
Case Report
Austin J Clin Case Rep. 2021; 8(2): 1196.
The Pedicled Deep Inferior Epigastric Perforator (DIEP) Flap for Vulva Reconstruction
Bachleitner K*, Ndhlovu M, Schoeller T, Amr A and Weitgasser L
Department of Hand, Breast and Reconstructive Microsurgery, Teaching Hospital of the University of Tubingen Germany
*Corresponding author: Kathrin Bachleitner, Department of Hand, Breast, and Reconstructive Microsurgery of the Center for Plastic Surgery at the Marienhospital Stuttgart, Teaching Hospital of the University of Tubingen, Boheimstr 37, 70199 Stuttgart, Germany
Received: February 12, 2021; Accepted: March 01, 2021; Published: March 08, 2021
Abstract
Pain, scar contracture and soft tissue defects are common late sequel of acne inversa and Fournier’s gangrene. Aesthetical as well as functional reconstruction of the external vulva and labia majora can be very challenging. We present two cases where a pedicled Deep Inferior Epigastric Perforator (DIEP) flap for vulva reconstruction was implemented. In order to reconstruct both labia majora, we partially split the flap and raised a bilaterally pedicled DIEP flap. Many local flap techniques have been published on vulvar reconstruction. The aim of this paper is a discussion of the present literature and a review of current strategies for soft tissue restoration with the DIEP flap for vulva reconstruction. Wepresent and discuss two cases which were successfully reconstructed using the described surgical technique
Keywords: Vulva reconstruction; Pedicled flap; Hemi-DIEP; DIEP flap; Fournier gangrene; Acne inversa
Introduction
Most partial or full thickness soft tissue defects of the vulva are repaired with local flaps from the groin, the gluteal region or the inner thigh. In cases where these donor sites are already scarred or do not offer enough soft tissue for reconstruction, surgeons need to be more creative and need to seek alternative options. Only few publications have shown alternatives to local random pattern advancement or rotation flaps [1-3]. In patients with excess abdominal tissue the DIEP flap represents a favourable donor site for vulva reconstruction. Excess literature has been published about the free DIEP flap for breast and extremity reconstruction [4,5]. Only very few studies examined the pedicled DIEP flap for reconstruction of defects localized in close proximity to the lower abdomen, including the hip, groin and vulva so far. A standardized flap harvest as well as a controlable and favourable donor site morbidity represent outstanding advantages of the DIEP flap, which now represents the gold standard for autologous breast reconstruction. Opposed to breast-, vulva reconstruction can be more challenging due to the heterogeneity of each individual defect as well as the complexity and shape of the anatomy, which needs to be reconstructed. Several aspects such as sexual intercourse, micturition, cosmetic resurfacing, and replenishing dead space need to be carefully considered when choosing a flap and it’s donor site for reconstruction. Adjuvant radiotherapy or previous operations and scarring significantly increase complication rates, reduce healing capacity and can burn bridges for straightforward reconstructions with local flaps. Here we would like to discuss the current available literature on vulvar reconstruction with DIEP flap and present two cases of full thickness total vulvar reconstructions with bilaterally pedicled DIEP flaps.
Search Strategy and Inclusion Criteria of Literature Review
Literature research reporting on the use of the DIEP-flap for vulva reconstruction was done in PubMed (US National Library of Medicine, Bethesda, MD). We included articles using the DIEP flap for reconstruction of defects in the vulvar and vaginal region. The literature research was performed using the terms “DIEP-flap for vulva reconstruction” and “vulvar reconstruction”. The “related articles” feature was used to find additional articles and the references of the selected articles were screened for further publications.
Results of Literature Review
8 papers were found fulfilling our criteria. The reports were published between 2004 and 2015. To date only 29 reports of patients receiving a vulva reconstruction with the DIEP flap were identified. Patients were aged 19 to 77 years with an average of 56 years. The dimensions of the defects successfully reconstructed with DIEP flap ranged from 9 to 15 cm, whereas the maximal flap length measured 37 cm. Total flap necrosis did not occur in any patients whereas 2 partial flap necrosis, requiring reoperations were noted (6, 9%). Other complications included haematoma (3, 4%) and wound dehiscence (3, 4%). Altogether complications occurred in 17, 2% of patients.
Muneuchi [6] was 2005 among the first who described vulvar reconstruction with a pedicled DIEP flap. A present longitudinal scar in the midline of the lower abdomen from additional procedures, such as hysterectomy and salpingectomy necessitated a vertical flap design (15x8 cm). The flap was transferred through a subcutaneous tunnel into the defect. The transferred flap was then thinned by taking down the layer of fat to scarpa’s fascia in order to match the thickness to the surrounding thin skin.
Fang et al. [7] reported about 12 cases of thinned DIEP-flaps for perineal reconstruction. Debulking was performed initially after anatomy was analysed by preoperatively CT-scan. According to the authors, this step furthermore reduced the overall flap harvesting time. Here, the flap was thinned in a plane deep to the superficial inferior epigastric vein, also correlating to scarpa’s fascia. In the reported series a partial necrosis of the distal flap tip occurred in only a relatively large transverse flap measuring 24x8.5 cm.
Negosanti [8] proposed that all kinds of vulvar defects can be repaired either by a DIEP flap or a Lotus pedicled flap. According to their classification especially in type II resections (resections of vulvar and vagina), when more tissue to fill the pelvic dead space is required, a pedicled DIEP flap is preferred. The mean size of the defect reconstructed with aDIEP flap was 14.4x10.4x4.6 cm; All patients reported satisfactory results, both functionally and aesthetically.
Bodin [9] was the first who reported a Hemi-DIEP flap with two vascular pedicles for vulva reconstruction. This technical modification provides multiple benefits. Harvesting two pedicles offeresimproved blood supply of the DIEP flap angiosome, therefore avoiding distal flap necrosis, especially when the full width of the abdominal skin is required. Additionally flap modelling is more easily achievable with two hemi-abdominal flaps. The surgical procedure however is more time consuming and requires two rectus abdominis muscle dissections, which can increase the overall donor site morbidity and risk for postoperative lower abdominal bulging (Table1).
Author
Number of patients
Reconstruction of
Complications
Transverse vs. Vertical
Cause
Others
Muneuchi 2005 [6]
1
Vulva
0
Vertical (15x8 cm)
SC
-
Wang 2007 [15]
5
Vagina
1 haematoma
Rhomboid design (9x10-11x12 cm)
4x vaginal agenesis
1 total vaginal resection because of tumour-
Santanelli 2007 [16]
3
Vulva (+ vaginal introitus)
1 distal tip necrosis
Vertical (25x9-37x11 cm)
2x SC, 1x PD
-
Fang 2011 [7]
12
Vulva, vagina
1 partial flap necrosis
1 wound dehiscence
à only men9 vertical
3 transverse (4 men)5x vaginal agenesis
3x vulva or vaginal tumour4x penoscrotal PD
8 women
4 menFlap thinning
Cheng 2013 [17]
2
Vulva
0
Transverse
SC
Flap thinning
Negosanti 2015 [8]
5
Vulva
0
-
1x PD, 3x SC, 1x LSA
-
Zhang 2015 [11]
4
Vulva
1 minor complication
(151.1±67.12cm2)
-
1x ALT combined with a DIEP flap
Bodin
2015 [9]1
Vulva
0
Transverse
SC
Bilateral Hemi-DIEP
SC: Squamous Carcinoma; PD: Paget Disease; LSA: Lichen Sclerosus Atrophicus.
Table 1: DIEP-Flap for vulva reconstruction.
Another case series [10], published earlier in 2004, was excluded in our review, since no true DIEP flaps but muscle sparing TRAM flaps were used. Here the use of four unipedicled and two bipedicleddivided flaps were reported.
Case 1
A 33-year-old female presented with adherent scars and local fat atrophy in the pubic and vulva region after developing Fournier’s gangrene following an abortion. She consequently suffered a concomitant sepsis and total soft tissue necrosis of the vulva including labia majora and minora bilaterally. Multiple debridements followed. She then complained of painful hypersensitivity in the suprapubic region and chronic dyspareunia due to tight scarring and excessive pain with any form of penetration. This was mainly due to the excessive scar contractures and the lack of subcutaneous tissue and padding in the supra pubic region (Figure 1). After multiple debridements a soft tissue reconstruction was attempted using local flaps at a regional hospital. The local flaps utilized included bilateral random pattern gluteal rotation flaps, bilateral inner thigh VY-advancement flaps, and multiple transposition from groin and suprapubic area.
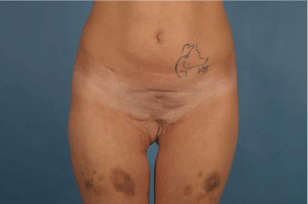
Figure 1: On preoperative examination after suffering from Fournier’s
gangrene.
Since multiple flaps already have been utilized from both inner thighs, groins, gluteal areas and suprapubic area and excessive scars were present a pedicled local DIEP-flap was used to replace the painful contracted scars and reshape the pubic region and to reconstruct both labia majora.
After perivulva scar release and recreation of the defect, a pedicled DIEP-flap was raised and mobilised. Dissection of the both pedicles was performed until the required length was obtained up to the origin from the external iliac artery and vein. The flap was then rotated 90° and guided through a subcutaneous tunnel into the genital defect. The deepithelialised portion of the pedicled DIEP-flap proximally was utilized for padding of the suprapubic area and buried, whilst the distal part was split (about 7cm) in order to reconstruct both labia majora and fully re-drape the full thickness vulvar defect (Figure 2).

Figure 2: Intraoperative procedure for vulva reconstruction with pedicled
DIEP-flap. (A): Rotating and partly splitting the flap. (B): Tunneling the flap
and shifting into the vaginal region.
The postoperative course was uneventful and no complications were recorded. To enhance the aesthetic result, minor corrections, such as liposuction and thinning of the flap were performed three months postoperatively. In the most recent follow-up two years postoperatively the paint is still satisfied with both functional and aesthetic result after the reconstruction (Figure 3).
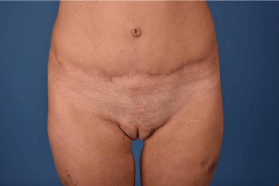
Figure 3: 1-year postoperative result.
Case 2
A 41-year-old female presented with severe scar contractures and hypersensitive pubic and perilabial areas after extensive debridement and secondary wound healing after years of suffering from hidradenitis suppurativa. She complained of excessive dyspareunia, constantly exsudating wounds and inability of intimacy due to scarring and disfiguration causing social reclusiveness and social withdrawal (Figure 4).
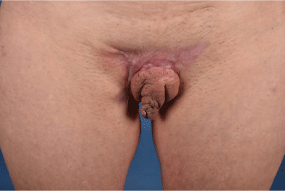
Figure 4: On preoperative examination of a patient suffering from acne
inversa.
On examination, a perivulvular scar was responsible for the distortion and disfiguration of the labia majora causing a pin cushion effect where both labia were profusely swollen due to chronic scar contracture and localized lymphedema. The massive scar contracture impaired bilateral thigh abduction. Sexual intercourse was not possible due to excessive pain when anticipated. A gynaecological exam excluded synechias or narrowing of the introitus vaginae. Dysesthesia was caused by a lack of subcutaneous padding due to scarring of the entire pubic and inguinal region.
As part of the reconstruction, a wide excision of scars was performed and a tunnelled bi-pedicled DIEP flap was raised. The flap was then guided through a subcutaneous tunnel into the labial region. The DIEP flap was then split into two independent flaps based on each individual pedicle for better positioning and malleability. The defect was entirely re-draped with flap tissue and an anatomical reconstruction was achieved. Further refinement surgery such as liposuction, scar release in the gluteal and inner thigh region with a rotation and transposition flap and wedge resection of labia minorae were additionally carried out (Figure 5).
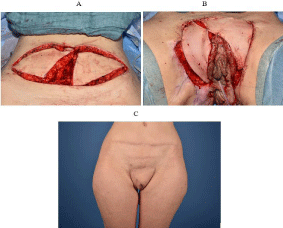
Figure 5: Double-pedicled- DIEP for vulva reconstruction, peri and
postoperative results. (A): Raising a double pedicled DIEP-flap and fully
splitting the flap. (B): Covering the defect zone after scar removal. (C): One
year post operative result.
Discussion
Vulva and vaginal debridement and consequent partial and full thickness defects as well as excessive scarring go along with a massive loss of quality of life [8]. Distortion of body image due to aesthetical and functional impairments may lead to psychological discomfort and further social reclusive behaviour. Zhang et al. [11] proved that vulvar reconstruction significantly improves quality of life and wellbeing. History of multiple operations, radical debridements and adjuvant radiotherapy often lead to extensive soft tissue defects, scarring and chronic pain as well as loss of function and dyspareunia.
The thin nature of the skin and overall lack of skin in the genital region makes reconstruction with local flaps difficult and can facilitate delayed wound healing and an increased postoperative morbidity [11].
The goal of vulvar reconstruction is to offer an adequate sized skin fold resembling the appearance of the labia majora8. Symmetry with the contralateral side, absence of stenosis at the vaginal orifice, functioning micturition, pain reduction through scar release correction and sufficient soft tissue padding are just a handful of demands that have to be met. Extensive soft tissue defects, which include both the vagina and perianal regions, are even more challenging due to amount of required malleable tissue.
A variety of different flaps have been described for vulva and vaginal reconstruction, ranging from local and free fasciocutaneous flaps and muscle flaps [12-14]. The choice of surgical approach, flap type and donor site depend on many factors, such as the patient’s prior treatment (including scars) and operations, which need to be carefully reviewed when formulating a reconstructive plan. The DIEP flap for vulva and vaginal reconstruction was first described by Muneuchi in 2005 [6]. More reports followed by Wang et al. [15] and Santanelli et al. [16].
The DIEP flap is known for its use in breast reconstruction as a free flap and rarely associated with genital reconstruction. Especially, when locoregional flaps have already been utilized, in irradiated defects or extensive scarring, the DIEP flap is considered as a gold standard for reconstruction by some authors [17]. The flap angiosome can be utilized either in a vertical or transverse design, depending on persisting scars e.g. long median longitudinal scars through radical vulvectomy or prior surgery [6,16]. The transverse donor site scar, after a DIEP flap harvest is easy to hide and can represent a favourable cosmesis in patients having excessive lower abdominal fat.
The flap raise and pedicle dissection is standardised and the blood supply of the angiosome is reliable and well known. In pedicled flaps no micro-anastomosis are needed and when the flap is transfered on a single pedicle it has a relatively wide reach around it’s donor site and can be used for reconstructions of the hip, groin and pubic area. It’s skin paddle, especially when using both pedicles can be even larger and the flap can be used for sufficient volume replacement with flap weights up to 1.5 kg or more. The large skin paddle with sufficient soft tissue thickness can furthermore be utilized to fill dead space or for resurfacing of large sized defects [7,8]. There have been concerns that the DIEP flap might be excessively bulky for genital reconstruction. However the thickness of the flap can easily be adjusted and flap thinning is safely possible when performed deep to scapha’s fascial plane [7,17] between the Scarpa´s fascia and the Superficial Inferior Epigastric Vein (SIEV).
To our knowledge, only two cases of bipedicled DIEP flaps have been reported in the literature so far, whereas only one of them was used for reconstruction of the vulva. Bodin et al. [9] reported an extended vulva reconstruction using a bipedicled transversely oriented DIEP flap and Zeng et al. [18] reported reconstruction of a bilateral extended groin defect with a hemi-DIEP flap.
The present manuscript presents a further report of a bipedicled DIEP flap for vulvar reconstruction and also describes and discusses a reconstruction using a smaller flap based on a single pedicle in comparison.
In both cases, an extensive bilateral defect of the vulva and both labia majora was reconstructed. In one case the DIEP-flap, which was only elevated on one pedicle was split partially for better contouring and an improved reconstructive result. The second case presented describes a flap raised on bilateral pedicles, which were then divided into two independent DIEP flaps. The advantage here was improved blood supply of the entire DIEP flap angiosome, a larger overall flap size as well as improved mobility of each individual flap offering better positioning and malleability. A drawback of bipedicled flaps is the bilateral insult of the abdominal wall, which can cause a higher risk for developing a postoperative lower abdominal bulge and longer operating time.
In this case presentation, we provide a small insight into the extraordinary utility of the pedicled DIEP flap for vulvar defect reconstruction. Although local random pattern rotation or VYadvancement flaps from the gluteal region or upper medial thigh and groin still present standard workhorses in most departments, the pedicled DIEP flap can be a powerful alternative option in cases where extensive scarring, radiotherapy and previous operations have burned all other bridges.
The aim of this manuscript was to increase overall awareness of how to troubleshoot and successfully manage these highly complex full thickness vulvar defects and extensive scarring of the genital region. The two cases described offer insight into two different reconstructive scenarios and options for reconstruction, which present a valuable alternative option for reconstruction, especially in patients where other flaps have already been used and the lower abdomen offers a favourable donor site. The pedicled DIEP flap is relatively quick and easy to harvest and provides malleable, mobile, well-padded and reliably perfused flap tissue, which is difficult to recruit elsewhere in close proximity to the genital area.
Conclusion
In conclusion, the vulvar region represents a challenging area to reconstruct and all options for a pleasing functional and soft tissue restoration need to be utilized including single or bipedicled lower abdominal flaps.
Note: The authors have no financial disclosures. All authors approved the final version to be published.
References
- Spear SL, Pellegrino CJ, Attinger CE, Potkul RK. Vulvar reconstruction using a mons pubis flap. Annals of plastic surgery. 1994; 32: 602-605.
- Bertani A, Riccio M, Belligolli A. Vulval reconstruction after cancer excision: the island groin flap technique. British journal of plastic surgery. 1990; 43: 159-161.
- Lee PK, Choi MS, Ahn ST, Oh DY, Rhie JW, Han KT. Gluteal fold V-Y advancement flap for vulvar and vaginal reconstruction: a new flap. Plastic and reconstructive surgery. 2006; 118: 401-406.
- Koshima ISS. Inferior epigastric artery skin flaps without rectus abdominis muscle. . British journal of plastic surgery. 1989; 42: 645-648.
- Van Landuyt KBP, Hamdi M, Tonnard P, Verpaele A, Monstrey S. The versatile DIEP flap: its use in lower extremity reconstruction. British journal of plastic surgery. 2005; 58: 2-13.
- Muneuchi G, Ohno M, Shiota A, Hata T, Igawa HH. Deep Inferior Epigastric Perforator (DIEP) flap for vulvar reconstruction after radical vulvectomy: a less invasive and simple procedure utilizing an abdominal incision wound. Annals of plastic surgery. 2005; 55: 427-429.
- Fang BR, Ameet H, Li XF, Lu Q, Wang XC, Zeng A, et al. Pedicled thinned deep inferior epigastric artery perforator flap for perineal reconstruction: a preliminary report. Journal of plastic, reconstructive & aesthetic surgery: JPRAS. 2011; 64: 1627-1634.
- Negosanti L, Sgarzani R, Fabbri E, et al. Vulvar Reconstruction by Perforator Flaps: Algorithm for Flap Choice Based on the Topography of the Defect. International journal of gynecological cancer: official journal of the International Gynecological Cancer Society. 2015; 25: 1322-1327.
- Bodin F, Robert E, Dissaux C, Weitbruch D, Bruant-Rodier C, Rodier JF. Extended vulvar immediate reconstruction using the bilateral transverse pedicled DIEP flap. Journal of plastic, reconstructive & aesthetic surgery: JPRAS. 2015; 68: 745-747.
- Murakami M, Hyakusoku H, Akimoto M, Mita S, Sasaki S. Use of deep inferior epigastric artery flaps for reconstruction of the female genitalia. Scandinavian journal of plastic and reconstructive surgery and hand surgery. 2004; 38: 215- 219.
- Zhang W, Zeng A, Yang J, Cao D, He X, Wang X, et al. Outcome of vulvar reconstruction in patients with advanced and recurrent vulvar malignancies. BMC cancer. 2015; 15: 851.
- Hashimoto I, Nakanishi H, Nagae H, Harada H, Sedo H. The gluteal-fold flap for vulvar and buttock reconstruction: anatomic study and adjustment of flap volume. Plastic and reconstructive surgery. 2001; 108: 1998-2005.
- Luo S, Raffoul W, Piaget F, Egloff DV. Anterolateral thigh fasciocutaneous flap in the difficult perineogenital reconstruction. Plastic and reconstructive surgery 2000; 105: 171-173.
- Huang JJ, Chang NJ, Chou HH, Wu CW, Abdelrahman M, Chen HY, et al. Pedicle perforator flaps for vulvar reconstruction--new generation of less invasive vulvar reconstruction with favorable results. Gynecologic oncology. 2015; 137: 66-72.
- Wang X, Qiao Q, Burd A, Liu Z, Zhao R, Song K, et al. A new technique of vaginal reconstruction with the deep inferior epigastric perforator flap: a preliminary report. Plastic and reconstructive surgery. 2007; 119: 1785-1790.
- Santanelli F, Paolini G, Renzi L, Persechino S. Preliminary experience in reconstruction of the vulva using the pedicled vertical deep inferior epigastric perforator flap. Plastic and reconstructive surgery. 2007; 120: 182-186.
- Cheng A, Saint-Cyr M. Split and thinned pedicle Deep Inferior Epigastric Perforator (DIEP) flap for vulvar reconstruction. Journal of reconstructive microsurgery. 2013; 29: 277-282.
- Zeng A, Xu J, Yan X, You L, Yang H. Pedicled deep inferior epigastric perforator flap: an alternative method to repair groin and scrotal defects. Annals of plastic surgery. 2006; 57: 285-288.