
Research Article
Austin J Clin Med. 2018; 5(1): 1033.
Dose Determination for Hydrophilic and Lipophilic Drugs for Chemotherapy and Immunotherapy
Barry J Allen*
Faculty of Medicine, University Western Sydney, Australia
*Corresponding author: Barry J Allen, Faculty of Medicine, University Western Sydney, Australia
Received: March 22, 2018; Accepted: April 19, 2018; Published: April 26, 2018
Abstract
Patient dose normalisation for optimal doses found in phase 1 clinical trials remains underutilised in Clinical Oncology. The Body Surface Area (BSA) is dominant despite its lack of rigor, apparent inadequacies and the frequent need for dose adjustment. The BSA method has been critiqued over the decades. In this paper, the use of in vivo body composition methods to determine fat mass and fat free mass are proposed, which would form the new basis for normalisation of lipophilic and hydrophilic drugs. Issues relating to volume of distribution and drug clearance remain largely unknown, but at least the starting patient dose is expected to be better placed. Clinical trials are needed to justify both this approach and the BSA method.
Keywords: (AUC): Area under the Curve; (TBW): Total Body Water; (BSA): Body Surface Area; (BM): Body Mass; (FFM): Fat Free Mass
Introduction
The distribution of drugs from the injection site by the vascular system to the target tissue is governed by blood flow, solubility, binding to macromolecules and ability to cross special barriers. Drugs can be hydrophilic or lipophilic or both. Lipophilic drugs can pass through cell membranes due to their solubility in membrane bilayers but not so hydrophilic drugs, which require aqueous channels or pores. Large molecules require endocytosis, which entails engulfment of the molecule and transport into the cell by pinching off the drug filled vesicle.
Bioavailability is the fraction of the injected dose that reaches the systemic circulation with unchanged properties. The extent of drug absorption can be measured by the Area under the Curve (AUC) for plasma concentrations over time. For hydrophilic drugs, the concentration depends on the volume of distribution of the Total Body Water (TBW).
TBW and other body compartments have been studied by in vivo body composition in many medical conditions in the 1980s. However, current Oncology dose protocols have not moved on from either Body Surface Area (BSA) or Body Mass (BM) in the normalisation of dose for each patient. Anticancer drugs have a narrow therapeutic window and significant patient variability in therapeutic and toxic effects. As such, it is important that dose optimisation is achieved.
This paper reviews the evidence against using BSA and proposes an alternative dose normalisation approach that uses the Fat Free Mass (FFM) for hydrophilic drugs.
Body Surface Area
BSA plays a key role in several medical fields, including cancer chemotherapy, transplantology, burn treatment and toxicology. BSA is often a major factor in the determination of the course of treatment and drug dosage. Mathematical formulae to calculate BSA from measurements of height, weight and other parameters date from the late 19th century [1]. Drug doses, fluid therapy, caloric requirements and physiological parameters such as cardiac output, glomerular filtration rate and a variety of respiratory function parameters are all frequently expressed in terms of a BSA, which is often used in preference to BM. The calculated surface area of a human body may be a better indicator of metabolic mass than body weight because it is less affected by abnormal adipose mass [2]. The simplest formula is BSA(m2)=√(weight(kg) x height (cm))/60. Just how this relates to metabolic mass is unclear. However, the original rationale for using body surface area as an estimate for metabolic rate has never been tested and the algorithms used to approximate body surface area have little evidence to support their use in this role. Recent developments in technology using indirect calorimetry allow easy measurement of metabolic rate in the clinical setting. Such measurements should be used for standardization when weight alone is considered inadequate.
Discrepancies between most of the known BSA formulae can reach 0.5m2 for the standard adult physique [3]. Although many previous studies have demonstrated that certain BSA formulae provide an almost exact fit with the patients examined, all of these studies have been performed on a limited and isolated group of people. 25 BSA formulae were analysed to reveal that the choice of a particular formula is a difficult task. Differences among calculations made by the formulae are so great that, in certain cases, they may considerably affect patients' mortality, especially for people with an abnormal physique or for children.
This problem is also apparent in the treatment of dogs. The dose of most cancer chemotherapeutic drugs administered to dogs is calculated on the basis of estimated BSA, yet some chemotherapy trials have revealed that this dosing method increases toxicosis in small dogs [4]. The current formula used to estimate BSA in dogs may be inaccurate or the assumption that BSA correlates with chemotherapeutic drug exposure may be unfounded. Results suggest that the relationship between BSA and the physiologic and pharmacologic factors that influence drug exposure may not be closely correlated. Further studies are warranted to determine dosing methods that normalize chemotherapeutic drug toxicity in dogs.
The effects of BSA on the pharmacokinetics of anti-cancer drugs have been studied retrospectively to find that in most cases, use of BSA does not reduce the inter-individual variation in the pharmacokinetics of adults [5]. As such, the rationale for further use of this tool in dosing adults is lacking. Alternative dosing strategies have been proposed in order to replace the BSA-based dosing. Flat-fixed dosing regimens have been suggested that do not typically lead to greater pharmacokinetic variability, the implementation of genotyping and phenotyping strategies, and therapeutic drug monitoring, may probably be of more clinical value. In the end, the non-scientifically based BSA-based dosing strategy should be replaced by alternative strategies. Despite the lack of basic fundamentals, BSA-based dosing still seems "untouchable" in clinical oncology.
Consequently, the use of BSA in determining the dosage of medications with a narrow therapeutic index, such as chemotherapy, does not enhance to the concept of personalised medicine.
Drug Clearance
Drug clearance between individuals can vary by 4-10 folds due to differing drug elimination processes related to genetic and environmental factors [6].
Overdosing is easily recognised but it is possible that unrecognised under dosing is more common and may occur in 30% or more of patients receiving standard regimens. Those patients who are under dosed are at risk of a significantly reduced anticancer effect, there being an almost 20% relative reduction in survival for women receiving adjuvant chemotherapy for breast cancer and up to 10% for cisplatin-based chemotherapy for advanced testicular cancer.
The Area under the Curve (AUC), shown below, gives the integrated dose for concentration (y axis) vs time (x axis). The shape of this curve f(x) depends on many factors but it is the concentration in the target tissue that gives the therapeutic effect. The integrated dose over time provides the average effect and cannot be less than the dilution of the hydrophilic drug in the Total Body Water (TBW) (Figure1).
4.1. A specific AUC example is the Calvert (1989) formula for carboplatin dosing where:
Dose (mg) = (target AUC) x (GFR + 25).
Where AUC = target area under the concentration versus time curve in mg/mL•min and Glomerular Filtration Rate (GFR) is measured by 51Cr-EDTA clearance. Pre-treatment platelet count and performance status are important prognostic factors for severity of myelosuppression in previously treated patients. Dose adjustments for single agent or combination therapy are modified from controlled trials in previously treated and untreated patients with ovarian carcinoma. Recommendations are based on the lowest post-treatment platelet or neutrophil value. AUC-based carboplatin dosing was found to be more accurate than dosing based on BSA.
Strategies using clinical parameters, genotype and phenotype markers, and therapeutic drug monitoring, all have potential and each has a role for specific drugs. However, no one method is a practical dose calculation strategy for many drugs. A potential and pragmatic system for initial dose calculation uses dose clusters and structured subsequent dose revision based on treatment-related toxicities and therapeutic drug monitoring. However, these models need to be tested in clinical trials [7].
Current practice is to put an upper limit on BSA for obese patients. Another approach is to rejig the dose following adverse events in early treatments. While effective, these procedures admit to profound deficiencies in dose personalisation.
Obesity
Both direct and indirect methodologies have been utilized to assess body composition [8]. Commonly used direct measures include underwater weighing, skin fold measurement, and bioelectrical impedance analysis and dual-energy x-ray absorptiometry. A number of indirect measures have been developed such as height, bodyweight and sex, and include Body Mass Index (BMI), Body Surface Area (BSA), Ideal Bodyweight (IBW), percent IBW, adjusted bodyweight, Lean Bodyweight (LBW) and Predicted Normal Weight (PNWT). The V(d) of a drug is dependent upon its physiochemical properties, the degree of plasma protein binding and tissue blood flow. Drug Clearance (CL) is the primary determinant to consider when designing a maintenance dose regimen and is largely controlled by hepatic and renal physiology. In the obese, increases in cytochrome P450 2E1 activity and phase II conjugation activity have been observed. However, the effects of obesity on renal tubular secretion, tubular reabsorption, and glomerular filtration have not been fully elucidated. The elimination half-life (t1/2) of a drug depends on both the V(d) and CL. Since the V(d) and CL are biologically independent entities, changes in the t1/2 of a drug in obese individuals can reflect changes in the V(d), the CL, or both. Pharmacokinetic data in obese patients do not exist for the majority of drugs. In situations where such information is available, clinicians should design treatment regimens that account for any significant differences in the CL and V(d) in the obese. As with the V(d), a single, well validated size metric to characterize drug CL in the obese does not currently exist.
Dosages based on pharmacokinetic data obtained in normal-weight individuals could induce errors in the drug prescription for obese patients [9]. Most of the pharmacokinetic information concerning obesity deals with distribution. Drugs with moderate to weak lipophilicity are homogeneous. In obese individuals, the total volume of distribution V(d) is moderately increased or similar for most drugs, but the V(d) per kilogram of bodyweight is significantly smaller. These drugs distribute to a limited extent in excess bodyweight.
For highly lipophilic drugs (cyclosporin, propranolol), V(d) and Vd/kg are decreased suggesting that factors other than lipid solubility intervene in tissue distribution. For drugs with distribution restricted to lean tissues, the loading dose should be based on the ideal bodyweight of patients. For drugs markedly distributed into fat tissue the loading dose is based on total bodyweight. Adjustment of the maintenance dose depends on possible changes in clearance. These recommendations do not include BSA, but emphasise ideal (for hydrophilic) and actual (for lipophilic) body weight.
The BF compartment includes all membranes and adipose tissue and determines the ultimate dilution of lipophilic drugs, the actual concentrations being determined as above. However, BF could well be a superior normalisation parameter to those listed above.
5.1. Hydrophilic and lipophilic drugs and total body water
Clinical response to chemotherapy often ranges from none to complete remission (often temporary). It is therefore difficult to determine the optimum dose, instead the median value from a range of body shapes in a clinical trial would be used. Most drugs are hydrophilic and dissolve in water to form a solution, the efficacy of which is governed by its concentration in the critical tissue. Too low a concentration and the drug is ineffective, too high and it’s toxic.
The use of dose determination based on BM or BSA has long been shown to be inadequate in body composition studies [10,11], but is still used by Oncologists. Fat is not a relevant factor for a water soluble drug, so the total body water (TBW) should be used as the preferred starting point for dose normalisation of hydrophilic drugs as this gives the overall drug concentration, which is the primary dose parameter. Cytotoxic drug elimination should be measured over time as the peak concentration could be more important that the integrated dose, but this is not practical in a patient management protocol.
Total Body Water
TBW can be measured directly using, for example, the protocol developed by [12,13]. This is a laboratory protocol that requires heavy water for dilution, which is not readily available. However, a much more practical method is to determine the fat free mass (FFM). The FFM excludes the fat compartment but includes total body protein (TBP), bone (TBB) and water (TBW). Bone mass is fixed, protein varies slowly but water can change daily by hydration or elimination.
FFM = BM – BF = TBP + TBB + TBW ~ c + TBW
6.1. The rate of change in these parameters is:
d(FFM)/dt ~ d(TBW)/dt Consequently, the FFM gives the best indirect estimate of TBW, which relates to the efficacy of a drug in the target tissue.
A simple example of the use of FFM in determining the personalised dose is given on the basis that the recommended dose is 1 unit of drug/kg BM. The “standard man” weighs 70 kg, which may be the median bodyweight in a phase 1 clinical trial. The dose given would then be 70 units. However, for 20% body fat, the FFM would be 70-14 = 56kg. For a thin person with the same bwt and 10% fat, the FFM = 70-7 = 63kg. For a fat person with 30% fat, it would be 70-21 = 49kg (Table 1).
FM%
10
20
30
FFM kg
63
56
49
Dose (relative)
0.89
1
1.14
Table 1: Normalised hydrophilic drug doses.
FM%
10
20
30
FM kg
7
14
21
Dose (relative)
0.5
1
1.5
Table 2: Normalised lipophilic drug doses.
6.2. The hydrophilic drug doses for the 70kg man with different fat masses are given below:
Assuming that the average FM is 20% for the clinical trial dose determination, then the thin man will be under dosed by 11% and the fat man over dosed by 14% if FFM is not used to normalise dose (Table 1). While most patients will lie within this band, obese or cachectic patients will be severely under or over dosed. It is therefore essential that FM be measured first to determine the optimal dose (Table 2).
6.3. The lipophilic drug doses for the 70kg man with different fat masses are given below:
Assuming that the lipophilic drug is completely soluble in the fat mass, then there are major differences in patients with different fat masses as shown in Table 2, when normalised to the 20% BF.
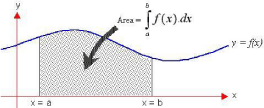
Figure 1:
Drugs that exhibit both hydrophilic and lipophilic activity have relative doses somewhere between those shown in Table 1 and Table 2.
Measurements
Body composition measurement with Dual Energy X-Ray Absorptiometry (DEXA) is used increasingly for a variety of clinical and research applications. DEXA total body scans give accurate and precise measurements of body composition, including Bone Mineral Content (BMC), Bone Mineral Density (BMD), lean tissue mass, fat tissue mass and fractional contribution of fat [14]. The scans are fast, simple, non-invasive with insignificant x-ray exposure. However, the role of DEXA in clinical evaluations and research studies has errors that are still of concern.
DEXA may not be readily available in the Oncology setting. However, BF can be readily measured with adequate accuracy by measuring the thickness of subcutaneous fat in multiple places on the body with a vernier caliper [15,16]. This includes the abdominal area, the subscapular region, arms, buttocks and thighs. These measurements are then used to estimate total body fat. The equations predict body fat within 3-5% of the value obtained from underwater weighing but only if the person is of similar age, gender, state of training, fatness and culture to the population from which the equations were originally derived [17-19]. With this qualification, the sum of skin folds is an entirely practical, very low cost protocol for patient management and dose normalisation.
Conclusion
The point of this analysis is that the current BSA or BM protocols only apply to near standard patients. Typically, dosage is changed by the Oncologist on the basis of patient needs and clinical response. However, an Oncologist using the more appropriate FFM method could find that such adjustments would be reduced, although the management might be outside the current guidelines. Although accepted for a century, the body surface area for patient dose determination has been shown to be inadequate. Phase 1 clinical trials should generate FFM data, which can then be used for patient dose normalization. This data can be readily obtained in any clinical trial, which then allows for obese or cachectic patients. Such trials could also incorporate direct measurement of TBW as well as FFM.
Personalised patient therapy clearly requires improved normalisation from clinical trial data in order to optimise the therapeutic response with minimal adverse events. The FFM method is expected to provide a much more suitable starting point for patient dose determination than BSA or BM. As such, the FFM should be specified in all phase 1 clinical trials. Only then can the FFM protocol be tested against the “standard” BSA method.
References
- Gibson S, Numa A. The importance of metabolic rate and the folly of body surface area calculations. Anaesthesia. 2003; 58: 50-55.
- Du Bois D, Du Bois EF. A formula to estimate the approximate surface area if height and weight be known. Arch Intern Med. 1916. 1989; 5: 303-311.
- Redlarski G, Palkowski A, Krawczuk M. Body surface area formulae: an alarming ambiguity. Sci Rep. 2016.
- Price GS, Frazier DL. Use of body surface area (BSA)-based dosages to calculate chemotherapeutic drug dose in dogs: I. Potential problems with current BSA formulae. J Vet Intern Med. 1998; 12: 267-271.
- Mathijssen RH, de Jong FA, Loos WJ, van der Bol JM, Verweij J, Sparreboom A. Flat-fixed dosing versus body surface area based dosing of anticancer drugs in adults: Does it make a difference? Oncologist. 2007; 12: 913-923.
- Gurney H. How to calculate the dose of chemotherapy. Br. J. Cancer. 2002; 86: 1297-1302.
- Gao B, Klumpen HJ, Gurney H. Dose calculation of anticancer drugs. Expert Opin. Drug Metab. Toxicol. 2008; 4: 1307–1319.
- Hanley MJ, Abernethy DR, Greenblatt DJ. Effect of obesity on the pharmacokinetics of drugs in humans. Clin Pharmacokinet. 2010; 49: 71-87.
- Cheymol G. Clinical pharmacokinetics of drugs in obesity. An update. Clin Pharmacokinet. 1993; 25: 103-114.
- Aslani A, Smith RC, Allen BJ, Pavlakis N, Levi J. The predictive value of body protein for chemotherapy-induced toxicity. Cancer. 2000; 88: 796-803.
- Allen BJ, N. Blagojevic N. In vivo body composition studies in malnourished patients. ANZ Nucl. Med. 1987: 20-22.
- Blagojevic N, Allen BJ. In vivo determination of total body water and lean body mass in subjects by deuterium dilution. ANZ Nucl. Med. 1989: 14-16.
- Blagojevic N, Allen BJ, Gaskin KJ, Baur LA. Determination of total body water by fourier transform infrared analysis. Aust. Phys. Eng. Sci. Med. 1990; 13: 110-116.
- Kiebzak GM, Leamy LJ, Pierson LM, Nord RH, Zhang ZY. Measurement precision of body composition variables using the lunar DPX-L densitometer. J Clin Densitom. 2000; 3: 35-41.
- Rutherford WJ, Diemer GA, Scott ED. Comparison of Bioelectrical Impedance and Skinfolds with Hydrodensitometry in the Assessment of Body Composition in Healthy Young Adults. Journal of Research. 2011: 6; 56-60.
- Skinfolds table.
- Allen BJ, Pollock CA, Russell J, Oliver C, Smith RC. Role of body protein as a prognostic indicator in wasting disease. Asia Pacific J Clin Nutr, Supplement. 1995; 4: 31-33.
- Calvert AH, Newell DR, Gumbrell LA, et al. Carboplatin dosage: Prospective evaluation of a simple formula based don renal function. J Clin Oncol. 1989; 7: 1748-1756.
- Morgan DJ, Bray KM. Lean body mass as a predictor of drug dosage. Implications for drug therapy. Clin Pharmacokinet. 1994; 26: 292-307.