
Case Report
Austin J Clin Case Rep. 2022; 9(3): 1248.
Complete Avulsion of the Nipple-Areolar Complex Treated by One-Stage Reconstruction Using a Graft In Situ
Wu Y-H¹, Tan Q-W², Lu S³, Zhang W-F³, Lv Q³ and Chen J¹*
¹Department of Breast Surgery, West China Hospital, Sichuan University, Chengdu, China
²Department of Breast Surgery, Clinical Research Center for breast, West China Hospital, Sichuan University, Chengdu, China
³Department of Thyroid and Breast Surgery, Qiandongnan People’s Hospital, Guizhou, China
*Corresponding author: Jie Chen, Department of Breast Surgery, West China Hospital, Sichuan University, Guoxue Street 37#, Chengdu 610041, China
Received: February 28, 2022; Accepted: March 19, 2022; Published: March 26, 2022
Abstract
Background: Cases of complete avulsion of the Nipple-Areolar Complex (NAC) due to trauma are rare. The avulsed NAC can be replanted in situ if the vessels and nerves were anastomosed appropriately. However, this type of surgery is more complex, and requires longer operation times and the surgeon with training and experience of anastomosis of small vessels. We are looking for a more simple and effective method, which can be widely used.
Case Presentation: We reported a 19-year old girl whose left NAC had been completely avulsed by accident. We used a simple one-stage reconstruction surgery to modify the avulsed NAC as a tissue graft in situ. After 24 months, the reconstructed left nipple showed a similar appearance to the right. In addition, the patient showed high satisfaction with her breast appearance.
Discussion: Tissue graft in situ might be a simple, safe and reliable surgical procedure for completely NAC post-avulsion transplantation.
Keywords: Nipple reconstruction; Nipple-areolar complex avulsion; Tissue graft in situ
Introduction
Complete avulsion of the Nipple-Areolar Complex (NAC) due to trauma is a rare event. It has been reported that, the avulsed NAC can be replanted successfully in situ if the vessels and nerves were anastomosed appropriately [1]. However, this type of surgery is more complex, and requires longer operation times and the surgeon with training and experience of anastomosis of small vessels. In this case, we reported a sample one-stage reconstruction for women with complete NAC avulsion without vascular anastomosis.
Case Presentation
A 19 years old female patient fell from the bunk bed while sleeping, and hurt her left nipple. She admitted to our hospital 5 hours later. By physical examination, we found her left nipple was nearly completely avulsed, which only around 1/4 skin tissue was connected with the skin around the breast (Figure 1a and 1b). We removed all necrotic tissue and subcutaneous fat under the nipple-areolar complex (Figure 1c and 1d). There was a rough surface and a nearly 10 × 5 mm epidermis defect at 6 o’clock of the breast skin. Furthermore, the avulsed NAC began to show the signs of ischemia, which including dark colour, low skin temperature and no active bleeding in the wound. After debridement and sterilisation, we also found that there were no suitable blood vessels or nerves for anastomosis.
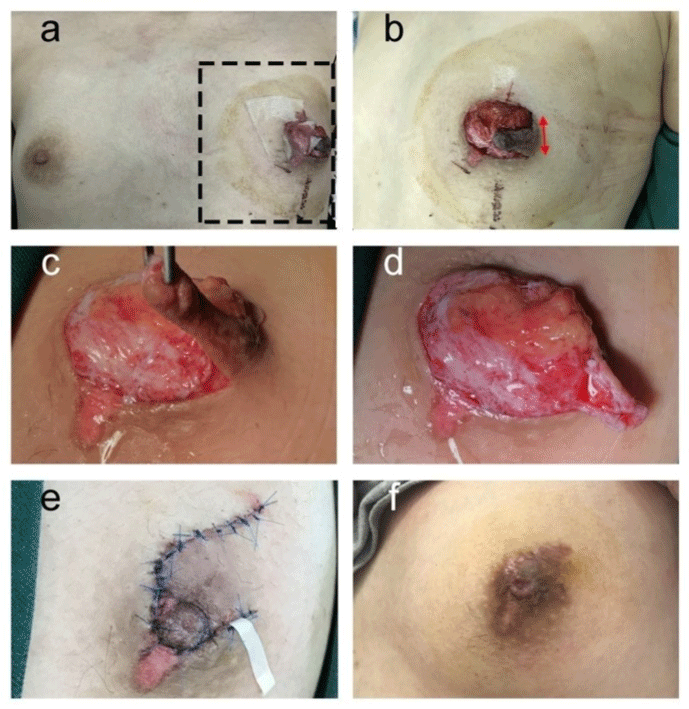
Figure 1: a) An 19-year-old female patient presented with a completely
avulsed left NAC caused by trauma (red arrow); b) Only around 1/4 skin was
connected with skin around the breast; c, d) We removed all necrotic tissue
and subcutaneous fat under the nipple-areolar complex. e) We performed an
interrupted suture to reconstruct the NAC. f) Six months after the surgery, the
reconstructed left nipple was survived.
After discussing with the patient, we decided to reconstruct a new NAC in situ by using the avulsed one. To improve the survival of NAC, we removed necrotic skin and tissue, subcutaneous adipose tissue and some ducts on the avulsed NAC in order to get thinner transplanted NAC skin grafts which can provide a better survival chance for avulsed NAC. Because the patient had bilateral low height nipples, we didn’t use the underlying breast tissue to make pillar flap as other report [2]. We performed an interrupted suture to reconstruct the NAC (Figure 1e), and a drainage of rubber was inserted under the NAC for avoiding seroma. Six months after the surgery, the reconstructed left nipple was survived (Figure 1f). 24 months after the surgery, the reconstructed left nipple showed a similar appearance to the right (Figure 2). Though, the patient has a little hypoesthesia with left side NAC. Moreover, we did the BREAST-Q to evaluate both satisfaction and quality of life for patient at 6 months and 24 months after the operation. Also, we did AIS (Aesthetic Items Scale) to evaluate aesthetic outcome for the doctors at the same time. We found that both patient and doctor had high satisfaction with this surgery, and scores did not decrease over time (Table 1 and 2).

Figure 2: 24 months after surgery. a) Coronal view of both breasts. b) Left
breast. c) Right breast. d) Side view of left nipple. e) Coronal view of left
nipple.
Variables
BREAST-Q Score (from 0-100)
6 months after surgery
24 months after surgery
Psychosocial Well-Being
55
64
Sexual Well-Being
50
50
Satisfaction with Breasts
82
88
Physical Well-Being: Chest
52
45
Table 1: BREAST-Q for Patient.
Variables
AIS Score (from 0-5)
6 months after surgery
24 months after surgery
Shape
4.6
5
Volume
5
5
Symmetry
5
4.6
Scars
3
4
NAC
3.2
4
Table 2: AIS for doctor.
Discussion
NAC is an indispensable structure of the breast and breast aesthetic. Cases of complete avulsion of the Nipple-Areolar Complex (NAC) due to trauma are rare. However, when it happens, the fragile blood supply has made the clinical managements challenge, especially for one-stage NAC reconstruction. After the first description of nipple reconstruction using a local flap and tissue graft since 1940 [3,4], various surgical methods have been developed for NAC reconstruction, mainly including local flap and flap with autologous/ alloplastic grafts [5]. Most of these methods have been used in the final stage of breast reconstruction following mastectomy for breast cancer patients. And there are very few reports of using the avulsed one for NAC reconstruction.
The choice of NAC reconstructive procedures is often dictated by the patient’s characteristics and needs as well as by the surgeon’s preference. In our case study, the patient refused the use of flap from elsewhere in the body fearing further surgical scars. During preoperative conversion, we have told the patient that the connected skin was only less than 1/4 of all NAC , and the damaged NAC was completely detached from underlying breast gland tissue, emphasized the loss of vascular supply could increase the risk of ischemia and necrosis of NAC. So, vascular anastomosis might be an attractive option. However, this type of surgery is more complex, and requires longer operation times and the surgeon with training and experience of anastomosis of small vessels. Besides, the avulsion injury often makes vessels and nerves not suitable for anastomosis like this case. All these factors contribute to the final decision of an in situ NAC transplantation like/as free-skin graft, considering.
The rate of complications varies on the reconstruction surgery type. It is well known that free-skin graft has a higher complication rate to that of the local flap [5]. These complications include malposition, loss of nipple projection, loss of sensation and nipple necrosis. Partial or complete necrosis is a common complication. To avoid necrosis, we trimmed the subcutaneous adipose tissue and ducts of NAC to improve the survival of NAC. It is important to note that it is not applicable when graft is severely ischemic, necrotic, locally-infected, or severely damaged.
Loss of nipple projection and breast symmetry is another concerned question to patients and surgeons. It usually occurs within the first 3-6 months after reconstruction [6]. In our case, the projection of the contralateral nipple was not obvious and breast symmetry was well preserved after 24 months post operation, indicating the well aesthetic outcome of our surgery technique.
Altogether, our one-step in situ NAC reconstruction was simple, safe, and time-saving. Our case study provides a feasible method for emergency NAC avulsion. However, proper patient selection and sufficient pro-operative discussion is necessary.
Declaration
Acknowledgements: We thank the patient for the permission of case publication with written informed consent.
Compliance with Ethical Standards: The authors declare that they have no conflicts of interest to disclose. This article does not contain any studies with human participants or animals performed by any of the authors. The patient who involved in this case report has informed consent for the use of her body pictures and agreed with us to publish this article. This study was supported by Science and Technology Supporting Plan of Science & technology Department of Sichuan Province, China (No: 2015SZ0146).
References
- Wellisch DK, Schain WS, Noone RB, Little JW. The psychological contribution of nipple addition in breast reconstruction. Plast Reconstr Surg. 1987; 80: 699-704.
- Shen H, Xu JH, Yao JM, Lv Y, Zheng LJ, Zeng B. Reconstruction after complete avulsion of the nipple caused by a human bite using an amputated tissue graft in situ. J Plast Surg Hand Surg. 2013; 47: 548-549.
- Berson MI. Construction of pseudoareola. Surgery. 1946; 20: 808.
- Adams WM. Labial transplant for correction of loss of the nipple. Plast Reconstr Surg. 1949; 4: 295.
- Sisti A, Grimaldi L, Tassinari J, Cuomo R, Nisi, G. Nipple-areola complex reconstruction techniques: A literature review. EJSO. 2016; 42: 441-465.
- Haslik W, Nedomansky J, Hacker S, Nickl S, Schroegendorfer KF. Objective and subjective evaluation of donor-site morbidity after nipple sharing for nipple areola reconstruction. J Plast Reconstr Aes. 2015; 68: 168-174.