Case Report
Austin J Clin Neurol 2014;1(3): 1015.
A Case of Recurrent Sleep Paralysis: Beyond Narcolepsy
Vijaya Yelisetty and Kanika Bagai*
Department of Neurology, Vanderbilt University School of Medicine, Tennessee, USA
*Corresponding author: Kanika Bagai, Department of Neurology, Vanderbilt Sleep Disorders Center, Vanderbilt University School of Medicine, A- 0118 Medical Center North, Nashville, TN 37232, Tennessee, USA
Received: June 20, 2014; Accepted: August 20, 2014; Published: August 22, 2014
Abstract
Isolated episodes of sleep paralysis can occur in healthy people at least once in their lifetime; however recurrent isolated sleep paralysis (RISP) events are less common and often worrisome. Recurrent episodes of sleep paralysis are often seen in patients with narcolepsy. Here, we present a unique case of a middle-aged woman who presents with symptoms of RISP in her fifth decade that was not associated with narcolepsy.
Introduction
We describe a case of a 52-year-old woman who presents with initial symptoms of recurrent isolated sleep paralysis.
Case Presentation
A 52 year-old woman presented to the sleep clinic with complaints of sleep difficulties and symptoms of “unable to move her body while in bed”. These episodes of isolated sleep paralysis (ISP) occurred randomly either at sleep onset, or upon awakening in the morning. These events lasted for a few minutes, were often frightening and resolved spontaneously. These were not associated with vivid dreams and occurred randomly with a frequency of twice per month over the last year. She had experienced similar symptoms of sleep paralysis on rare occasions in the remote past, but reported worsening in the frequency recently. Furthermore, she reported similar episodes of inability to move her body after awakening from occasional daytime naps on weekends.
Upon further questioning on the details of sleep history, she noted symptoms of multiple nighttime awakenings, loud snoring and daytime fatigue. She reported an irregular sleep schedule with varying bedtimes on weekdays and weekends and was getting only 4-5 hours of sleep. She was fatigued all day and took naps during the day occasionally on weekends. Her Epworth sleepiness scale (ESS) was 6/24. She denied symptoms of cataplexy, hypnic hallucinations or automatic behaviors. She exhibited mild restless leg symptoms but they did not disrupt her sleep.
Past medical history was significant for diabetes, hypertension, hyperlipidemia, generalized anxiety disorder, and asthma. There was no family history of narcolepsy or similar symptoms of sleep paralysis.
Social history was negative for smoking, alcohol use or any illicit drug use.
Medications included albuterol, fluticasone-salmeterol inhaler, olmesartan, montelukast, metformin, sitagliptin, glyburide, omeprazole and cetirizine.
On physical exam, vital signs were stable. She had a crowded oropharynx (Friedman palate position 3); otherwise remainder of the physical exam was within normal limits.
Laboratory data including complete blood count, complete metabolic panel, TSH, Vit B12, Vit D levels were within normal limits as below:
Complete blood count: WBC: 5.7k/ul; Hemoglobin 12.6 gm/dl, hematocrit 37%, platelets count 258k/ul.
Chemistries: Sodium 141 mmol/l, potassium 4.1 mmol/l, chloride 107 mmol/l, bicarbonate 25 mmol/l, glucose 213 mg/dl, BUN 19 mg/ dl, creatinine 0.9 mg/dl, Calcium 9.3 mg/dl, total protein 7.4 gm/dl, albumin 4.1 gm/dl, total bilirubin 0.6 mg/dl, alkaline phosphatase 68 intU/l, ALT 23 intU/l, AST 26 intU/l.
Endocrine data: TSH: 1.03 mcU/ml, Free T4: 0.87 ng/dl, 25-hydroxy Vit D: 27 ng/ml, Vitamin B 12: 249 pg/ml.
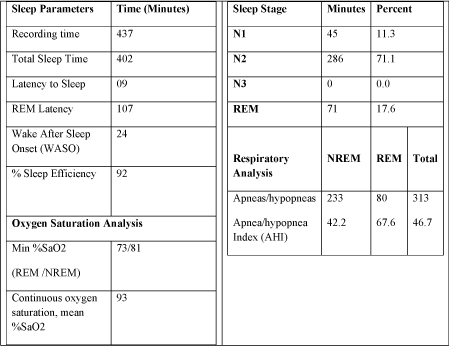
We counseled patient on sleep hygiene, including not varying bedtime on weekends and weekdays and getting at least 7-8 hours of sleep at night. Her symptoms of recurrent isolated sleep paralysis (RISP) persisted despite improvement in her sleep hygiene and increasing the total sleep time. We ordered an overnight polysomnogram (PSG) followed by next day multiple sleep latency test (MSLT) to evaluate her symptoms. The PSG results are summarized in Table 1.
Table 1: Polysomnogram Results.
Results of the PSG indicated obstructive sleep apnea (OSA) with an apnea-hypopnea index (AHI) of 46 events/ hour. Since PSG demonstrated OSA, the MSLT was cancelled. Following PSG, she underwent continuous positive airway pressure (CPAP) titration study for management of OSA. CPAP setting of 9 cm of water resulted in improvement of her breathing events and a home CPAP machine was prescribed at that setting.
At six months and one-year follow up, she demonstrated adequate adherence with CPAP therapy (AHI improved to 0.8events/ hour). She noted improvement of nocturnal awakenings and daytime fatigue with CPAP usage. Her ESS improved to 3/24. Moreover, she reported improvement of RISP with no further experiences associated with nighttime sleep. On rare occasions when she took daytime naps without CPAP usage, she continued to experience ISP symptoms upon awakening. She reported that she took short naps out of boredom and not necessarily because of sleepiness or fatigue. We recommended that patient use CPAP during daytime naps as well as overnight to improve daytime RISP symptoms.
Discussion
Our patient’s differential diagnosis at first presentation includes inadequate sleep hygiene with insufficient total sleep time, periodic paralysis, sleep-related breathing disorder and narcolepsy without cataplexy. Although narcolepsy was initially considered, daytime sleepiness was not a prominent symptom. We initially ordered a PSG with an MSLT. However, when OSA was established as the cause of her symptoms, MSLT was cancelled.
Periodic paralysis (PP) is a rare genetic disorder related to defect in muscle ion channels and characterized by episodic painless muscle weakness [1]. It is often triggered by rigorous exercise, stress, fasting, and changes in temperature. . It can be associated with low blood potassium levels (hypokalemic PP) and high potassium levels (hyperkalemic PP). Hypokalemia PP is one of most common causes of PP and it can be familial with an autosomal dominant inheritance pattern or acquired as in patients with thyrotoxicosis [1,2]. Although PP was a possible diagnosis for consideration, our patient did not exhibit any daytime intermittent muscle weakness and her symptoms of paralysis often occurred at sleep onset while in bed. Furthermore, as indicated by her metabolic panel, her chemistries were with normal range.
Isolated sleep paralysis is a phenomenon during which a person is unable to move or speak but has clear consciousness and occurs at sleep onset or upon transitions into wakefulness [3,4]. The experience is usually frightening and lasts one to several minutes and disappears either spontaneously or upon external stimulation. These episodes are often associated with visual or auditory hallucinations [5,6].
Sleep paralysis can occur in association with narcolepsy, occur in an isolated form in otherwise healthy individuals, or in a familial form that is genetically transmitted in an X-linked dominant form [4].
Isolated sleep paralysis involves intrusion of REM sleep into wakeful state and is associated with muscle paralysis. Ocular and respiratory movements are intact [6]. Although it is commonly associated with narcolepsy, it can occur in otherwise healthy individuals without symptoms of narcolepsy. ISP can occur at least once in a lifetime in 40-50% of normal subjects [4]. It is thought to be elicited by sleep deprivation and sleep disruption due to many different conditions. It has also been reported in association with anxiety disorders, panic attacks, obstructive sleep apnea or insufficient sleep syndrome, nightmares and post-traumatic stress disorder [5]. In our case, it is likely that sleep disruption (especially disruption of REM sleep) due to underlying OSA predisposed patient to experience ISP events.
The treatment for RISP is usually prevention of sleep deprivation and other underlying precipitants. SSRIs (selective serotonin reuptake inhibitors) may be considered in refractory cases to reduce the frequency of episodes [3,6].
Our patient had poor sleep hygiene and insufficient sleep initially which she improved with our recommendations. She continued to have sleep disruption with multiple nighttime awakenings due to underlying OSA and associated symptoms of RISP. With optimal management of OSA with CPAP therapy, our patient was able to achieve continuous sleep without repeated awakenings and her symptoms of ISP subsequently resolved.
In summary, this case highlights a unique presentation of recurrent isolated sleep paralysis as an initial presenting symptom of obstructive sleep apnea and the efficacy of CPAP in its management. Although previous studies have described cases of narcolepsy with OSA and effect of CPAP therapy, the novelty of our case lies in the fact that our patient experienced RISP in the absence of narcolepsy, and yet her sleep paralysis episodes completely resolved with CPAP therapy. Further studies are indicated to better understand the incidence of ISP in sleep apnea cases.
References
- Fontaine B. Periodic paralysis. See comment in PubMed Commons below Adv Genet. 2008; 63: 3-23.
- Lin SH. Thyrotoxic periodic paralysis. See comment in PubMed Commons below Mayo Clin Proc. 2005; 80: 99-105.
- Vaughn, Bradley. Cardinal Manifestations of Sleep Disorders. In: Kryger MH, Roth T, Dement C, editors. Principles and Practice of Sleep Medicine. 5th ed. Philadelphia: WB Saunders. 2011; 653.
- American Academy of Sleep Medicine. International Classification of Sleep Disorders (ICSD) 3rd ed. Darien, IL. 2014. 254-256.
- Fukuda K, Miyasita A, Inugami M, Ishihara K. High prevalence of isolated sleep paralysis: kanashibari phenomenon in Japan. See comment in PubMed Commons below Sleep. 1987; 10: 279-286.
- McCarty DE, Chesson AL Jr. A case of sleep paralysis with hypnopompic hallucinations. Recurrent isolated sleep paralysis associated with hypnopompic hallucinations, precipitated by behaviorally induced insufficient sleep syndrome. See comment in PubMed Commons below J Clin Sleep Med. 2009; 5: 83-84.