
Research Article
Austin J Clin Case Rep. 2021; 8(5): 1211.
Another Brick in the Wall of an Ongoing Discussion– Reduction of Anastomotic Leaks after Colorectal Resection by Preoperative Mechanical Bowel Preparation in Combination with Oral and Parenteral Antibiotics?–A Clinical Retrospective Single Center Study
Safia O¹*, Tallbot SR², Kuebler S¹ and Mall JW¹
¹Department of General-Visceral and Minimally Invasive Surgery; KRH Siloah, Academic Teaching Hospital of the Hannover Medical School, Germany
²Department of Institute for Laboratory Animal Science and Central Animal Facility, Hannover Medical School, Germany
*Corresponding author: Safia O, Department of General- Visceral and Minimally Invasive Surgery; KRH Siloah, Academic Teaching Hospital of the Hannover Medical School, Stadionbruecke 4, 30459 Hannover, Germany
Received: April 29, 2021; Accepted: May 19, 2021; Published: May 26, 2021
Abstract
Background: In colorectal surgery, postoperative Anastomotic Leak (AL) is a serious complication. Besides the surgeon`s experience, bowel preparation may have an impact on AL, but the published data are still inconclusive. The purpose of this retrospective single center study was to investigate the role of preoperative Mechanical Bowel Preparation (MBP) in combination with Oral Antibiotic Bowel Preparation (OBP) and parenteral antibiotics in a certified highvolume colorectal center.
Methods: In the period of January 2017 to December 2019, all colon and rectal surgeries were recorded and separated into emergency and elective surgeries. Patients in the elective surgery group were further divided into two groups: patients with Bowel Preparation (BP) and patients without BP and were evaluated concerning to AL, postoperative hospital length of stay and mortality.
Results: Between 2017 to 2019, 625 patients underwent colorectal surgery. 262 patients had emergency operations and were therefore excluded from the study. 363 patients underwent colorectal elective surgery (197men, 166 women). 44.0% received Combined Bowel Preparation (CBP), 46.8% received no BP, 3.3% received OBP only, 4.1% received MBP only, and for 1.1% nothing was documented. CBP was not only associated with a reduction in the rate of AL (P=0.038) (14.1% vs. 4.4%), but also with reduction in mortality (P=0.032) (7.6% vs. 1.2%) and length of stay (P=0.016) (14 vs. 11 days).
Conclusion: Our retrospective data showed a significant impact of preoperative intestinal preparation with MBP in combination with OBP and parenteral antibiotics on AL, length of stay and mortality. Therefore we strongly recommend the use of this regimen of preoperative BP in elective colorectal surgery.
Keywords: Anastomotic insufficiency; Preoperative bowel preparation; Anastomotic leak; Elective colorectal resection
Introduction
In colorectal surgery, postoperative AL is considered one of the most serious complications, which can have multiple causes and whose genesis has not been conclusively clarified to date [1]. Until today we do not know how significant the role of BP is in reducing the rate of postoperative AL. In particular, the effect of combined intravenous and oral antibiotic prophylaxis together with MBP has not yet been adequately studied [2].
Many studies show a reduction in postoperative complications by combining MBP with OBP before colorectal surgical procedures. In 2017 Klinger and colleagues suggested that combined bowel preparation should be used before any elective colorectal resection unless contraindications exist” [3]. Nevertheless, it is still not common practice in Germany to use a combination of MBP with OBP as well as intravenous antibiosis in elective colorectal surgery. Zmora et al. found that elective colorectal surgery was safer without MBP. Accordingly, preoperative MBP should be performed selectively, e.g., in cases where intraoperative colonoscopy would likely be required [4].
Atkinson et al. suggested that preoperative antibiotic administration alone results in a decrease in Surgical Site Infections (SSI) and advised against MBP [5]. Particularly with the proliferation of fast-track surgery, selective BP and preoperative antibiotic preparation of the bowel was increasingly criticized [6].
Overall, findings are inconsistent. Further studies demonstrate that CBP alone can reduce the incidence of postoperative AL. No effect has been demonstrated with the use of MBP alone or OBP alone [7,8]. The effectiveness of CBP is based on the massive reduction of bowel contents and the resulting significant reduction of gram-negative germs. These are usually considered to be the source of infectious pathogens in anastomotic infections. Accordingly, the local dilution of oral antibiotics in the intestine is lower and there is a faster and easier reduction of the bacterial load in the intestine [9].
According to the changing recommendations in the past years we applied different regimens to our elective colorectal surgery patients. Whereas from Jan 2017 to Feb. 2018 no routine bowel preparation was administered, we changed the regimen to strict bowel preparation with administration of oral antibiotics in the following period after. Therefore it was feasible to compare the two groups of patients. The aim of this retrospective study was to investigate whether the standardized administration of CBP (MBP + OBP) had an impact on the incidence of AL in elective colorectal surgery compared to no BP in a certified high-volume bowel center. A standardized antibiotic regimen and MBP was used.
Materials and Methods
Study design
Between January 2017 and December 2019, all consecutive colon and rectal surgery files were recorded and initially separated into emergency and elective surgery retrospectively. There were 625 patients enrolled in the study. In elective surgeries, patients received CBP one day before the scheduled surgery. A standard protocol for oral antibiotics and mechanical bowel preparation was used. This consists of 3x1g Neomycin, 3x500mg Metronidazole, 2000 ml Moviprep® (Macrogol), 2000 ml clear liquid.
All patients who were ventilated preoperatively or were septic were excluded. Emergency surgeries did not receive standard BP and were therefore not included in the study. Also excluded were all elective surgeries with discontinuity resection, as AL could not occur in those patients. Furthermore, patients with other main oncologic diagnoses such as hematological or lymphatic cancer were excluded. Undocumented or unknown procedures were also excluded. Thus, 363 patients remained for evaluation in the study (Figure 1).
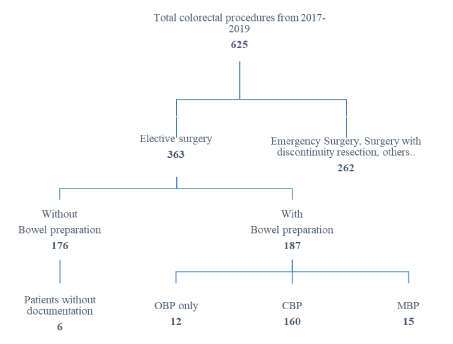
Figure 1: Study design of the collected patients and different groups.
Data collection
Patients were divided into two groups. In the first group no BP was performed, in the second group a preoperative BP (MBP & OBP) was administered. In the further evaluation, two groups were considered in which only mechanical or antibiotic bowel preparation was performed. These two groups were included in the group with preoperative BP without differentiation between combined or simple BP in the analysis. For statistical analysis, different variables were combined, and a dummy variable was created that gave us the total BP. This summary contains the combined information: MBP or/ and OBP (Table I). In addition, all groups were evaluated separately (Table II). As a result, five subgroups were created. Patients were categorized according to the applied BP:
• No bowel preparation
• Only mechanical bowel preparation
• Antibiotic bowel preparation only
• Total preoperative bowel preparation (Including patients with MBP or/and OBP)
• Combined preoperative bowel preparation (Only patients with MBP and OBP)
From January 2017 to February 2018, all patients received no BP, after having changed the standard preoperative protocol preparation for CRC patients undergoing elective surgery from March 2018 to December 2019 most patients received BP. There were 170 patients without any bowel preparation and 160 patients with CBP. 12 patients received OBP only without the MBP. These were mainly patients with a known allergic reaction to MOVIPREP® and/or patients with advanced bowel stenosis to protect them from ileus or aspiration pneumonia. 15 patients received only MBP without OBP. These patients either had a previous allergic reaction to oral antibiotics or received negligent treatment. In 6 patients, no documentation was found at all, and they were included in the no BP- group. In an additional seventh case no documentation was filed for antibiotics only. All patients received preoperative parenteral antibiotics with a 2nd generation cephalosporin and metronidazole immediately before surgery.
Statistical tests and procedures: Categorical data were counted and converted to percentages. In the tables, the percentage fractions were divided according to the group memberships. For continuous data (length of stay and age), the median and range were calculated. Normal distribution tests were performed using Shapiro-Wilk’s test and control QQ plots. Both continuous data (length of stay and age are not normally distributed) do not meet the requirements of a t-test or ANOVA, therefore analysis using non-parametric statistics is indicated.
Group differences in the tables were calculated for categorical data using a Fisher’s Exact Test. When creating the subgroup table, the chi-square test had to be used because the number of subgroups and samples did not allow the Fisher’s Exact Test to be calculated. To exclude a possible inaccuracy nevertheless, the p-value of the chi-square test was determined with the help of a 10000-fold bootstrapping. For the calculation of the group differences of the continuous data, the Kruskal-Wallis test was used, or the Mann Whitney U-test in the case of two group comparisons.
Results
The median age of the patients (n=364) was 69 years. The youngest patient was 20 years old, and the oldest was 93 years old. The median age of patients without BP (n=176) was 70 years, and with BP (n=187) was 68 years. Thus both groups were comparable regarding age (p=0.389). 68% of surgical indications were due to malignant tumors. 61.8% of the total AL occurred in patients with malignant tumors of the lower GI tract. With 85 patients and 23.4% of the total group, diverticulitis was the second most common reason for indication of elective surgery after malignant tumors. Approximately 94% of patients in all groups had an ASA status of II or III. In the group of patients with postoperative AI, all patients had either an ASA II (n=168) or ASA III (n=173) stage. Overall, blood was transfused in 12.4% of all patients. In 4 patients with postoperative AL (11.8%) blood was transfused intraoperatively. No correlation was found between AL and blood transfusions. However, our data showed that the number of blood transfusions performed was related to the BP applied. Blood transfusion was necessary more often when no BP was applied initially than in patients who received CBP (p=0.02).
In addition, there was a significant difference in the length of stay and mortality of patients in relation to the different BP. The average length of stay was 12 days in the entire group. The group with CBP showed a statistically significant difference of only 11 days (p=0.016). In the entire group of patients with preoperative BP, the average length of stay was 12 days (p=0.02) and 14 days without BP. Of a total of 363 patients operated on, 17 (4.7%) patients died. Of these, two patients received CBP (11.7%). Two patients suffered postoperative AL (11.7%). The difference in BP had a significant effect on mortality (p=0.003). Laparoscopic surgery was performed in 175 patients (48.2%). Laparotomy was performed in 188 patients (51.8%). Of these, 20 patients (10.6%) developed postoperative AL (58.8%). There was no significant difference regarding the type of surgery (laparoscopic vs. open) (p=0.12). In the operation-specific data of patients with AL, the influence of the area of the anastomosis is on the border of significance, but not yet decisive. Even if the p-value is close to the limit (p=0.07), a possible significance can be assumed.
Our results show that CBP is clearly associated with a reduction in AL-rate from 14.1% (Z=24 of 170) in patients without BP, to 4.4% (Z=7 of 160) in patients with CBP (p=0.038). Also, in the evaluation of the total group (Table II) a statistically significant difference regarding the AL-rate from 13.6% without BP (Z=24) to 5.3% with BP (Z=10) (p=0.011) could be registered. Table I shows the descriptive analysis of the total study data according to the different subgroups. All data collected mentioned up to this point are summarized in Table I. In the groups that received only antibiotics or only MBP, the enrolled number of cases was too small for statistical evaluation. Regarding the main study endpoint AL, there was a significant difference between both groups favouring the CBP. (Figure 2) (Odds- Ratio (OR) =0.35880, 2.5%=0.14821, 97.5%=0.8081, P=0.01071). If the OR is less than 1, the presence of the feature “bowel preparation” lowers the probability for the presence of the feature AL.
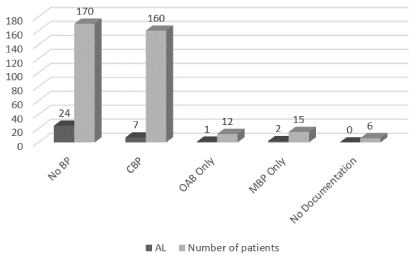
Figure 2: Anastomotic leakage (AL) in the different subgroups.
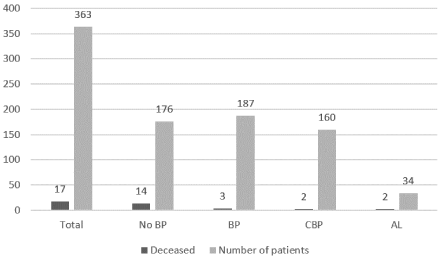
Figure 3: Mortality in the different subgroups.
Whole group
Without BP
(N=176)Whole group
With BP
(N=187)Total
(N=363)p value
Length of stay
0.021
Median
(Range)14
(5.000, 145.000)12
(5.000,98.000)12
(5.000,145.000)
Mortality
0.005
Yes
No14 (8.0%)
162 (92.0%)3 (1.6%)
184 (98.4%)17 (4.7%)
346 (95.3%)
Types of intervention
0.916
Laparoscopic
Open84 (47.7%)
92 (52.3%)91 (48.7%)
96 (51.3%)175 (48.2%)
188 (51.8%)
Anastomosis technique
0.251
Hand
Stapler57 (32.4%)
119(67.6%)50 (26.7%)
137 (73.3%)107 (29.5%)
256 (70.5%)
MBP
< 0.001
Yes
No
n.d*0 (0.0%)
170 (96.6%)
6(3.4%)175 (93.6%)
12 (6.4%)
0(0.0%)175 (48.2%)
182 (50.1%)
6(1.7%)
OBP
< 0.001
Yes
No
n.d.*0 (0.0%)
170 (96.6%)
6 (3.4%)172 (92.0%)
14 (7.5%)
1 (0.5%)172 (47.4%)
184 (50.7%)
7 (1.9%)
Anastomotic leakage
0.011
No
Yes152 (86.4%)
24 (13.6%)177 (94.7%)
10 (5.3%)329 (90.6%)
34 (9.4%)
Table I: Descriptive analysis of study data with division of total group into with and without bowel preparation.
Discussion
In the past decades bowel preparation prior to colorectal surgery has been managed inconsistently and variably in different continents. Substantial clinical studies have been published with inconsistent findings regarding efficacy and efficiency due to different outcomes [9-14]. It has often been suggested that vigorous preoperative MBP, along with the use of OBP, reduces the risk of septic complications after elective colorectal surgery [12]. After patients regularly received MBP in the 1970s, the first study questioning the need for MBP was published in 1972 In the 1990s, various studies failed to demonstrate a difference in wound infection and AL rates between groups of participants who did or did not receive MBP [16-20]. Moreover, a trend suggesting that MBP could pose risks such as significant preoperative homeostasis disturbances, renal function impairment, nausea, vomiting, and electrolyte disturbances was noted [9,21]. However, in recent years, new studies have demonstrated that preoperative CBP, consisting of MBP in conjunction with OBP, including standard parenteral antibiotics, reduces the rate of AL. In 2013 a study by Roos et al. suggested that the combination of perioperative selective decontamination of the digestive tract and perioperative intravenous antibiotics in elective gastrointestinal surgery reduces the rate of postoperative infections, including AL, compared with the use of intravenous antibiotics alone [22]. Similar results were shown in 2015 by a study by Chen et al. [9]. Data from Klinger et al. in 2017 showed that compared to no BP, CBP prior to colon or rectal surgery was associated with a reduced likelihood of SSI, infectious complications, AL, wound dehiscence, C. difficile colitis, and reduced length of stay [3]. Garfinkle et al. confirmed these findings in another study 2017 as well [12]. However, no additional benefit was found from CBP compared with OBP administration alone. A recent 2020 study by Purun Lei et al showed that the combination of MBP and OBP was associated with a significant decrease in the overall incidence of SSIs, superficial SSIs, and hospital costs [23].
Our results clearly indicate that preoperative CBP is definitely associated with a reduction of the rate of anastomotic insufficiency following colorectal surgery compared to patients without BP. Furthermore, a consecutive reduction in mortality and the length of stay of the patients, reduced from 14 days to 11 days was observed. Also, in the evaluation of the total group (Table II), a statistically significant difference was found regarding the AL rate, mortality, and length of stay. During the evaluation, it was deliberately not distinguished whether the oncologic patients with AL had a higher tumor stage, so that a realistic picture of the general care after colorectal surgery could be obtained. Here, a clear correlation between the combined preoperative BP and the reduction of the AL-rate was shown. Given the limitation of a retrospective study design our results nevertheless strongly indicate to favour preoperative bowel preparation in patients undergoing elective colorectal surgery. In our results it is apparent that CBP leads to lower rates of anastomotic insufficiency and the data support the results of other investigators as mentioned above [3,9,22,23]. However, it is still unknown what the ideal MBP and OBP are. In addition, this work does not answer the question as to whether exclusive OBP or MBP also may lead to a reduced AL rate. The best time of administration of preoperative BP is also unclear.
CBP
(N=160)No BP
(N=170)n.d.
(N=6)OBP
Only
(N=12)MBP
Only
(N=15)Total
(N=363)p value
Age
0.389
Median
(Range)68
(20.00,93.00)70
(28.00,90.00)58.5
(50.00, 80.00)71.5
(38.00,90.00)78
(34.00,86.00)69
(20.00,93.00)Sex
0.649
Male
Female88 (55.0%)
72 (45.0%)94 (55.3%)
76 (44.7%)4 (66.7%)
2 (33.3%)5 (41.7%)
7 (58.3%)6 (40.0%)
9 (60.0%)197(54.3%)
166(45.7%)BMI
0.272
Median
(Range)26.4
(17.60,40.00)25.6
(13.80, 46.90)24.95
(19.10, 28.10)24.35
(14.00, 39.50)25.3
(19.50, 40.80)25.8
(13.80, 46.90)Diagnosis
0.502
Cancer
Diverticulitis
IBD
Benign Tumor
Other112 (70.0%)
37 (23.1%)
3 (1.9%)
1 (0.6%)
7 (4.4%)112(65.9%)
40 (23.5%)
8 (4.7%)
5 (2.9%)
5 (2.9%)2 (33.3%)
3 (50.0%)
0 (0.0%)
0 (0.0%)
1 (16.7%)8 (66.7%)
3 (25.0%)
0 (0.0%)
0 (0.0%)
1 (8.3%)13 (86.7%)
2 (13.3%)
0 (0.0%)
0 (0.0%)
0 (0.0%)247(68.0%)
85 (23.4%)
11 (3.0%)
6 (1.7%)
14 (3.9%)Types of intervention
0.12
Laparoscopic
Open84 (52.5%)
76 (47.5%)81 (47.6%)
89 (52.4%)3 (50.0%)
3 (50.0%)2 (16.7%)
10 (83.3%)5 (33.3%)
10 (66.7%)175(48.2%)
188(51.8%)Anastomosis technique
0.225
Hand
Stapler40 (25.0%)
120(75.0%)54 (31.8%)
116(68.2%)3 (50.0%)
3 (50.0%)6 (50.0%)
6 (50.0%)4 (26.7%)
11 (73.3%)107(29.5%)
256(70.5%)Anastomotic leakage
0.038
Yes
No7 (4.4%)
153 (95.6%)24 (14.1%)
146(85.9%)0 (0.0%)
6 (100.0%)1 (8.3%)
11 (91.7%)2 (13.3%)
13 (86.7%)34 (9.4%)
329(90.6%)Mortality
0.032
Yes
No2 (1.2%)
158 (98.8%)13 (7.6%)
157(92.4%)1 (16.7%)
5 (83.3%)1 (8.3%)
11 (91.7%)0 (0.0%)
15(100%)17 (4.7%)
346(95.3%)Length of stay
0.016
Median
(Range)11
(5.00, 98.00)14
(5.00, 145.00)10.5
(8.00,27.00)15.5
(6.00, 67.00)13
(7.00, 41.00)12
(5.00, 145.00)
Table II: Descriptive analysis of patients with division into subgroups.
The debate on the role of MBP in combination with OBP in elective colorectal surgery has now been a topic for more than 50 year during which further questions have remained open that have not been conclusively resolved to date. However, there seems to be no doubt about the fact that MBP in combination with OBP can meaningfully contribute to the reduction of anastomotic insufficiency and consecutively to mortality.
Conclusion
This retrospective study shows that combined preoperative CBP is associated with a reduction in anastomotic insufficiency rate, mortality, and length of hospital stay. This is desirable not only from a medical but also from an economic point of view.
References
- Weidenhagen R, Spelsberg F, Strauss T. Anastomoseninsuffizienz in der kolorektalen Chirurgie. 2007; 42: 165-172.
- Flemming S, Germer CT. Oral antibiotic prophylaxis for bowel decontamination before elective colorectal surgery: Current body of evidence and recommendations. 2020; 91: 128-133.
- Aaron L, Klinger, MD, Heather Green MS. The Role of Bowel Preparation in Colorectal Surgery (Results of the 2012-2015 ACS-NSQIP Data. 2017 Wolters Kluwer Health 1-7. 2019; 269: 671-677.
- Oded Zmora, MD, Ahmad Mahajna, MD, Bar-Zakai B. Colon and Rectal Surgery without Mechanical Bowel Preparation, A Randomized Prospective Trial. 2003; 363-367.
- Atkinson SJ, Swenson BR, Hanseman DJ, et al. In the absence of a mechanical bowel prep, does the addition of pre-operative oral antibiotics to parental antibiotics decrease the incidence of surgical site infection after elective segmental colectomy? Surg Infect (Larchmt). 2015; 16: 728–732.
- Kehlet H. et al. Physiologic effects of bowel preparation. Diseases of the colon & rectum. 2004; 47: 1397-1402.
- Scarborough JE, Mantyh CR, Sun Z, Migaly J. Combined mechanical and oral antibiotic bowel preparation reduces incisional surgical site infection and anastomotic leak rates after elective colorectal resection: an analysis of colectomy-targeted ACS NSQIP. Ann Surg. 2015; 262: 331–337.
- Moghadamyeghaneh Z, Hanna MH, Carmichael JC, et al. Nationwide analysis of outcomes of bowel preparation in colon surgery. J Am Coll Surg. 2015; 220: 912–920.
- Chen M, Song X. Department of General Surgery, Xiamen Traditional Chinese Medicine Hospital, Xiamen, China, Comparing Mechanical Bowel Preparation with Both Oral and Systemic Antibiotics Versus Mechanical Bowel Preparation. 2016; 59: 70-77.
- Bucher P, Gervaz P, Soravia C, et al. Randomized clinical trial of mechanical bowel preparation versus no preparation before elective left-sided colorectal surgery. Br J Surg. 2005; 92: 409–414.
- Guenaga KF, Matos D, Wille-Jorgensen P. Mechanical bowel preparation for elective colorectal surgery. Cochrane Database Syst Rev. 2011; 9: CD001544.
- Richard Garfinkle, M.D., Jad Abou-Khalil, M.D, et al. Is There a Role for Oral Antibiotic Preparaion Alone Before Colorectal Surgery? ACS-NSQIP Analysis by Coarsened Exact Matching. 2017; 60: 734-736.
- Kim EK, Sheetz KH, Bonn J, et al. A statewide colectomy experience: the role of full bowel preparation in preventing surgical site infection. Ann Surg. 2014; 259: 310–314.
- Bucher P, Mermillod B, Gervaz P, Morel P. Mechanical bowel preparation for elective colorectal surgery: a meta-analysis. Arch Surg. 2004; 139: 1359– 1364.
- Hughes ESR. Asepsis in large-bowel surgery. Ann Roy Coll Surg Engl. 1972; 51: 347-356.
- Brownson P, Jenkins AS, Nott D, Ellenbogen S. Mechanical bowel preparation before colorectal surgery: results of a prospective randomised trial. Br J Surg. 1992; 79: 461-462.
- Burke P, Mealy K, Gillen P, Joyce W, Traynor O, Hyland J. Requirement for bowel preparation in colorectal surgery. Br J Surg. 1994; 81: 907-910.
- Fillmann EEP, Fillmann HS, Fillmann LS. Cirurgia colorretal eletiva sem preparo. Rev Bras Coloproct. 1995; 15: 70-71.
- Miettinen RPJ, Laitinen ST, Makela JT, Paakkonen ME. Bowel preparation with oral polyethylene glycol electrolyte solution vs. no preparation in elective open colorectal surgery. Dis Colon Rectum. 2000; 43: 669-677.
- Santos JCM Jr, Batista J, Sirimarco MT, Guimarães AS, Levy CE. Prospective randomised trial of mechanical bowel preparation in patients undergoing elective colorectal surgery. Br J Surg. 1994; 81: 1673-1676.
- McCoubrey AS. The use of mechanical bowel preparation in elective colorectal surgery. Ulster Med J Sep. 2007; 76: 127–130.
- Roos D, Dijksman LM. Systematic review of perioperative selective decontamination of the digestive tract in elective gastrointestinal surgery. 2013; 100: 1584-1588.
- Lei P, Ruan Y, Yang X. Preoperative mechanical bowel preparation with oral antibiotics reduces surgical site infection after elective colorectal surgery for malignancies: results of a propensity matching analysis. 2020; 18: 35.
Citation: Safia O, Tallbot SR, Kuebler S and Mall JW. Another Brick in the Wall of an Ongoing Discussion– Reduction of Anastomotic Leaks after Colorectal Resection by Preoperative Mechanical Bowel Preparation in Combination with Oral and Parenteral Antibiotics?–A Clinical Retrospective Single Center Study. Austin J Clin Case Rep. 2021; 8(5): 1211.