
Special Article – Urinary Tract Infections
Austin J Clin Med. 2015;2(1): 1021.
Emphysematous Pyelonephritis: When Minimally Invasive Approaches are not Enough
Cornejo-Dávila V¹*, Cantellano-Orozco M¹, Martínez-Arroyo C¹, Morales-Montor JG¹ and Pacheco-Gahbler C¹
¹Division of Urology, Hospital General “Dr. Manuel Gea González”, Mexico
*Corresponding author: Cornejo-Dávila V, Division of Urology, Hospital General “Dr. Manuel Gea González”, Calzada de Tlalpan 4800 Col, Sección XVI, Tlalpan, Zip code: 14080, Mexico
Received: January 16, 2015; Accepted: March 04, 2015; Published: April 15, 2015
Abstract
The author presents a case of a diabetic patient that developed a severe left emphysematous pyelonephritis manifested by septic shock that was managed initially with minimally invasive techniques with percutaneous drainage and wide-spectrum antibiotics. Besides her clinical improvement the gas wasn’t resolved entirely even after a second percutaneous drainage and eventually ended in a simple nephrectomy due to persistent fever. What would seem like a pretty common management for this clinical entity, nowadays it represents the exception rather than the rule. This case exemplifies how even though the minimally invasive approaches are used to spare the kidney, a nephrectomy still plays a role in the management of patients with this complicated infection.
Keywords: Emphysematous pyelonephritis; Nephrectomy; Minimally invasive; Mexico
Abbreviations
UTI: Urinary Tract Infection; CT: Computed Tomography; EPN: Emphysematous Pyelonephritis
Introduction
Urinary tract infections comprehend a wide spectrum of presentations that can vary from mild clinical pictures such as noncomplicated cystitis to life-threatening conditions with extensive tissue destruction such as emphysematous pyelonephritis. An emphysematous pyelonephritis represent a gas-producing infection developed by gram negative bacteria that metabolize the excess of carbohydrates (mainly glucose) with formation of carbon dioxide, that starts to accumulate in the urinary tract and collecting systems; this gas later extends through the renal parenchyma and can reach the perinephric and even pararenal space. These patients usually develop sepsis and/or septic shock, and often require intensive care support associated with high mortality [1]. They require wide spectrum antibiotics [2] and a minimally invasive procedure to drain the gas and/or purulent material on most cases. In the past a nephrectomy was performed frequently in early stages of the disease, which lead to a greater overall and trans-surgical mortality due to sepsis and bleeding by trying to dissect a heavily inflamed kidney and surrounding structures [3]. To avoid an increased morbidity, the use of minimally invasive treatments such as percutaneous drainage and ureteral stents replaced the other approaches [4,5] however, there are infections that won’t resolve with these treatments and patients will eventually need a nephrectomy to achieve a cure. We present a case of emphysematous pyelonephritis that exemplifies that situation.
Case Presentation
A 48-year-old woman arrived to the emergency department with a one-week history of fever, malaise, nausea and left flank pain. She had a history of diabetes and hypertension with poor control and had been hospitalized six months previously for a urinary tract infection that was treated empirically with quinolones at a community hospital. She had no follow-up and no cultures taken. On admission she was diagnosed with septic shock, diabetic ketoacidosis and renal failure; after being resuscitated with intravenous fluids and started on inotropes and insulin infusion protocol, wide-spectrum antibiotics (ertapenem and amikacin adjusted to renal function) were also initiated. Once being stable an abdominal computed tomography was performed (Figure 1) establishing a diagnosis of left emphysematous pyelonephritis Huang 3b with extension of the gas throughout Gerota’s fascia on the lower pole. Forty-eight hours after admittance an image-guided percutaneous drainage with a 10 French catheter was performed (Figure 2A and 2B) obtaining gas and 100 mL of purulent material; the catheter was left on continuous suction. An extended-spectrum betalactamases-producing E.coli strain with resistance to quinolones and trimethoprim was isolated from the obtained material as well as in a blood culture. She had a slow improvement with an average of 50 mL of purulent material drained per day; one week after admission the sepsis and renal failure had remitted but the gas persisted on a follow-up CT (Figure 2C and 2D). Given those findings a second image-guided percutaneous drainage was done obtaining more gas and scarce purulent material. On the thirteenth inpatient day, her evolution was stationary, persisting with spikes of fever and gas on lower renal pole with distortion of renal parenchyma’s anatomy was observed on another CT despite the catheter (Figure 3). The decision of performing an open simple nephrectomy was made, with findings of an intense perinephric inflammatory reaction and purulent material within the kidney; chronic pyelonephritis with abscess and multifocal necrosis was reported on the pathological report. After the procedure she remained non-febrile and was discharged on postoperatory day 3. On follow-up at the urology clinic she was doing well, had a negative urine culture, normal glycemia and normal creatinine levels.
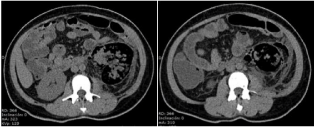
Figure 1: CT scan at admission. Air extending outside of the Gerota,
corresponding to Huang 3b.
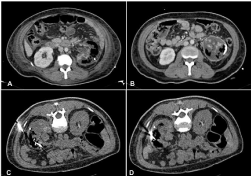
Figure 1: Persistence of gas after first percutaneous drainage (A and B) and
second percutaneous drainage(C and D).
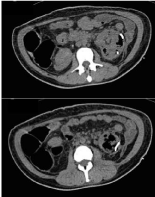
Figure 3: After second drainage, the catheter is in place but there’s still
unresolved gas on lower pole and the renal parenchyma’s anatomy remains
distorted.
Discussion
There are several reports of emphysematous pyelonephritis cases in the international literature [6] varying from mild cases confined to collecting systems to severe ones that practically replace the normal anatomy of one or both kidneys; to adequately classify each case in the clinical setting, the Huang classification is preferred [7].
Class 1: gas in the collecting system only
Class 2: gas in the renal parenchyma without extension to the extrarenal space
Class 3A: extension of gas or abscess to the perinephric space
Class 3B: extension of gas or abscess to the pararenal space
Class 4: bilateral EPN or solitary kidney with EPN
A high index of suspicion is needed to establish an early diagnosis; usually these patients are admitted with septic shock without an obvious source and acute complications related to the diabetes, such as diabetic ketoacidosis or hyperosmolar non-ketotic diabetic coma, and not uncommonly it can even manifest as the presenting symptom of the disease on a “previously healthy” patient [8]. This situation can often mislead the diagnosis or have the physician underestimate the underlying severity within the kidney and urinary tract, which is why imaging studies are essential to determine if there’s a complication and which one it is. For the particular case of emphysematous pyelonephritis, Huang’s classification on CT is useful to determine extent, treatment modality and it also has prognostic value [9].
Wide-spectrum antibiotics have to be delivered as soon as possible since the delay in the onset of appropriate therapy can result in early deterioration and death. Even though there are reports of cases treated with antibiotics alone [10-12] the idea that the patient will probably need a complementary treatment has to be present at all times when approaching these patients.
Once the patient has been diagnosed with imaging studies and the extent of the damage has been determined, the minimally invasive approaches to drain the gas and/or purulent material have demonstrated to improve the outcomes [13,14]. In our previous study involving management of complicated UTIs [15] a total of 14 patients with emphysematous pyelonephritis were included on a time span of barely a year and a half, 68% of these patients were at least classified as Huang 3 by CT. 64% of them were treated with a minimally invasive approach, which resolved the gas on all but two patients that ended having a nephrectomy; also we treat these patients with carbapenems empirically and downscale antibiotic only if a susceptible strain is isolated, due to the high prevalence of antibiotic resistance and extended spectrum betalactamases prevalence in our community. The mortality in our group of emphysematous pyelonephritis was 28%. In other studies mortality has been reported as low as 8% (Chen) [16], 18.8% (Huang), 33% (Tsu) [1], 45% (Dutta) [17] and in some patient subgroups can reach 100% (Aswathaman). In the study by Huang et al patients that were treated initially with percutaneous drainage but failed to respond appropriately and had to undergo nephrectomy had a survival of 90%. Somani et al [13] noted that mortality was higher when treated with medical management alone (50%), that it decreased to half (25%) with emergency nephrectomy but the lowest mortality was achieved with percutaneous drainage (13.5%); in cases when this last approach failed and nephrectomy was made, mortality still was lower than when performed on an emergency setting (6.6%). In the present case, the patient survived without compromise of her overall renal function by performing the nephrectomy in a non-emergency situation.
In patients with emphysematous pyelonephritis the kidney should be spared as much as possible, therefore the current standard of treatment include wide spectrum antibiotics combined with minimally invasive approaches which include percutaneous drainage and ureteral stents; however when nephrectomy is performed accordingly, good results can also be achieved.
Conclusion
An appropriate antibiotic treatment combined with the use of minimally invasive approaches will resolve most cases of emphysematous pyelonephritis, however, nephrectomy still has to be performed in some patients in order to control the infection and improve patients’ survival, preferentially in a non-emergency setting.
References
- Tsu JH, Chan CK, Chu RW, Law IC, Kong CK, Liu PL, et al. Emphysematous pyelonephritis: an 8-year retrospective review across four hospitals. Asian J Surg. 2013; 36: 121-125.
- Pallett A, Hand K. Complicated urinary tract infections: practical solutions for the treatment of multiresistant Gram-negative bacteria. J Antimicrob Chemoter. 2010; 65: 25-33.
- Shokeir AA, El-Azab M, Mohsen, El-Diasty T. Emphysematous pyelonephritis: a 15-year experience with 20 cases. Urology. 1997; 49 : 343 -346.
- Aswathaman K, Gopalakrishnan G, Gnanaraj L, Chacko NK, Kekre NS, Devasia A. Emphysematous pyelonephritis: outcome of conservative management. Urology. 2008; 71: 1007-1009.
- Lin WC, Chen YF, Lin CH, Ho YJ, Tzeng YH, Chiang HJ, et al. Reappraisal of the management and outcome of emphysematous pyelonephritis. Kaohsiung J Med Sci. 2009; 25: 16-24.
- Mohsin N, Budruddin N, Lala S, Al-Taie S. Emphysematous pyelonephritis: a case report series of four patients with review of literature. Ren Fail. 2009; 31: 597-601.
- Huang JJ, Tseng CC. Emphysematous pyelonephritis clinicoradiological classification, management, prognosis and pathogenesis. Arch Intern Med. 2000; 160: 797-805.
- Surur J. Acute bilateral emphysematous pyelonephritis. BMJ Case Reports. 2011.
- Kondo T, Okuda H, Suzuki M, Okumura T, Toma H. A case of emphysematous pyelonephritis improved with conservative therapy – indication for conservative therapy. Hinyokika Kiyo. 2000; 46: 335- 338.
- Punnose J, Yahya TM, Premchandran JS, Ahmed HF. Emphysematous pyelonephritis responding to medical therapy. Int J Clin Pract. 1997; 51: 468 -470.
- Jain SK, Agarwal N, Chaturvedi SK. Emphysematous pyelonephritis: a rare presentation. J Postgrad Med. 2000; 46: 31-32.
- Flores G, Nellen H, Magaña F, Calleja J. Acute bilateral emphysematous pyelonephritis successfully managed by medical therapy alone: A case report and review of the literatura. BMC Nephrology. 2002; 3: 4.
- Somani BK, Nabi G, Thorpe P, Hussey J, Cook J, N’Dow J. Is percutaneous drainage the new gold standard in the management of emphysematous pyelonephritis? Evidence from a systematic review. J Urol. 2008; 179: 1844-1849.
- Ahmed R. E-Nahasa, Ahmed A. Shokeira, Amogu Kalu Eziyia, Tamer S. Barakata, Kehinde Habeeb Tijania, Tarek El-Diastyb, et al. Kidney preservation protocol for management of emphysematous pyelonephritis: Treatment modalities and follow-up. Arab J Urol. 2011; 9: 185-189.
- Cornejo-Dávila V, Palmeros-Rodríguez MA, Uberetagoyena-Tello de Meneses I, Mayorga-Gómez E, Garza-Sainz G, Osornio-Sánchez V et al. Management of complicated urinary tract infections in a referral center in Mexico. Int Urol Nephrol. 2015; 47: 229-233.
- Chen MT, Huang CN, Chou YH, Huang CH, Chiang CP, Liu GC. Percutaneous drainage in the treatment of emphysematous pyelonephritis: 10-year experience. J Urol. 1997; 157: 1569-1573.
- Dutta P, Bhansali A, Singh SK, Gupta KL, Bhat MH, Masoodi SR. Presentation and outcome of emphysematous renal tract disease in patients with diabetes mellitus. Urol Int. 2007; 78: 13-22.