of sinusitis origin. Malignant staphylococcal infection of the face is a rare cause of orbital cellulitis requiring appropriate clinical and paraclinical management. A delayed diagnosis and an inappropriate treatment can be a source of serious complications, affecting visual and even vital prognosis.
References
- Tognetti L, Martinelli C, Berti S, Hercogova J, Lotti T, Leoncini F, et al. Bacterial skin and soft tissue infections: review of the epidemiology, microbiology, aetiopathogenesis and treatment. J Eur Acad Dermatol Venereol. 2012; 26: 931-941.
- Briere M, Boutoille D, Caillon J, Potel G, Batard E. Infections a staphylocoques: aspects physiopathologiques, bacteriologiques et cliniques. EMC - Maladies infectieuses. 2014; 11: 1-9.
- Hurwitz Clinical Pediatric Dermatology. Bacterial, Mycobacterial, and protozoal infections of the Skin. In Fifth Edition: Elsevier Edn. 2016: 334-359.
- Caby F, Bismuth R, Bossi P. Infection’s a staphylocoques. EMC (Elsevier Masson SAS Paris), Traite de medecine Akos. 2010.
- Wane AM, Ba EA, Ndoye-Roth PA, Kameni A, Demedeiros M, Dieng MR, et al. Une experience senegalaise des cellulites orbitaires. J Fr. Ophtalmol. 2005; 28: 1089-1094.
- Ebright JR, Pace MT, Nazis AF. Septic thrombosis of the cavernous sinuses. Arch Intern Med. 2001; 161: 2671-2376.
- Fanella F, Inger E. Presentation and management of pediatric orbital cellulitis. Can J Infect Dis Med Microbiol. 2011; 22: 97-100.
- Mouriaux F, Rysanek B, Babin E, Cattoir V. Les cellulites orbitaires. J Fr Ophtalmol. 2012; 35: 52-57.
- Boivin L, Adenis J. Infections orbitaires de l'enfant : clinique, imagerie et traitement. J Fr Ophtalmol. 2009; 32: 368-373.
- Basraoui D, Elhajjami A, Jalal H. Imaging of orbital cellulitis in children: about 56 cases. Pan Afr Med J. 2018; 30: 94.