
Case Report
Austin J Clin Case Rep. 2021; 8(3): 1201.
Anesthetic Concerns in Patient with Wolf-Hirschhorn Syndrome: A Case Report
Sari M¹* and Cicekci F²
¹Department of Anesthesiology and Reanimation, Agri Teaching and Research Hospital, Turkey
²Department of Anesthesiology and Reanimation, University of Selcuk, Turkey
*Corresponding author: Sari M, Department of Anesthesiology and Reanimation, Agri Teaching and Research Hospital, Turkey
Received: December 04, 2020; Accepted: March 13, 2021; Published: March 20, 2021
Abstract
Wolf-Hirschhorn Syndrome (WHS) is a well-known, rare genetic disease, which isusually accompanied by prenatal and postnatal growth tension in psycho-motor retardation, which is associated with severe mental retardation, typical facial anomalies, midline defects, skeletal anomalies, hypotonia and contractions. It occurs as a result of deletion (4p-) in the distal part of the short arm of the 4th chromosome. It was aimed to discuss anesthesia management under general anesthesia accompanied by the literature in a case diagnosed with WHS who undergoing undescended testis and colostomy operations with developmental retardation.
Introduction
Wolf-Hirschhorn Syndrome (WHS) is a very rare hereditary disease resulting from the deletion of the distal short arm of chromosome 4 [1]. The prevalence of WHS has been reported to be approximately 1: 50,000 and is twice as common in females [1]. Patients with WHS are characterized by typical craniofacial features such as hypertelorism and “Greek warrior helmet appearance” of the nose, microcephaly, prominent glabella and a high forehead, ocular hyperlorism, epicanthus, high arched eyebrows, a short philtrum, micrognathia, and underdeveloped ears, facing downwards [1,2]. These patients have characteristic musculoskeletal anomalies, congenital heart defects, hearing loss, urinary tract malformations and structural brain abnormalities. Patients with WHS often have seizures and the prognosis is very poor. 38% of these patients die of heart failure or pneumonia before reaching the age of 2 [1-3]. WHS patients require corrective surgery due to the presence of various anomalies and general anesthesia is performed in many cases. However, due to the presence of various abnormalities, managing the airway, regulating muscle relaxation and controlling vital signs during surgery may be difficult. A patient diagnosed with WHS underwent Total Intravenous Anesthesia (TIVA). With the review of the literature related to this case report, we aimed to present our anesthesia concerns.
Case Presentation
A male patient, 65.2 cmheight and 4.5kg, 22 months and previously diagnosed with WHS by gene analysis, was admitted to undescended testis and colostomy surgery by pediatric surgery.He had a history of cardiac disease, cleft palate, seizure, including congenital aortic stenosis and pulmonary stenosis. The patient also had microcephaly and characteristic facial dysmorphism (Figure 1). The patient’s motor skills were such that he couldn’t stand alone without manual support. There was no abnormal family history. There were no prescription drugs for seizure management other than phenobarbital. Patient had previously received anesthesia for aortic correction surgery and cleft palate operation.
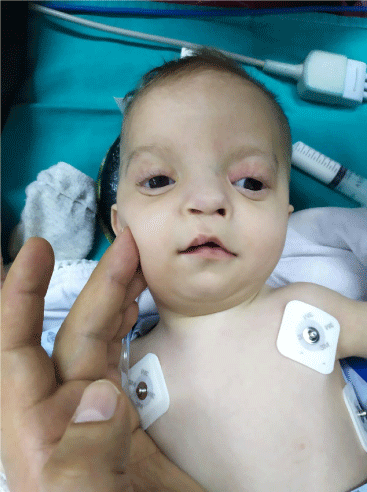
Figure 1: The patient has a high forehead with microcephaly, prominent
glabella, ocular hyperthyroidism, epicanthus, high arched eyebrows, a short
philtrum, a downward-facing mouth, and micrognatia typical of craniofacial
features.
Balloon valvuloplasty secondary changes, pulmonary stenosis and patent foromen oval were detected in patient’s echocardiogram in the preoperative evaluation. Infective endocarditis prophylaxis was performed 30 minutes before the operation. In the patient’s airway evaluation, difficult airway was predicted with grade III in the Mallampati classification system.
No premedication was performed during transfer. Heart rate was 110/min, blood pressure 84/51 mmHg, sPO2 96%, respiration rate 20/min and body temperature 36.2°C among preoperative vital signs. Prior to induction of anesthesia, preoxygenation was provided for more than about 3 minutes due to concerns about the difficulty endotracheal intubation.
Induction was performed with 3mg/kg propofol 1% 0.6 mg/ kgrocuronium was administered to facilitate tracheal intubation. The patient’s laryngoscopy was grade 4 in the Cormack Lehane classification. The second laryngoscopy was performed with Macintosh number 2 and pediatric frovaand 3 mm ID uncuffed tube. Intubation was confirmed by 5 point auscultation and capnogram. Anesthesia maintenance was achieved with 0.125-0.3 mg/kg/min IV propofol and 0.1-0.15 mcg/kg/min remifentanil.After intubation, blood pressure was 70-85/40-55 mmHg, heart rate was110-1557min, end-tidal CO2 was 33-42 mmHg.The temperature of the patient was provided by heating bed in the range of 36.4-37°C. The surgery was completed for 39 minutes without any surgical and anesthesia complications.Minimal blood loss occurred during the case. 50 cc’s of isotonic infusion was provided. The patient was transferred to the pediatric intensive care unit intubated for longer extubation time and more controlled extubation.
Discussion
Wolf-Hirschorn syndrome is a very rare hereditary disease caused by partial loss of the distal short arm of chromosome 4. It is associated with a high mortality rate of approximately 30% in the first 2 years of life due to congenital heart disease [3]. Patients with Wolf-Hirschhorn syndrome have characteristics such as short height and slow height gain, variable degrees of mental disability, epilepsy and heart disease following growth delay. Selection of a suitable size tracheal tube and preservation of intraoperatively stable hemodynamics may be critical problems for anesthetic management. It is known that an unexpected tracheal tube size may be required for short patients [4]. The appropriate size (inner diameter) of tracheal tubes for children was investigated [5,6]. Simple formulas were proposed using weight and height to estimate the optimal tracheal tube size and the age (in years) of the child was used in the formulas to select the size of the tracheal tube.However, age-based formulas [(age/4)+4] have been reported to be erroneous up to 60% of children [4]. In a study by Ginsburg et al. [5], during induction of a 21-monthold WHS female infant, tracheal intubation was difficult due to the fact that glotis was narrower than normal and intubation was achieved with 3.5 mm endotracheal intubation tube. Special attention should be paid to airway management because there are various craniofacial- abromalies in WHS patients. Prior to induction of anesthesia, the patient’s airway density should be examined and anesthesiologists should be prepared for the possibility of difficult intubation [10]. We thought that endotracheal intubation might be difficult in our patient, so we carefully took the patient’s medical history, examined the airway and performed related tests. We performed all procedures carefully, so endotracheal intubation was performed without great difficulty and anesthesia induction was performed safely.
Congenital heart disease is often associated with Wolf- Hirschhorn syndrome. Depending on the degree and type of heart disease, careful monitoring of hemodynamics is important. ASD, VSD and PS are considered mild in this patient. Anesthetic agents and their haemodynamic responses may cause significant circulatory disturbances [6].
Malignant Hyperthermia (MH) has been reported previously in Wolf-Hirschhorn Syndrome. If fever develops in a WHS patient during and after anesthesia, anesthesiologists should consider malignant hyperthermia and other causes, but our patient did not develop MH. MHhas been reported to occur during general anesthesia and after a surgical procedure. MH symptoms are tachypnea, tachycardia and hyperthermia [1]. If these symptoms develop, anesthesiologists should consider other possible causes such as overheating and infection and administer dantrolene.
Conclusion
As a result, patients with WHS may have various pre-peroperative problems. However, with careful evaluation of the airway, cardiovascular system and central nervous system and an appropriate anesthesia plan, anesthesiologists can perform a safe general anesthesia in WHS patients.
References
- Battaglia A, Filippi T, Carey JC. Update on the clinical features and natural history of Wolf-Hirschhorn (4p-) syndrome: experiencewith 87 patients and recommendations for routine health supervision. Am J Med Genet C Semin Med Genet. 2008; 148: 246-251.
- Battaglia A, Carey JC, South ST, Wright TJ. Wolf-Hirschhorn Syndrome. In: Gene Reviews [PMID: 20301362]. Pagon RA, Bird TD, Dolan CR, Stephens K (Editors). Seattle (WA), University of Washington, Seattle. 2002.
- Shannon NL, Maltby EL, Rigby AS, Quarrell OW. An epidemiological study of Wolf-Hirschhorn syndrome: life expectancy and cause of mortality. J Med Genet. 2001; 38: 674-679.
- Ginsburg R, Purcell-Jones G. Malignant hyperthermia in the Wolf- Hirschhorn syndrome. Anaesthesia. 1988; 43: 386-388.
- American Society of AnesthesiologistsTask Force on Management of the Difficult Airway. Practice guidelines for management of the difficult airway: an updated report by the American Society of AnesthesiologistsTask Force on Management of the Difficult Airway. Anesthesiology. 2013; 118: 251-270.
- Schubert S, Schmitz T, Weiss M, Nagdyman N, Huebler M, Alexi-Meskishvili V, et al. Continuous, non-invasive techniques to determine cardiac output in children after cardiac surgery: Evaluation of trans esophageal doppler and electric velocimetry. J Clin Monit Comput. 2008;22: 299-307.